Clear Sky Science · en
Neurotransmitter alterations in seasonal affective disorder
Why winter mood swings matter
Many people feel their mood dip when the days grow short and gray, but for some, winter brings a full-blown depression known as seasonal affective disorder (SAD). This study looks inside the brain to see how chemical messengers differ in people with SAD compared with healthy individuals during the dark months. By focusing on key brain chemicals beyond the well-known serotonin, the researchers aim to better understand why winter hits some people so much harder—and what that might mean for future treatments.
The brain’s seasonal slowdown
SAD is a recurring form of major depression that appears in fall and winter and lifts in spring and summer. It is closely linked to reduced daylight and is often treated with bright light therapy, which can be highly effective. For decades, most explanations for SAD have centered on serotonin, a brain chemical involved in mood. Studies have shown that brain serotonin systems change with the seasons and respond to light-based treatments. But serotonin does not act alone. Two other major brain messengers—GABA, which generally calms brain activity, and glutamate, which usually excites it—interact closely with serotonin and may also shape how our mood responds to changing seasons.
Zooming in on winter brains
To probe these other brain chemicals, the team scanned the brains of 14 adults with SAD and 14 healthy people of similar age and sex, all during the fall or winter, when symptoms are strongest. They used a non-invasive method called magnetic resonance spectroscopy imaging, which can estimate levels of certain chemicals in specific brain regions. The researchers focused on five areas, including the hippocampus, a structure deep in the brain that is crucial for memory, emotion, and the flexibility of brain connections. Instead of measuring absolute amounts, they looked at the ratio of GABA and glutamate-related signals to a more stable reference signal from another molecule, creatine.
A key calming signal runs low
The main difference the researchers found between the two groups was in the hippocampus. People with SAD showed significantly lower levels of GABA relative to creatine in this region compared with healthy participants. In contrast, there were no clear differences in glutamate-related measures or in the other brain regions examined. The drop in GABA did not neatly track with how severe people’s symptoms were on standard depression and seasonality questionnaires, which may reflect the small sample size or the fact that overall mood likely depends on broader brain networks rather than a single region.
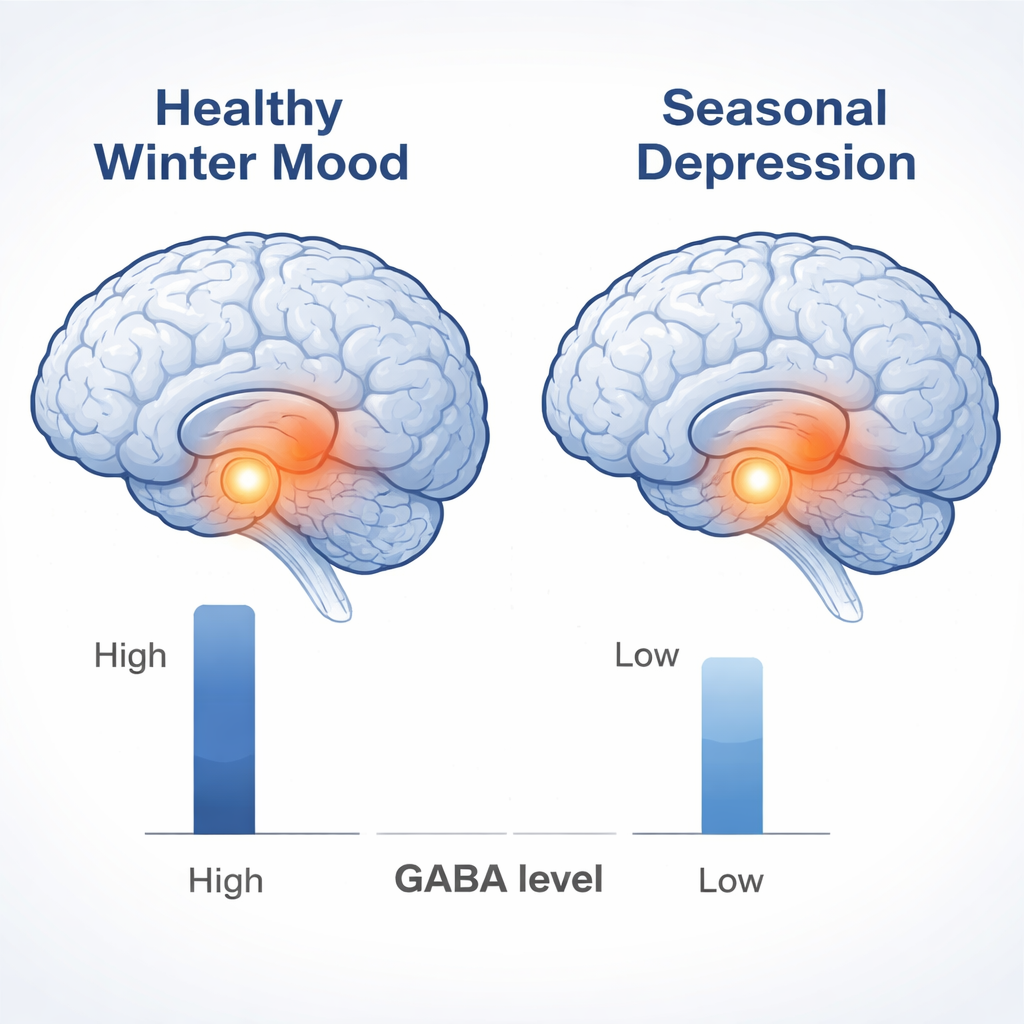
What this means for depression and treatment
The hippocampus has long been implicated in major depression, with prior work showing altered connections, chemical changes, and even structural differences in this region. Reduced GABA here has been linked to problems with memory and the brain’s ability to adapt and reorganize. The finding that SAD shares a similar pattern of lower hippocampal GABA with other types of depression suggests there may be common biological threads running through different depressive disorders, even though treatments differ. While standard antidepressants tend to target serotonin directly and are first-line treatment for non-seasonal depression, SAD is most often treated with bright light therapy, which appears to act through light-sensitive pathways and seasonal biology.
Looking ahead: shedding light on winter blues
For a layperson, the takeaway is that SAD is not just about “feeling down in winter” or simply a lack of willpower. This study adds evidence that brain chemistry—specifically lower levels of a calming signal in the hippocampus—differs in people with seasonal depression. Although the work involved a modest number of participants and cannot yet explain exactly how these changes cause symptoms, it strengthens the idea that environmental factors like daylight and deep brain chemistry are tightly intertwined. Understanding these shared mechanisms across depression types may eventually help tailor treatments more precisely, combining light-based approaches, medications, or other therapies to better support people whose moods darken with the season.
Citation: Spurny-Dworak, B., Dörl, G., Stöhrmann, P. et al. Neurotransmitter alterations in seasonal affective disorder. Sci Rep 16, 6683 (2026). https://doi.org/10.1038/s41598-026-37634-4
Keywords: seasonal affective disorder, winter depression, brain chemistry, GABA, hippocampus