Clear Sky Science · en
Correlation of inflammatory mediators with osteophyte formation in end-stage knee osteoarthritis
Why achy knees grow bony “spurs”
Many people with long‑standing knee arthritis develop hard, bony bumps around the joint, often called bone spurs. These outgrowths can limit movement and add to pain, yet doctors still debate why they form and how they relate to the underlying disease. This study looked inside severely damaged knees to see whether chemical signals of inflammation in the joint fluid are linked to how large these bony outgrowths become, offering clues to both disease mechanisms and future treatments.
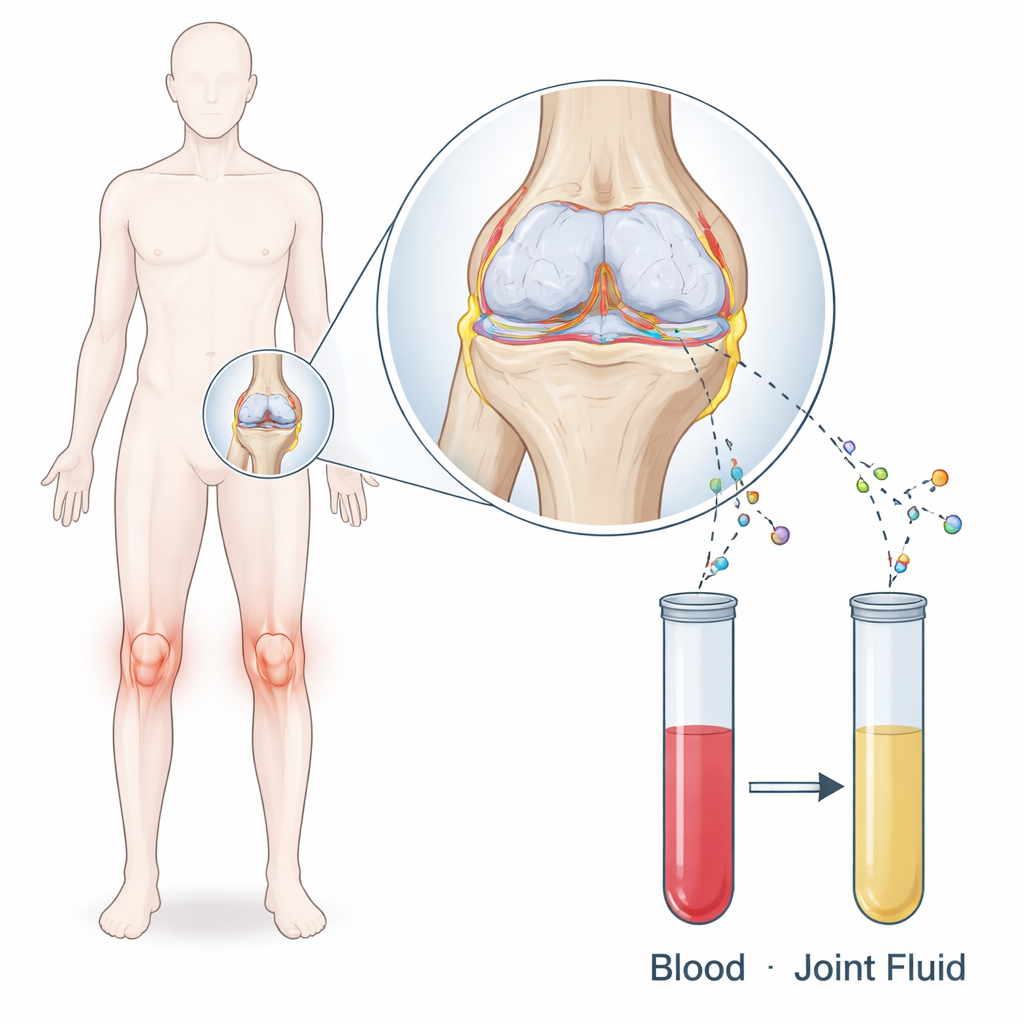
The hidden world inside an arthritic knee
Osteoarthritis is more than simple “wear and tear.” As the smooth cartilage that cushions the bones breaks down, the joint environment fills with chemical messengers released by injured cells and surrounding tissues. The researchers focused on three of these messengers: MMP‑1, an enzyme that helps break down cartilage; IL‑8, a signal that draws in inflammatory cells; and IL‑18, another inflammatory signal known to influence bone remodeling. They wanted to know whether the levels of these substances in blood and in the thick joint fluid that bathes the knee are tied to the size of osteophytes, the bony ridges that form at the edge of arthritic joints.
How the team measured bone changes and joint chemistry
The study enrolled 44 patients, most of them older women, all with end‑stage knee osteoarthritis so severe that they were scheduled for total knee replacement. On the day of surgery, the team drew blood and collected joint fluid directly from the knee. Using sensitive lab tests, they measured levels of MMP‑1, IL‑8, and IL‑18 in both fluids. To assess bone spur size, they analyzed standing X‑rays of each knee. Two experienced surgeons traced the area of the bony outgrowths on the inner side of the thigh bone and shin bone using a digital “freehand” measuring tool. Repeating the measurements showed that this method was reliable, with little difference between readers or over time.
What the numbers revealed about bone spurs
Several clear patterns emerged. First, IL‑18 levels in the blood were strongly linked to IL‑18 in the joint fluid, suggesting that inflammation inside the joint can spill over into the circulation. Within the joint fluid itself, higher levels of IL‑18 tended to go hand in hand with larger osteophytes on both the thigh and shin bones. This relationship remained even after accounting for patients’ age and body weight, especially for bone spurs on the thigh bone. In contrast, the other two molecules—MMP‑1 and IL‑8—did not show a meaningful connection with osteophyte size in this group of severely affected patients. Age was related to larger bone spurs, but body mass index and leg alignment were not, perhaps because all participants were already at an advanced disease stage.
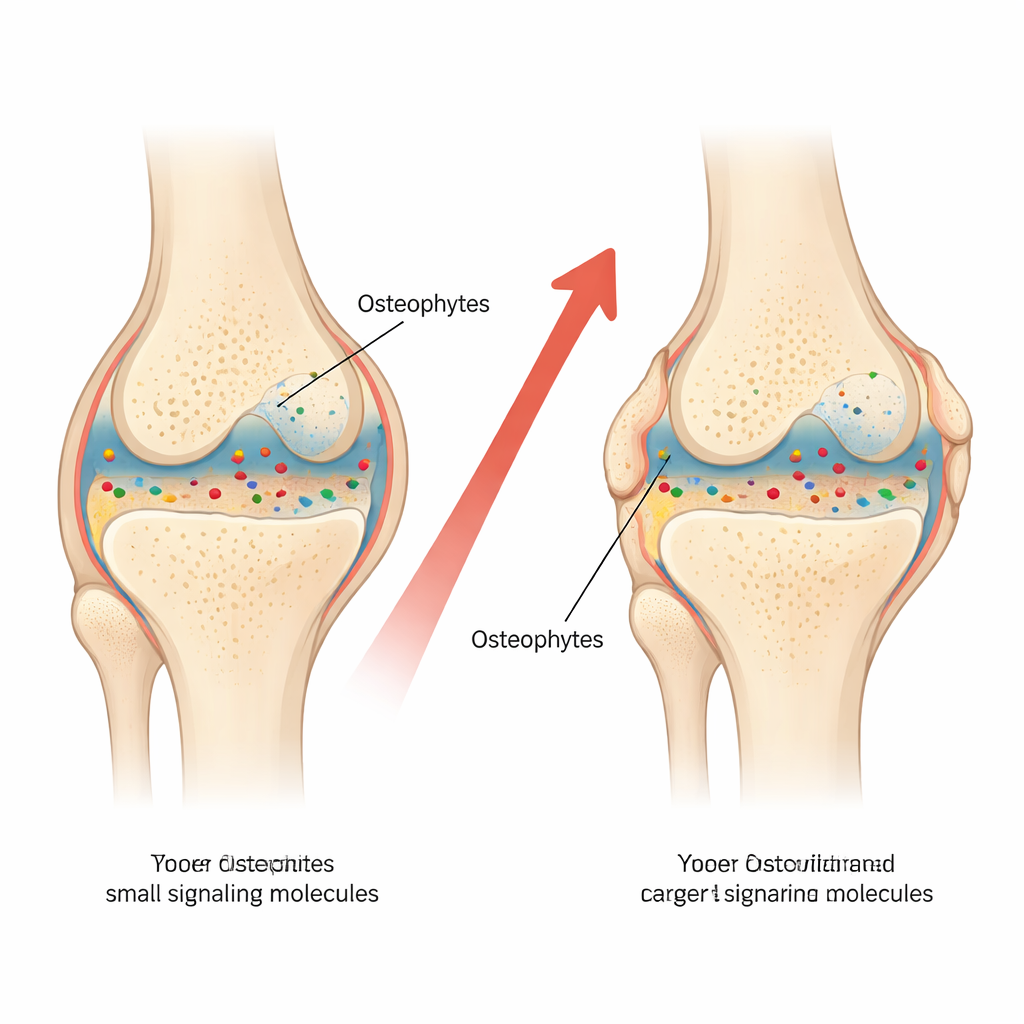
Inflammation, local chemistry, and growing bone
The fact that only IL‑18 in joint fluid—not in blood—tracked with osteophyte size points to the importance of the local chemical environment inside the knee. Osteophytes are thought to arise when stressed joint tissues send signals that trigger a process similar to growth plate activity in children’s bones. IL‑18 is known from other research to influence bone‑forming cells and the cells that make cartilage. The authors suggest that higher IL‑18 levels in joint fluid do not necessarily “cause” bone spurs on their own, but mark an active, inflammation‑rich setting that favors abnormal bone growth at the joint margins.
What this means for people with severe knee arthritis
For patients, the study’s message is that the bony enlargements seen on X‑rays are not just passive signs of aging. They appear to be linked to specific inflammatory signals, especially IL‑18, within the diseased joint. If future research confirms these findings, IL‑18 in joint fluid could become a useful indicator of how aggressively osteoarthritis is reshaping the knee and might even become a target for new drugs aimed at slowing or reshaping this process. While current treatments still focus largely on pain relief and joint replacement, understanding the chemistry that drives bone spur formation opens the door to more precise, biology‑based therapies in the years ahead.
Citation: Lim, DH., Youm, YS., Cho, SD. et al. Correlation of inflammatory mediators with osteophyte formation in end-stage knee osteoarthritis. Sci Rep 16, 6318 (2026). https://doi.org/10.1038/s41598-026-37394-1
Keywords: knee osteoarthritis, bone spurs, joint inflammation, interleukin-18, synovial fluid