Clear Sky Science · en
24-hour urine chemistry shows higher stone formation risk after malabsorptive than restrictive type bariatric surgery
Why Weight-Loss Surgery and Kidney Stones Are Linked
Bariatric (weight-loss) surgery can be life‑changing for people with severe obesity, helping control diabetes, blood pressure, and other problems. But doctors have noticed another, less welcome effect: some patients seem more likely to develop painful kidney stones afterward. This study asks a practical question that matters to patients and clinicians alike: does the type of bariatric surgery you choose change your future risk of forming kidney stones?
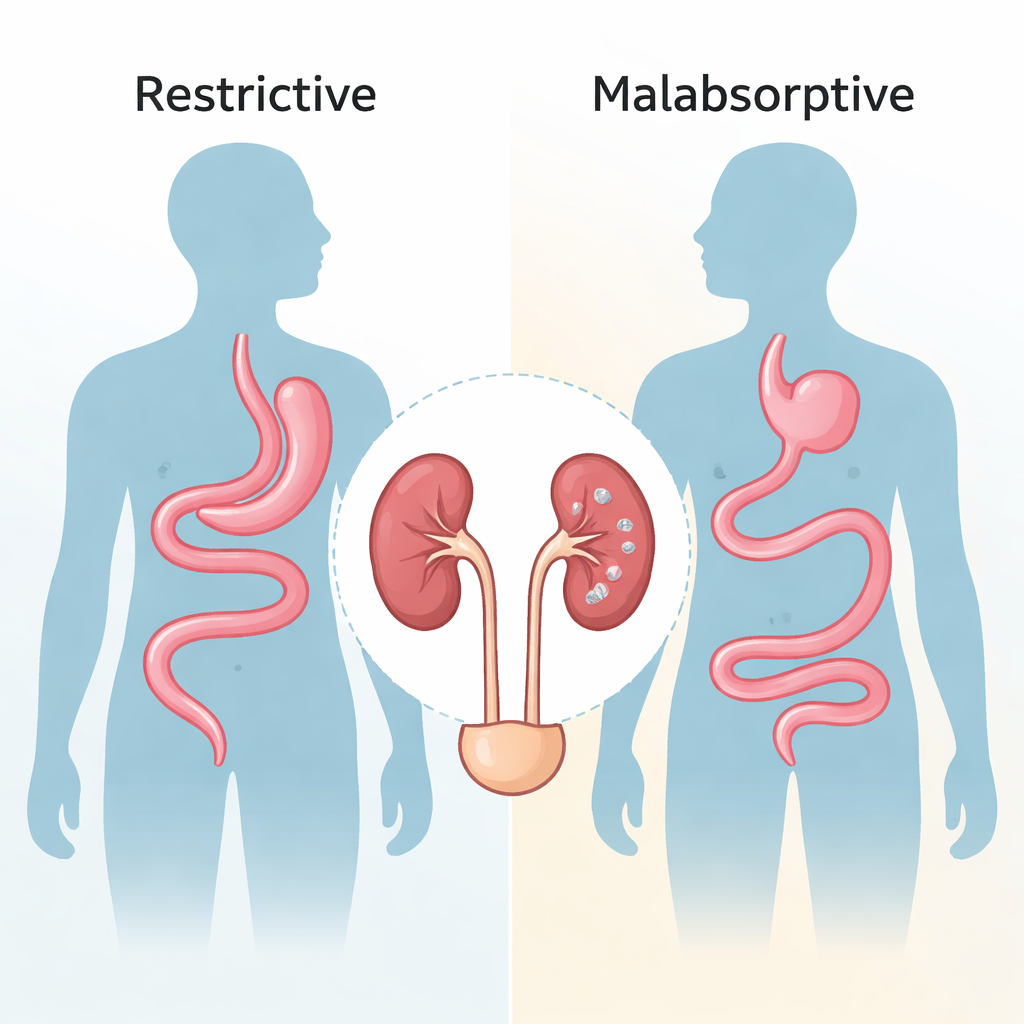
Two Different Paths to Weight Loss
Bariatric operations fall into two broad categories. “Restrictive” procedures, such as sleeve gastrectomy, mainly shrink the stomach so people feel full with less food. “Malabsorptive” procedures, like Roux‑en‑Y gastric bypass, also reroute part of the small intestine, so fewer nutrients are absorbed. Both can lead to major weight loss, but they alter digestion in different ways. Because kidney stones often arise from changes in the mix of salts and acids the kidneys filter and excrete, the researchers suspected these surgical approaches might not be equal when it comes to stone risk.
Measuring Stone Risk in Urine
To probe this, doctors in Hong Kong followed 90 adults who underwent bariatric surgery at their center between 2017 and 2019. Within a year after surgery, each patient collected all urine produced over 24 hours. The team measured levels of substances known to encourage or discourage stone formation, including oxalate, calcium, magnesium, uric acid, citrate, and the acidity (pH) of the urine. Rather than just counting future stones – which can take years to appear – they focused on these chemical “risk signatures” that are well‑established predictors of kidney stone formation.
Malabsorptive Surgery Shows a Riskier Pattern
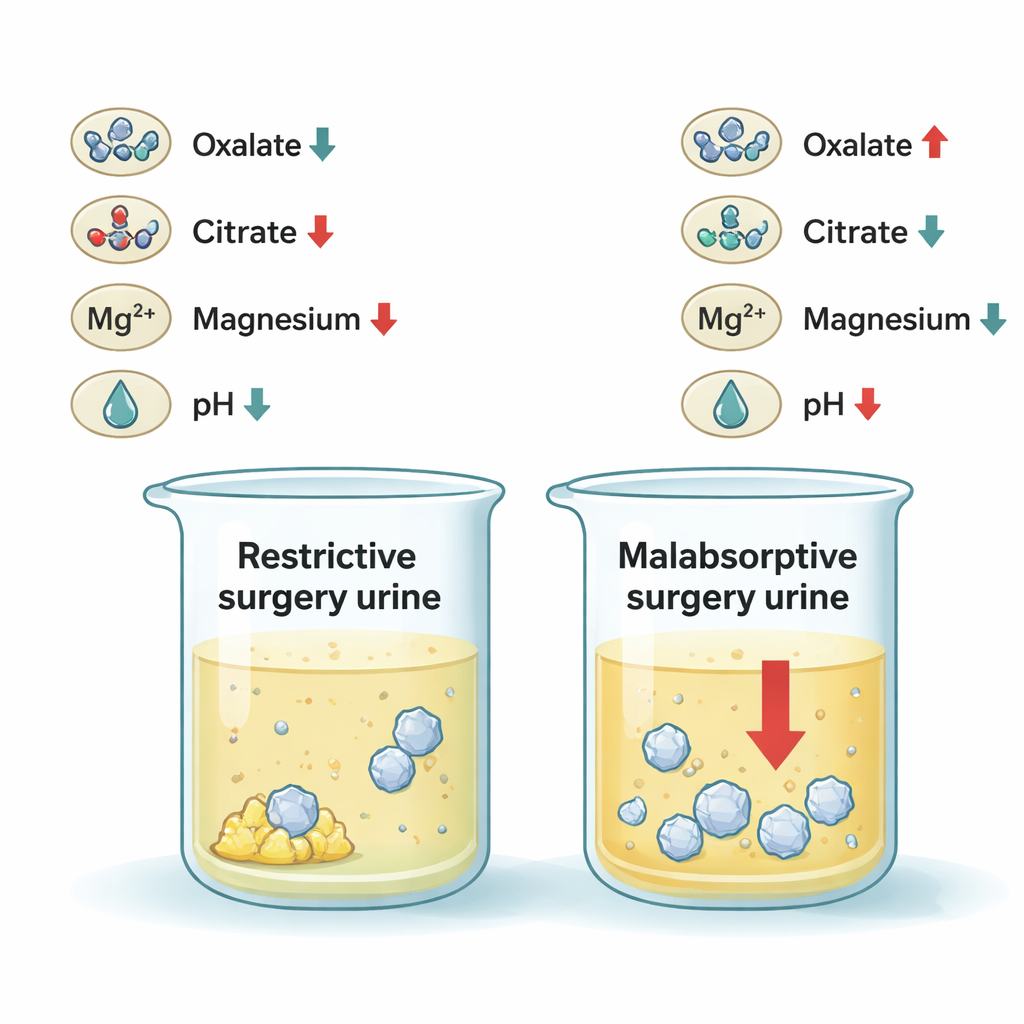
When the researchers compared the 35 people who had malabsorptive operations with the 55 who had restrictive surgery, a clear pattern emerged. The malabsorptive group had more oxalate in their urine and lower levels of several protective factors, including citrate and magnesium, along with more acidic urine. More than half of these patients met criteria for high oxalate, over 70% had low citrate, and more than half had urine that was acidic enough to favor stone formation. In contrast, the restrictive group showed these risky patterns much less often, though they were more likely to have high uric acid in their urine, which can promote a different type of stone.
Why the Gut Affects the Kidneys
The differences likely trace back to how malabsorptive surgery changes digestion. After bypassing sections of the small intestine, fats and bile acids are less completely absorbed and can bind up calcium in the gut. That leaves more “free” oxalate available to be absorbed into the bloodstream and then excreted in urine, raising stone risk. Chronic mild diarrhea and shifts in gut bacteria after bypass can also increase oxalate absorption and make the body more acidic overall, lowering urine pH and citrate levels. Restrictive surgery, which mainly reshapes the stomach without bypassing intestine, disturbs these processes less, though changes in diet and metabolism can still raise uric acid output.
What This Means for Patients
The study concludes that, at least in the first year after surgery, malabsorptive bariatric procedures create a more “stone‑friendly” urine chemistry than restrictive operations. That does not mean such surgeries should be avoided; for many people, their benefits for weight, diabetes, and survival are substantial. But it does suggest that patients and surgeons should factor kidney stone risk into the choice of procedure, and that those who undergo malabsorptive surgery may need closer follow‑up. Simple steps such as staying well hydrated, adjusting diet, and monitoring urine chemistry could help prevent painful stones and protect kidney health in the long term.
Citation: Liu, A.Q., Choy, E.KH., Siu, B.W.H. et al. 24-hour urine chemistry shows higher stone formation risk after malabsorptive than restrictive type bariatric surgery. Sci Rep 16, 6590 (2026). https://doi.org/10.1038/s41598-026-37440-y
Keywords: bariatric surgery, kidney stones, Roux-en-Y gastric bypass, sleeve gastrectomy, urine chemistry