Clear Sky Science · en
Longitudinal modeling of Post-COVID-19 condition over three years: A machine learning approach using clinical, neuropsychological, and fluid markers
Why lingering COVID symptoms still matter
Millions of people around the world continue to feel unwell months or even years after catching COVID‑19. This condition, often called long COVID or Post‑COVID‑19 Condition, can bring crushing fatigue, “brain fog,” sleep problems, and other symptoms that are hard to pin down with standard medical tests. The study described here followed a group of adults for three years after infection and used modern computer techniques to search their blood, clinical check‑ups, and thinking‑skills tests for patterns that reveal how long COVID changes over time and which measures best track recovery or ongoing illness.
Following patients over the long haul
Researchers in Germany enrolled 93 adults who had confirmed SARS‑CoV‑2 infection and persistent neurological or neuropsychological complaints. These participants, most in mid‑life, were examined four times: roughly 6, 14, 23, and 38 months after their initial infection. At each visit, they completed detailed questionnaires about fatigue, mood, and sleep; underwent brief and more extensive tests of attention, memory, and mental speed; and gave blood samples for a broad panel of laboratory measurements. These included standard markers of health, signals of inflammation, immune system activity, and specialized proteins released when brain cells are injured.
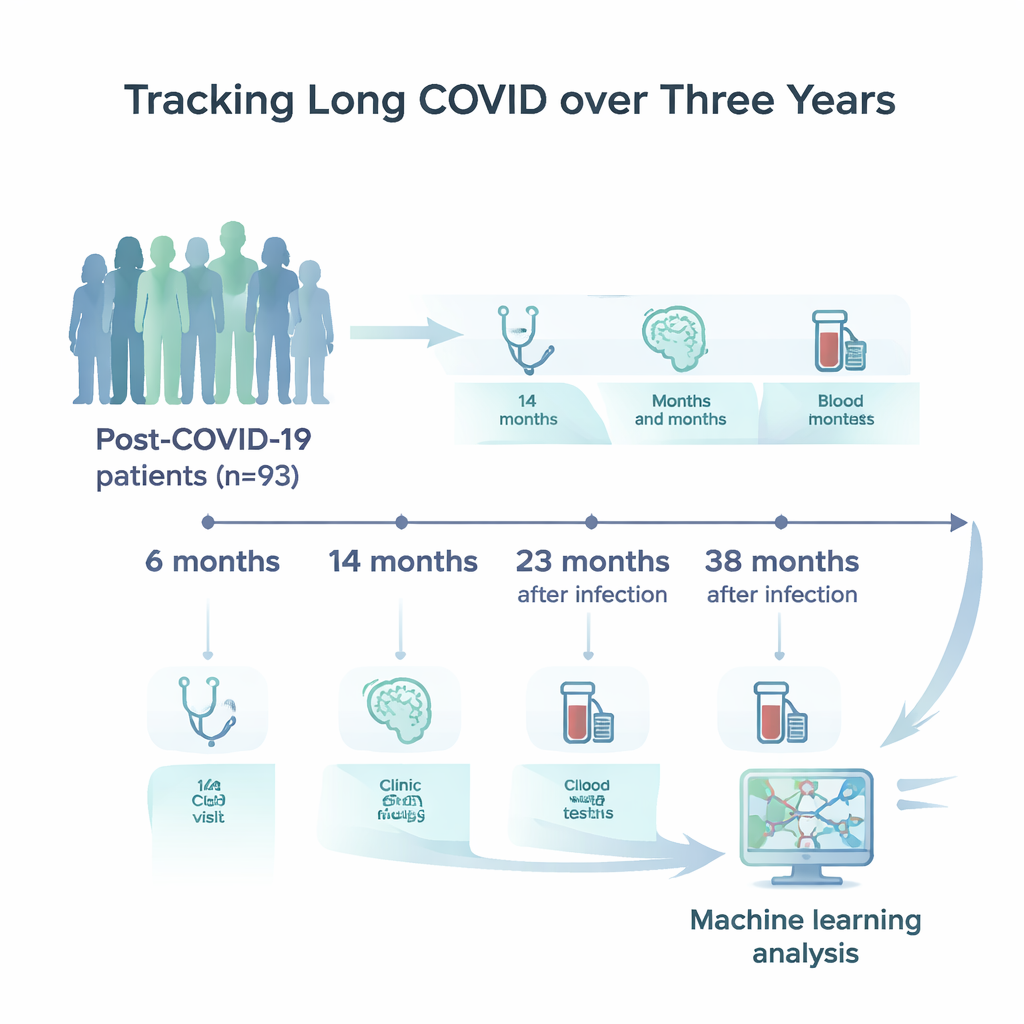
Letting computers find hidden patterns
Instead of looking at one symptom or blood test at a time, the team turned to machine learning, a branch of artificial intelligence that can sift through many variables at once and spot subtle relationships. They trained a range of computer models to answer a specific question: given the combined data from one clinic visit, can the algorithm determine which follow‑up year that visit came from? In other words, does a person’s overall profile at 6 months look measurably different from their profile at 2 or 3 years? The researchers carefully handled missing values, used cross‑validation to avoid over‑fitting to a small sample, and compared different families of models, from simple decision trees to sophisticated gradient‑boosting methods.
Which signals tell time best
The models performed strikingly well. When comparing visits that were farther apart in time—such as the first and fourth visits—some algorithms correctly assigned the year in well over 90 percent of cases. Even between closer timepoints, accuracy remained high, only dipping somewhat between the third and fourth visits, suggesting that patients’ profiles change more slowly at later stages. The best‑performing methods were tree‑based gradient boosting models, which excel at finding non‑linear patterns. To open the “black box” and see what drove these decisions, the team used explainability tools called SHAP and LIME that rank which features push a prediction in one direction or another.
Immune clues, brain fog, and shifting importance
Across multiple analyses, a consistent picture emerged. Levels of inflammatory molecules in the blood—especially certain interleukins such as IL‑2, IL‑8, and IL‑10—were among the strongest clues separating earlier from later follow‑ups. Measures of the body’s antibody response to the virus, particularly antibodies targeting the spike protein (which also reflect vaccination over time), were also powerful indicators. On the cognitive side, tests of verbal memory and word‑finding, along with scores related to fatigue and sleepiness, contributed important information, especially in the earlier stages after infection. As time went on, immune markers tended to gain weight in the models, while some of the neuropsychological measures became less central, hinting that the biological drivers of long COVID may evolve over the years.
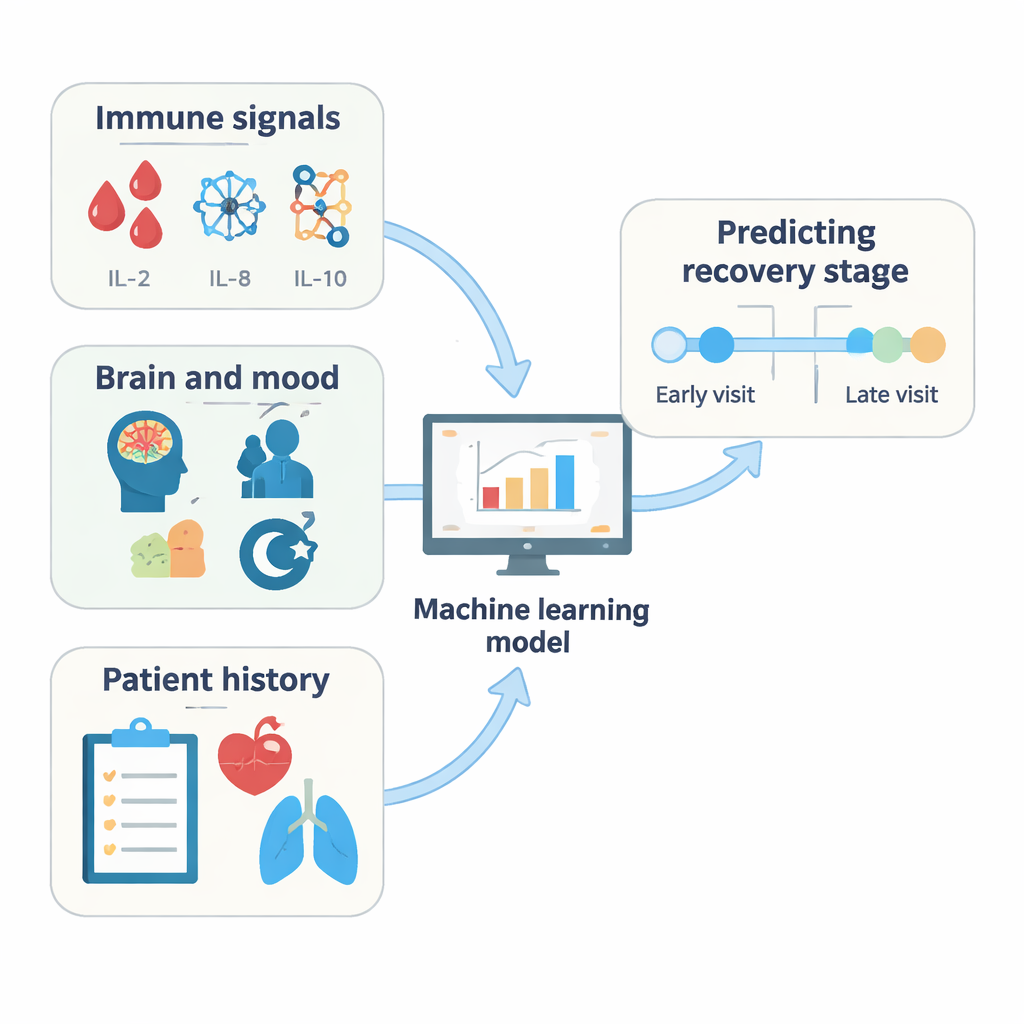
What this means for patients and care
For non‑specialists, the key message is that long COVID is not just a vague collection of complaints. When tracked carefully over several years, objective signals in the blood and in thinking‑skills tests change in ways that computers can reliably recognize. This study suggests that a combination of immune markers, antibody levels, and targeted cognitive and fatigue assessments could help doctors monitor who is recovering, who remains at risk for lasting problems, and which patients might benefit most from emerging treatments that focus on the immune system. While more and larger studies are needed before these tools reach routine practice, the work shows how artificial intelligence can help turn the messy reality of long COVID into clearer, more actionable information for patients and clinicians.
Citation: Walders, J., Wetz, S., Costa, A.S. et al. Longitudinal modeling of Post-COVID-19 condition over three years: A machine learning approach using clinical, neuropsychological, and fluid markers. Sci Rep 16, 6517 (2026). https://doi.org/10.1038/s41598-026-37635-3
Keywords: long COVID, machine learning, inflammation, cognitive symptoms, immune biomarkers