Clear Sky Science · en
Homocysteine levels and cancer risk in hypertensive adults across MTHFR C677T genotypes
Why a blood test might reveal hidden cancer risk
Many people with high blood pressure visit clinics regularly for check‑ups and blood tests. This routine care offers a unique chance to spot other health dangers early. In this study, researchers asked whether levels of a common blood molecule called homocysteine, together with a person’s genetic make‑up, could signal a higher risk of developing cancer. If so, a simple lab value that is already measured in many patients could help doctors identify who needs closer monitoring or preventive care.
A common molecule with a dark side
Homocysteine is a normal by‑product of how our bodies handle protein. Under usual conditions, vitamins such as folate help recycle it, keeping levels in check. When homocysteine builds up, however, it can irritate blood vessels, damage DNA, and disturb how genes are switched on and off – processes that may pave the way to cancer. A key player in this recycling system is a gene called MTHFR. A frequent variant of this gene, named C677T, makes the enzyme it encodes run less efficiently. People who inherit two copies of this variant (the TT type) tend to have higher homocysteine levels, especially if their folate intake is modest.
Following thousands of patients over time
The research team drew on the China H‑Type Hypertension Registry Study, which tracks tens of thousands of adults with high blood pressure in Rongcheng, a city in eastern China. From more than 87,000 participants who were cancer‑free at the start, 1,419 went on to develop cancer during several years of follow‑up. For each of these patients, the investigators selected a similar participant of the same age, sex, and neighborhood who did not develop cancer, and compared their baseline blood tests and genetic results. After excluding people with missing data, they analyzed 1,219 cancer patients and 1,219 matched controls.
Homocysteine, genes, and who faced more cancers
Across the entire group, each stepwise rise in homocysteine was linked to a modest but measurable increase in the chance of being diagnosed with cancer, even after accounting for smoking, alcohol use, body weight, blood fats, blood sugar, and other factors. When the researchers divided people into three bands of homocysteine, those in the highest band tended to have more cancers than those in the lowest. The most striking pattern emerged when they looked separately at people with different MTHFR C677T genotypes. Among individuals with the TT type, high homocysteine was strongly tied to greater risks of cancers in both the digestive system and other organs, including lung cancer. In contrast, those with the CC or CT types showed weaker and less consistent links.
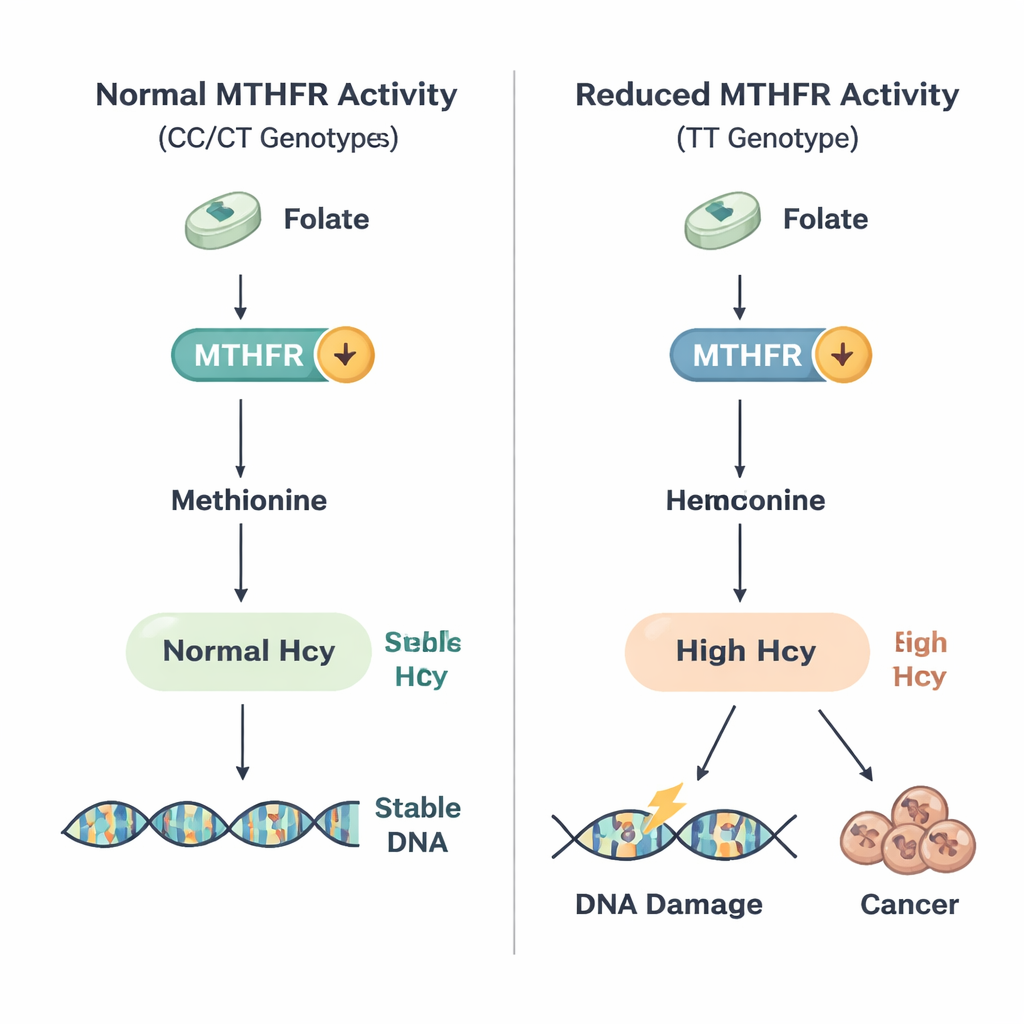
Clues to how homocysteine may harm cells
Why might high homocysteine be especially risky for people with the TT genotype? The study and prior work suggest that these individuals have a less flexible folate system: even when folate is available, their reduced‑activity enzyme cannot fully stabilize homocysteine levels. Persistently elevated homocysteine can then promote DNA damage, oxidative stress, and chronic inflammation, all of which can drive cells toward cancerous change. The researchers also found that the usual negative relationship between folate and homocysteine was weaker in TT carriers, hinting that diet alone may not completely offset their inherited vulnerability.
What this means for patients and doctors
For people living with high blood pressure, this study suggests that a routine homocysteine measurement, combined with a one‑time genetic test for MTHFR C677T, could help flag a subgroup at especially high cancer risk. The findings do not prove that homocysteine directly causes cancer, and they come from a single region and a group limited to hypertensive adults. Still, they raise the possibility that lowering homocysteine through improved diet, vitamin supplementation, or other measures could one day become part of cancer prevention – particularly for those with the TT genotype. Larger, longer studies will be needed to test whether changing homocysteine levels can truly change cancer outcomes.
Citation: Li, W., Xu, G., Yang, L. et al. Homocysteine levels and cancer risk in hypertensive adults across MTHFR C677T genotypes. Sci Rep 16, 7251 (2026). https://doi.org/10.1038/s41598-026-37849-5
Keywords: homocysteine, cancer risk, MTHFR C677T, hypertension, folate metabolism