Clear Sky Science · en
Gait adaptations to walker-assisted locomotion in elderly: a principal component analysis of spatiotemporal and kinematic parameters
Why walking with a smart walker matters
As people get older, walking often becomes slower and less steady, raising the risk of falls, broken bones and loss of independence. Many seniors use walkers to stay mobile, but these devices can also subtly change how they move—sometimes in ways that are not well understood. This study explores how a high-tech “smart walker” alters the walking pattern of healthy older adults, using detailed motion measurements and advanced statistics to tease apart which changes come from aging and which are caused by the device itself.
How aging and walking supports are connected
Falls are a major health problem in later life, with about one in three people over 65 taking at least one fall each year. To lower this risk, clinicians often prescribe walkers. Yet standard walkers can be hard to maneuver and may even increase wobbliness if used incorrectly. Engineers have begun to build smart walkers that include sensors, motors and control systems to provide smoother support and guidance. Before such devices are rolled out widely to people with conditions like stroke or Parkinson’s disease, researchers need to understand how they change walking in otherwise healthy older adults. That “clean” picture becomes the baseline for spotting whether future patients are improving, compensating or adopting new, potentially unhelpful movement habits.
A closer look at smart walker-assisted walking
The team studied 14 older volunteers in their mid‑60s who did not have walking impairments. Each person completed two simple 10‑meter walks: one without any device and one using a smart walker called the UFES vWalker. This robotic walker has force sensors, laser scanners and wheels controlled by software that converts the user’s pushing force into a safe, low top speed of 0.4 meters per second. While participants walked, a wearable motion capture suit with small sensors on the pelvis, thighs, shins and feet recorded how fast they walked, how long each step took, how wide their steps were, and how their hip, knee and ankle joints moved through the walking cycle.
What changed when the walker was used
When using the smart walker, participants moved more slowly, took shorter and slightly narrower steps, and spent more time with both feet on the ground. The timing from one step to the next also became more variable. Joint angles changed as well: the hips stayed in a more flexed, “bent‑forward” posture throughout the walk, while the knees tended to bend less during the swing phase. Many ankle and hip movements increased, reflecting the hunched posture people adopted to hold the forearm supports of the walker. These shifts were not random. Using a statistical technique called principal component analysis, the researchers grouped related measurements into broader “domains” such as pace, rhythm, symmetry, base of support and joint motion. Normal walking showed clear domains similar to those found in previous aging studies, but walker‑assisted walking produced a different pattern, including new domains linked specifically to how the leg swings and how steps are generated when body weight is partially supported by the device.
Hidden patterns in how we walk
By mixing standard step‑by‑step measures with joint motion data, the analysis revealed how different parts of walking are coordinated. In normal walking, pace and variability formed one key domain, while rhythm, symmetry and base of support formed others; adding joint angles separated out distinct motion patterns for hip, knee and ankle. With the smart walker, however, knee and ankle movement during early stance became tightly linked to how quickly people walked, while hip and knee motion during leg swing were tied to differences between the left and right steps. Another new domain, called step dynamics, captured how step length, timing differences and ankle push‑off interacted when the walker was involved. These device‑specific domains suggest that the smart walker does more than simply stabilize the user—it actively reshapes how the legs coordinate to produce each step.
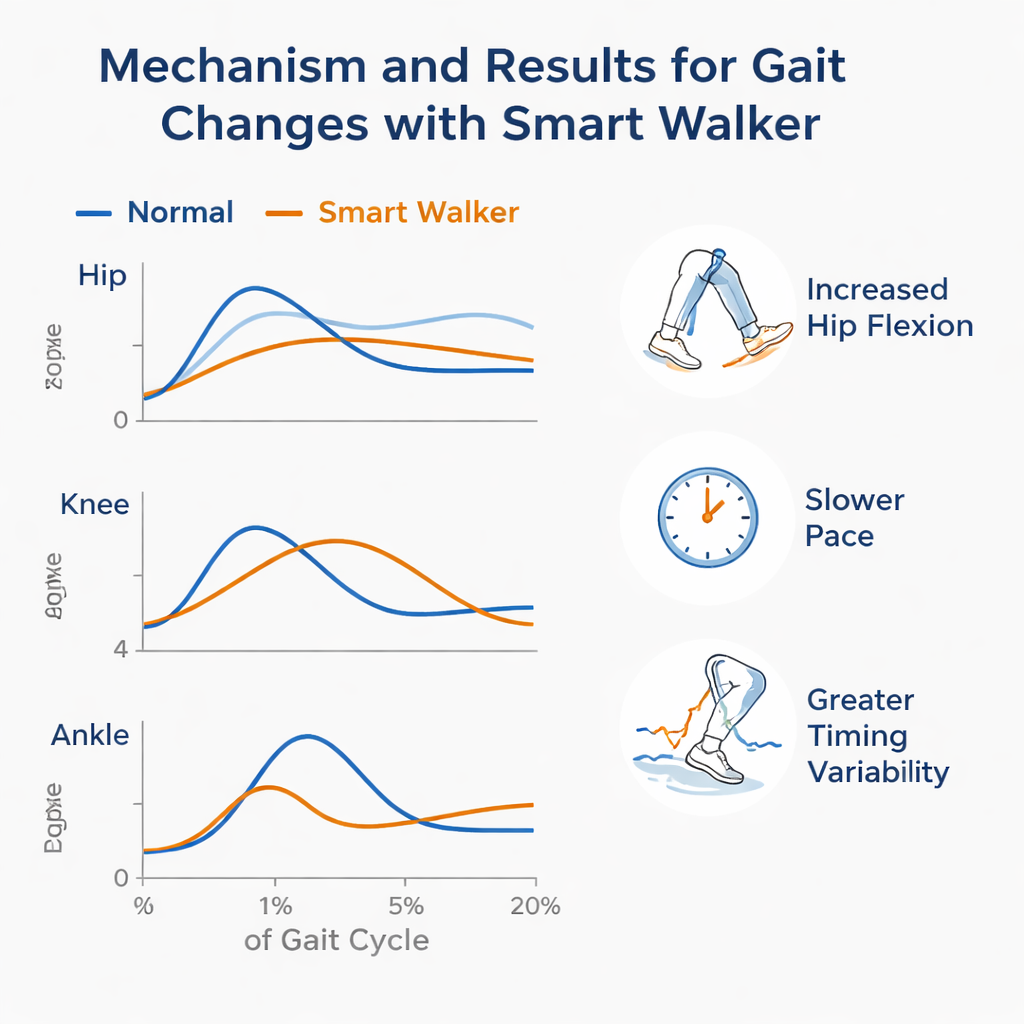
What this means for safer walking in old age
For a non-specialist, the key message is that smart walkers can make walking slower and more controlled, but they also encourage a bent‑forward posture and a different pattern of step timing and leg movement than seen in normal walking. These device‑driven changes are not necessarily bad; in the short term they may help people feel more secure. But if rehabilitation programs rely on a smart walker for too long without careful adjustment, users might “learn” a walking style that is hard to unlearn later. The authors argue that therapists and designers should use these findings to fine‑tune support level, handle height and training goals so that smart walkers act as stepping‑stones toward safer, more natural walking—rather than permanent crutches that lock in new, less efficient habits.
Citation: Elias, A., Loureiro, M., Machado, F. et al. Gait adaptations to walker-assisted locomotion in elderly: a principal component analysis of spatiotemporal and kinematic parameters. Sci Rep 16, 6872 (2026). https://doi.org/10.1038/s41598-026-37448-4
Keywords: smart walker, elderly gait, fall prevention, rehabilitation robotics, wearable motion sensors