Clear Sky Science · en
Efficacy of mebendazole in the spontaneous NZBxNZWF1 animal model of systemic lupus erythematosus
Why an old worm pill might help a complex immune disease
Systemic lupus erythematosus, or lupus, is a long‑term disease in which the immune system turns against the body’s own tissues, often damaging the kidneys. Many patients still get only partial relief from today’s drugs, which can also cause serious side effects. This study explores an unexpected candidate: mebendazole, a cheap, long‑used medicine for intestinal worms, to see whether it can calm the overactive immune system in a trusted mouse model of lupus.
Turning a parasite drug toward lupus
Lupus is driven by misfiring immune cells that make antibodies against the body’s own DNA, forming clumps that lodge in organs such as the kidneys and spark inflammation. Researchers have learned that specific cell signaling circuits, especially one called the ERK pathway, are often underactive in key immune cells in lupus. This underactivity is linked to changes in how DNA is chemically marked, which in turn can switch harmful genes on or off. Earlier laboratory work showed that mebendazole can nudge this ERK pathway back into action and block another inflammatory switch known as p38. Because mebendazole already has a long safety record as an antiparasitic drug, the team asked whether it could be “repositioned” as a treatment for lupus.
Testing mebendazole in lupus‑prone mice
The researchers used NZBxNZWF1 mice, a classic strain that naturally develops lupus‑like disease with high levels of anti‑DNA antibodies and kidney inflammation. They ran two types of experiments. In the “preventive” arm, treatment started before clear disease signs appeared; in the “therapeutic” arm, treatment began after the illness was established. Mice received different oral doses of mebendazole on a schedule similar to how people might take pills, and were compared with animals given standard drugs: methotrexate, used in many autoimmune diseases, or an antibody therapy that targets B cells. The team tracked urine protein (a marker of kidney damage), levels of anti‑DNA antibodies in blood, and deposits of antibody in the kidney filters.
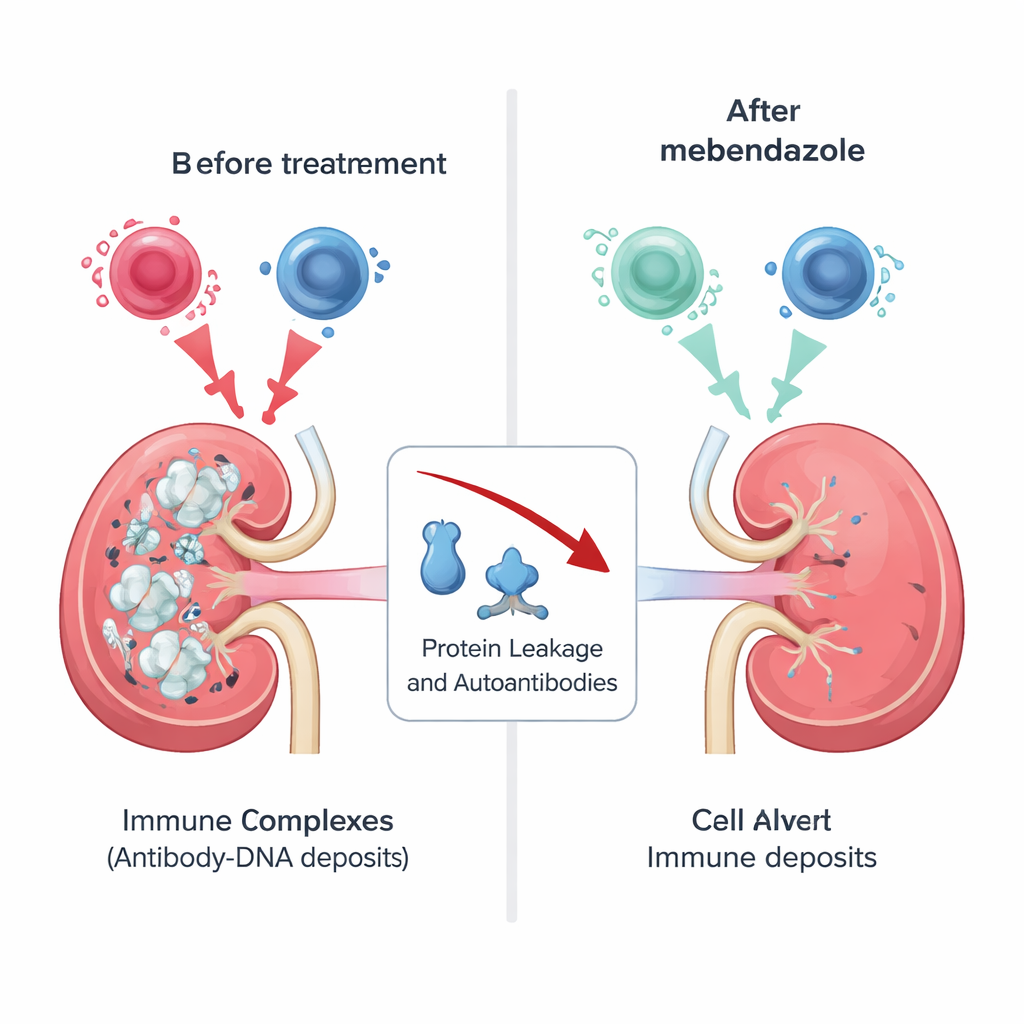
Kidney damage and autoantibodies are reduced
In both early and late treatment settings, mebendazole clearly improved several hallmarks of disease. Mice treated with well‑tolerated doses had less protein leaking into their urine, lower levels of anti‑DNA antibodies over time, and fewer antibody deposits in the kidney’s filtering units than untreated animals. These benefits were seen alongside normal weight gain and few obvious side effects at doses up to 25 mg per kilogram of body weight; a higher dose caused health problems and was dropped from detailed analysis. In some measures, mebendazole performed similarly to existing comparison treatments, suggesting that it can meaningfully blunt the autoimmune attack in this model.
Hints at how the drug is working
To better understand what lies behind these improvements, the scientists also looked at immune cell counts and signaling. In the therapeutic study, mebendazole treatment was linked to changes in the proportions of T cells and B cells in blood and spleen, although not always in the same pattern as the B‑cell‑depleting antibody. Separate laboratory tests on normal mouse B cells showed that mebendazole could slightly boost activity of the ERK pathway at drug levels similar to those measured in treated mice. This aligns with earlier observations in human T cells and supports the idea that mebendazole fine‑tunes immune signaling rather than simply wiping immune cells out. However, the experiments were not designed to pinpoint a single mechanism, and the authors emphasize that several pathways, including p38 inhibition, could be involved.
What this could mean for people with lupus
While mouse studies cannot guarantee success in humans, the consistent improvements seen here—better kidney measures, fewer harmful antibodies and limited side effects—suggest that mebendazole deserves closer study as a potential lupus treatment. Because it is already widely used for other conditions, much is known about its safety and how the body handles it, which could speed the path to carefully designed clinical trials. If future research confirms these findings and clarifies how the drug reshapes immune responses, an inexpensive pill long used to treat worms might one day expand the treatment toolbox for people living with lupus.
Citation: Eloranta, M.L., Nygren, P., Larsson, R. et al. Efficacy of mebendazole in the spontaneous NZBxNZWF1 animal model of systemic lupus erythematosus. Sci Rep 16, 6357 (2026). https://doi.org/10.1038/s41598-026-37930-z
Keywords: lupus, autoimmune disease, mebendazole, kidney inflammation, drug repurposing