Clear Sky Science · en
Human amnion epithelial cell-derived exosomal miR-25-3p enhances mucin expression in conjunctival goblet cells via downregulating BCL2L11
Why a smoother eye surface matters
Anyone who has struggled with dry, scratchy eyes knows how much a healthy tear film matters for clear, comfortable vision. A key part of this protective layer is mucus made by tiny factories called goblet cells that line the white of the eye and the inner eyelids. When these cells are damaged or lost, as in dry eye disease or severe inflammatory conditions, the surface of the eye becomes vulnerable. This study explores an emerging “cell-free” therapy that uses microscopic packages released from donated placental tissue to help goblet cells survive and make more of the mucus that keeps our eyes moist and protected.
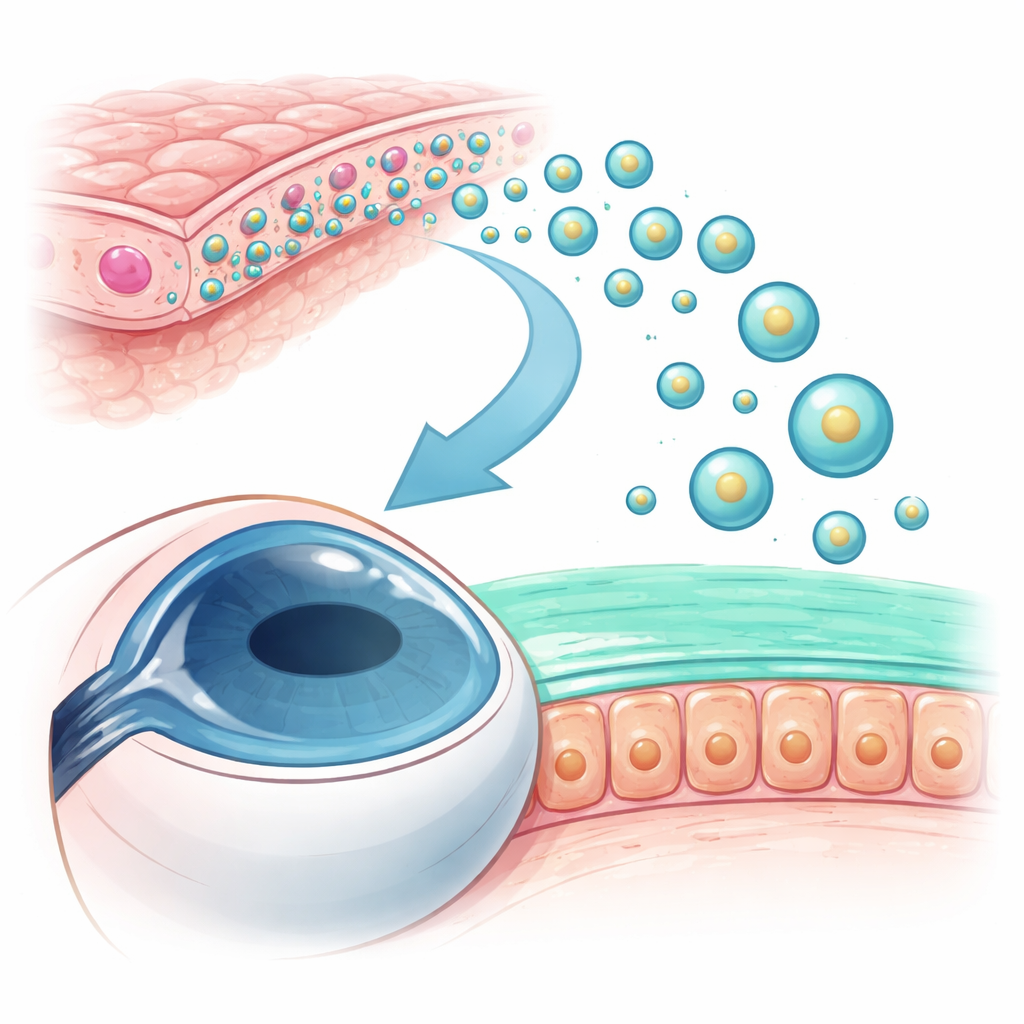
Tiny delivery packets from birth tissue
The researchers focused on human amnion epithelial cells, which come from the thin membrane surrounding a baby during pregnancy and are already known for their wound-healing and anti-inflammatory properties. These cells release nanosized bubbles, called exosomes, that carry proteins and genetic regulators from one cell to another. The team isolated these vesicles from amnion cell cultures, confirmed their typical cup-shaped appearance and size range under an electron microscope, and verified the presence of well-known exosome marker proteins. This characterization step showed that they had obtained a clean preparation of the tiny packets they wanted to test.
A microscopic message to eye surface cells
The next question was whether these exosomes could reach and influence conjunctival goblet cells, the mucus-producing cells that are so important for eye comfort. The scientists labeled the exosomes with a fluorescent dye and added them to human goblet cells grown in dishes. Under the microscope, they saw bright signals inside the cells, especially at higher exosome doses, confirming that goblet cells readily took up these tiny packets. Inside the exosomes, they found a particular small RNA molecule, miR-25-3p, safely tucked away from degrading enzymes, and they showed that blocking exosome production in the source cells sharply reduced the release of this molecule. Together, these tests revealed that miR-25-3p is mainly shipped out within exosomes and can be delivered straight into goblet cells.
Helping mucus factories work better and survive
Once they established this delivery route, the authors examined what happens to goblet cells after they receive amnion-derived exosomes. Cells treated with exosomes produced more of MUC5AC, a major mucus component that forms the slippery, protective coat on the eye’s surface. Measurements of both the protein inside cells and the amount secreted into the surrounding fluid showed a clear, dose-dependent rise. At the same time, fewer goblet cells showed hallmarks of programmed cell death, meaning the treatment helped them survive. When the researchers boosted miR-25-3p directly, these beneficial effects became even stronger, pointing to this small RNA as a key active ingredient inside the exosomes.
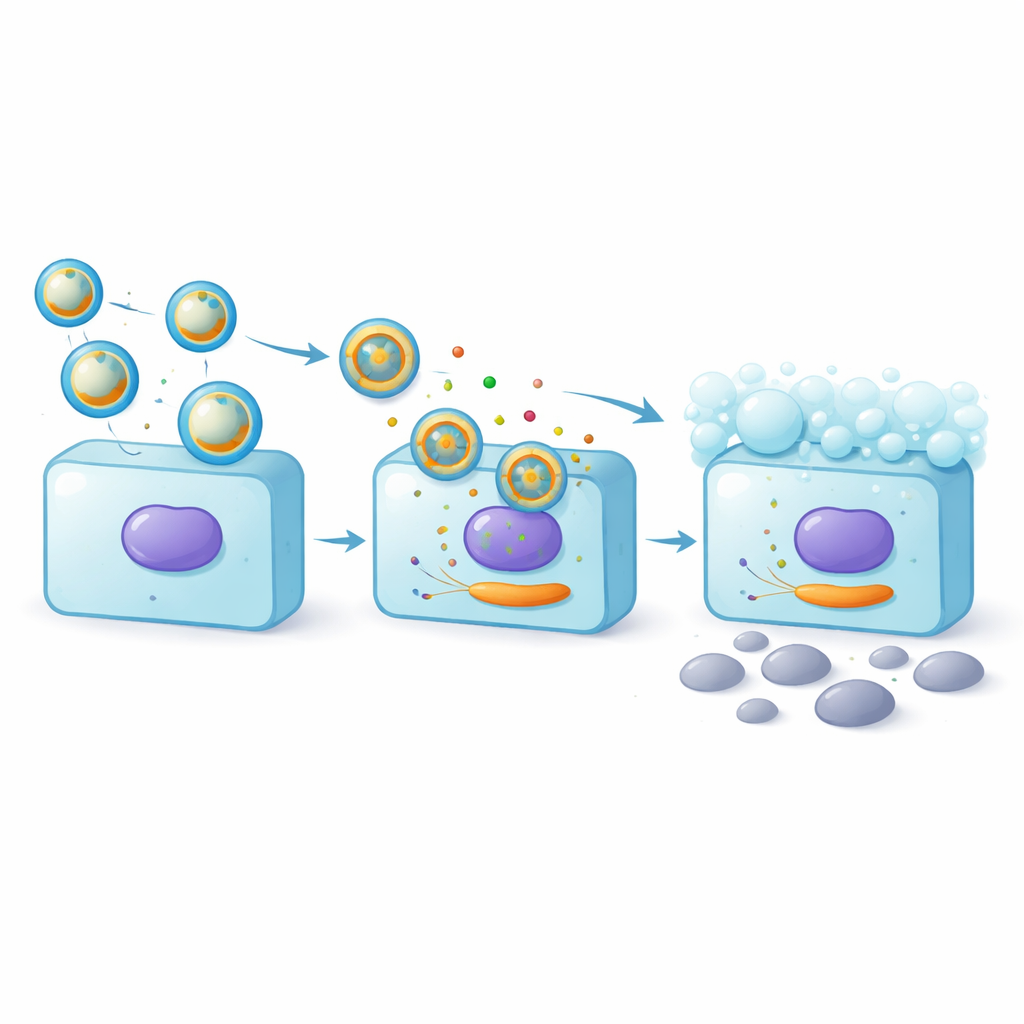
Switching off a cell death trigger
To understand how miR-25-3p protects goblet cells, the team looked for its molecular target and homed in on BCL2L11, a gene that promotes cell death. Using a reporter system, they confirmed that miR-25-3p can bind to BCL2L11’s message inside the cell and dampen its activity. Goblet cells exposed to amnion exosomes showed lower levels of BCL2L11, especially when the exosomes were enriched in miR-25-3p. When the researchers artificially ramped up BCL2L11, some of the protective effects of miR-25-3p were lost: cell death increased again and mucus production dropped. This tug-of-war demonstrated that a major part of the exosomes’ benefit comes from miR-25-3p turning down BCL2L11 and thereby supporting both goblet cell survival and mucus output.
What this could mean for people with dry eyes
In simple terms, this study shows that microscopic packets released from donated birth tissue can deliver a protective genetic message to the eye’s mucus-producing cells. That message, carried by miR-25-3p, helps shut off a built-in self-destruct switch and encourages goblet cells to make more of the mucus that keeps the eye surface smooth and defended. Although these experiments were done in laboratory dishes and more work in animal models and patients is needed, the findings outline a promising cell-free strategy: using purified exosomes rather than whole cells to restore a healthy tear film and possibly ease diseases where the eye surface becomes dry, inflamed, and fragile.
Citation: Zhang, Y., Wu, W., Meng, T. et al. Human amnion epithelial cell-derived exosomal miR-25-3p enhances mucin expression in conjunctival goblet cells via downregulating BCL2L11. Sci Rep 16, 7958 (2026). https://doi.org/10.1038/s41598-026-37794-3
Keywords: dry eye disease, tear film mucus, exosomes, ocular surface therapy, goblet cells