Clear Sky Science · en
Bronchial artery infusion of PD-1 inhibitors plus chemotherapy improves progression-free survival in advanced NSCLC: a prospective cohort study
Why this new lung cancer approach matters
For many people with advanced lung cancer, modern immunotherapy drugs have brought new hope—but they do not work for everyone and can cause serious side effects. This study explores a different way to deliver a widely used type of immunotherapy, called PD-1 inhibitors, by sending the drug straight into the arteries that feed the lung tumor instead of through a standard vein in the arm. The researchers asked a simple but important question: can more precise delivery make treatment work better without making it more dangerous?
A closer look at a common cancer
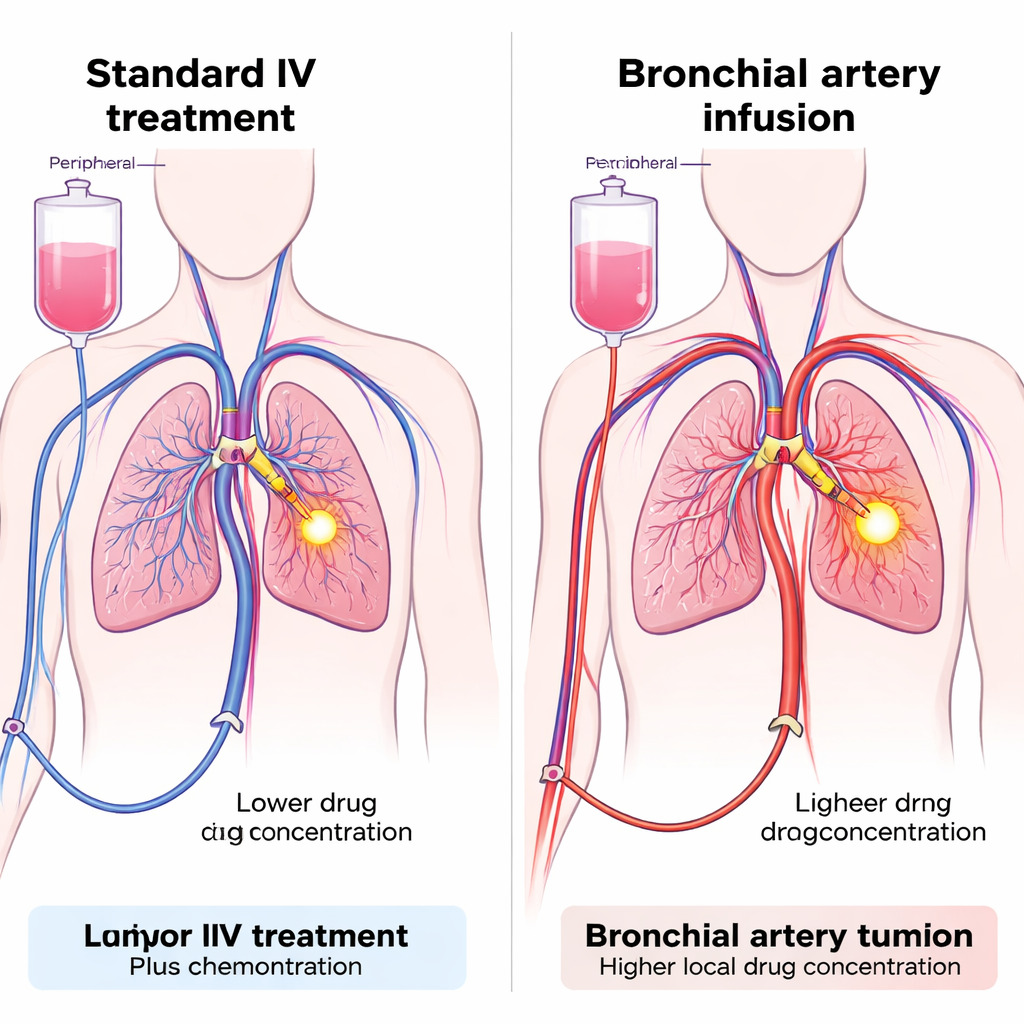
Non-small cell lung cancer (NSCLC) is the most common form of lung cancer and a leading cause of cancer death worldwide. Drugs that block PD-1, a braking signal on immune cells, can help the body’s defenses recognize and attack tumor cells. These medicines, often combined with chemotherapy, are now standard care for advanced NSCLC. Yet many patients still see their disease worsen despite treatment, and some develop immune-related complications such as lung inflammation, liver problems, or skin reactions. One reason may be that, when given through a vein, the drug spreads throughout the body, so the amount that actually reaches the tumor can be lower than ideal while the rest of the body is exposed to the full dose.
Delivering drugs straight to the tumor’s blood supply
The team tested a technique called bronchial artery infusion (BAI), which uses tiny catheters threaded through an artery in the leg to reach the arteries feeding the lung tumor. Once in place, both chemotherapy and the PD-1 inhibitor can be injected directly into those vessels, bathing the tumor area in a high local dose while limiting how much spills into the rest of the circulation. BAI is already used in some hospitals to deliver chemotherapy for difficult lung tumors, but using it to give immunotherapy is new. The researchers designed a prospective cohort study of 47 patients with advanced NSCLC who had not responded well to standard first-line treatment. All patients received chemotherapy by BAI; the key difference was how the PD-1 inhibitor was given—either through the tumor-feeding arteries (BAI group) or by the usual intravenous route (Venous group).
Better tumor control with targeted delivery
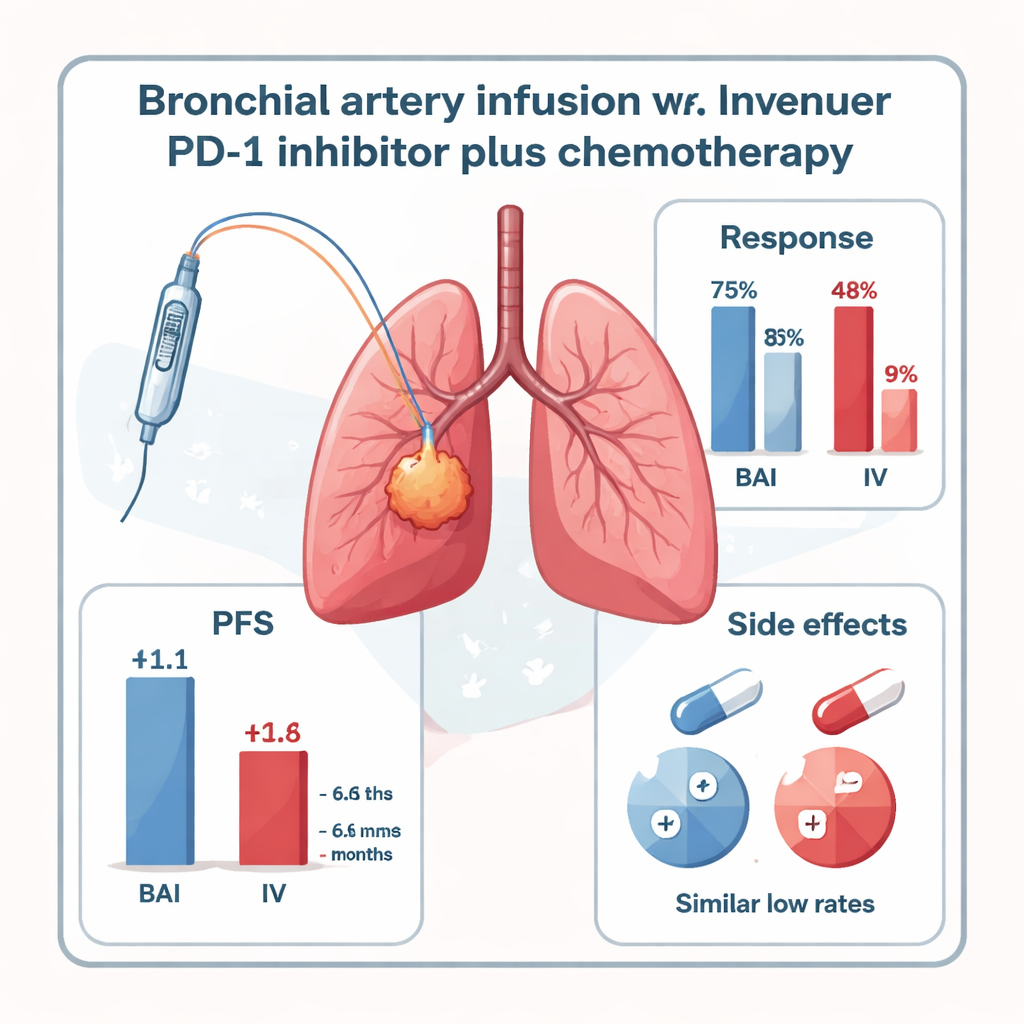
When the patients were checked at six months, those who received the PD-1 inhibitor through BAI had noticeably better disease control. Nearly half of the BAI group (47.8%) saw their tumors shrink enough to meet formal response criteria, compared with only 16.7% in the standard intravenous group. When stable disease was included, 73.9% of BAI patients had their cancer controlled, versus 41.6% in the venous group. The time before the cancer started growing again—known as progression-free survival—was also longer with BAI: a median of 11.1 months compared with 6.6 months for intravenous treatment. Overall survival showed a trend in favor of BAI (17.9 vs. 15.2 months), though the study was too small for this difference to be clearly proven.
Safety and limits of the study
Importantly for patients and doctors, sending the PD-1 inhibitor directly into the bronchial arteries did not appear to make treatment more dangerous. No severe (grade 3–4) treatment-related side effects were seen in either group. Mild to moderate immune-related lung inflammation (pneumonitis) occurred at similar low rates in both groups, and other side effects such as nausea, brief heart rhythm changes, or thyroid problems were uncommon and manageable with supportive care. However, the study has limits: it involved only 47 patients at a single center, was not randomized, and mostly included a specific type of centrally located squamous lung cancer with clearly visible feeding arteries. Larger, more diverse trials are needed to confirm whether these results hold up.
What this could mean for future lung cancer care
To a layperson, the message is that how a drug is delivered can be almost as important as which drug is chosen. By steering immunotherapy directly into the blood vessels that nourish a lung tumor, doctors in this study appeared to keep the cancer in check for longer without adding serious risks. While this approach is still experimental and requires specialized equipment and expertise, it points toward a future where cancer treatment is not only targeted at the molecular level, but also at the level of blood flow and anatomy. If confirmed in larger randomized trials, bronchial artery infusion of immunotherapy could become a valuable option for patients whose advanced lung cancer has stopped responding to standard treatment.
Citation: Liu, B., Zhou, J., He, W. et al. Bronchial artery infusion of PD-1 inhibitors plus chemotherapy improves progression-free survival in advanced NSCLC: a prospective cohort study. Sci Rep 16, 7067 (2026). https://doi.org/10.1038/s41598-026-37607-7
Keywords: non-small cell lung cancer, immunotherapy, PD-1 inhibitor, bronchial artery infusion, targeted drug delivery