Clear Sky Science · en
A comparative evaluation of time-series models for forecasting inpatient deaths and discharges against medical advice
Why hospital numbers matter
When we enter a hospital, we trust that doctors and nurses will do everything they can to keep us safe. Two warning signs that something may be going wrong are how many patients die in the hospital and how many leave against medical advice, walking out even when doctors advise them to stay. Being able to forecast these numbers a few months ahead can help hospitals spot trouble early, prepare enough staff and beds, and improve care before problems escalate.
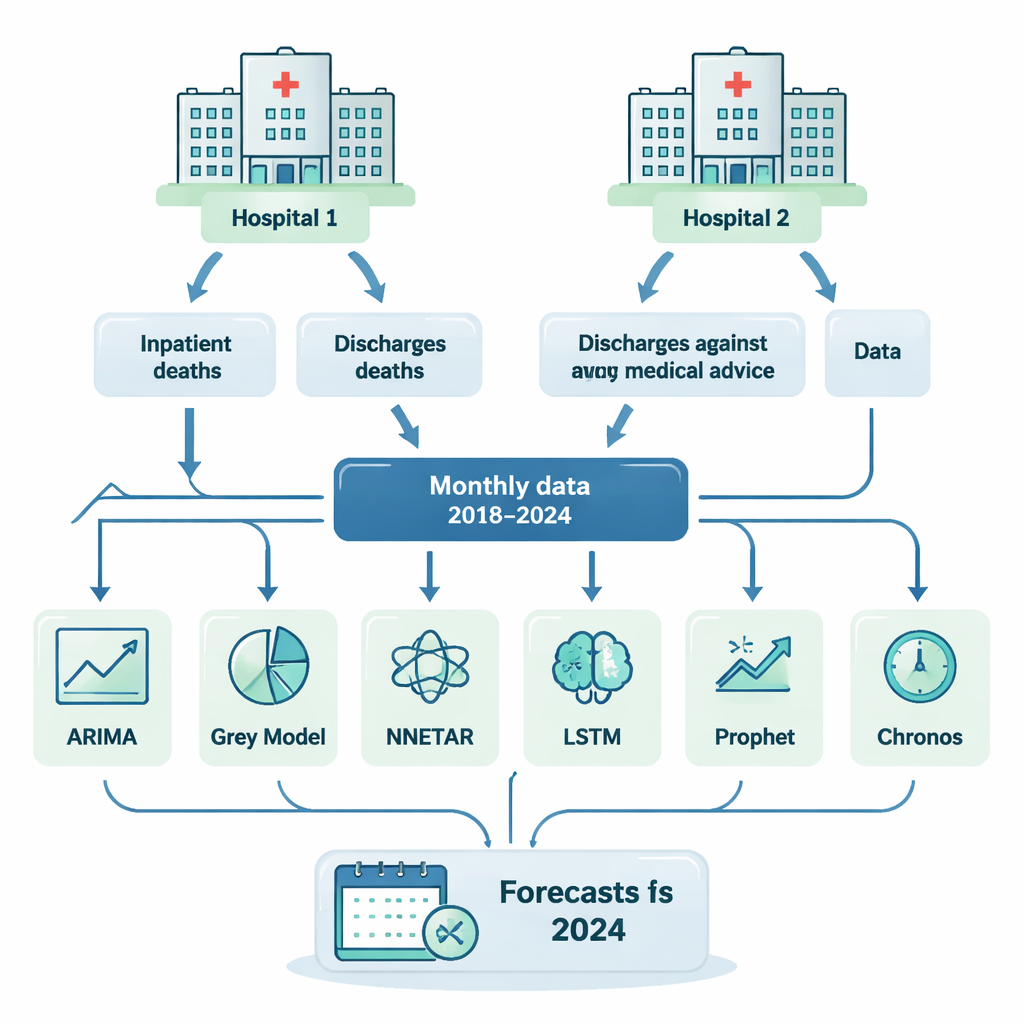
Two hospitals, two warning signals
This study focused on two large referral hospitals in different regions of China. For each hospital, the researchers tracked two key outcomes every month from 2018 to 2024: inpatient deaths (patients who died while admitted) and discharges against medical advice (patients who chose to leave early despite medical warnings). These measures are widely used as indicators of care quality and system stress. The team deliberately avoided heavy data cleaning or adjustment so that the forecasts would reflect the messy, real-world information that hospital managers actually see.
Putting forecasting tools to the test
The authors compared six different forecasting approaches that are commonly discussed in statistics and artificial intelligence. Some, like ARIMA and the Grey Model, are traditional statistical tools. Others, such as NNETAR and LSTM, use neural networks that try to learn patterns from past data. Prophet models trends and seasonal swings, like regular yearly cycles. The newest entrant, Chronos, is a large pretrained model that has already learned from huge collections of time-series data and can be applied to new problems with little tuning. All six methods were trained on data from 2018 through 2023 and then asked to predict what actually happened in 2024, with accuracy judged by how far the forecasts strayed from the real monthly numbers.
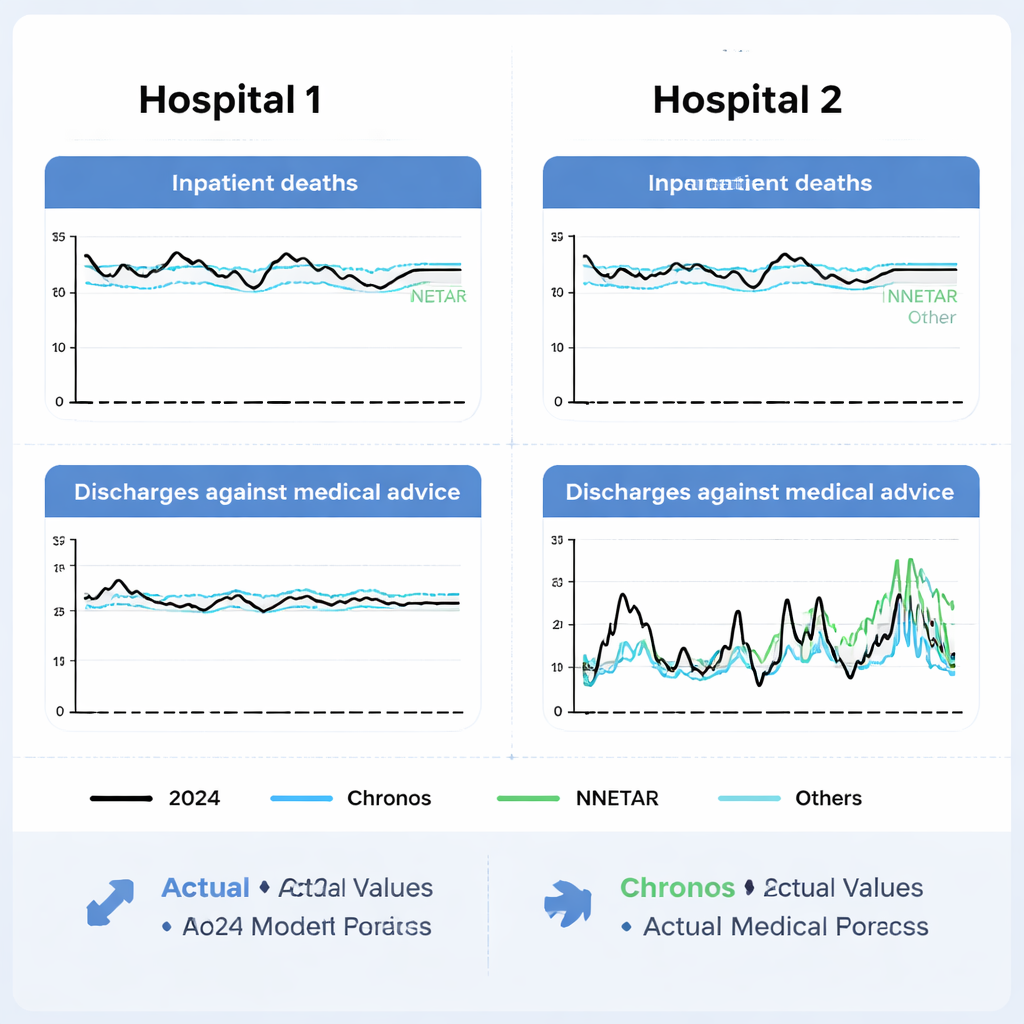
What worked best, and when
Across both hospitals, Chronos gave the most reliable forecasts for inpatient deaths. Its errors were smaller than those of the other approaches, and statistical tests confirmed that these gains were unlikely to be due to chance, especially when compared with a popular deep learning model called LSTM. For discharges against medical advice, the picture was more nuanced. In the hospital where these discharges were frequent and fairly steady over time, Chronos again performed best. But in the hospital where such discharges were less common and bounced around unpredictably from month to month, a simpler neural network, NNETAR, produced more accurate predictions than the more complex models.
Why complexity is not always king
One striking lesson from the study is that adding complexity does not guarantee better forecasts. The LSTM model, which is powerful in theory but has many adjustable parts, struggled with the relatively small data sets available here and often overfit—capturing noise rather than true patterns. Chronos, by contrast, benefitted from the broad experience it gained during pretraining on other time series, allowing it to stay robust even when each hospital provided only a few years of data. At the same time, the success of NNETAR in the noisier discharge data shows that in some settings, lighter-weight models that make fewer assumptions can do a better job of handling unstable, low-volume signals.
What this means for patients and hospitals
For non-specialists, the takeaway is straightforward: smarter forecasting tools can help hospitals see around the corner. By choosing models that fit the shape of their data—pretrained systems like Chronos for stable indicators, and simpler networks like NNETAR when numbers are small and jumpy—hospital leaders can get earlier warnings about rising deaths or sudden shifts in patients leaving against medical advice. These forecasts are not crystal balls, especially when dealing with small, volatile numbers, but they are valuable dashboards. Used wisely, they can prompt closer review of care practices, more agile staffing and bed management, and faster responses to emerging problems, ultimately supporting safer, more reliable care for patients.
Citation: Pang, C., Jiayong, D., Jiang, D. et al. A comparative evaluation of time-series models for forecasting inpatient deaths and discharges against medical advice. Sci Rep 16, 6607 (2026). https://doi.org/10.1038/s41598-026-37913-0
Keywords: hospital forecasting, inpatient mortality, discharge against medical advice, time series models, healthcare quality