Clear Sky Science · en
CDS-PD: a novel clinical decision support platform for Parkinson’s disease
Why a Smarter Diagnosis Tool Matters
Parkinson’s disease affects millions of people worldwide, and getting the diagnosis right—especially early on—can change the course of treatment, quality of life, and even who qualifies for promising clinical trials. Yet the official checklist doctors are supposed to use is long and complicated, so it is rarely followed step by step in busy clinics. This article describes a new computer-based assistant, called CDS-PD, designed to help neurologists apply those gold-standard rules consistently and accurately at the point of care.
Making Sense of a Complex Checklist
Modern guidelines for diagnosing Parkinson’s disease, created by an international movement disorders society, go far beyond simply noticing tremor or stiffness. They require doctors to confirm key features, rule out warning signs that suggest other brain disorders, and weigh a mix of supportive and negative clues. On paper, this process is time-consuming and easy to misapply, even for experienced specialists. As electronic health records have become standard in hospitals and clinics, one major piece has been missing: an integrated tool that can capture all the relevant details and automatically run the official diagnostic algorithm in real time.
Building a Digital Assistant for Neurologists
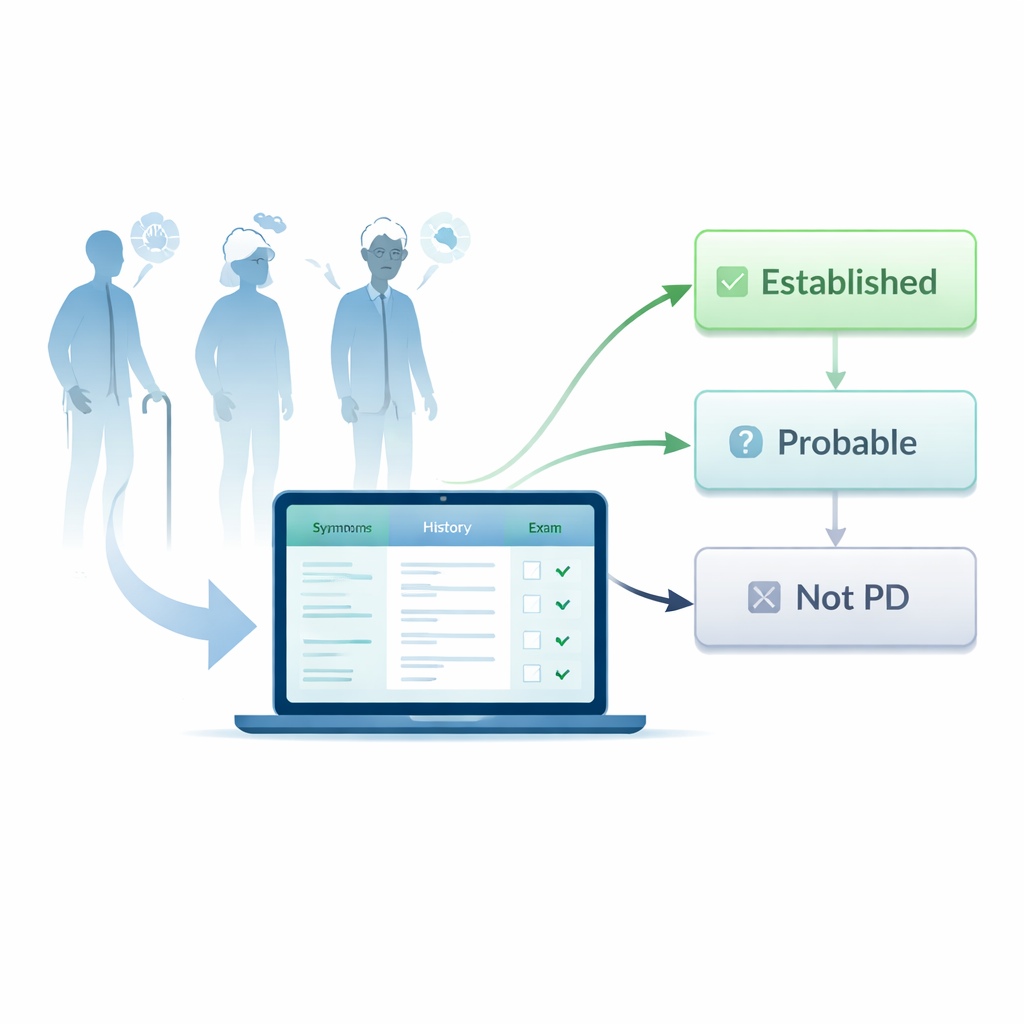
The research team created CDS-PD as a web-based platform that mirrors how movement disorder specialists actually see patients. The system organizes information into 11 clear sections, ranging from motor and non-motor symptoms to family history, environmental exposures, medications, examination findings, and test results. Within each section, users select from structured options, date pickers, and carefully checked fields instead of relying on free-text notes. Built-in quality checks ensure that required information is not skipped and that values fall within sensible ranges, reducing common data-entry errors that can undermine a diagnosis.
Turning Patient Data into a Clear Answer
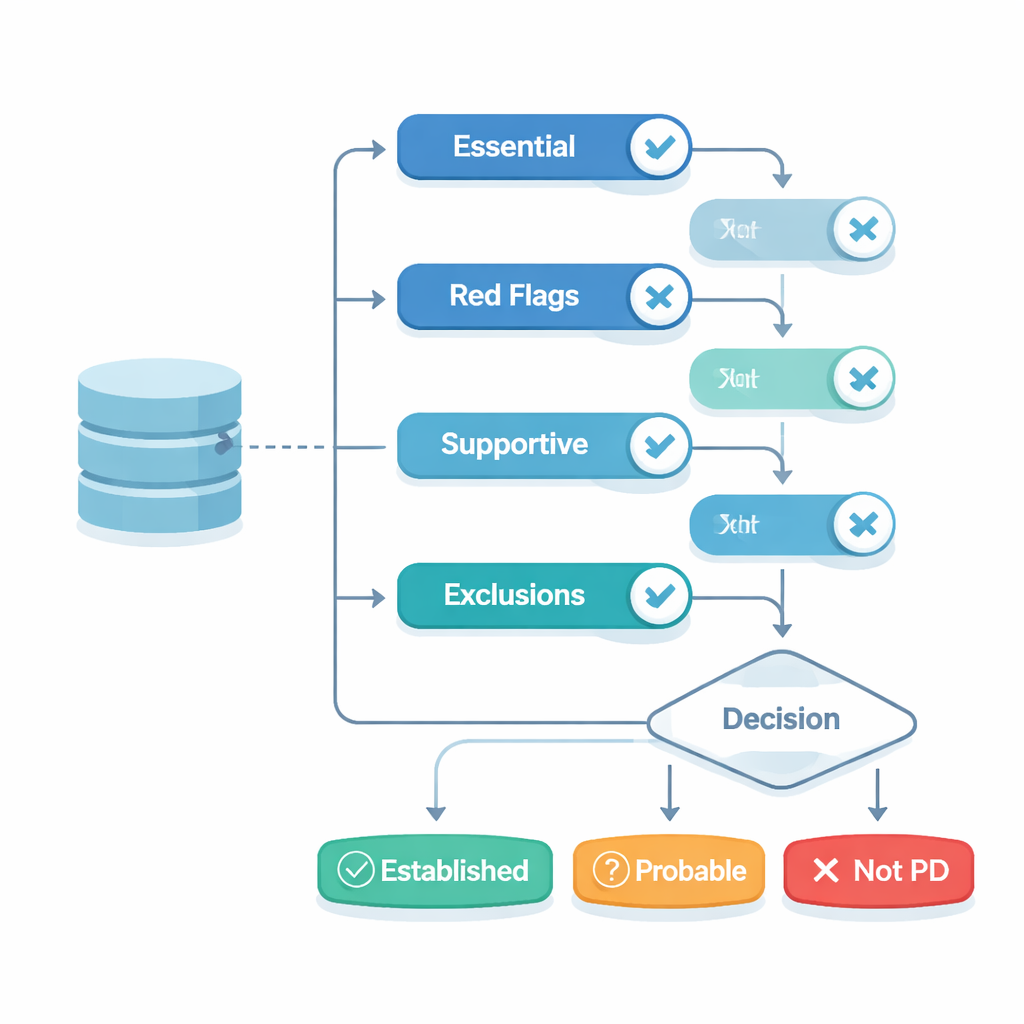
Behind the scenes, CDS-PD translates 24 separate elements of the official Parkinson’s criteria into yes–no questions tied directly to the stored data. These cover essential features that must be present, strong red flags that count against Parkinson’s, supportive clues that make the diagnosis more likely, and conditions that formally exclude it. The platform’s software then follows the same multi-step decision pathway set out in the guidelines to sort each patient into three groups: clinically established Parkinson’s, clinically probable Parkinson’s, or not Parkinson’s disease. If necessary information is missing or inconsistent, the system prompts users to fix it before issuing a result, making the process more reliable than a memory-based paper review.
Testing the Platform in Real Clinics
To see how well CDS-PD performs, the authors tested it in a multicenter research study of 43 people who had already lived with Parkinson’s symptoms for at least five years. Experienced movement disorder neurologists first made their diagnoses using the traditional paper checklist, and only afterward were the same data entered into the platform, so the clinicians were blinded to the software’s output. Across two medical centers, the platform’s decision matched the physicians’ final classification over 93 percent of the time. In the three cases where they disagreed, the computer flagged a rarely considered breathing symptom that had been documented but not weighed in the doctors’ paper-based scoring, highlighting how a systematic tool can reduce human oversight.
Looking Ahead to Earlier and Broader Use
While this first study is small and limited to people with long-standing disease, it shows that a thoughtfully designed decision support system can faithfully apply complex diagnostic rules and sometimes catch details clinicians overlook. The authors are already extending CDS-PD to help distinguish early Parkinson’s from related conditions, to sort patients into clinically meaningful subtypes, and eventually to plug directly into hospital record systems. For patients and families, the promise is straightforward: clearer, more consistent diagnoses delivered sooner, which can open doors to better-tailored care and participation in research aimed at slowing or preventing the disease in the first place.
Citation: Gupta, D.K., Golnari, P., Prantzalos, K. et al. CDS-PD: a novel clinical decision support platform for Parkinson’s disease. Sci Rep 16, 6553 (2026). https://doi.org/10.1038/s41598-026-37316-1
Keywords: Parkinson’s disease, clinical decision support, diagnostic criteria, neurology, health informatics