Clear Sky Science · en
Alcoholic and non-alcoholic acute pancreatitis mortality in the United States, 2006–2023: A nationwide trend analysis
Why this matters for everyday health
Most people never think about their pancreas until something goes wrong. Yet acute pancreatitis—a sudden, painful inflammation of this small organ—sends many adults to emergency rooms and can be deadly. This study looks at nearly two decades of U.S. death records to answer a simple but urgent question: who is still dying from pancreatitis, and why? The answers reveal a quiet shift toward alcohol-driven disease, rising risk in younger adults, and warning signs that our drinking habits may be undoing medical progress.
A closer look at a dangerous flare-up
Acute pancreatitis happens when the pancreas becomes abruptly inflamed, causing severe abdominal pain and, in the worst cases, failure of vital organs. Doctors classify cases as mild, moderately severe, or severe based on how long organ failure lasts and whether complications develop. Because fatal cases almost always involve lasting organ failure, tracking deaths over time offers a powerful window into how often the disease turns truly life-threatening, and whether that burden is shifting across age, sex, and communities.
National trends: good news and bad news
The researchers analyzed all U.S. death certificates from 2006 through 2023 in which acute pancreatitis was listed as the main cause of death—more than 52,000 deaths in total. Overall, the risk of dying from acute pancreatitis fell: after adjusting for changes in the age structure of the population, the national death rate dropped from about 1.5 to 1.2 deaths per 100,000 people. This decline likely reflects better hospital care, earlier triage to intensive care, and more standardized treatment for common non-alcohol causes such as gallstones. Yet the total number of deaths barely changed, indicating that progress in some groups is being offset by worsening outcomes in others.
Alcohol’s rising toll on the pancreas
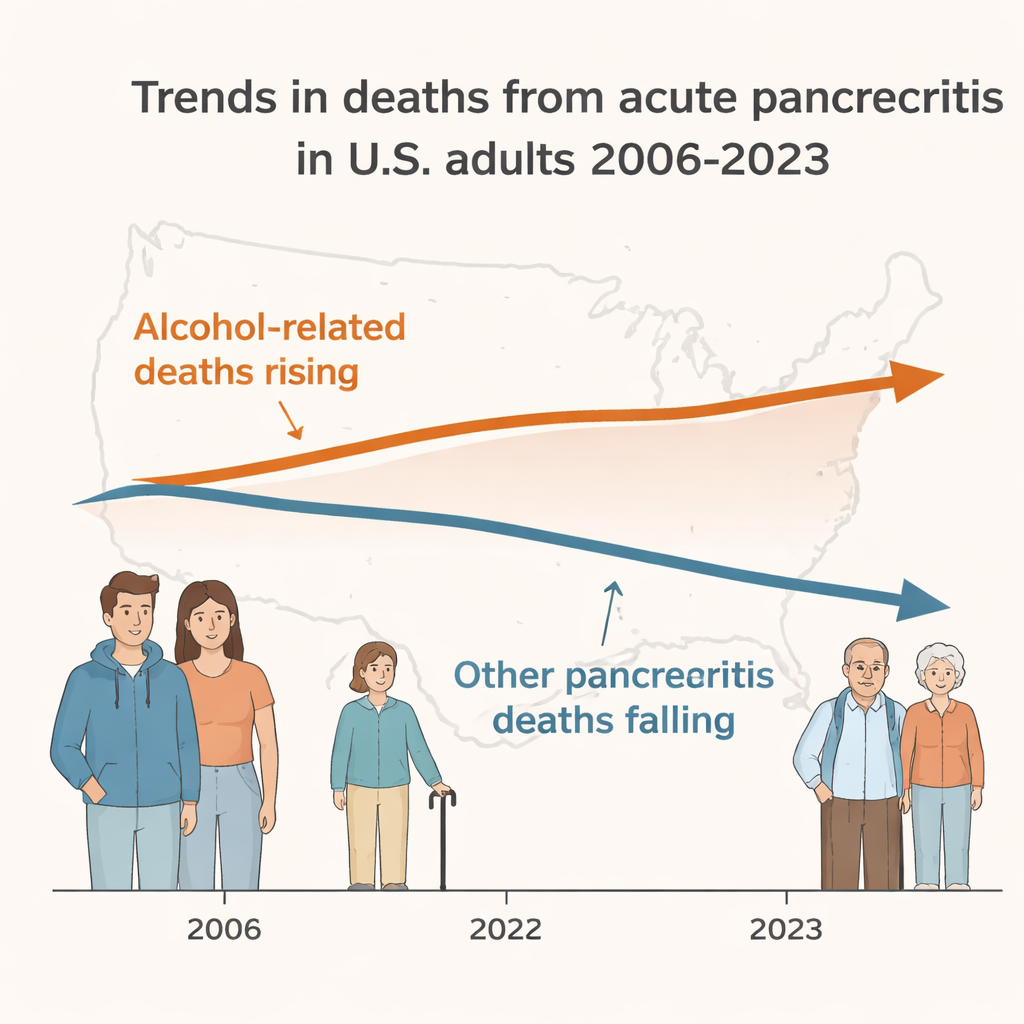
When the team separated alcohol-related acute pancreatitis from other types, a stark contrast emerged. Deaths from non-alcoholic pancreatitis fell, and their age-adjusted death rate declined steadily. Alcoholic pancreatitis moved in the opposite direction: deaths rose by more than 60 percent, and its death rate nearly doubled. This surge touched nearly every corner of society—men and women, cities and small towns, and all major U.S. regions. It was especially striking in adults aged 25 to 44, where deaths climbed sharply, suggesting that heavy drinking is increasingly turning a midlife organ injury into a cause of premature death just as people enter their peak working and family-raising years.
Who is most affected—and how the pandemic fit in
Most pancreatitis deaths still occurred among non-Hispanic White adults, but the absolute number of deaths rose among Hispanic individuals and those grouped as “non-Hispanic Other,” even though death rates (once age was accounted for) fell in all racial and ethnic categories. Rural counties continued to have slightly higher death rates than metropolitan areas, reflecting long-standing gaps in access to intensive care and advanced procedures, but alcohol-related deaths increased in both settings. Across nearly all groups, the authors saw a bump in death rates around 2019–2021, during the height of the COVID-19 pandemic, followed by a return toward the longer-term trend. That temporary spike likely reflects a mix of increased heavy drinking, delayed emergency care, and strained hospital resources.
What this means for prevention and policy
By design, the study cannot link individual drinking patterns or treatment delays directly to each death. Still, its population-wide view points clearly to a new reality: while doctors have become better at preventing deaths from gallstone- and procedure-related pancreatitis, alcohol-related disease is rising fast enough to threaten those gains. The authors argue that progress will now depend less on new intensive care techniques and more on how well we confront harmful drinking. That means weaving rapid addiction assessment and referral into pancreatitis care, expanding access to alcohol-use treatment, and strengthening community policies that reduce heavy drinking—especially among younger adults.
Takeaway: a preventable source of early death
To a layperson, the main message is straightforward: medical advances are steadily lowering the risk that a sudden attack of pancreatitis will be fatal—unless alcohol is involved. In that setting, deaths are climbing, younger adults are increasingly affected, and the pandemic appears to have poured fuel on the fire. The pancreas may be hidden deep in the abdomen, but what happens to it reflects choices and systems that can be changed. Tackling high-risk alcohol use and ensuring timely, high-quality care could prevent many of these deaths and keep the overall gains in pancreatitis survival from slipping away.
Citation: Yang, D., Zhang, F., Bai, L. et al. Alcoholic and non-alcoholic acute pancreatitis mortality in the United States, 2006–2023: A nationwide trend analysis. Sci Rep 16, 6427 (2026). https://doi.org/10.1038/s41598-026-37268-6
Keywords: acute pancreatitis, alcohol-related disease, mortality trends, public health, COVID-19 pandemic