Clear Sky Science · en
Reduced rehabilitation continuity after stroke in patients with substance use disorder based on a TriNetX retrospective cohort study
Why this matters for everyday life
Stroke is often seen as an illness of old age, but more and more younger adults are being affected, especially those who struggle with alcohol or drug problems. This study asks a simple but important question: when people with a history of substance use have a stroke, do they get the rehab care they need to recover—and do they stick with it? The answers shed light on hidden gaps in our health system that affect thousands of working‑age adults and their families.
Who was studied and what was measured
Researchers tapped into a huge international database of electronic medical records, covering more than 150 million patients from over 130 health systems. From this, they identified adults who had a first stroke between 2019 and 2023, then divided them into two groups: those with a diagnosed substance use disorder and those without. They focused on what happened in the first six months after the stroke—specifically, whether patients started any kind of rehab, such as physical, occupational, or speech therapy, and how many rehab sessions they actually attended. To make a fair comparison, they matched patients in the two groups so they were similar in age, medical conditions, and social risk factors, such as poverty or unstable housing. 
Starting rehab: more need, more first visits
The study found a striking pattern. Stroke survivors with a history of substance use were noticeably more likely to begin rehab than those without such a history. About one‑third of patients with substance use disorders entered some type of rehab within 180 days, compared with less than one‑fifth of those without. This was true across all age groups and for both men and women, but the difference was especially large among younger adults between 18 and 44, and among working‑age men. The researchers interpret this as a sign that people with substance use problems may experience more severe strokes or greater overall health challenges, leading doctors to refer them to rehab more often and more urgently.
Sticking with rehab: fewer sessions, earlier drop‑off
Yet the promising start hid a troubling reality: patients with substance use disorders attended fewer rehab sessions on average than those without. Over the first six months after stroke, the group with substance use disorder completed fewer billed therapy visits, suggesting more missed appointments, early drop‑out, or difficulty returning regularly. This pattern held across most age and sex groups, with the biggest gap seen in men aged 45 to 64—a group that often juggles work, family responsibilities, and financial pressures. The authors point to several likely reasons, including depression and other mental health issues, unstable housing or transportation, limited insurance coverage, and the everyday chaos that can accompany ongoing substance use.
Young adults face layered challenges
The study highlights that many stroke patients with substance use disorders are adolescents and young adults—people who may already have struggled in school, at work, or in relationships before their stroke. Problems with memory, attention, and decision‑making, which are common in substance use disorders and made worse by stroke, can make it harder to follow complex treatment plans or keep up with regular appointments. At the same time, most rehab programs were originally designed for older adults and may not fit the needs, schedules, or motivations of younger people. The authors argue that these younger stroke survivors need age‑appropriate, flexible rehab that also addresses mental health and addiction, rather than focusing only on physical recovery. 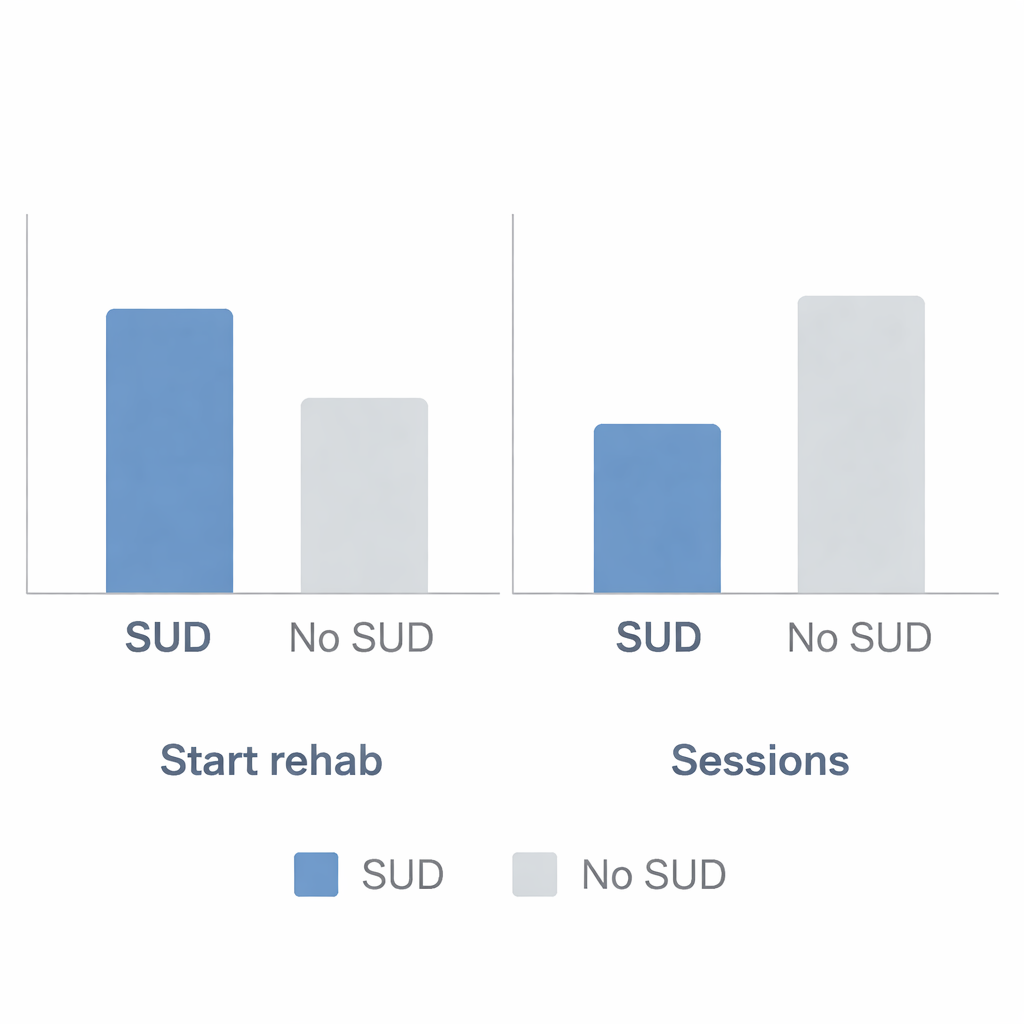
What this means for patients and families
In plain terms, the study shows that people with substance use problems are getting through the clinic door for rehab after a stroke—but they are not staying long enough to reap the full benefit. For families, this underscores the importance of not only securing that first therapy appointment, but also helping loved ones keep going week after week. For health systems, it signals an urgent need to redesign stroke rehab to better support this high‑risk group—for example, by coordinating closely with addiction and mental health services, offering more flexible scheduling or tele‑rehab options, and paying attention to basic needs like transportation and housing. By making it easier for these patients to stay engaged, we may improve recovery, reduce disability in working‑age adults, and lessen the long‑term burden of stroke on society.
Citation: Kao, HH., Liu, T., Lin, WC. et al. Reduced rehabilitation continuity after stroke in patients with substance use disorder based on a TriNetX retrospective cohort study. Sci Rep 16, 6734 (2026). https://doi.org/10.1038/s41598-026-37919-8
Keywords: stroke rehabilitation, substance use disorder, young adults, treatment adherence, mental health and recovery