Clear Sky Science · en
Classification of paroxysmal atrial fibrillation using sinus rhythm electrocardiograms using the symmetric projection attractor reconstruction method
Why this heart rhythm study matters
Atrial fibrillation is a common heart rhythm problem that can quietly increase a person’s risk of stroke and early death. One puzzling form, called paroxysmal atrial fibrillation, comes and goes in short bursts, so people can have a perfectly normal‑looking heart tracing when they see their doctor. This study asks a provocative question: even when the electrocardiogram (ECG) looks normal, does it still carry a subtle fingerprint of hidden rhythm trouble that computers can detect—and could that spare patients weeks of uncomfortable heart monitoring?
Hidden clues in an everyday heart test
Doctors usually diagnose atrial fibrillation by catching an episode on an ECG that records the heart’s electrical activity. For people whose episodes are brief and infrequent, standard tests—and even 30‑day portable monitors—often miss the problem. The researchers behind this work explored whether a short, 10‑second ECG taken while the heart is beating normally could still reveal who has a history of paroxysmal atrial fibrillation. If that were possible, a routine test in a clinic or emergency department might flag at‑risk patients without waiting for the next attack.
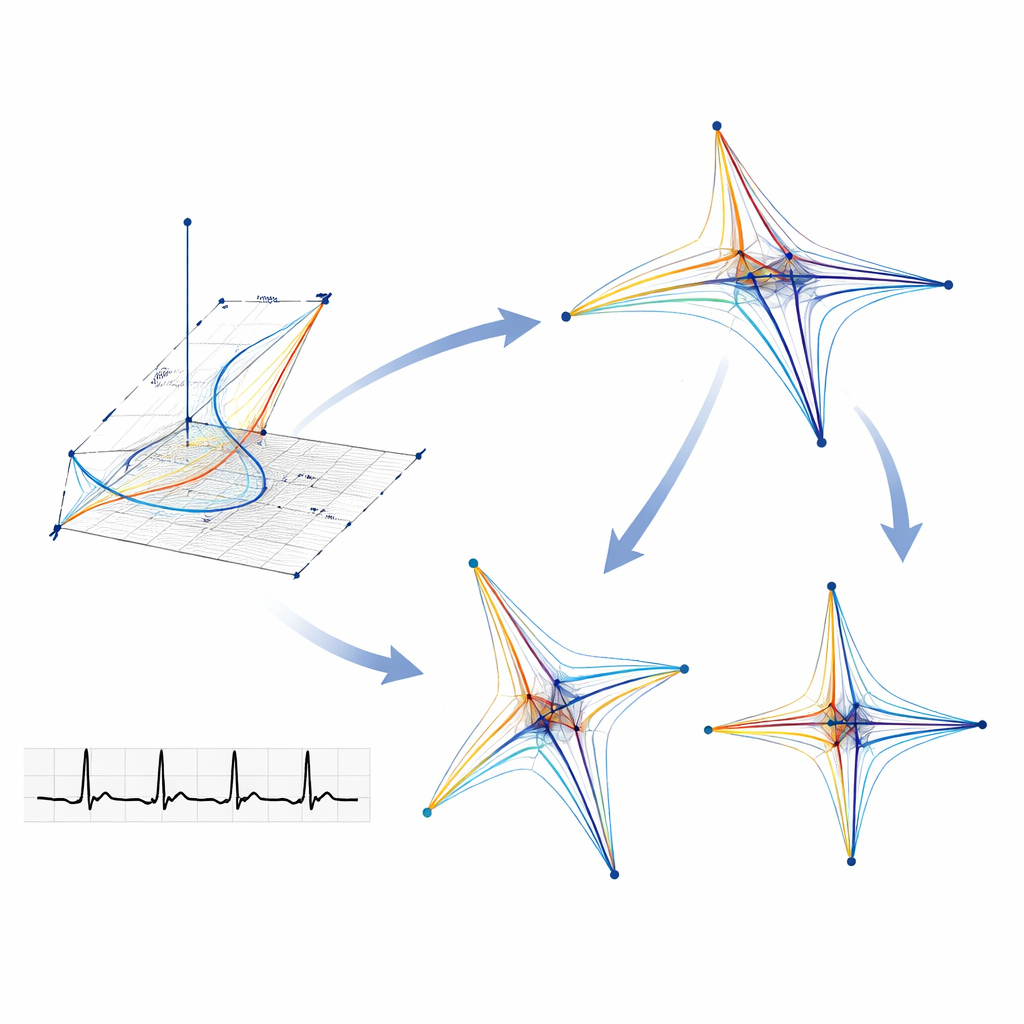
Turning heartbeats into geometric shapes
To hunt for these hidden clues, the team used a signal‑processing approach called Symmetric Projection Attractor Reconstruction. Instead of focusing on familiar ECG landmarks—the sharp spikes and waves doctors usually inspect—this method treats the entire repeating heartbeat as a pattern in time. It samples each beat at several points and plots those values against each other, turning the one‑dimensional signal into a two‑dimensional geometric picture called an attractor. Subtle changes in how the heart’s electrical signal rises, falls and varies from beat to beat show up as differences in the shape, size and density of these attractor patterns, even when the original ECG looks normal to the eye.
Training computers to spot risky patterns
The investigators drew on a large open database of ECGs that included people with documented atrial fibrillation episodes and carefully matched control subjects without known rhythm problems, balancing for age and sex. For each 10‑second normal‑rhythm tracing, they generated attractor images from all 12 ECG leads and converted these shapes into numerical summaries describing how densely points clustered in different directions and distances from the center. These summaries were then fed into two standard machine‑learning approaches, one that classifies a new case based on its nearest neighbors in the dataset and another that builds a decision tree of if‑then rules. The team also tested practical questions important for real‑world use, such as which ECG lead works best and whether lower sampling rates—common in everyday clinic machines—hurt performance.
How well the method worked
Across many combinations of settings, the best configuration used attractor features describing how densely points were arranged around the circle, taken from ECGs sampled at 125 hertz and classified with the nearest‑neighbors method. Under these conditions, the system correctly distinguished people with and without paroxysmal atrial fibrillation about 81% of the time. It was highly reliable at identifying truly healthy controls (about 95% specificity) but more modest at picking up all affected patients (about 67% sensitivity). A decision‑tree approach nudged sensitivity higher to about 73% but sacrificed some ability to avoid false alarms. Importantly, the method needed only 10 seconds of normal‑rhythm data, yet its sensitivity was roughly double that reported for 30‑day long‑term heart monitoring in earlier work.
Who benefits and what still needs work
The researchers found that performance was fairly stable across different age groups but somewhat better in men than women, likely reflecting imbalances in the underlying dataset. Other heart conditions present in some patients tended to reduce accuracy, and the timing between the documented fibrillation episode and the normal‑rhythm ECG also seemed to matter. These findings suggest that future studies with larger, more diverse patient groups—and careful tracking of other diagnoses and recording times—could further refine the tool and clarify where it works best, such as in clinics, emergency rooms or wearable devices.
A step toward earlier, easier detection
For a layperson, the key message is that a standard, quick heart test may hold more information than doctors can currently see. By converting normal‑looking heartbeats into geometric patterns and letting algorithms compare those shapes across many patients, this study shows it is possible to flag people with a history of paroxysmal atrial fibrillation using only a few seconds of normal rhythm. While the method is not yet perfect, it offers a promising path toward faster, more comfortable screening that could help identify people at risk of stroke earlier and guide who should receive closer follow‑up or preventive treatment.
Citation: Creasy, S., Lip, G.Y.H., Tse, G. et al. Classification of paroxysmal atrial fibrillation using sinus rhythm electrocardiograms using the symmetric projection attractor reconstruction method. Sci Rep 16, 9705 (2026). https://doi.org/10.1038/s41598-026-37491-1
Keywords: atrial fibrillation, electrocardiogram, machine learning, heart rhythm, early detection