Clear Sky Science · en
Metabolic implications of COVID-19 with a focus on lipid profiles and inflammatory markers
Why COVID-19 Still Matters for the Heart
The COVID-19 pandemic is often discussed in terms of coughs, fevers and vaccines, but the virus also leaves a quieter mark on the body: it can disrupt our metabolism and heart health long after the initial infection fades. This study from Johannesburg, South Africa, followed people hospitalized with moderate to severe COVID-19 and compared them with diabetic and healthy volunteers. By tracking blood fats, blood pressure and key immune signals over several months, the researchers explored how COVID-19 reshapes the chemistry of the blood and what that might mean for long-term risk of heart attack and stroke.
Who Was Studied and What Was Measured
The research team enrolled 169 adults during South Africa’s Delta wave in 2021. Eighty-four were hospitalized with COVID-19, while the other participants were either people with diabetes or healthy volunteers who had not been hospitalized with the virus. The COVID-19 patients tended to have more weight problems and high blood pressure than the comparison groups: about 60% were obese, and more than half had hypertension or diabetes. Within two days of admission, the team collected detailed information on body size, blood pressure, blood sugar, standard cholesterol tests, a special cholesterol-like particle called lipoprotein(a), and a panel of inflammatory molecules that track how strongly the immune system is activated.
How COVID-19 Alters Blood Fats and Inflammation
When patients were acutely ill with COVID-19, their cholesterol profile looked very different from that of the diabetic and healthy controls. Levels of “bad” LDL cholesterol, “good” HDL cholesterol, and total cholesterol were all lower, while triglycerides and the ratio of triglycerides to HDL were higher. These shifts echo patterns seen in other severe infections and hint at the body burning through or redistributing fats during intense inflammation. The sickest patients—those who did not survive—tended to be heavier, have higher blood sugar and show especially low LDL cholesterol. They also had very high levels of inflammatory markers such as C‑reactive protein, ferritin and clusters of immune signaling proteins known as Th1 and Th17 cytokines. In simple terms, a body under extreme inflammatory stress showed both disturbed blood fats and a storm of immune activity.
Signals That Predicted Who Did Poorly
The researchers used statistical models to ask which measurements best foretold death, need for intensive care or need for breathing support. After taking age, sex and race into account, several clear patterns emerged. Being female was linked with a lower risk of dying, while each step up in body mass index sharply increased the chances of death, intensive care admission and respiratory support. Strikingly, lower LDL cholesterol at admission predicted a higher risk of death: patients below about 1.8 mmol/L were more likely to die in hospital. At the same time, certain inflammatory molecules—especially interleukin‑6 and related Th17 and Th1 cytokines—were strongly tied to severe outcomes. When LDL cholesterol was combined with body mass index and these inflammatory markers, the model did a much better job of identifying high‑risk patients than any single factor alone.
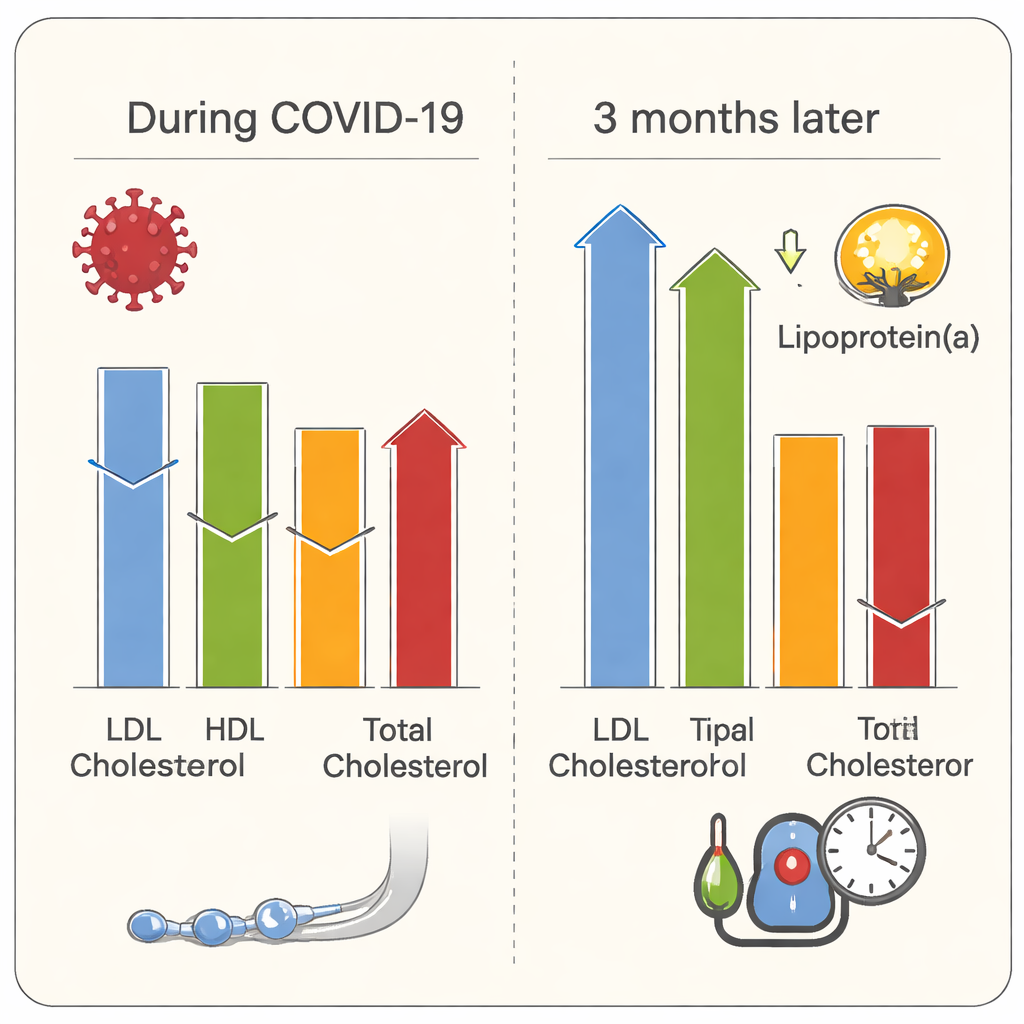
What Lingers Months After Infection
The story did not end when patients left the hospital. Three months after recovery, 44 survivors returned for follow‑up. Their blood pressure was significantly higher than before infection, and nearly one in four had developed new high blood pressure. Their waistlines and body mass index remained higher than in the control groups. Blood fats also “rebounded”: total, LDL and HDL cholesterol all rose compared with the hospital phase, while triglycerides fell. A notable finding involved lipoprotein(a), a genetically influenced particle that promotes clotting and artery disease. Levels of lipoprotein(a) were higher in COVID‑19 survivors than in healthy controls at follow‑up and were particularly elevated in Black and Mixed‑Race participants, who are already known to have higher baseline levels. Although lipoprotein(a) itself did not track closely with short‑term inflammation in this study, its persistent elevation at values considered high risk for heart disease raises concern about long‑term complications.
What This Means for Everyday Health
For lay readers, the message is that COVID-19 is not only a breathing problem: it can unsettle blood fats, blood pressure and the immune system in ways that may increase heart and stroke risk months after infection, especially in people who are overweight or have metabolic conditions. During severe illness, very low LDL cholesterol and high inflammatory markers seem to flag those at greatest danger, and after recovery, new high blood pressure, abnormal cholesterol and raised lipoprotein(a) suggest a lingering vulnerability. The authors argue that hospitals and clinics, particularly in resource-limited settings, should consider routine monitoring of blood pressure and cholesterol (including lipoprotein[a] where possible) in COVID‑19 survivors, and that larger studies are needed to confirm whether treating these changes early can prevent future heart disease.
Citation: Mohamed, F., Gunter, S., Currin, S. et al. Metabolic implications of COVID-19 with a focus on lipid profiles and inflammatory markers. Sci Rep 16, 6217 (2026). https://doi.org/10.1038/s41598-026-37439-5
Keywords: COVID-19 and heart risk, cholesterol changes, lipoprotein(a), inflammation and immunity, post-COVID recovery