Clear Sky Science · en
Interleukin-7 induces EMT to promote tumor growth and metastasis in NSCLC via Notch1/TGF-β pathway
Why a signaling protein matters in lung cancer
Lung cancer remains one of the deadliest cancers worldwide, largely because it is often discovered after it has already spread. This study focuses on a naturally occurring immune messenger, interleukin‑7 (IL‑7), and asks a pressing question: in non‑small cell lung cancer (NSCLC), does IL‑7 help the body fight the tumor, or does it actually help the tumor grow and move? By tracing how IL‑7 affects lung cancer cells in patients, cell cultures, and mice, the researchers uncover a pathway that appears to push tumors toward greater growth, spread, and treatment resistance.
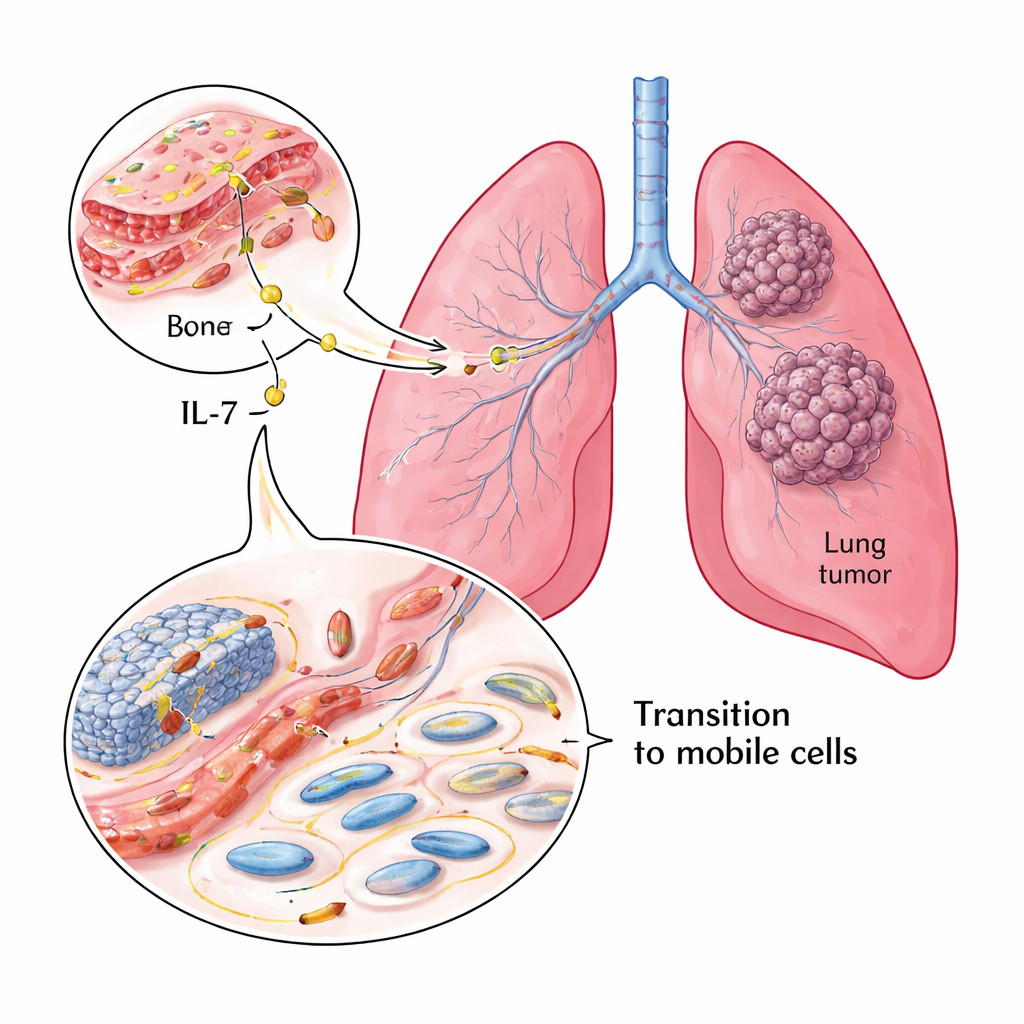
A closer look at lung tumors and patient outcomes
The team began by examining tumor samples from 119 patients with NSCLC. Using staining techniques on preserved tissue, they measured the levels of IL‑7, its receptor (IL‑7R), and two key markers that describe how “anchored” or “mobile” cancer cells are. E‑cadherin is associated with tightly connected, less mobile cells, while Vimentin is linked to more flexible, invasive cells. Most tumors showed high IL‑7 and IL‑7R. When IL‑7 and IL‑7R were abundant, E‑cadherin tended to be low and Vimentin high—an unfavorable pattern. Patients whose tumors retained more E‑cadherin survived longer, while those with high IL‑7R had poorer survival, making IL‑7R a strong predictor of outcome.
How cancer cells switch from staying put to breaking away
To move beyond correlation, the researchers tested how IL‑7 directly affects lung cancer cells grown in the lab. When two NSCLC cell lines were exposed to IL‑7, the cells shifted from a compact, cobblestone appearance toward a more elongated, free‑moving shape. Inside the cells, protein levels changed in step: E‑cadherin dropped, while “mobile cell” markers such as N‑cadherin, Vimentin, and Snail1 rose. The actin skeleton of the cells, which helps them crawl, also became more prominent and formed protrusions. Blocking the IL‑7 receptor reversed these effects, indicating that IL‑7 drives this shape‑shifting process—known as epithelial‑to‑mesenchymal transition (EMT)—through its own receptor on lung cancer cells.
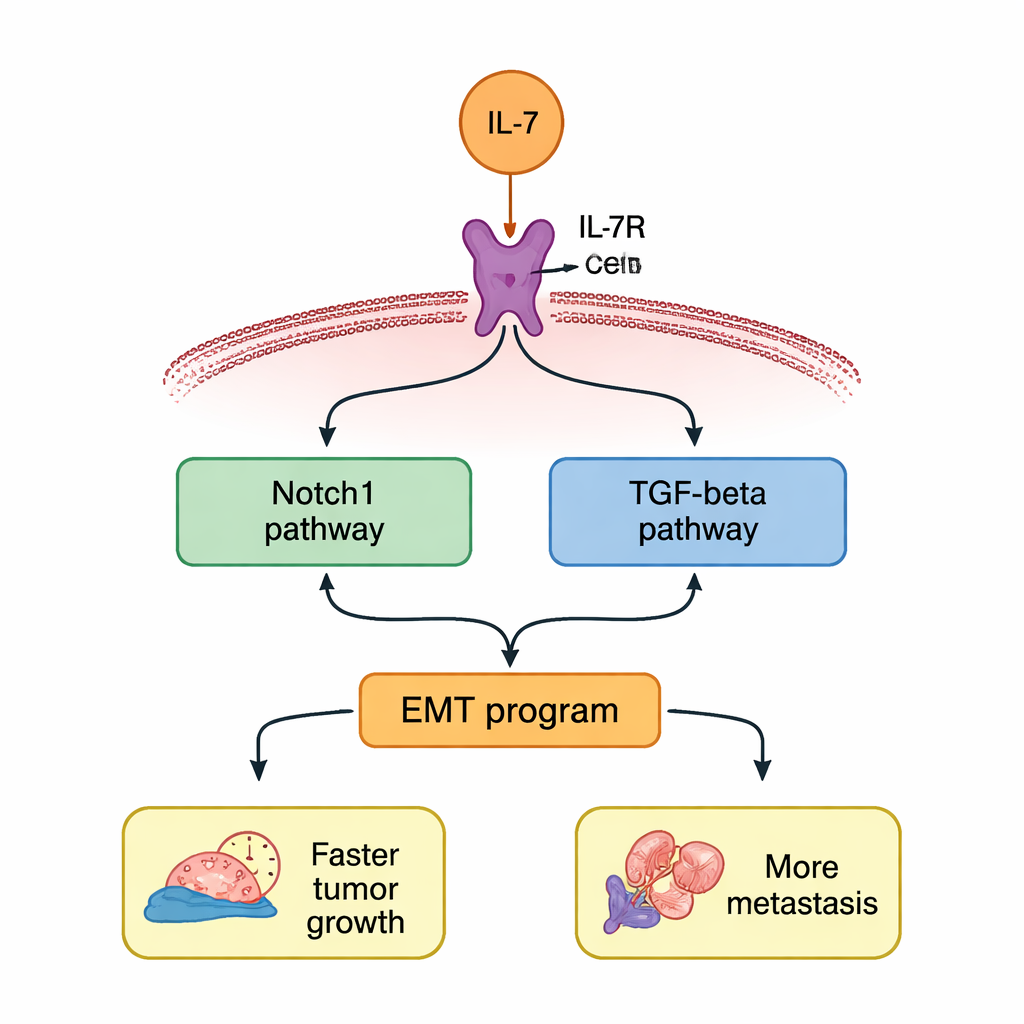
Two linked pathways that amplify the danger
The study then asked how IL‑7 sends these instructions inside the cell. The authors focused on two well‑known signaling routes, often active in aggressive cancers: Notch1 and TGF‑β. After IL‑7 treatment, both Notch1 and TGF‑β increased at the gene and protein levels in lung cancer cells. If the researchers blocked IL‑7R, these rises disappeared. When they used specific drugs to inhibit Notch1 or TGF‑β, both pathways quieted down together, suggesting a kind of positive feedback loop where each route helps sustain the other. Cutting either pathway partly shut down the EMT program and reduced the IL‑7‑driven boost in cell growth, migration, and invasion.
From petri dish to living lungs
To see whether these laboratory findings hold up in living organisms, the team turned to mouse models. In one set of experiments, lung cancer cells were implanted under the skin. Mice given IL‑7 developed larger, heavier tumors than controls. Tumor tissue from these animals showed lower E‑cadherin, higher Vimentin and Snail1, and greater activity of Notch1 and TGF‑β. When the mice also received inhibitors of Notch1 or TGF‑β, tumor growth and these aggressive markers were markedly reduced. In a second model, cancer cells were injected into the bloodstream via the tail vein. Here, IL‑7‑treated mice ended up with more lung metastases and heavier lungs, while pathway‑blocking drugs again curbed this spread.
What this means for future lung cancer care
Taken together, the work paints IL‑7 not as a simple immune helper, but as a double‑edged sword in NSCLC. In this setting, IL‑7 appears to push tumor cells to loosen their bonds, adopt a more mobile identity, and travel to new sites, all through a reinforcing network centered on the Notch1 and TGF‑β pathways. For patients, these findings suggest that high IL‑7R in tumors may flag a worse prognosis and that carefully designed therapies targeting IL‑7/IL‑7R or its downstream routes could help slow tumor growth and metastasis. While more research is needed to map the exact molecular links and to test safety in humans, this study highlights a promising new set of levers for shifting the balance against lung cancer.
Citation: Shao, Y., Cheng, H., Ni, W. et al. Interleukin-7 induces EMT to promote tumor growth and metastasis in NSCLC via Notch1/TGF-β pathway. Sci Rep 16, 7326 (2026). https://doi.org/10.1038/s41598-026-37876-2
Keywords: non-small cell lung cancer, interleukin-7, epithelial-mesenchymal transition, Notch1 pathway, TGF-beta signaling