Clear Sky Science · en
Interpretable machine-learning risk prediction of unplanned extubation among cancer patients with peripherally inserted central catheters
Why this matters for people with cancer
Many people receiving cancer treatment rely on a thin tube placed in a vein of the upper arm, called a peripherally inserted central catheter, or PICC, to deliver drugs safely over weeks or months. When this tube comes out too early by accident or due to problems, treatment is disrupted, new procedures are needed, and patients may be put at risk. This study asks a simple but powerful question: can we predict who is most likely to have this kind of mishap, using both their health status and how well they care for the catheter at home?
A closer look at a common treatment lifeline
PICCs are widely used in cancer care because they spare veins from repeated needle sticks and protect tissues from harsh chemotherapy drugs. Yet the most dreaded day for patients and nurses is when a PICC must be pulled out early, or slips out on its own. In this study from a major hospital in China, 212 adults with cancer who received PICC lines between early 2021 and mid‑2022 were followed from catheter insertion until removal. About 11 out of every 100 patients experienced unplanned extubation—most often because the line was accidentally pulled, became blocked, caused serious skin reactions, or was linked to suspected bloodstream infection.
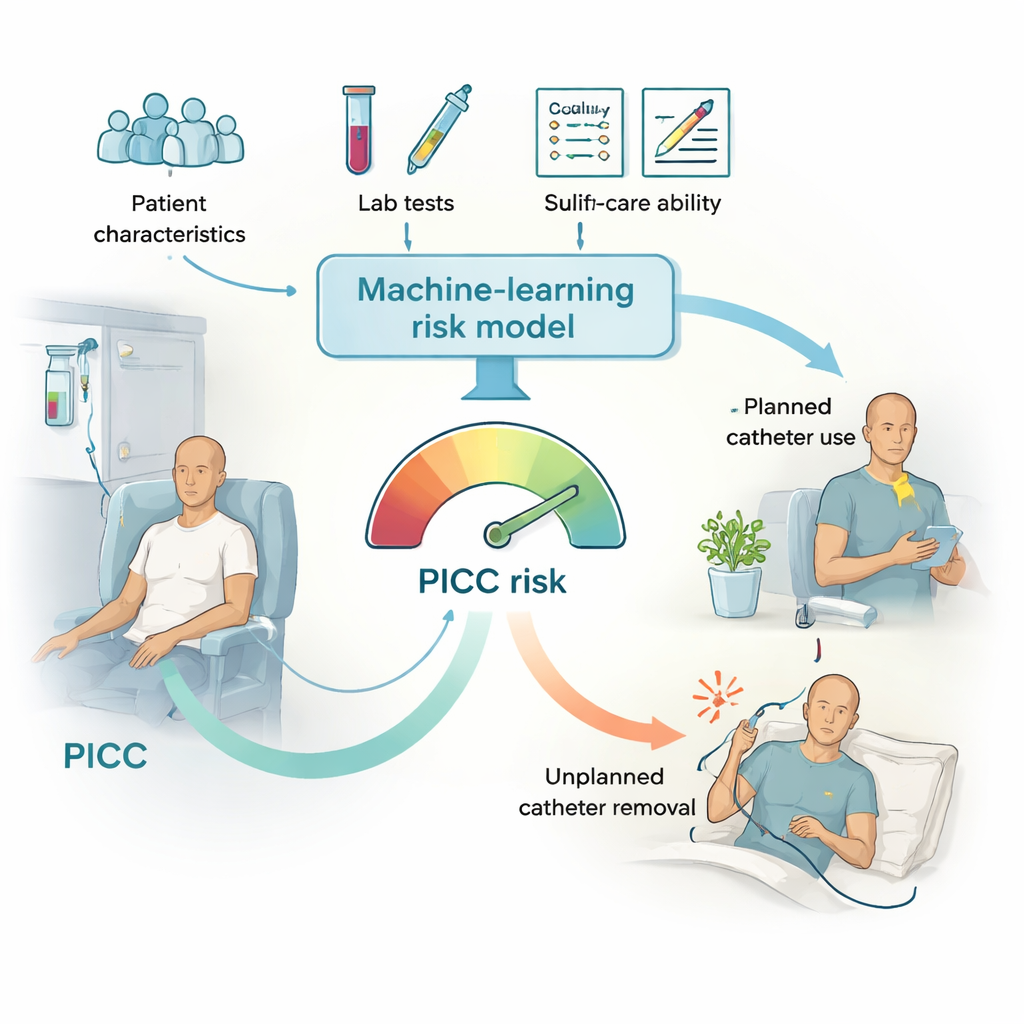
Beyond medical charts: life quality and self-care
Earlier research on PICC problems focused on medical details such as diabetes, blood test results, or the type of catheter used. The authors of this paper suspected that everyday life factors might be just as important. They measured two things shortly before each patient’s PICC was removed: a quality of life score describing how well patients could move, care for themselves, perform daily tasks, and cope with pain and anxiety; and a self-management score capturing how well patients understood and followed PICC care steps at home, from watching for dressings that curl to protecting the arm during bathing and exercise. On a simple two‑dimensional plot, patients who avoided unplanned catheter removal clustered in the upper-right corner—those who felt relatively well and were also good at self-care—while many of those with problems fell outside this zone.
A new combined measure: weighted quality of life
To capture this pattern more precisely, the team created a new number they called “weighted quality of life,” or WQOL, calculated by multiplying the quality of life and self‑management scores. This composite score reflects not just what patients are capable of doing, but what they actually do in their daily routines. Using several types of machine-learning models—which are computer programs that learn patterns from data—the researchers compared dozens of possible risk factors for unplanned PICC removal. They found that WQOL was the single most influential predictor, even more informative than quality of life or self‑management alone. Patients with low WQOL, such as those who knew how to look after a PICC but felt too unwell to keep up the care, were much more likely to lose their catheter early.
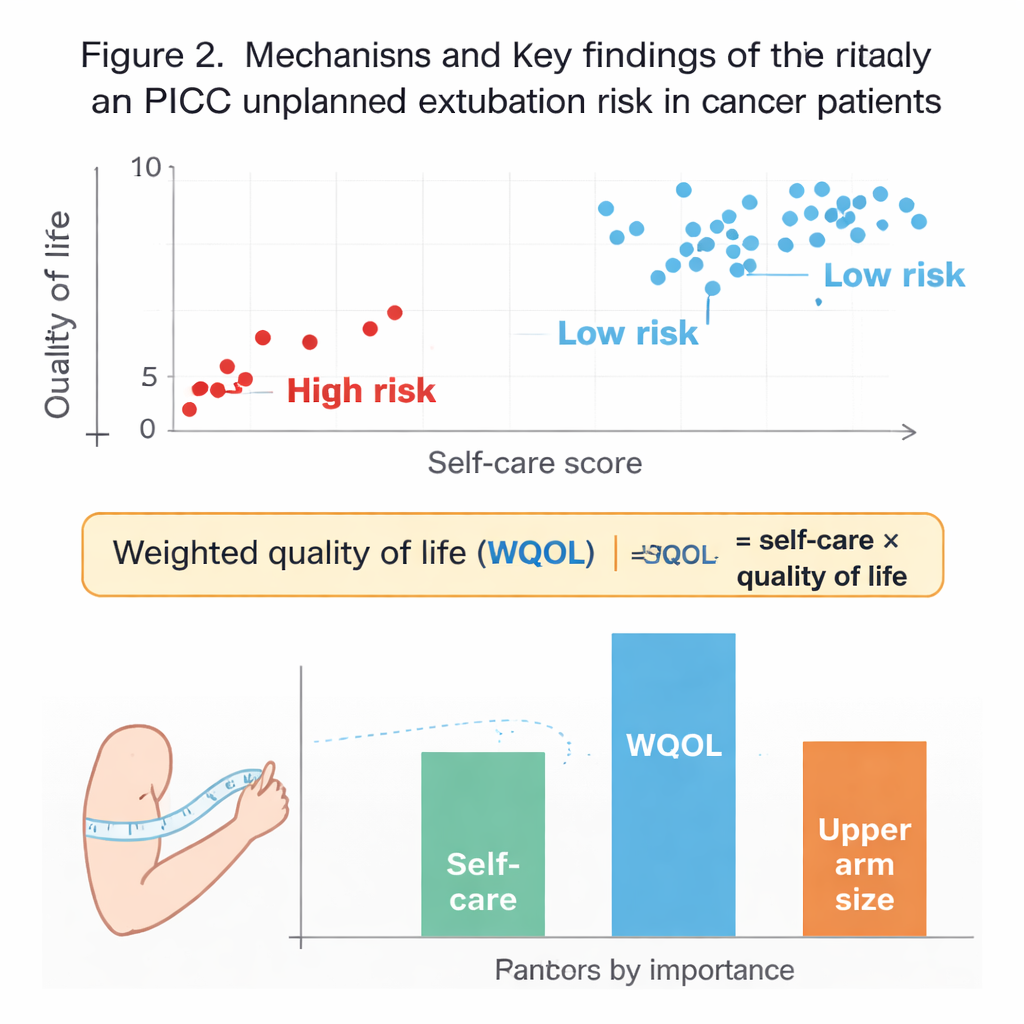
Other body clues hiding in plain sight
While WQOL stood out, the models also highlighted two other contributors. First, poor self-management on its own remained a clear risk: patients who neglected catheter protection while dressing, showering, or moving around were more prone to accidental dislodgement. Second, a larger upper arm circumference on the PICC side emerged as an often overlooked danger signal, especially among older women. The authors suggest that looser skin and greater arm size may allow the dressing to shift or curl more easily during everyday movements, making it easier for the catheter to be tugged out. These insights point toward simple steps—closer teaching and follow‑up for home care, better immobilization devices, and activity advice for patients with larger arms—that could help keep lines secure.
What this means for patients and caregivers
For people with cancer, the main message is hopeful: by paying attention not only to medical test results but also to how well patients feel and how confidently they manage their PICC at home, healthcare teams can better identify who is at higher risk of losing this vital treatment line. The study’s machine-learning approach, combined with an explanation tool that shows exactly which factors matter most for each individual, suggests that the new WQOL score could become a practical checklist item in cancer clinics. Used wisely, it may guide nurses to offer extra support or home visits to those with low WQOL, helping prevent avoidable complications, reduce repeated procedures, and keep cancer treatment on track.
Citation: Yang, Y., Yang, Y., Liu, Q. et al. Interpretable machine-learning risk prediction of unplanned extubation among cancer patients with peripherally inserted central catheters. Sci Rep 16, 7311 (2026). https://doi.org/10.1038/s41598-026-37411-3
Keywords: cancer, PICC line, catheter complications, machine learning, quality of life