Clear Sky Science · en
Explainable multi-modal approach for uncovering key predictors of stroke-risk from ECG, EMG, blood pressure, and respiratory signals
Why breathing and heart signals matter for stroke
Stroke strikes fast but usually develops silently over years. Doctors know that high blood pressure, heart rhythm problems, and lifestyle habits raise risk, yet predicting who is in real danger remains difficult. This study shows that how we breathe – especially how our bodies handle carbon dioxide – carries hidden clues about stroke risk. By combining breathing, heart, muscle, and blood pressure signals in an explainable artificial intelligence (AI) model, the authors reveal new ways to spot high‑risk patients and help clinicians understand why an algorithm makes its call.
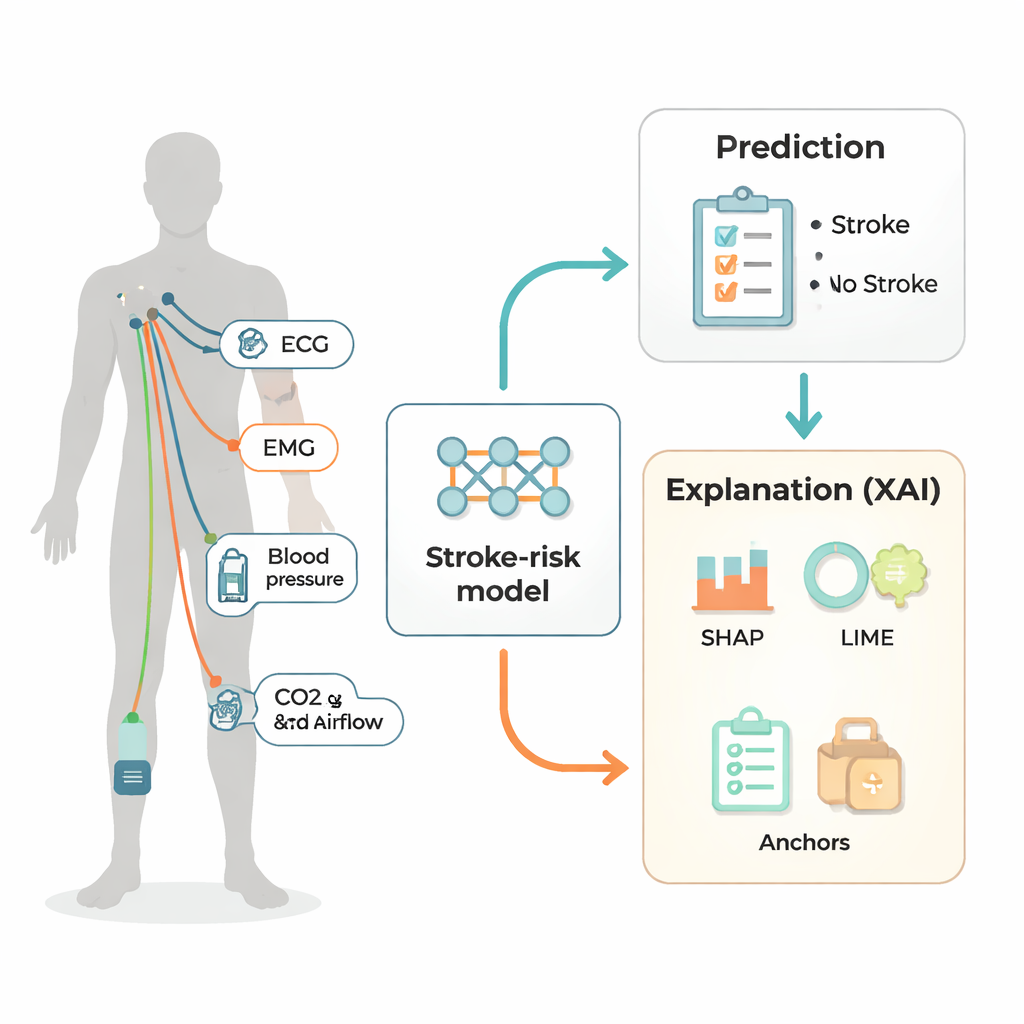
Listening to the body’s quiet signals
Instead of using brain scans, which are expensive and not suited to continuous monitoring, the researchers turned to simple electrical and pressure measurements taken from 64 volunteers, some who had suffered an ischemic stroke and some who had not. They recorded seven signals while people sat and then stood: heart activity (two ECG channels), leg muscle activity (two EMG channels), blood pressure from a finger cuff, and two breathing signals at the mouth – carbon dioxide in exhaled air and the rate of airflow. These measurements are similar to those that could be collected by hospital bedside monitors or advanced wearables, making the approach potentially practical for regular check‑ups.
Turning raw waves into patterns the computer can read
The team chopped each person’s 10‑minute recording into many 14‑second slices that partly overlapped, enough time to capture several breaths and repeated heartbeats. For every slice, they calculated a wide range of simple numerical descriptors – averages, variability, how often the signals crossed zero, and how their energy was spread across different frequencies. These features summarize the “style” of each signal without storing the full waveforms, reducing computing cost and noise. All features from the seven signals were then stacked together to represent a single sample of how that person’s body was behaving in that brief period.
A simple brain‑inspired model that outperforms deeper networks
Rather than using a deep, complex neural network, the authors chose a very simple one: a single‑layer perceptron. This model takes all the numeric features, multiplies each by a learned weight, adds them up, and passes the result through a squashing function to produce a probability of “stroke” or “no stroke.” Despite its simplicity, this model reached an accuracy of about 85–88 percent, beating more sophisticated methods such as recurrent and convolutional neural networks, ensemble echo state networks, and popular machine‑learning classifiers when all were tested on the same data. Crucially, when the respiratory signals (carbon dioxide and airflow) were removed, accuracy dropped to around 59 percent, a statistically significant decline, showing that breathing data adds critical information that other signals alone do not capture.
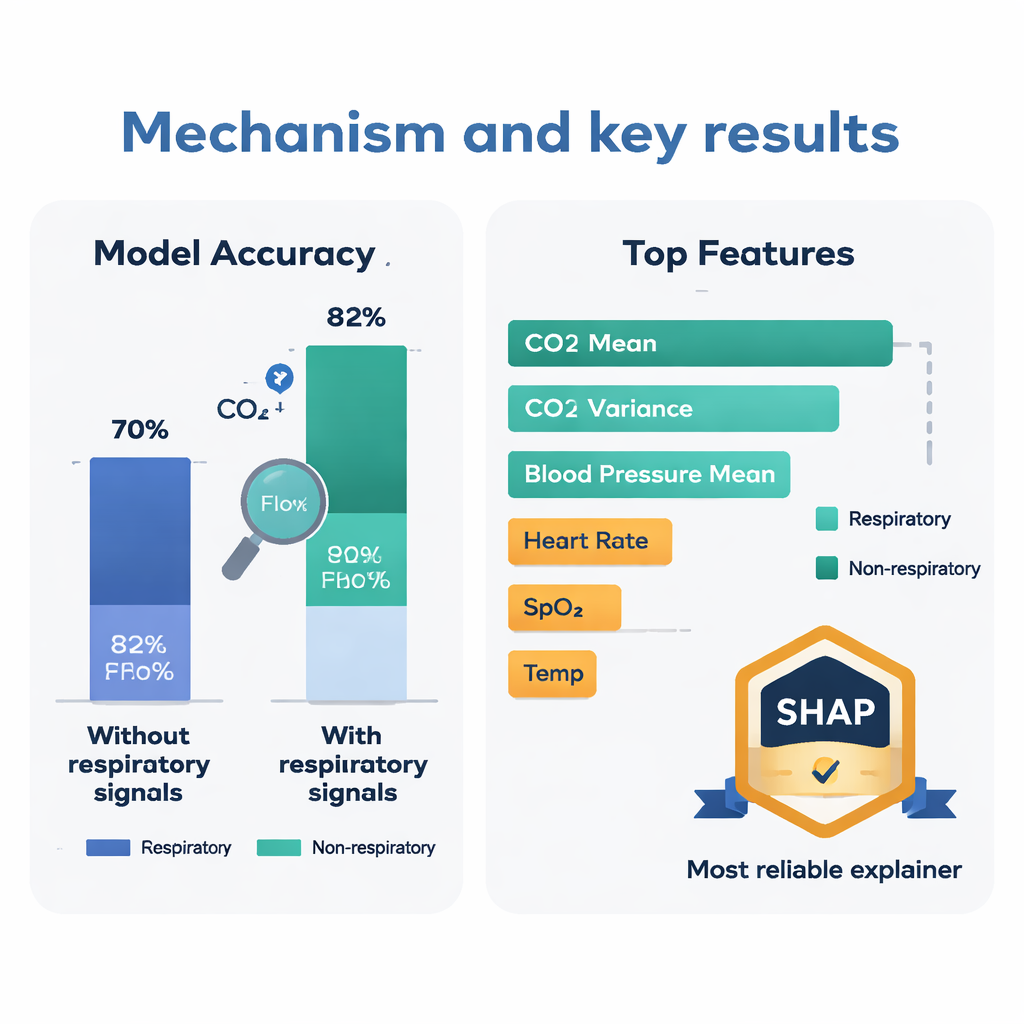
Opening the black box: which signals truly matter
Doctors are rightfully wary of black‑box AI, so the team used three explanation tools – SHAP, LIME, and Anchors – to see which features the model relied on most. All three pointed to respiratory features, especially those derived from carbon dioxide, as key drivers of predictions. SHAP, a game‑theory‑based explainer, ranked the average level of exhaled carbon dioxide, its variability, and the average blood pressure as the top three contributors to deciding whether a sample looked like it came from a stroke patient. High average carbon dioxide and high blood pressure tended to push the model toward “stroke,” while more irregular carbon dioxide patterns suggested lower risk. To judge which explainer to trust most, the authors used a special test: removing the top features each method named and seeing how much model performance worsened. SHAP caused the largest drop, earning it the title of most reliable interpreter.
What this means for patients and clinicians
For non‑experts, the takeaway is straightforward: how you breathe and clear carbon dioxide may be as telling about stroke risk as your blood pressure or heartbeat. This work suggests that routine monitors capturing respiratory gases, blood pressure, heart, and muscle signals could be linked to simple, transparent AI to flag people who deserve closer attention long before a stroke occurs. Because the model is both accurate and explainable, clinicians can see which aspects of a patient’s physiology are driving the risk estimate, supporting trust and targeted treatment. Larger studies are still needed, but the results highlight carbon dioxide‑related breathing measures as promising new markers for stroke prevention.
Citation: Krayem, J., Wong, L., Tham, L.K. et al. Explainable multi-modal approach for uncovering key predictors of stroke-risk from ECG, EMG, blood pressure, and respiratory signals. Sci Rep 16, 6906 (2026). https://doi.org/10.1038/s41598-026-37777-4
Keywords: stroke risk, respiratory signals, carbon dioxide, explainable AI, ECG and blood pressure