Clear Sky Science · en
Professional role and hierarchy shape adherence to electronic alerts for laboratory test ordering
Why this matters for everyday healthcare
Every blood test or lab check you receive uses time, money, and laboratory resources. Many of these tests are vital, but some are repeated too soon to add any new information. This study from hospitals in southern Switzerland looks at a simple digital prompt built into the medical record system that reminds clinicians when a test may be unnecessary—and asks who pays attention to those prompts, how that changes over time, and what it means for smarter, less wasteful care.

A gentle digital nudge at the bedside
The researchers examined an electronic alert built into the hospitals’ ordering software. Whenever a doctor or nurse tried to request a lab test that had been done recently, a full-screen pop-up appeared. It explained that a valid result was already available and suggested not repeating the test yet. Crucially, the alert did not block the order. The prescriber had to make an active choice: cancel the test or go ahead anyway. This kind of design, often called a “nudge,” aims to slow people down just long enough to rethink a routine decision without taking away their freedom to choose.
Nearly a million test orders under the microscope
To see how well this nudge worked, the team analyzed 929,808 lab test orders placed between mid-2021 and early 2024 in a Swiss hospital network. About one in eight orders triggered an alert because the test was being repeated sooner than recommended. In roughly one in nine of those cases, the clinician canceled the order after seeing the warning. On paper, that may sound modest, but across hundreds of thousands of orders it represents a substantial number of avoided, low-value tests—each one a small win for patients’ comfort, lab workloads, and healthcare costs.
Hierarchy and experience shape who listens
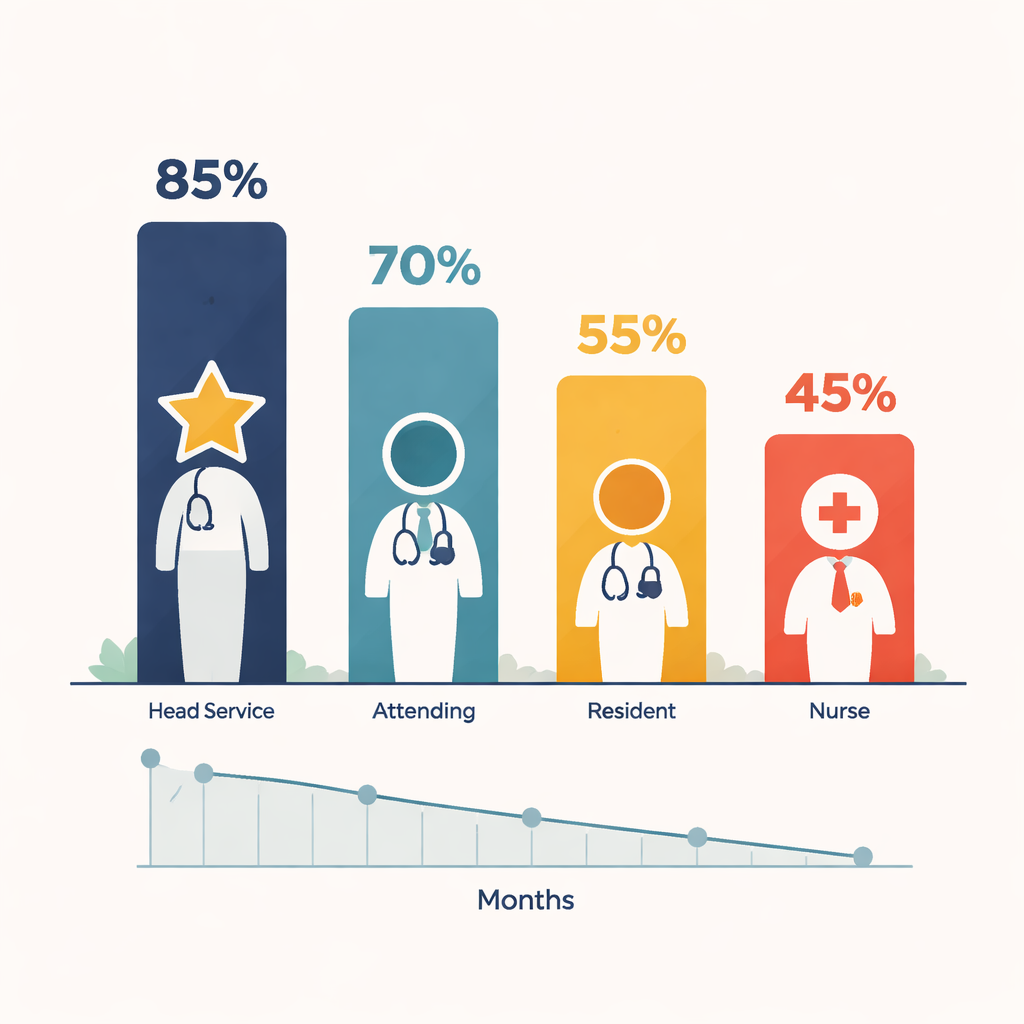
Not all clinicians reacted to the alerts in the same way. Senior doctors who led hospital services were the most likely to follow the warning and cancel unnecessary tests. Residents, at the bottom of the medical hierarchy, were least likely to do so, with attending physicians and nurses in between. Older and more experienced staff were generally more compliant than their younger colleagues, even though younger clinicians are usually more at ease with digital tools. A follow-up survey of over 300 staff members added nuance: nurses tended to see the alerts as genuinely helpful, while many physicians, especially senior ones, found them annoying or unconvincing—even as they were the ones most often changing their behavior.
When helpful prompts turn into background noise
Over the nearly three-year study, the rate at which clinicians accepted alerts declined steadily, a pattern known as “alert fatigue.” When people are bombarded with similar pop-ups day after day, they start clicking past them automatically, even if the message is sound. Interestingly, while acceptance of alerts fell, the overall rate of “appropriate” test ordering—situations where no alert was triggered—did not clearly improve. For some groups, such as residents and department heads, appropriate ordering crept upward; for others, including nurses and attending physicians, it slipped. This suggests that the nudge produced some early gains but struggled to change habits in a lasting way.
Rethinking how we design digital reminders
The authors conclude that simple, one-size-fits-all alerts are not enough to sustain better test ordering over time. Who you are in the hospital—your role, seniority, and confidence—strongly shapes whether you treat an alert as guidance, a prompt to consult a supervisor, or just another interruption. To keep digital nudges effective, the study suggests making them more tailored and context-aware, for example by adjusting how often they fire, how they look, and how specific they are based on the prescriber’s experience and the patient’s situation. For patients and the public, the message is reassuring but realistic: smart use of electronic alerts can cut back on unnecessary blood tests and support higher-value care, but these tools work best when they respect clinicians’ time and judgment and evolve with real-world practice.
Citation: Greco, A., Garo, M.L., Zandonà, M. et al. Professional role and hierarchy shape adherence to electronic alerts for laboratory test ordering. Sci Rep 16, 6669 (2026). https://doi.org/10.1038/s41598-026-37796-1
Keywords: electronic alerts, laboratory testing, nudging, clinical decision support, alert fatigue