Clear Sky Science · en
Oral HPV detection and genotyping by next-generation sequencing in a healthy Palestinian cohort: pilot study
Why the germs in your mouth matter
Most people have heard of the human papillomavirus (HPV) because of its link to cervical cancer, but far fewer know that HPV can also infect the mouth and throat and contribute to certain head and neck cancers. This study, carried out in Palestine, took a close look at HPV living in the mouth of healthy adults. By using cutting-edge DNA reading technology, the researchers wanted to see which types of HPV were present, how common they were, and whether a high-tech approach could work reliably in local clinics that currently have no HPV vaccination or screening programs.
Looking for a hidden virus
HPV is a very common virus family with more than 200 known types. Some types mainly cause harmless warts, while others are considered "high-risk" because they can, over time, help trigger cancers of the cervix, anus, or the mouth and throat. Oral HPV infections often cause no symptoms and can quietly persist for years, especially in people who smoke or have weakened immune systems. In Europe and North America, about 5–7% of healthy people carry HPV in their mouths, but there has been almost no data from Palestine. Without this basic information, it is hard for health authorities to plan vaccination campaigns, design screening programs, or even judge how serious a local HPV problem might be.
Collecting cheek swabs, not blood tests
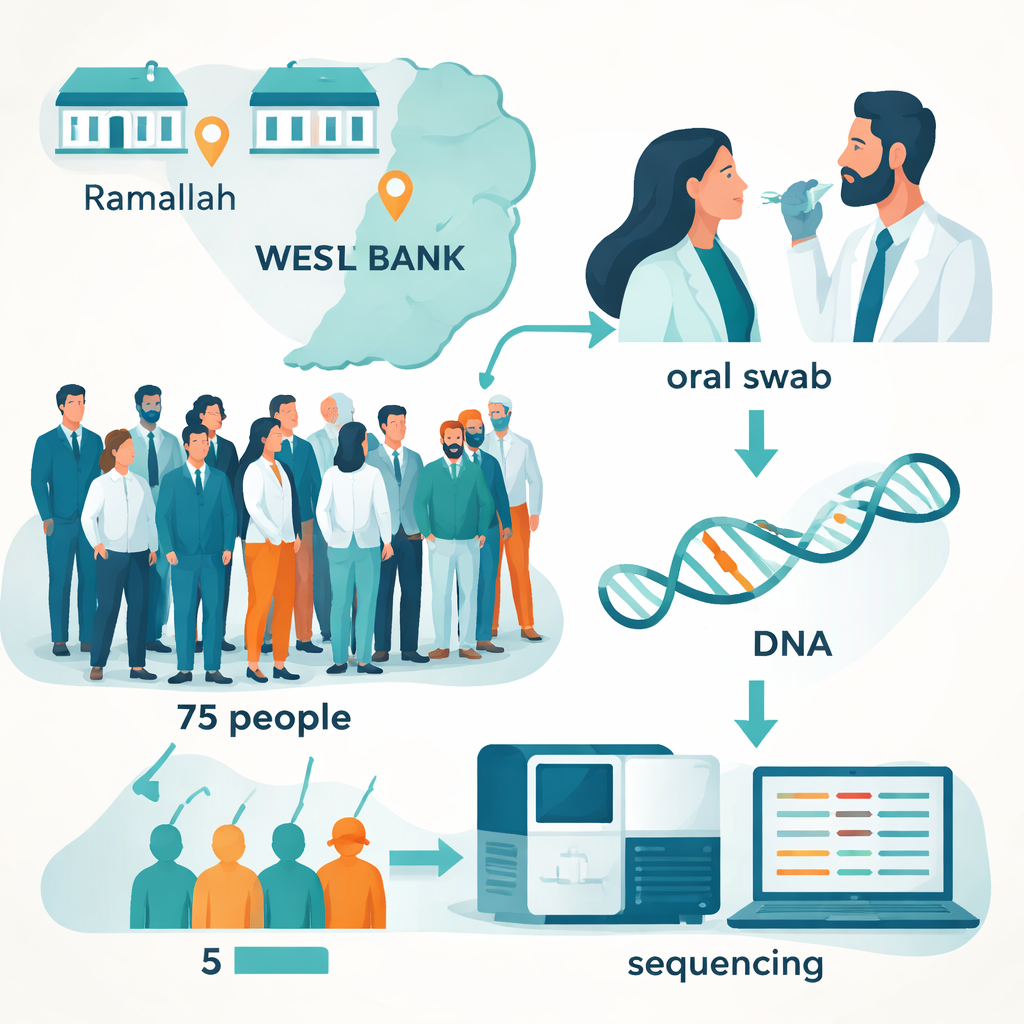
To begin filling this gap, the team recruited 75 adults who were visiting dental clinics in the central West Bank, in the cities of Ramallah and Bethlehem. All were over 18 and reported no major illnesses or history of cancer. Dentists gently rubbed sterile swabs along the inner cheeks, tongue, and floor of the mouth to collect cells. Each participant also answered a short anonymous questionnaire about age, gender, smoking, and basic HPV awareness and vaccination status. The study was intentionally small and designed as a "pilot"—its main purpose was to test whether a sophisticated laboratory method could reliably find and identify HPV in oral samples from this population, not to provide final national statistics.
Turning cheek cells into genetic clues
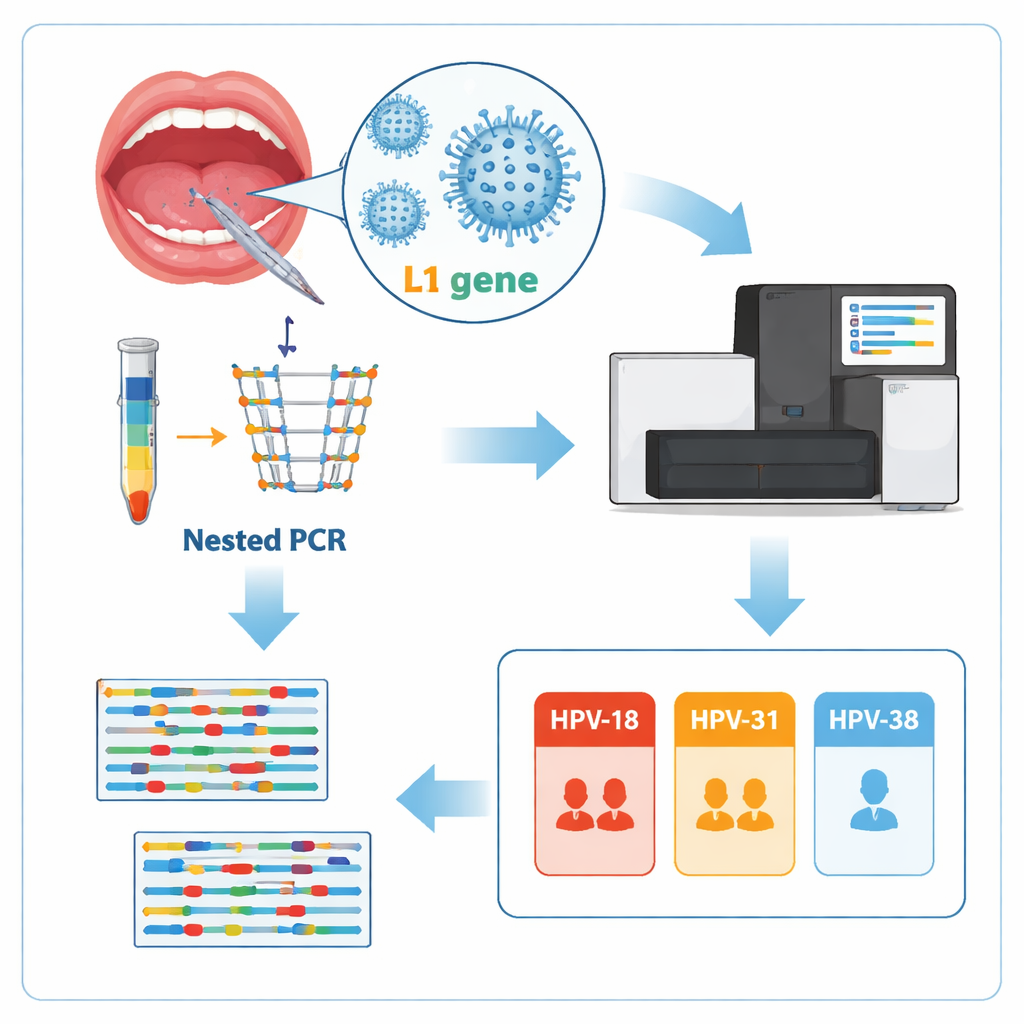
Back in the lab, the researchers extracted DNA from the swabs and used a two-step amplification process, known as nested PCR, to focus on a particular stretch of the virus’s genetic material called the L1 gene. This region acts like a fingerprint that distinguishes one HPV type from another. They then prepared the amplified DNA for next-generation sequencing (NGS), a high-throughput technology that reads millions of short DNA fragments in parallel. Using freely available online software, the team cleaned the raw data, pulled out reads that matched their HPV target, and compared those sequences to international databases to determine exactly which HPV types were present. To reduce the chance of false alarms from tiny bits of stray DNA, they only considered a sample truly positive if it contained at least 100 nearly identical sequence reads for a given HPV type.
What they found in healthy mouths
Out of the 75 people tested, 5 had clear evidence of oral HPV infection, corresponding to a rate of 6.7%, which is similar to reports from the United States and Iran. Three different HPV types were identified: HPV‑18 in two people, HPV‑31 in two people, and HPV‑38 in one person. Strikingly, HPV‑16—the type most strongly linked to head and neck cancers worldwide—was not detected in any of the samples. The types that were found include two well-known high-risk strains (HPV‑18 and HPV‑31) and one less familiar type, HPV‑38, which has been linked to certain skin and oral lesions. Using genetic comparison tools, the Palestinian virus sequences clustered closely with reference strains from other countries, confirming that the typing was accurate. Because only five people tested positive, the study could not reliably link HPV infection to age, sex, smoking, or other lifestyle factors, and most infected participants had never even heard of HPV.
Early signals and what they mean
This small study cannot tell us exactly how common oral HPV really is across Palestine, but it does show that high-risk HPV types are present in the mouths of otherwise healthy adults and that advanced DNA sequencing can be successfully run on local samples. The appearance of HPV‑38, which is not covered by current vaccines, and the absence of HPV‑16 in this small group hint that the mix of HPV types in the mouth may differ from what is seen in the cervix or in other countries. For lay readers, the main message is that HPV is not just a cervical issue: it can quietly infect the mouth as well, and modern tools now make it possible to track these infections more precisely. Larger, nationwide studies could build on this pilot work to guide vaccination policies, raise public awareness, and, ultimately, help prevent future HPV‑related cancers of the head and neck.
Citation: Safi, B., Khalid, M. & Nasereddin, A. Oral HPV detection and genotyping by next-generation sequencing in a healthy Palestinian cohort: pilot study. Sci Rep 16, 7282 (2026). https://doi.org/10.1038/s41598-026-37318-z
Keywords: oral HPV, head and neck cancer, Palestine, HPV genotyping, next-generation sequencing