Clear Sky Science · en
Habitat-based MRI radiomics for enhanced parkinson’s diagnosis
Why this matters for patients and families
Parkinson’s disease often creeps in slowly, with subtle tremors or stiffness that can be hard to pin down. Today, doctors still rely heavily on symptoms and specialized, expensive scans to make a diagnosis, and early cases are easily missed. This study shows that the same everyday MRI scans many hospitals already use can be mined for hidden patterns, offering a faster, less invasive, and remarkably accurate way to spot Parkinson’s disease.
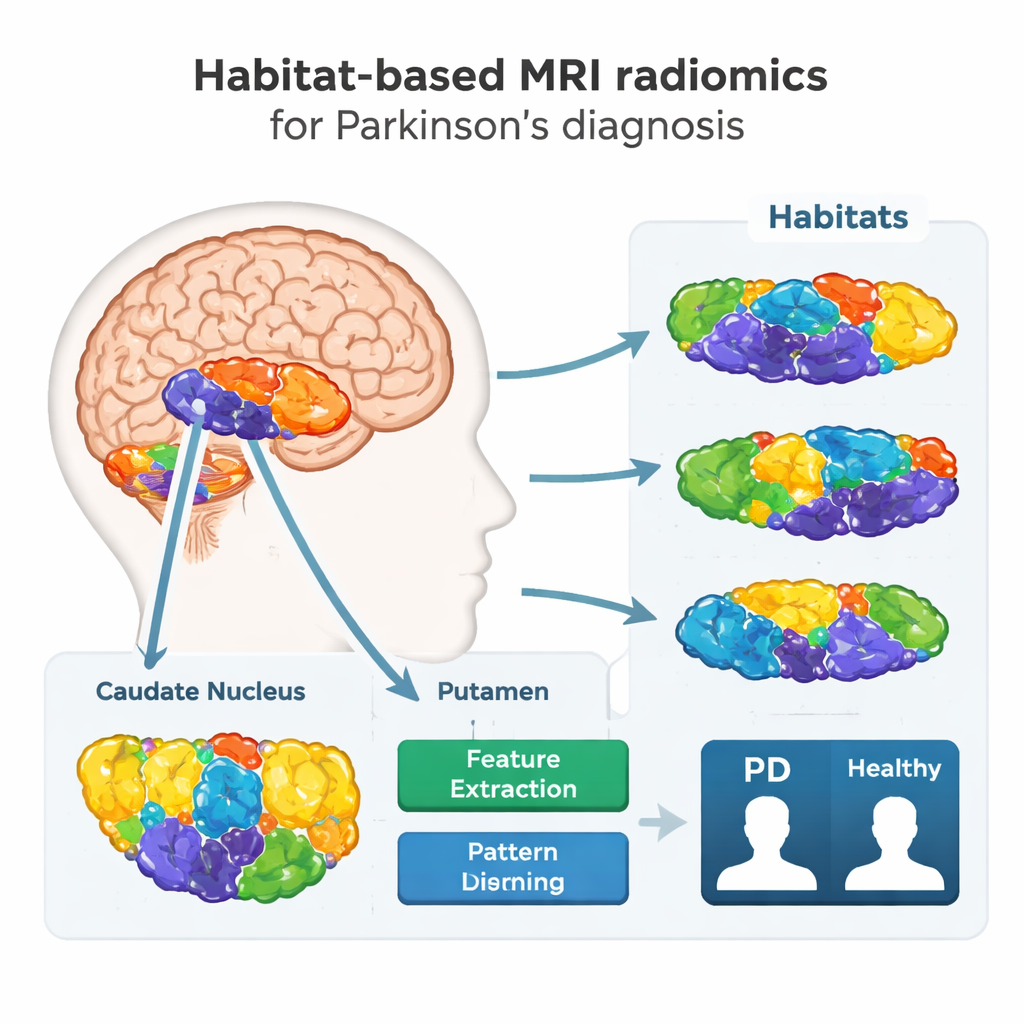
Looking inside the brain in a new way
The researchers focused on two deep brain structures, the caudate nucleus and the putamen, which are central to movement control and heavily affected in Parkinson’s disease. Instead of treating each structure as a single block of tissue, they asked a more detailed question: do different patches inside these regions behave differently on MRI, and can those differences reveal disease? To explore this, they collected routine MRI scans from 308 people—173 with Parkinson’s and 135 healthy volunteers—at two hospitals using different scanners, mirroring the variety found in real-world clinics.
From brain “neighborhoods” to digital fingerprints
Using a technique called habitat-based radiomics, the team broke each target region into smaller “neighborhoods,” or habitats, based on subtle differences in brightness and texture on the MRI images. A computer algorithm grouped voxels (tiny 3D pixels) with similar imaging characteristics into these habitats, then extracted hundreds of numerical features from each one. These features form a kind of digital fingerprint of tissue health, capturing tiny irregularities that are invisible to the naked eye but may reflect nerve cell loss, scarring, or iron buildup associated with Parkinson’s disease.
Training a diagnostic model from routine scans
With these fingerprints in hand, the scientists trained a machine-learning model, known as a support vector machine, to distinguish patients with Parkinson’s from healthy controls. They tested different ways of dividing the brain regions into habitats, from one large zone up to ten smaller ones. Both the main training set and an independent validation set were used to judge performance. When the regions were split into five habitats, the model performed best: on new, unseen data, it correctly identified Parkinson’s in nearly 9 out of 10 people and reached an overall diagnostic accuracy above 94% in the full study. This surpassed earlier approaches that treated each brain region as a single unit and often plateaued around 80–85% accuracy.
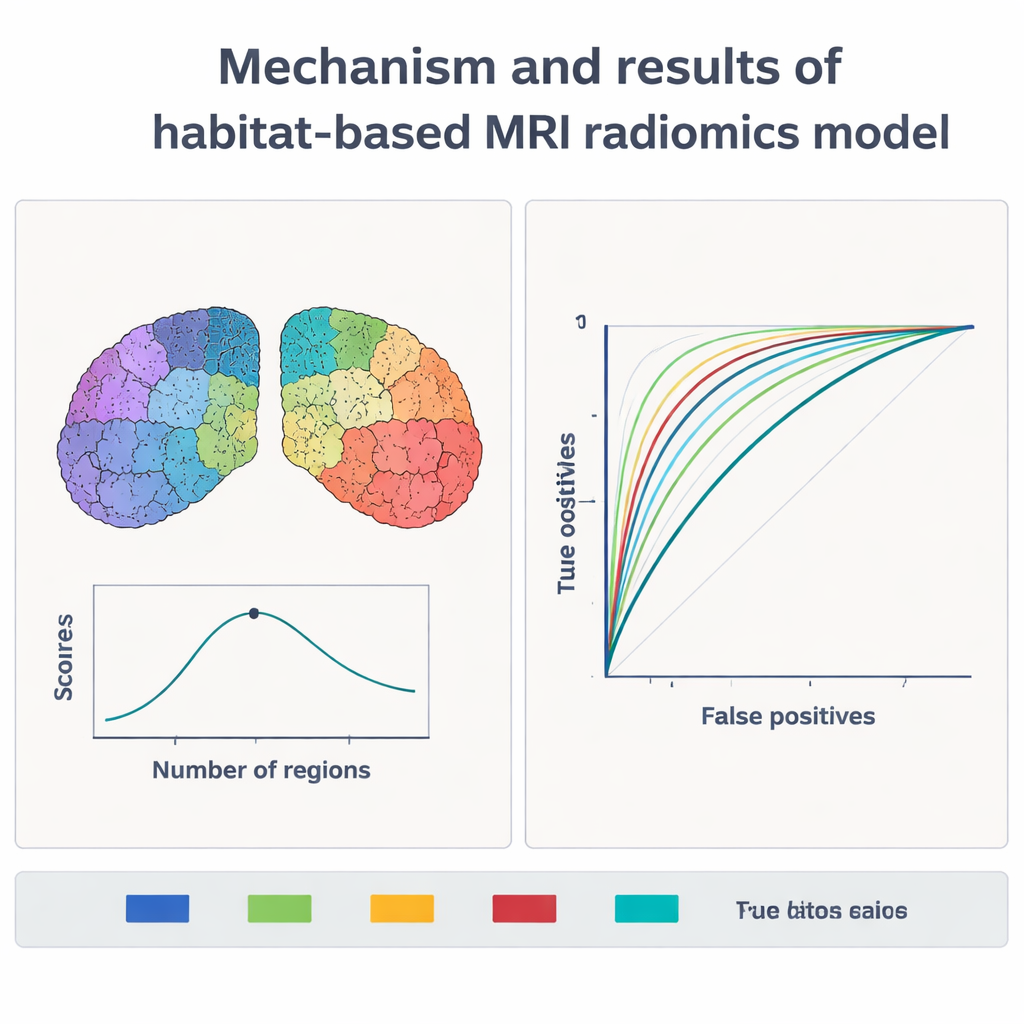
What the model is really seeing
To avoid building a “black box,” the team used an explanation method called SHAP to see which image features influenced the model’s decisions. The most important signals came from T2-weighted MRI, a common clinical sequence. In people with Parkinson’s, the relevant habitats showed greater variation in intensity, more extreme bright and dark spots, and skewed intensity distributions compared with healthy volunteers. These patterns likely mirror known disease processes in the basal ganglia, such as loss of dopamine-producing neurons, local scarring, and abnormal iron deposits. Importantly, the same features kept appearing when the data were split and reanalyzed in different ways, and they remained stable across scanners, suggesting the method is robust rather than a fluke of a single machine.
From research tool to clinic
Decision-curve analyses, which weigh the benefits of catching true cases against the harms of false alarms, indicated that the model could help clinicians decide who truly needs further testing, such as a DaTscan, and who can safely avoid extra, costly procedures. Because the method relies only on standard MRI scans and software, it could be especially valuable in settings where advanced nuclear imaging is unavailable or too expensive. The authors argue that habitat-based radiomics turns familiar MRI pictures into rich data maps, offering a powerful, non-invasive aid for earlier and more accurate Parkinson’s diagnosis and laying groundwork for future tools that might also track disease progression and guide treatment.
Citation: Li, YZ., Wang, Y., Cai, C. et al. Habitat-based MRI radiomics for enhanced parkinson’s diagnosis. Sci Rep 16, 4755 (2026). https://doi.org/10.1038/s41598-026-37923-y
Keywords: Parkinson’s disease, MRI, radiomics, machine learning, early diagnosis