Clear Sky Science · en
The effect of non-pharmaceutical interventions on influenza throughout the COVID-19 pandemic: an 8-year interrupted time series study
Why this matters for everyday life
During the COVID-19 pandemic, masks, lockdowns, and social distancing didn’t just curb coronavirus—they also dramatically changed the way the flu spread. This study from Sichuan Province in China looks back over eight years of data to ask a question that affects all of us: how much did these measures really hold back influenza, and what happened once life began to return to normal?
Big changes during an unusual period
The researchers examined weekly records from 30 hospitals across 21 cities in Sichuan between 2017 and 2024. They tracked two types of numbers: people with “influenza-like illness” (fever plus cough or sore throat) and patients who tested positive for the flu virus in the lab. This long stretch covered three distinct periods: before COVID-19 restrictions, during strict non-drug measures such as mask-wearing and lockdowns, and after those measures were lifted. By comparing these phases, the team could see how human behavior and policy reshaped flu transmission over time.
What happened when strict measures began
When China introduced strong non-pharmaceutical interventions (NPIs) in early 2020, influenza activity collapsed almost overnight. The study found that flu-like illnesses dropped by about 95 percent and lab-confirmed flu cases by about 98 percent right after these measures took effect. In other words, the combination of masks, school closures, travel limits, and reduced social contact nearly shut down flu transmission in the short term. These results echo findings from other countries: actions taken to control COVID-19 also blocked many other respiratory infections that spread through the air in similar ways.
The hidden cost of “immune debt”
However, the story did not end with low case counts. Because people were exposed to the flu virus far less often during the COVID-19 years, their immune systems had fewer chances to refresh their defenses. The authors describe this as a kind of “immune debt.” When strict measures were loosened and everyday mixing resumed, the number of people with flu-like illness surged to more than double the pre-pandemic baseline. Lab-confirmed flu cases did not spike as sharply at once, but their overall trend pointed upward, suggesting that larger outbreaks could still emerge as susceptible people accumulated.
New patterns after restrictions were lifted
Interestingly, once the second phase of changes took place—when formal controls ended but some protective habits remained—both flu-like illness and confirmed flu cases began to fall again week by week, instead of snapping back to old patterns. The study suggests several reasons. First, years of suppression likely broke many chains of flu spread, so it took time for the virus to regain a foothold. Second, some people kept voluntary behaviors such as mask use when sick, better hand-washing, and staying home with symptoms, all of which quietly slowed transmission. Third, the researchers note that other respiratory viruses may now compete with influenza, and that temperature strongly affected flu levels, with warmer weeks linked to fewer cases, while humidity played little role in this setting.
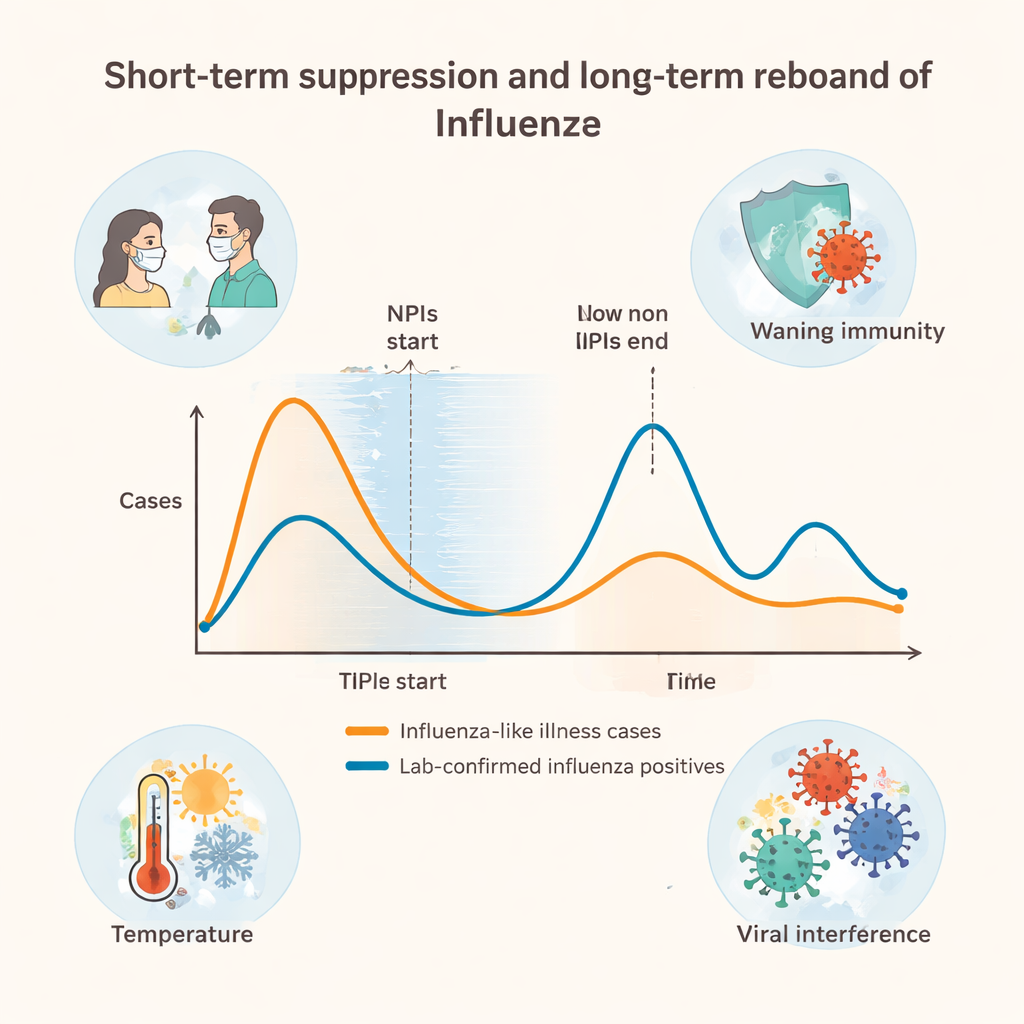
What this means for future outbreaks
For policymakers, the main message is that human actions can sharply bend the curve of flu epidemics, but they do not erase the virus or its long-term tendency to spread. Non-pharmaceutical interventions are powerful tools for buying time and protecting health systems during crises, yet prolonged use may simply postpone large outbreaks if immunity in the population is not renewed through vaccination or natural exposure. For the public, the study shows that everyday behaviors—masks in crowded places, hand hygiene, and staying home when ill—can make a big difference, especially when combined with flu vaccination. Thoughtfully timed measures, rather than permanent strict controls, may offer the best balance between controlling outbreaks and allowing our immune systems to keep pace with ever-changing respiratory viruses.
Citation: Li, Z., Zhou, L., Zhou, X. et al. The effect of non-pharmaceutical interventions on influenza throughout the COVID-19 pandemic: an 8-year interrupted time series study. Sci Rep 16, 6593 (2026). https://doi.org/10.1038/s41598-026-37911-2
Keywords: influenza, COVID-19, non-pharmaceutical interventions, immune debt, respiratory viruses