Clear Sky Science · en
Integrating body composition analysis and machine learning for non-invasive identification of metabolic dysfunction-associated fatty liver disease: a large-scale health examination-based study
Why hidden liver fat matters
Many people who feel perfectly healthy are quietly developing fat buildup in their livers, a condition now called metabolic dysfunction–associated fatty liver disease (MAFLD). It is closely tied to weight gain, high blood sugar, and heart disease, yet is often missed at routine check‑ups because standard measures like weight and basic blood tests do not fully reveal what is happening inside the body. This study explores whether a quick body composition scan combined with modern computer algorithms can flag those at risk long before serious liver damage occurs.
Looking inside the body without a needle
The researchers drew on records from more than 23,000 adults in China who had regular health examinations between 2017 and 2021, plus an additional 3,300 people examined later to double‑check the results. Everyone had two key tests: an abdominal ultrasound to see whether there was fat in the liver, and a body composition analysis using bioelectrical impedance, a bathroom‑scale‑like device that sends a very weak current through the body. This scan estimates how much fat, muscle, bone, and water a person carries, and how much of that fat sits deep inside the abdomen as visceral fat, the type most strongly linked to metabolic disease. 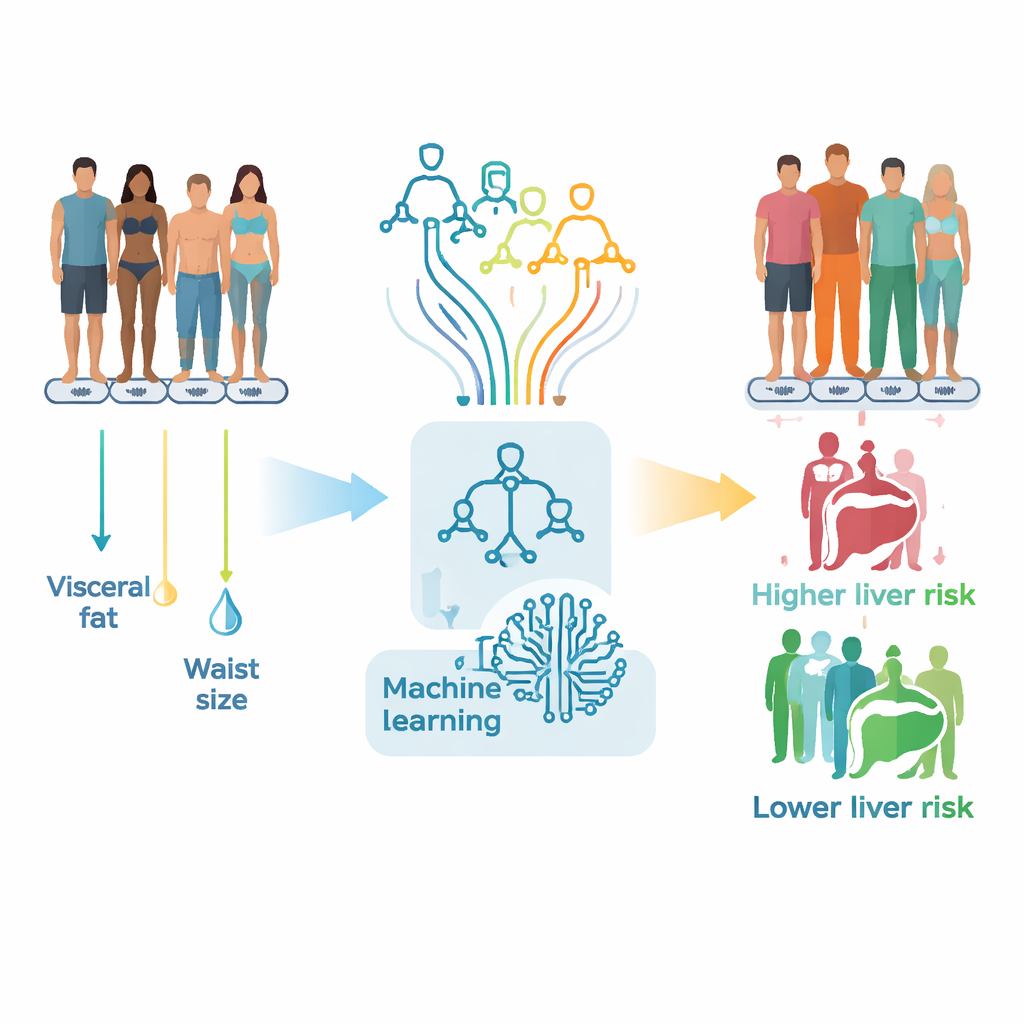
Turning body measurements into risk signals
From a long list of possible measurements, the team focused on 13 that can be collected without drawing blood, such as age, sex, waist size, body mass index (BMI), total body water, and a visceral fat rating. They then used statistical checks to remove overlapping or redundant measurements and relied on an interpretability method called SHAP to see which features carried the most information about liver fat. In the end, six measurements stood out as both reliable and practical: visceral fat rating, waist circumference, body weight, BMI, total body water, and the proportion of fluid outside cells (extracellular water percentage). These variables became the inputs for eight different computer models trained to distinguish people with MAFLD from those without it.
Machine learning that spots risk with high accuracy
The team built and compared several types of machine learning models, including simple logistic regression, support vector machines, and more advanced tree‑based methods such as gradient boosting and random forests. Using tenfold cross‑validation inside the main dataset, the tree‑based models consistently came out on top, reaching areas under the receiver operating characteristic curve (AUC) above 0.96. This means the models almost always scored a person with MAFLD higher than a person without it. When the researchers tested these models on the separate group of more than 3,000 later patients, performance remained very strong, with AUC values still above 0.95 and high accuracy and recall. In real‑world terms, the combined body composition and machine learning approach was very good at correctly flagging people who had fatty liver while keeping false alarms relatively low. 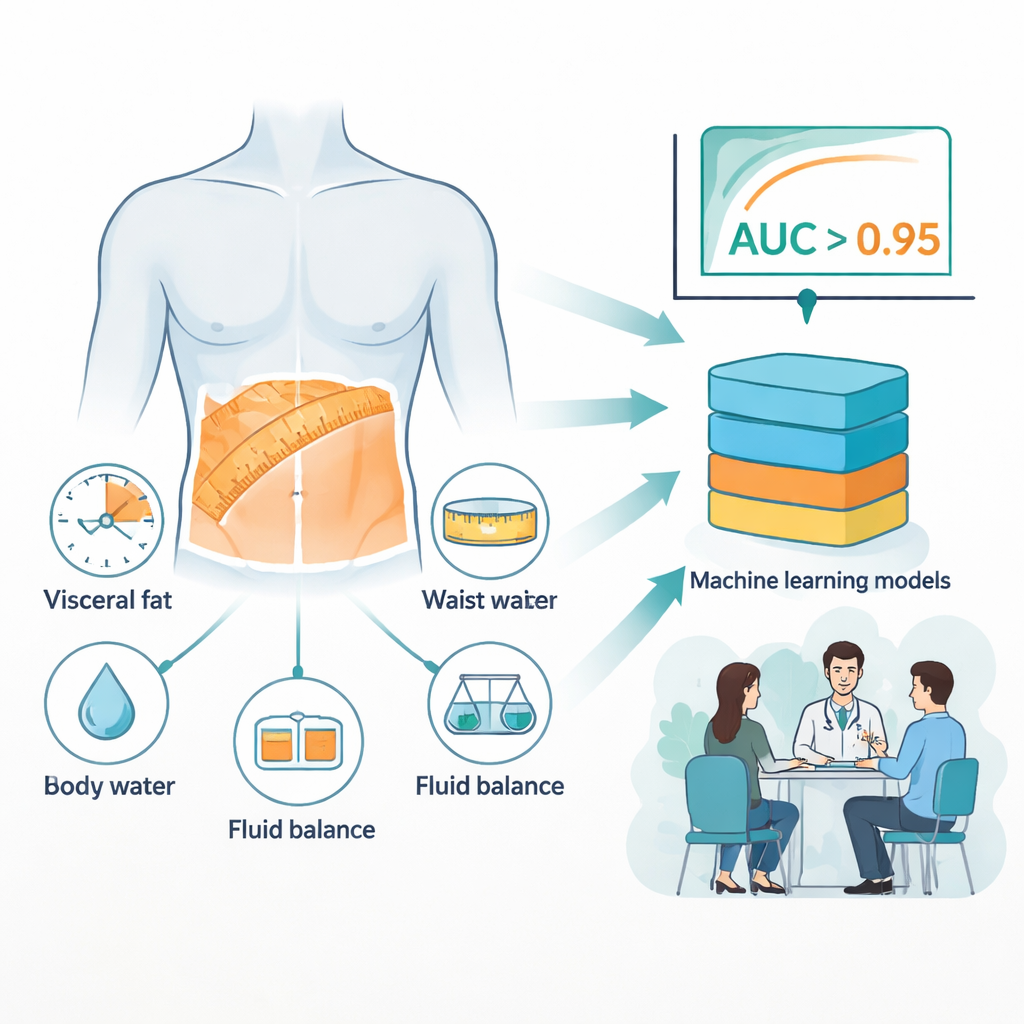
The special role of belly fat and body fluids
Across every model and subgroup—men and women, younger and older adults, lean and heavier people—visceral fat rating was the single most powerful signal of MAFLD. Waist circumference and BMI were also important but slightly less informative, underscoring that where fat is stored matters more than how much a person weighs overall. The study also highlighted the importance of body water balance. A higher proportion of extracellular water, which may reflect subtle fluid retention and inflammation, was associated with greater odds of fatty liver, while higher total body water tended to be protective, perhaps indicating better muscle mass and overall metabolic health.
What this could mean for everyday check‑ups
For patients, the takeaway is that a quick step onto a body composition device, combined with a behind‑the‑scenes machine learning model, could one day provide an early warning about liver health without needles, radiation, or expensive scans. The study suggests that focusing on deep belly fat and fluid balance offers a clearer picture of metabolic risk than weight or BMI alone. While more research is needed in different countries and over longer time periods, this approach points toward a future in which routine health visits quietly generate powerful, personalized risk scores that help doctors and patients act on MAFLD before it silently progresses.
Citation: He, Y., Cao, Y., Chen, Z. et al. Integrating body composition analysis and machine learning for non-invasive identification of metabolic dysfunction-associated fatty liver disease: a large-scale health examination-based study. Sci Rep 16, 7038 (2026). https://doi.org/10.1038/s41598-026-37852-w
Keywords: fatty liver, visceral fat, body composition, machine learning, noninvasive screening