Clear Sky Science · en
Different metabolic pathways associated with total cortisol exposure and the cortisol time profile: a randomized crossover trial
Why our body’s stress rhythm matters
Cortisol is often called the “stress hormone,” but it is also a daily workhorse that helps control blood sugar, blood pressure, immunity, and energy. People who cannot make cortisol, such as those with Addison’s disease, take hydrocortisone tablets to replace it. Doctors know that both too much cortisol and the wrong timing of doses can harm health. This study asks a simple but important question: do the total amount of cortisol and the pattern in which it appears in the blood leave different chemical “footprints” in the body?
Two ways of giving the same medicine
To explore this, researchers studied 18 adults with primary adrenal insufficiency, all taking similar total daily doses of hydrocortisone. In a randomized crossover trial, each person tried two treatment schedules: three standard tablets spread across the day, and a single dual-release tablet taken once in the morning. The once-daily tablet was designed to give a quick rise in cortisol after breakfast, then a slow, steady fall through the day, more like a natural rhythm. On special 24-hour clinic days, the team carefully measured cortisol in blood at several time points and collected all urine, while meals and activities were kept the same for everyone. 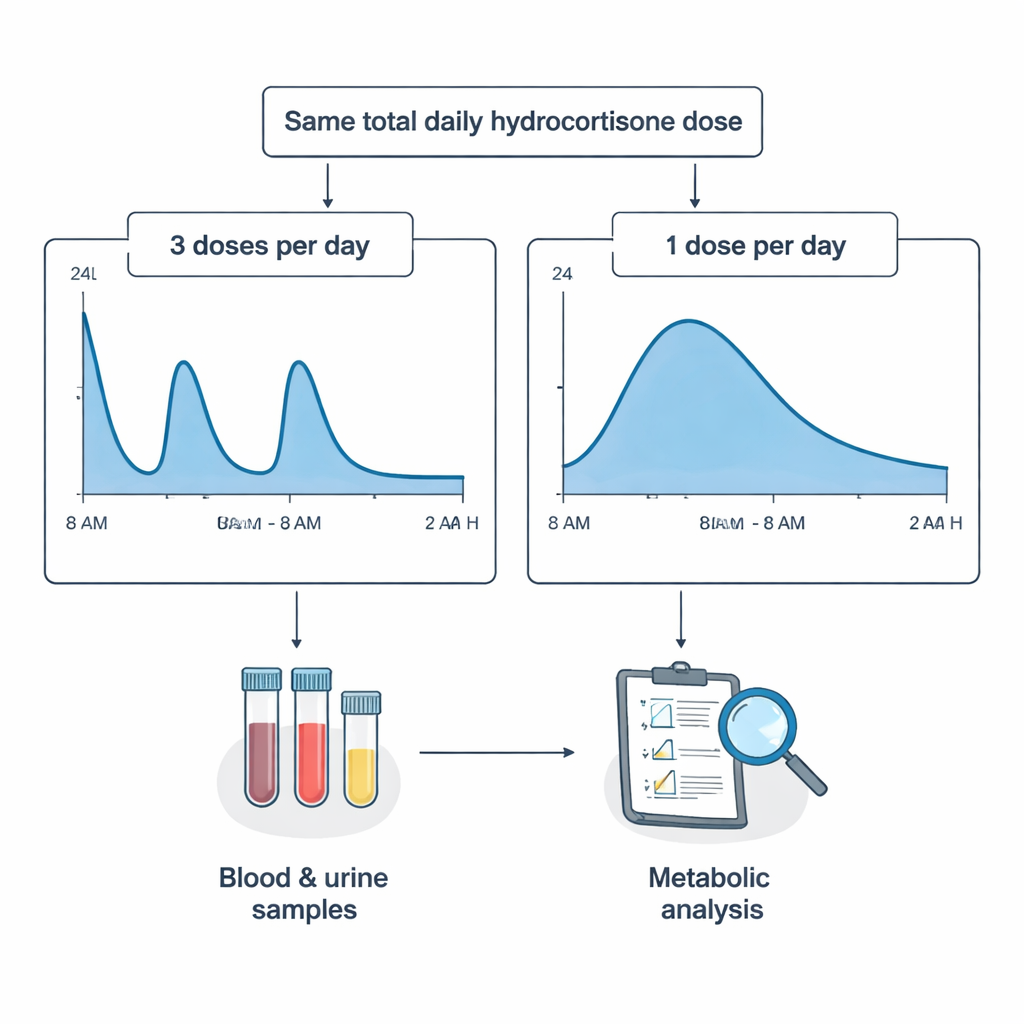
Measuring more than just hormone levels
Rather than looking only at cortisol, the scientists used advanced chemistry tools to scan for thousands of small molecules—metabolites—in blood and urine. These metabolites are the products and intermediates of the body’s metabolism and can reveal how organs are using fuel, responding to inflammation, or processing fats. The researchers quantified two aspects of cortisol: the overall 24-hour exposure (the area under the curve of all cortisol readings) and how smooth or “bumpy” the cortisol curve was over time, using a measure called autocorrelation. A smoother curve meant cortisol rose and fell gently; a bumpier curve meant sharp peaks and drops.
Same dose, different hormone curves
Even though patients took the same total daily dose of hydrocortisone, the two schedules produced different cortisol patterns. The three-times-daily schedule led to about 20% higher total cortisol exposure and more pronounced ups and downs across the day. The once-daily dual-release tablet produced a smoother time profile with lower overall exposure. After the once-daily treatment, patients also tended to have slightly lower body weight, blood pressure, and long-term blood sugar, hinting that the gentler cortisol curve might be kinder to metabolism.
Distinct chemical signatures in the blood
From over 2,400 detected metabolites, hundreds showed links to either the amount of cortisol, its daily rhythm, or both. When the team focused on well-identified compounds, they found that higher total cortisol exposure was tied mainly to pathways handling amino acids and energy. These included arginine (involved in blood vessel tone), tryptophan (linked to mood, immunity, and heart health), and amino acids that feed into the body’s main energy cycle, as well as glycerolipids, which are building blocks of fats. In urine, changes connected to vitamin C–related pathways also tracked with total cortisol. 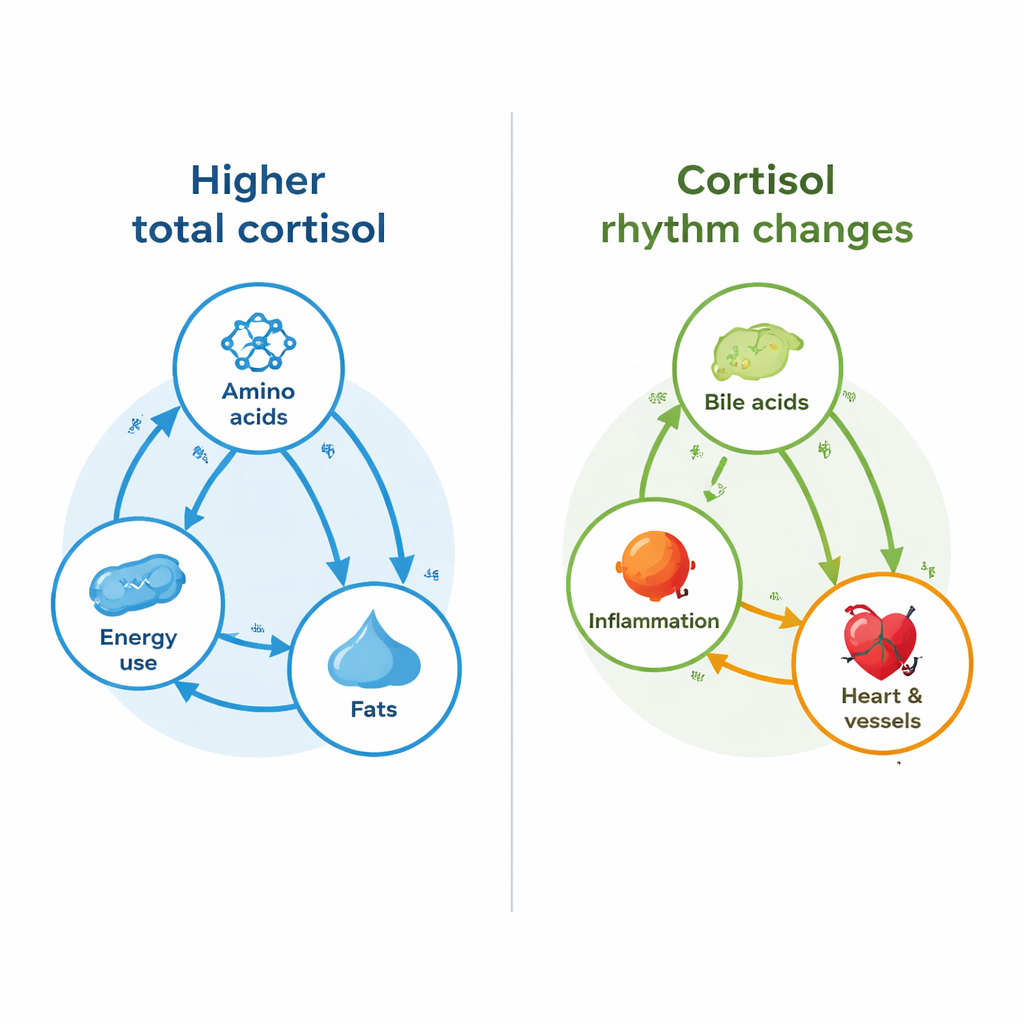
When timing shapes bile, inflammation, and the heart
In contrast, variability in the cortisol time profile was linked to a different set of chemicals. Metabolites connected to bile acid production and to sulfur-containing amino acids such as cysteine and methionine stood out. Bile acids help regulate fat and sugar handling and talk to hormone systems through specialized receptors in the liver and adrenal glands. Cysteine and methionine are involved in antioxidant defenses and cardiovascular risk. In urine, the researchers saw links between cortisol rhythm and molecules such as oleamide and succinic acid, both associated with sleep, brain signaling, and inflammatory responses. Together, these patterns suggest that how smooth or erratic the cortisol rhythm is may influence bile acids, inflammation, and blood vessel health in ways that differ from simply having more or less cortisol overall.
What this means for people on steroid treatment
For people who must take lifelong steroids, this work highlights that the body does not just “see” the total daily dose—it also responds to when and how that dose is delivered. The study shows that overall cortisol exposure and the day-long cortisol rhythm leave different fingerprints in the metabolome, touching energy use, bile acids, inflammation, and cardiovascular pathways in distinct ways. While these findings are exploratory, they point toward a future where doctors may personalize hydrocortisone therapy not only by dose, but also by shaping a healthier daily cortisol pattern, potentially guided by blood and urine markers that reveal how each patient’s body is responding.
Citation: McQueen, J., Garner, T., Chantzichristos, D. et al. Different metabolic pathways associated with total cortisol exposure and the cortisol time profile: a randomized crossover trial. Sci Rep 16, 6510 (2026). https://doi.org/10.1038/s41598-026-37816-0
Keywords: cortisol rhythm, hydrocortisone therapy, adrenal insufficiency, metabolomics, bile acids