Clear Sky Science · en
Preoperative radiomics models for predicting risks of distinct recurrence patterns in pancreatic ductal adenocarcinoma based on contrast enhanced CT
Why tracking cancer’s return matters
For people with pancreatic cancer, surgery offers the best chance of long-term survival. Yet even after surgeons remove all visible tumor, the disease often comes back, either near the original site or as new tumors elsewhere in the body. Today, doctors have limited tools to predict which patients are most likely to face which kind of recurrence, so everyone tends to receive similar follow-up and treatments. This study explores whether patterns hidden inside routine CT scans, combined with simple blood tests and staging information, can forecast how pancreatic cancer is likely to return—before the operation even takes place.
Looking inside scans for hidden clues
The research focused on pancreatic ductal adenocarcinoma, the most common and deadly type of pancreatic cancer. The team analyzed records from 290 patients who had surgery intended to cure their disease. Before surgery, all patients had contrast-enhanced CT scans, a standard imaging test in which a dye highlights blood vessels and organs. Instead of relying only on what a radiologist can see by eye, the scientists used a technique called radiomics: computer algorithms that measure hundreds of subtle features in each tumor image, such as shape, brightness, and texture. These features can reflect how aggressive or heterogeneous a tumor is, even when it looks similar to others on a standard scan.
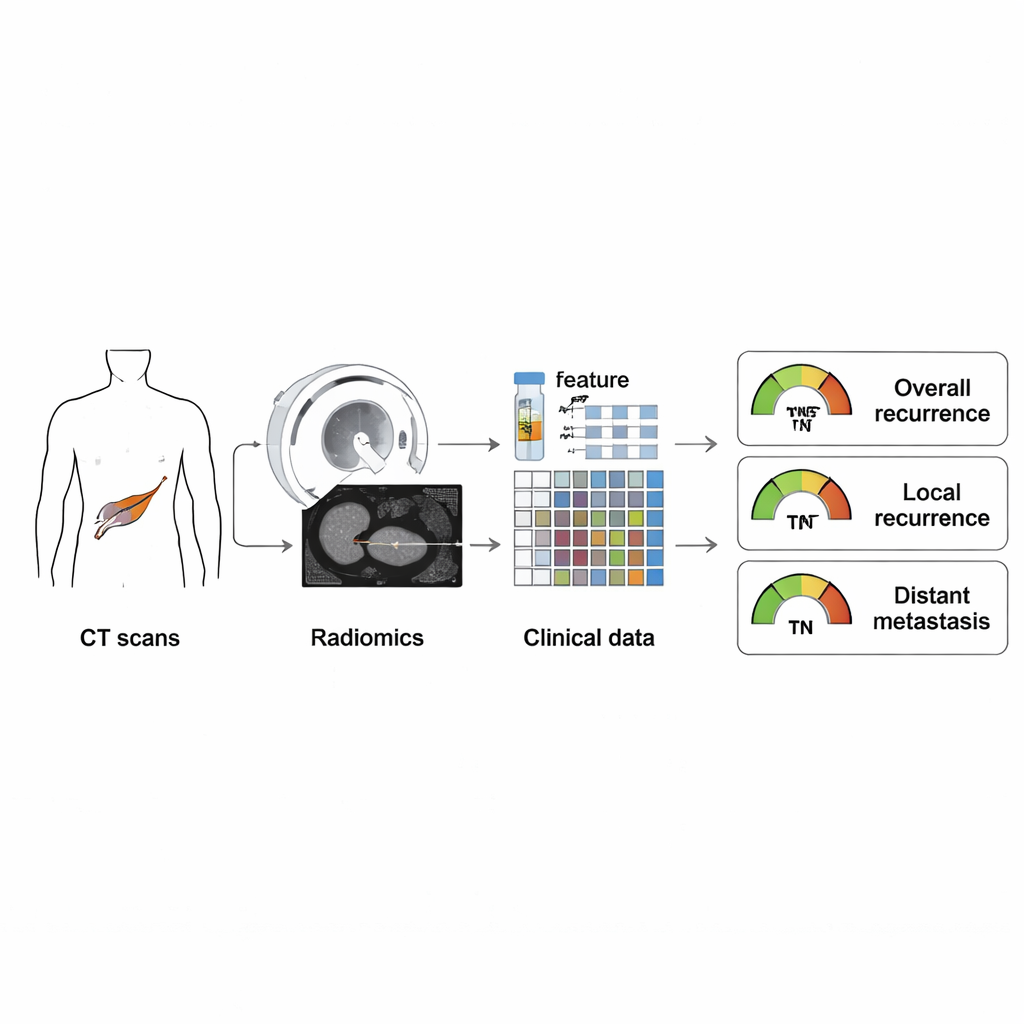
Blending scan data with everyday clinical facts
Radiomic features alone do not tell the whole story, so the researchers also included straightforward information doctors already collect. These clinical factors included the tumor’s stage according to the American Joint Committee on Cancer (AJCC), the pattern of how the tumor took up contrast on the CT scan, and blood levels of CA19-9, a commonly used pancreatic cancer marker. Using statistical modeling, they built three types of prediction tools: one based only on radiomics, one based only on clinical factors, and a combined model that integrated both. Each tool was trained on a portion of the patients and then tested on the remaining patients to see how well it could predict three outcomes: any recurrence, local recurrence near the original site, and distant spread to organs such as the liver or lungs.
Sorting patients into higher and lower risk
The combined models proved to be the most accurate. For example, when predicting whether a patient would have any recurrence within a year of surgery, the integrated model outperformed models that used only imaging or only clinical data. It was particularly strong in forecasting distant metastasis, where its one-year accuracy score (AUC) approached 0.90 in the training group and remained high in the test group. The researchers translated these results into a user-friendly chart, called a nomogram, that assigns each patient a risk score based on their CT-derived radiomics profile and clinical factors. Patients could then be grouped into “high-risk” and “low-risk” categories, which showed clearly different lengths of time before recurrence on follow-up.
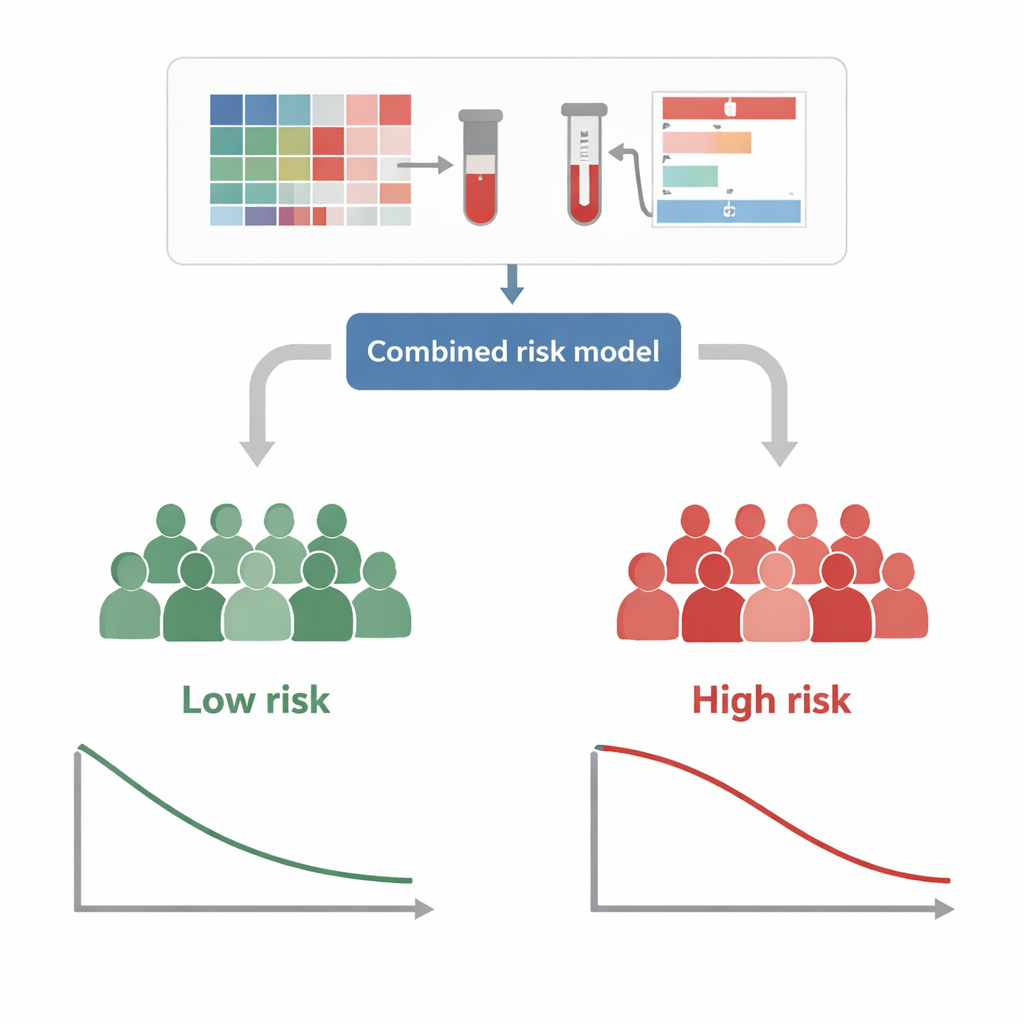
Turning predictions into tailored care
Because these predictions are based entirely on information available before surgery, they could help doctors personalize treatment plans. Someone flagged as high risk for distant metastasis might be steered toward more intensive chemotherapy before or after surgery, or considered for clinical trials. A patient at high risk for local recurrence might benefit from extra attention to the surgical margins, or from radiation therapy focused on the tumor bed. The models also help determine which patients may need closer imaging and blood-test follow-up in the first year after surgery, when recurrence is most likely to appear.
What this means for patients
In essence, this study shows that routinely collected CT scans contain far more information than the human eye can easily detect. By using radiomics to decode these hidden patterns and combining them with simple lab tests and staging data, doctors can better estimate how and where pancreatic cancer is likely to return. While the work still needs confirmation in larger, multi-hospital studies, it points toward a future in which patients receive more precisely tailored care: those at highest risk can be treated and monitored more aggressively, while lower-risk patients may avoid unnecessary procedures and anxiety.
Citation: Jiang, Y., Zeng, J., Sun, R. et al. Preoperative radiomics models for predicting risks of distinct recurrence patterns in pancreatic ductal adenocarcinoma based on contrast enhanced CT. Sci Rep 16, 7129 (2026). https://doi.org/10.1038/s41598-026-37459-1
Keywords: pancreatic cancer, radiomics, CT imaging, cancer recurrence, risk prediction