Clear Sky Science · en
Development and validation of a novel nomogram predicting axillary lymph node metastasis among breast cancer patients in Egypt
Why this matters to patients
For many women with breast cancer, the biggest fear after diagnosis is not only the cancer itself but also the long-term side effects of treatment. One of the most burdensome procedures is surgery to remove lymph nodes from the armpit, which can prevent cancer spread but often causes arm swelling, pain, and limited movement. This study explores whether a simple prediction tool could help doctors in Egypt better judge who truly needs this aggressive surgery—and who might safely avoid it.
The problem with “one-size-fits-all” surgery
Traditionally, surgeons have removed many lymph nodes from the armpit (a procedure called axillary lymph node dissection) to check whether breast cancer has spread. While effective at controlling disease, this operation is highly invasive and can leave patients with infections, chronic arm swelling (lymphedema), and shoulder problems that last a lifetime. A newer procedure, sentinel lymph node biopsy, removes fewer nodes but is still a surgery and is not always available in resource-limited settings. At the same time, modern screening means many women are diagnosed earlier, and more than three-quarters of the lymph nodes removed in some patients turn out to be cancer-free—evidence that many women may be overtreated.
A large Egyptian study seeking a smarter way
To tackle this issue, researchers at a major cancer center in Alexandria, Egypt, reviewed the records of 1,246 women treated for invasive breast cancer between 2018 and 2024. All had early to locally advanced disease (stages I–III) and underwent either full axillary dissection or sentinel node biopsy, so their lymph node status was known with certainty. The team collected detailed information that would typically be available around the time of surgery: patient age, tumor size and position within the breast, microscopic features, hormone and HER2 status, and imaging results from mammography and ultrasound. They then used statistical methods to search for combinations of factors that best predicted whether cancer had spread to the armpit nodes.
Building a risk “scorecard” for lymph node spread
From this analysis, five features emerged as the strongest independent clues to lymph node involvement: where in the breast the tumor sits (especially in the axillary tail or outer regions), how large it is, the tumor’s biological subtype, whether cancer cells are seen in tiny blood or lymph vessels, and whether ultrasound of the armpit shows suspicious-looking nodes. The researchers turned these factors into a visual scorecard, called a nomogram. Each factor adds a certain number of points; adding them up gives an individual woman’s estimated chance that her armpit nodes contain cancer. When tested against actual patient outcomes, the main model proved highly accurate, correctly separating women with and without node spread in more than 9 out of 10 cases—a level of performance that surpassed ultrasound alone and many previously published tools.
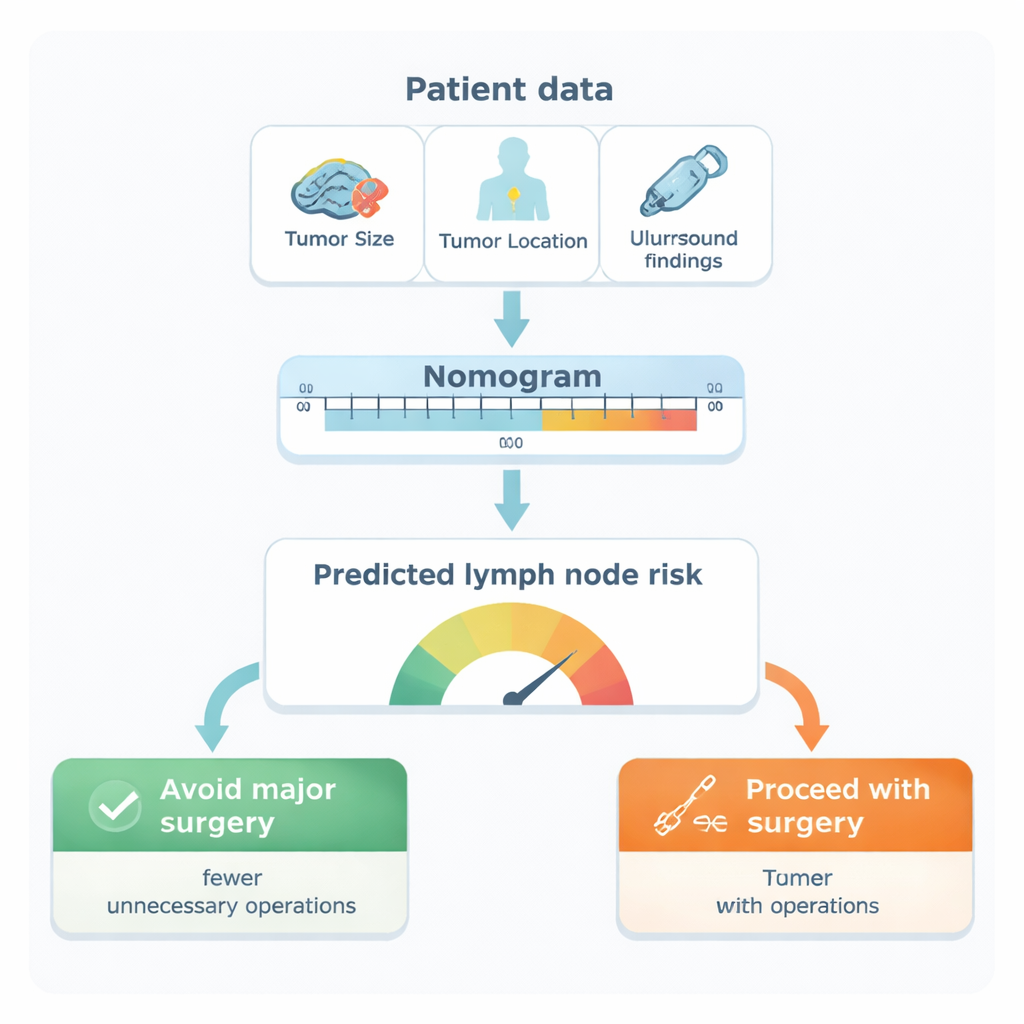
From numbers to decisions in the operating room
The team then asked how this scorecard could change real-world care. Using a method called decision curve analysis, they explored different “risk cutoffs” for choosing surgery. At a 20% risk threshold, the model would identify most women who truly had lymph node metastases (about 94% sensitivity) while sparing many women without spread from unnecessary dissection. In practical terms, women with a predicted risk below 20% would have only about a 1 in 8 chance of hidden node disease. According to the analysis, using the nomogram at this threshold could prevent roughly 11 avoidable axillary dissections for every 100 women evaluated, without meaningfully increasing the risk of missing serious disease.
What this means for patients and health systems
For patients, the study’s message is hopeful: in the future, a brief set of clinical and imaging findings could be combined into a simple risk score to guide more tailored surgery. Women at very low predicted risk of lymph node spread might avoid major axillary operations—and their long-term complications—especially in hospitals where more advanced techniques are scarce. Those at higher risk could still receive full staging and treatment. While the tool still needs to be tested in other hospitals and countries before it can be widely adopted, it offers a practical step toward more personalized, less damaging breast cancer care in Egypt and similar resource-limited settings.
Citation: Ismail, H.M., Arafa, M.A., Elsaid, A.A.A. et al. Development and validation of a novel nomogram predicting axillary lymph node metastasis among breast cancer patients in Egypt. Sci Rep 16, 7187 (2026). https://doi.org/10.1038/s41598-026-37354-9
Keywords: breast cancer surgery, lymph node metastasis, prediction nomogram, axillary management, Egypt oncology