Clear Sky Science · en
Development and validation of a novel scoring scale for colonic endocytoscopy staining quality
Looking Closely to Catch Colon Disease Early
Colon cancer often starts as tiny growths in the gut that can be hard to judge with the naked eye, even through a standard colonoscope. A newer technology called endocytoscopy lets doctors zoom in so far that they can see individual cells during an exam, offering a kind of “live biopsy” without cutting tissue. But this super‑zoom view only works if the tissue is stained clearly, much like focusing a camera lens. This study set out to build a simple, reliable way to score how good that staining is, so doctors can trust what they see and spot dangerous lesions earlier.
Why Image Staining Matters
Endocytoscopy gives a microscopic view of the colon’s inner lining, allowing doctors to inspect the shape of cells and the tiny glands they form—features that help distinguish harmless polyps from precancerous growths or cancer. To make these structures visible, the surface is sprayed with a blue dye and then rinsed. In practice, the quality of this staining has varied widely from one procedure or operator to another. Too much mucus, shaky hands, poor rinsing, or uneven dye can all blur the picture. Until now, there has been no standard way to judge how well a region has been stained, leaving assessments to each doctor’s personal experience and making training harder for newcomers.
A Simple Score for a Complex Picture
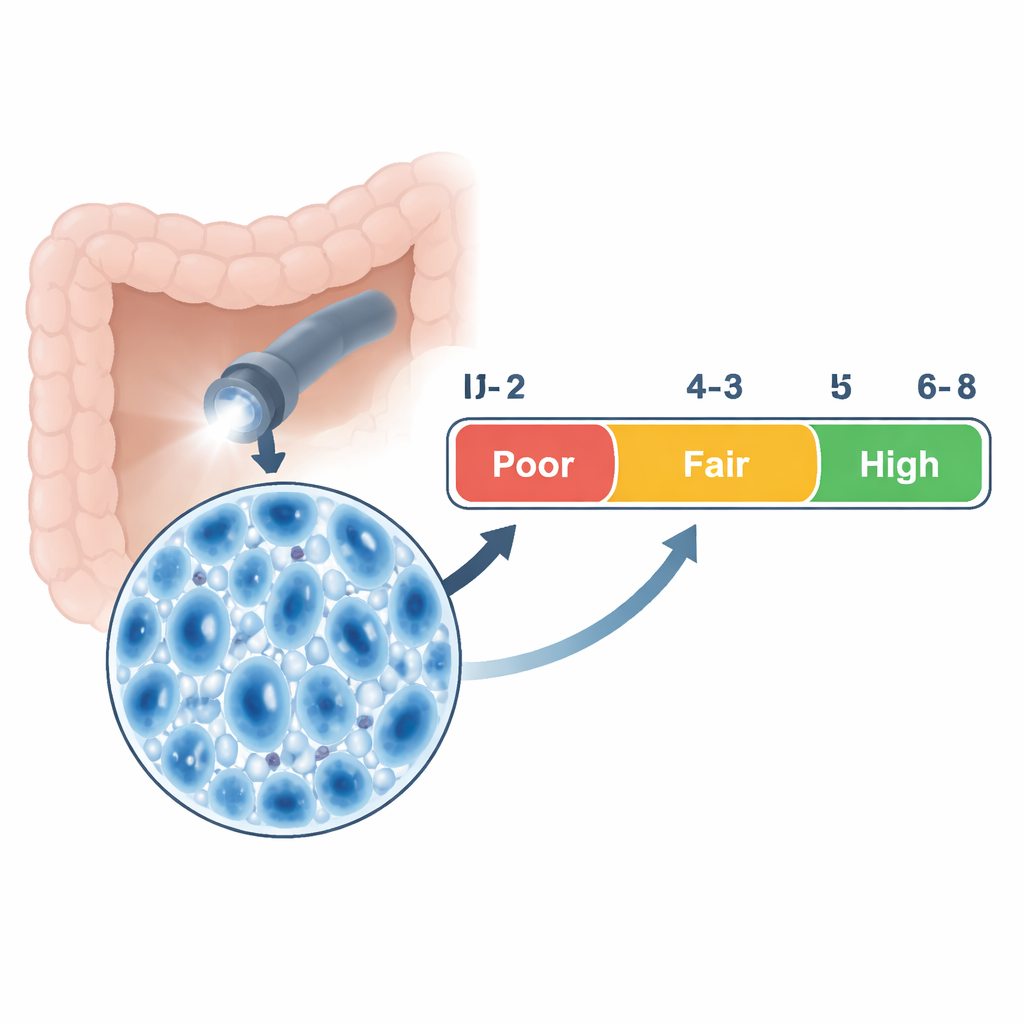
The researchers designed a four-part scale that breaks down staining quality into everyday, observable features: how clearly the cell nuclei are seen, how clearly the gland openings appear, how well mucus and excess dye have been washed away, and how sharp and steady the image itself is. Each part is scored from 0 to 2, producing a total between 0 and 8. Using statistical methods on thousands of endocytoscopy images, they grouped these total scores into three grades: poor (0–2), fair (3–5), and high (6–8) quality. Senior endoscopists with extensive experience scored a large first set of images, and any disagreements were resolved by discussion, creating a “gold standard” set of ratings that could be used to test the scale.
Putting the Scale to the Test
To check that the expert scores truly reflected how well the tissue was stained, the team also measured how dark the dye appeared in each image using specialized software. These measurements rose in step with the experts’ scores, showing a strong match between visual judgment and objective data. The scale itself showed excellent consistency across different senior doctors. Junior doctors then used the scale to score the same images before and after a month of structured training. After training, their agreement with the expert ratings improved markedly, indicating that the scale can flatten the learning curve and help less experienced physicians quickly approach expert-level judgment.
From Clearer Images to Better Diagnoses
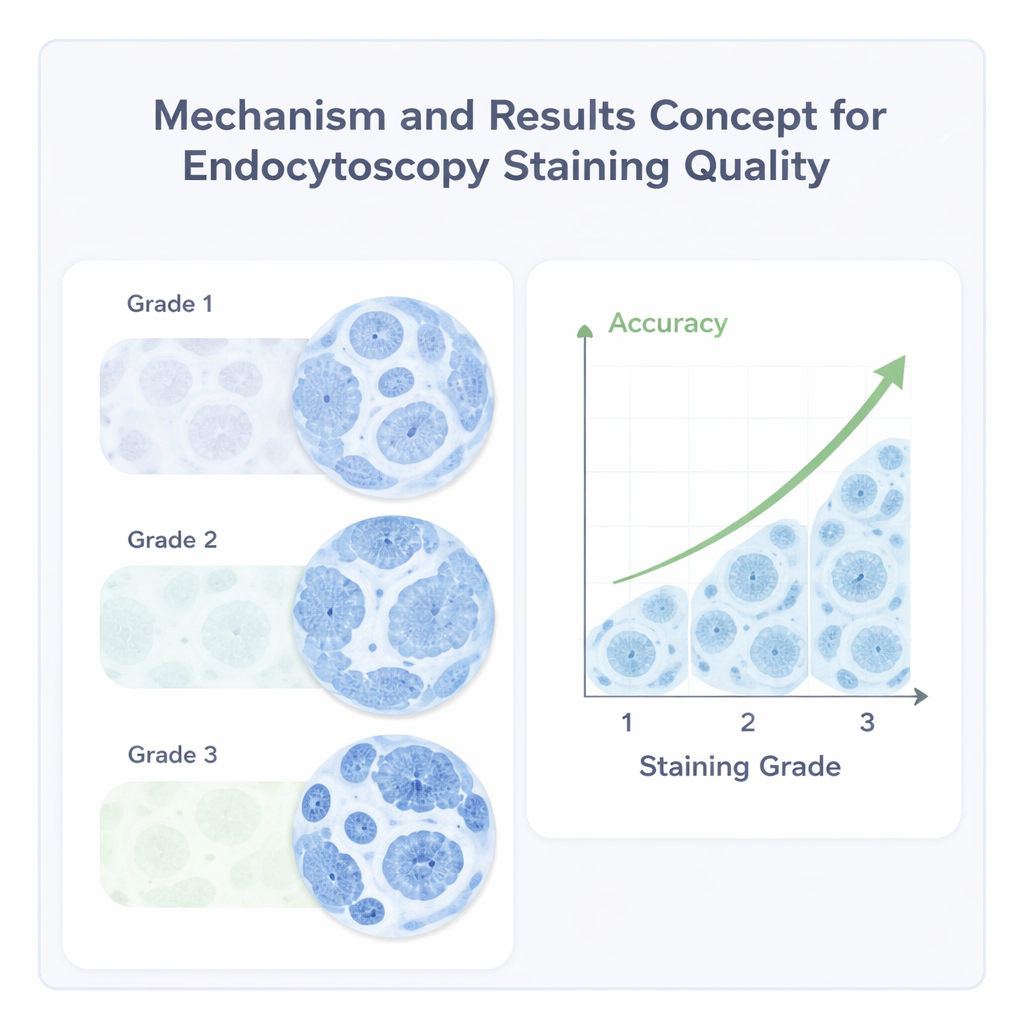
The study went further to ask whether better staining actually leads to better diagnoses. When the researchers compared endocytoscopy-based interpretations with the final laboratory results from removed tissue, they found a striking pattern: images with high staining quality produced correct diagnoses more than 96 percent of the time, while fair images did so about 82 percent of the time, and poor images only about 45 percent. They also showed that certain factors, such as the size and shape of the lesion and the experience level of the doctor, influenced how likely it was to achieve top-quality staining, highlighting where technique and training can make the biggest difference.
What This Means for Patients and the Future
For patients, the new staining quality score is not something they will see on a report, but it can quietly improve care. By giving clinics a clear, shared yardstick for what a “good” microscopic image looks like, the scale helps doctors refine their techniques, standardize training, and reduce guesswork during colon exams. It also creates a foundation for computer programs and artificial intelligence tools that could automatically flag blurry or poorly stained images in real time. While this study was done at a single center and focused on colon lesions, the same approach could eventually extend to the esophagus, stomach, and small intestine. In short, by making sure the smallest details are seen clearly, this work aims to make early detection of serious disease more reliable and more widely available.
Citation: Fan, J., Zhu, H., Liu, M. et al. Development and validation of a novel scoring scale for colonic endocytoscopy staining quality. Sci Rep 16, 7301 (2026). https://doi.org/10.1038/s41598-026-37406-0
Keywords: endocytoscopy, colon polyps, staining quality, optical biopsy, colorectal cancer screening