Clear Sky Science · en
Self-care behaviors among Iranian adults with non-alcoholic fatty liver disease based on the health belief model and structural equation modeling
Why beliefs matter for a silent liver disease
Non-alcoholic fatty liver disease (NAFLD) is a quiet but growing health problem, linked to extra fat building up in the liver of people who drink little or no alcohol. It is now one of the most common chronic liver conditions worldwide, including in Iran, where about one in three adults is affected. Because there is no simple pill to cure NAFLD, daily habits such as eating patterns, physical activity, weight control, and following medical advice become the main tools for staying healthy. This study asks a deceptively simple question: what makes some people with NAFLD actually follow these self-care steps, while others do not?
Looking at illness through the lens of everyday beliefs
The researchers used a well-known psychology framework called the Health Belief Model to explore how people’s beliefs shape their health actions. They surveyed 513 adults with NAFLD at a major clinic in Shiraz, Iran, asking about their age, education, income, family history, and other health conditions, as well as their knowledge and beliefs about NAFLD. These beliefs included how at risk they felt, how serious they thought the disease was, what benefits they saw in changing their lifestyle, what obstacles they perceived, and how confident they felt about carrying out self-care. The team also measured how often people reported doing recommended behaviors such as healthier eating, being physically active, managing their weight, and following medical advice.
Connecting the dots with a big-picture statistical map
Instead of looking at one belief at a time, the scientists used a technique called structural equation modeling, which allows many relationships to be examined together in a single "map." This approach tested how the different beliefs related to each other and to self-care, while also taking into account age, education, income, body weight, family history, and how often participants saw a doctor. The statistical model fit the data well and showed that the belief measures were reliable and distinct—suggesting that the questionnaire captured real differences in how people thought about their illness and their ability to manage it.
Feeling at risk and feeling capable drive action
The analysis revealed that two beliefs stood out as especially important for better self-care. People who felt more personally at risk for NAFLD complications (higher perceived susceptibility) and those who believed they could successfully stick to healthy routines (higher self-efficacy) reported more consistent self-care behaviors. By contrast, people who saw more obstacles—such as cost, time, or lack of support—were less likely to follow through. Together, these beliefs explained almost half of the differences in self-care behavior between individuals, a large amount for this kind of research. Awareness, belief in the benefits of self-care, and viewing the disease as serious also nudged people toward healthier actions, though their effects were smaller.
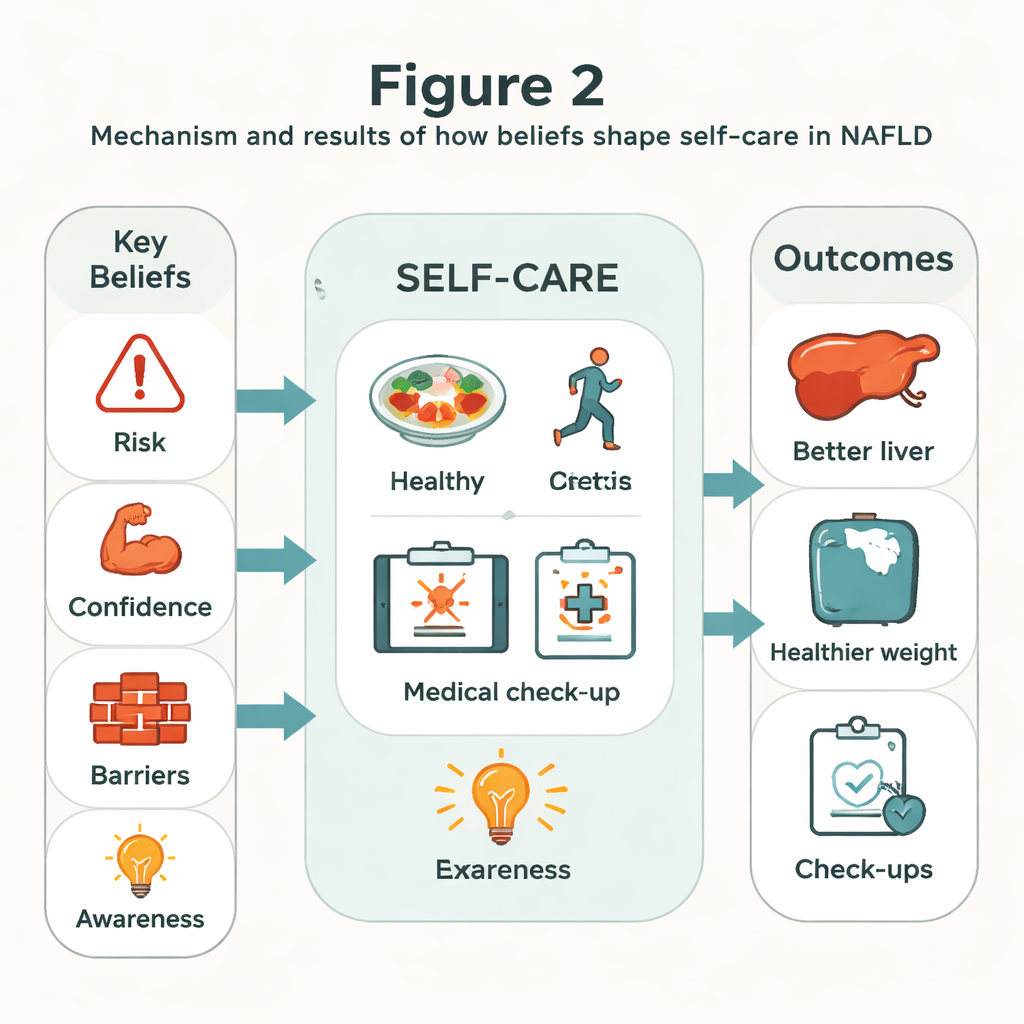
How background and life circumstances shape beliefs
Personal and social factors mattered too, but mostly through their impact on beliefs. Younger adults tended to feel more at risk than older ones. People with higher education levels were more confident about managing their condition, and those with higher incomes reported fewer barriers, such as difficulty affording healthy food or medical visits. Having a family history of liver disease was linked to stronger feelings of vulnerability. Regular doctor visits were tied to higher awareness and confidence. In the model, some of these background factors influenced self-care indirectly: for example, education boosted confidence, which in turn increased self-care, while low income raised perceived barriers, which dampened healthy behavior.
What this means for patients and health systems
For a layperson, the takeaway is clear: in NAFLD, what you believe about your risk and your own ability to act can be just as important as the information you receive. The study suggests that effective programs should do more than simply hand out diet sheets or exercise tips. Health workers may get better results by helping patients understand their personal risk, building step-by-step confidence through practical goals, and tackling real-world barriers such as cost, access, and time. Tailored education—delivered in clinics, groups, or through digital tools and family support—could make it easier for people to turn knowledge into daily habits. By working with people’s beliefs as well as their biology, such approaches may improve long-term liver health and reduce the growing burden of NAFLD.
Citation: Izadpanah, P., Ansarizadeh, M., Dahi, A.A. et al. Self-care behaviors among Iranian adults with non-alcoholic fatty liver disease based on the health belief model and structural equation modeling. Sci Rep 16, 7012 (2026). https://doi.org/10.1038/s41598-026-37661-1
Keywords: fatty liver disease, self-care, health beliefs, lifestyle change, patient education