Clear Sky Science · en
Investigation of the relationship between carotid intima-media thickness and angiopoietin-like factor 3 levels in metabolic dysfunction-associated steatotic liver disease
Why fatty liver and heart health matter
Many people have extra fat in their liver without realizing it, a condition now called metabolic dysfunction–associated steatotic liver disease (MASLD), formerly known as non‑alcoholic fatty liver disease. This seemingly silent problem is closely tied to obesity, diabetes, and abnormal blood fats—and it may quietly raise the risk of heart attack and stroke. The study in this article explores whether a liver-made protein in the blood, called ANGPTL3, and a simple ultrasound measure of neck artery wall thickness can help flag people with fatty liver and early blood vessel damage.
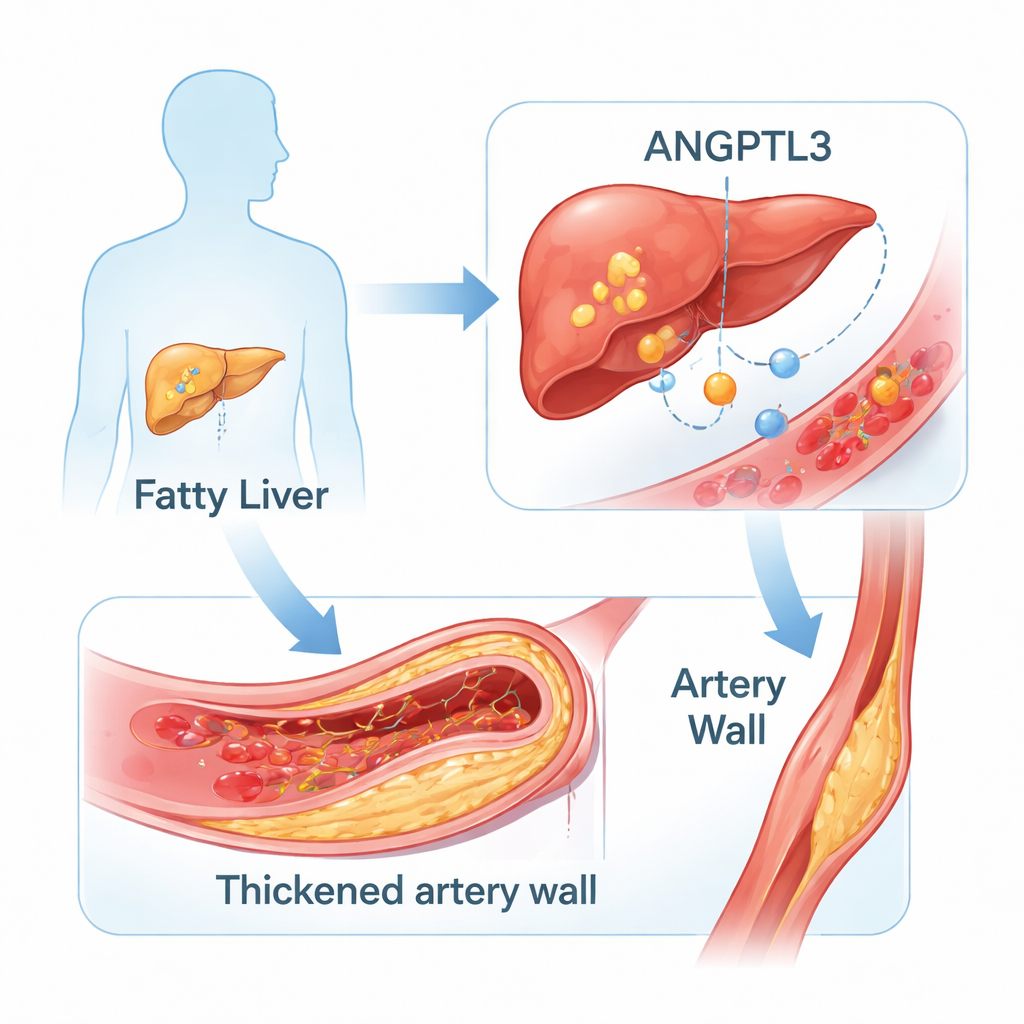
A closer look at fatty liver
MASLD describes a spectrum of liver changes that begins with simple fat build-up and can progress to inflammation, scarring, cirrhosis, and even liver cancer. It tends to occur in people with excess weight around the waist, high blood pressure, abnormal cholesterol, and insulin resistance—the cluster often called metabolic syndrome. Because liver biopsies are invasive, doctors increasingly rely on blood tests, body measurements, and ultrasound to detect fatty liver and estimate its severity in everyday practice.
A liver protein in the bloodstream
ANGPTL3 is a protein produced mainly by liver cells that helps control how the body handles fats in the blood. It slows down an enzyme that normally clears triglyceride-rich particles, so higher ANGPTL3 levels can lead to higher triglycerides and LDL (“bad”) cholesterol. Earlier research hinted that this protein might be linked to fatty liver, but the results were inconsistent and mostly based on small or mixed groups of patients. The authors of this study wanted to see whether people with MASLD have higher ANGPTL3 levels than healthy peers, and whether those levels track with early changes in the arteries.
What the researchers measured
The team studied 88 adults with MASLD and 88 healthy people of similar age and sex who did not drink alcohol or have chronic illnesses. They recorded height, weight, waist and hip size, blood pressure, and common blood tests including liver enzymes, cholesterol, triglycerides, blood sugar, and markers of inflammation. They also calculated a hepatic steatosis index, a simple score based on liver enzymes, body mass index, sex, and diabetes status, to estimate the likelihood of fatty liver. Importantly, they used ultrasound to measure carotid intima-media thickness (CIMT)—the combined thickness of the inner layers of the neck artery wall—which is widely used as an early indicator of artery damage and future cardiovascular risk.
Key findings about liver fat and artery walls
Compared with the healthy group, people with MASLD had higher body weight and body mass index, larger waists, more frequent diabetes and metabolic syndrome, and less favorable cholesterol and triglyceride levels. They also had higher blood sugar, a stronger marker of insulin resistance, and higher inflammatory markers such as C‑reactive protein. Crucially, their ANGPTL3 levels and carotid artery wall thickness were both significantly higher. Within the MASLD group, ANGPTL3 showed a strong positive relationship with CIMT: people with more of this liver protein tended to have thicker artery walls. Statistical tests suggested that a relatively modest increase in ANGPTL3 could help distinguish those with MASLD from healthy individuals, while CIMT and the hepatic steatosis index were even more accurate at doing so.
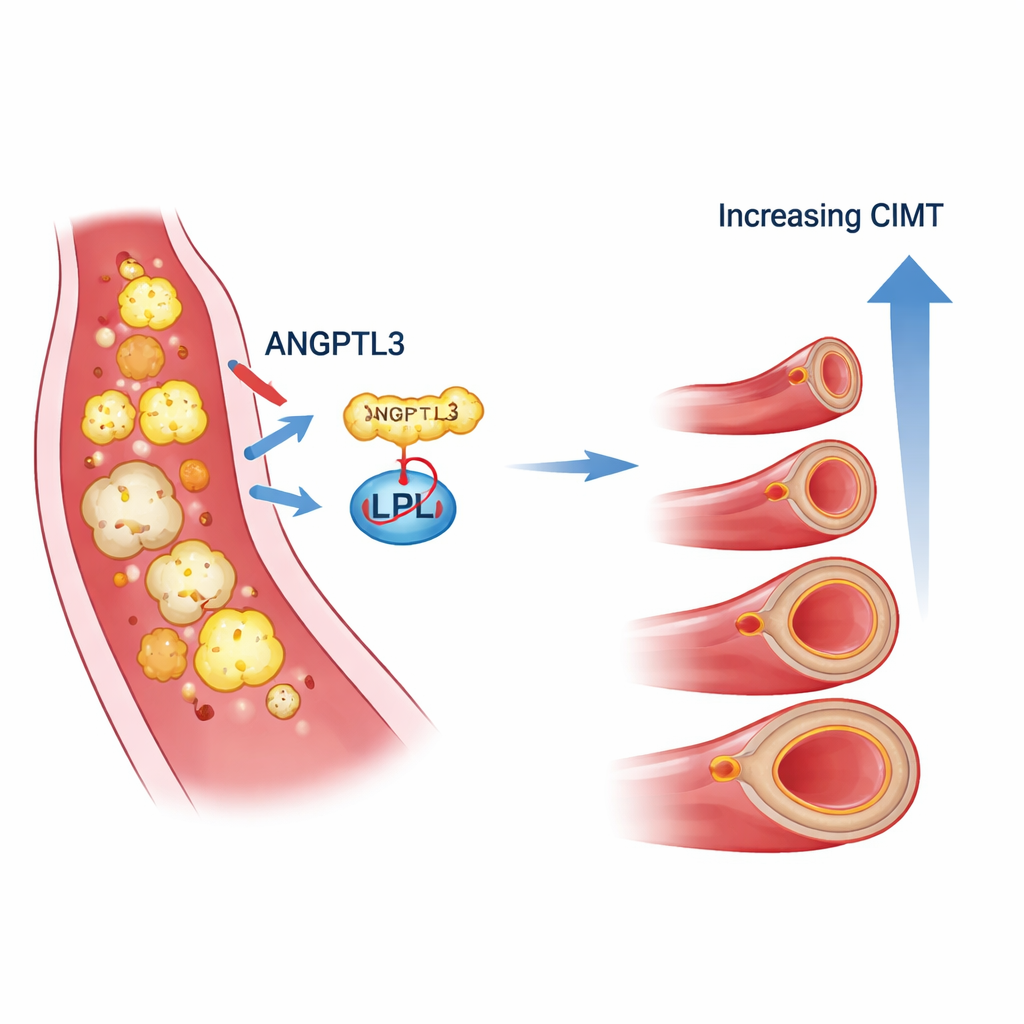
What this could mean for patients
Thickening of the neck artery wall is known to signal a higher chance of heart attack and stroke in the future, even before obvious plaque forms. The link between elevated ANGPTL3, fatty liver, and thicker artery walls in this study supports the idea that MASLD is not just a liver problem—it reflects a broader disturbance in metabolism that also affects blood vessels. Although this research cannot prove cause and effect, it suggests that ANGPTL3 may be one of the liver signals connecting unhealthy fat handling in the blood with early artery damage.
Take‑home message
For a layperson, the main conclusion is that extra fat in the liver goes hand in hand with an unfavorable blood fat profile and subtle changes in artery walls that may raise future heart and stroke risk. The study shows that levels of a liver-made protein, ANGPTL3, are higher in people with metabolic fatty liver disease and closely track with ultrasound signs of artery thickening. In time, ANGPTL3—and simple ultrasound measures like carotid intima-media thickness—may help doctors identify at-risk patients earlier and monitor how well lifestyle changes or new treatments are protecting both the liver and the heart.
Citation: Kadioglu Yeniyurt, E., Duran, E., Dumur, S. et al. Investigation of the relationship between carotid intima-media thickness and angiopoietin-like factor 3 levels in metabolic dysfunction-associated steatotic liver disease. Sci Rep 16, 6732 (2026). https://doi.org/10.1038/s41598-026-37389-y
Keywords: fatty liver disease, metabolic syndrome, cholesterol, cardiovascular risk, biomarkers