Clear Sky Science · en
Sustainable and interpretable heart disease prediction: a clinical decision support approach for biomedical healthcare applications
Why Smarter Heart Checks Matter
Heart disease is the world’s leading killer, yet many people still find out they are at risk only after a serious event such as a heart attack. Doctors already collect simple measurements—like age, blood pressure, cholesterol, and basic test results—but turning this information into a fast, reliable yes-or-no answer about heart disease is challenging. This study explores a new kind of computer model that can learn from those routine numbers, predict who is likely to have heart disease with very high accuracy, and, crucially, explain its reasoning in terms doctors can understand.
The Growing Burden of Heart Disease
Every year, cardiovascular diseases claim about 18 million lives worldwide. Many of these deaths could be prevented if high–risk patients were identified earlier and treated sooner. Traditional diagnostic tests can be invasive, expensive, or not accurate enough for borderline cases. In parallel, hospitals now store huge amounts of digital data about patients, from age and sex to blood pressure, cholesterol, and basic heart test readings. Turning this flood of information into clear, dependable risk estimates has become one of modern medicine’s biggest opportunities—and biggest challenges.
From Black Boxes to Transparent Helpers
In recent years, artificial intelligence has shown promise in spotting subtle patterns in medical data that humans might miss. However, many powerful models behave like “black boxes”: they may be accurate, but they cannot easily explain why they reached a particular decision. That lack of transparency is a problem in medicine, where doctors must justify diagnoses and treatment choices. The authors address this gap by designing a heart–disease prediction system based on a one‑dimensional convolutional neural network (1D CNN). Unlike older methods that require experts to handcraft which features to look at, this network automatically discovers useful patterns in standard patient measurements, yet is still designed to be efficient enough for clinics with limited computing resources.
How the Model Learns from Routine Checkups
The researchers trained their system on a widely used heart disease dataset containing 303 patient records, each with 14 commonly collected items such as age, sex, blood pressure, cholesterol level, type of chest pain, and results from basic heart tests. They carefully prepared the data: numerical values were standardized so that no single measurement dominated the learning process, and categories like chest pain type were converted into numeric form. To make the most of the relatively small dataset and mimic the natural noise of real clinical measurements, the team added a small amount of random variation to the training data. They then fed these records into a compact 1D CNN architecture with two main pattern‑detection layers, followed by layers that combine these patterns into a final “disease” or “no disease” prediction.
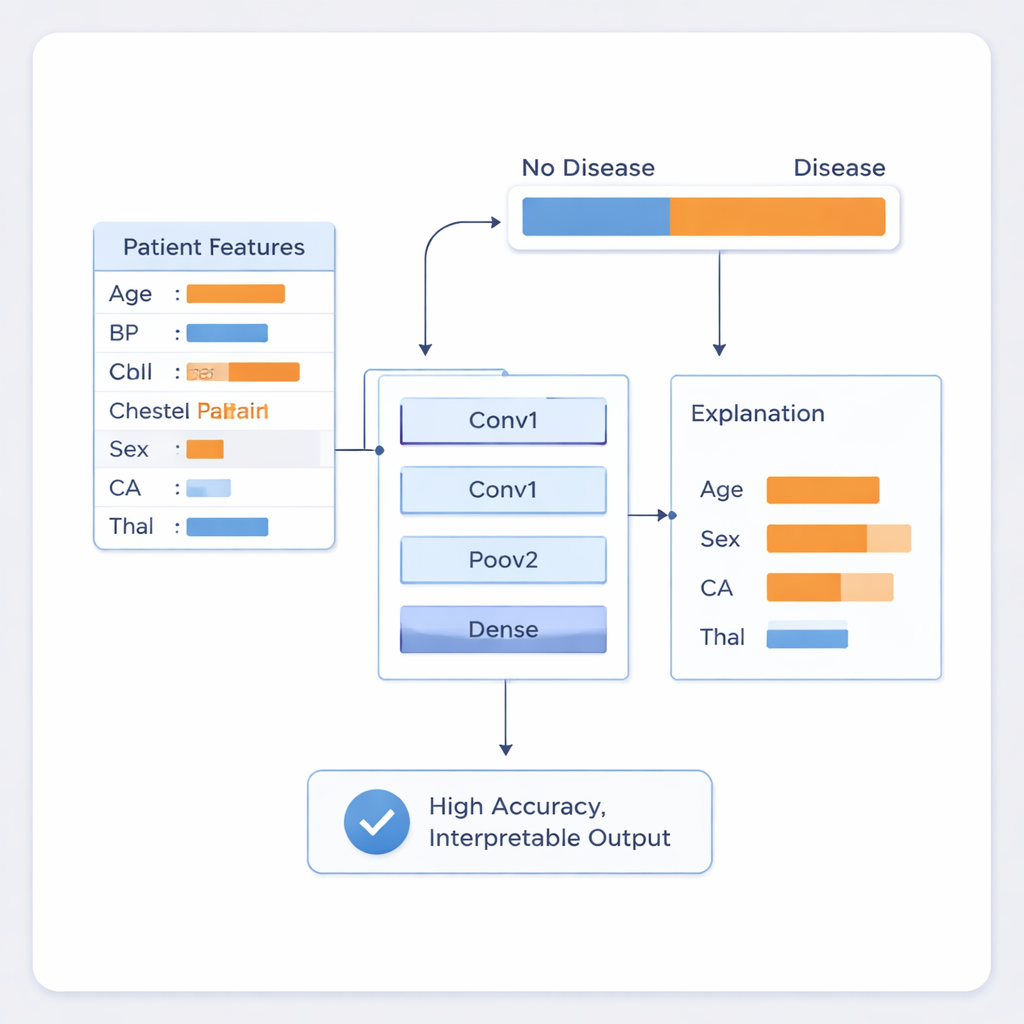
Turning Numbers into Trustworthy Explanations
Performance alone is not enough in a clinical setting, so the authors paired their model with two explanation techniques known as LIME and SHAP. These methods probe the trained network to estimate how much each input factor pushes a prediction toward “disease” or “no disease” for an individual patient. In practice, this means the system can tell a doctor not just that a patient is high‑risk, but also that, for example, their result is driven mainly by a combination of sex, the number of narrowed blood vessels, and a blood disorder called thalassemia. These highlighted features line up with established medical knowledge about heart disease risk, which helps clinicians judge when to trust the model and when to question it.
Results That Could Reach Everyday Clinics
On the test data it had never seen before, the model correctly classified heart disease status in about 98 out of 100 patients, reached perfect precision in labeling disease cases (it produced no false alarms in this sample), and showed near‑perfect ability to separate sick from healthy hearts overall. Equally important, the system was lightweight: it trained in a few minutes on standard cloud hardware and produced answers in a fraction of a second, suggesting it could run on ordinary hospital computers rather than specialized supercomputers. Although the study is based on one historical dataset and will need broader testing across hospitals and populations, it points toward a future in which routine checkup data, combined with transparent AI, can give doctors an extra, trustworthy “second opinion” to catch heart disease earlier, especially in resource‑strained healthcare settings.
Citation: Kehkashan, T., Abdelhaq, M., Al-Shamayleh, A.S. et al. Sustainable and interpretable heart disease prediction: a clinical decision support approach for biomedical healthcare applications. Sci Rep 16, 7213 (2026). https://doi.org/10.1038/s41598-026-37840-0
Keywords: heart disease prediction, explainable AI, clinical decision support, convolutional neural networks, medical data analytics