Clear Sky Science · en
Sex-specific associations between maternal prenatal and postnatal psychological distress and autism spectrum disorder in the Japan Environment and Children’s Study
Why this study matters to parents
Many expectant and new mothers worry that their mood or stress levels might affect their child’s development. This large Japanese study followed more than 63,000 children to explore a specific question: does a mother’s psychological distress before and after birth relate to her child’s chances of being diagnosed with autism spectrum disorder (ASD) at age six, and does this differ for boys and girls?
Following families from pregnancy to school age
Researchers drew on the Japan Environment and Children’s Study, a nationwide project that has been tracking children’s health since before they were born. Pregnant women completed a short, six‑question survey three times: in early pregnancy (around 15 weeks), in later pregnancy (around 27 weeks), and when their child was one year old. This survey measured general psychological distress, including symptoms of depression and anxiety. Based on whether mothers scored above or below a standard cut‑off at each time point, families were grouped into eight patterns, or “trajectories,” of distress across the perinatal period. Doctors’ diagnoses of ASD were then reported by parents when children were 3, 4, 5 and 6 years old. In total, 3.76% of boys and 1.04% of girls in the study were diagnosed with ASD by age six, rates similar to those seen in other recent studies.
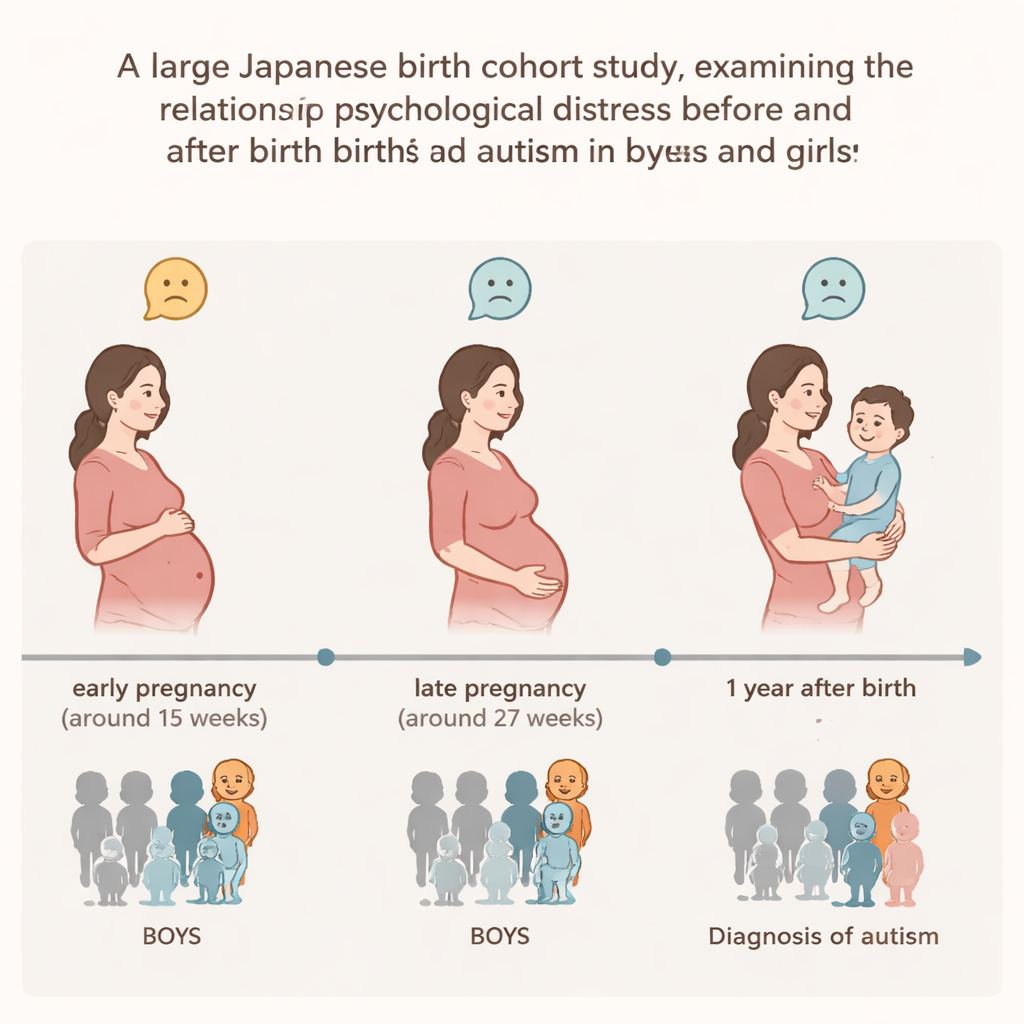
Different patterns for sons and daughters
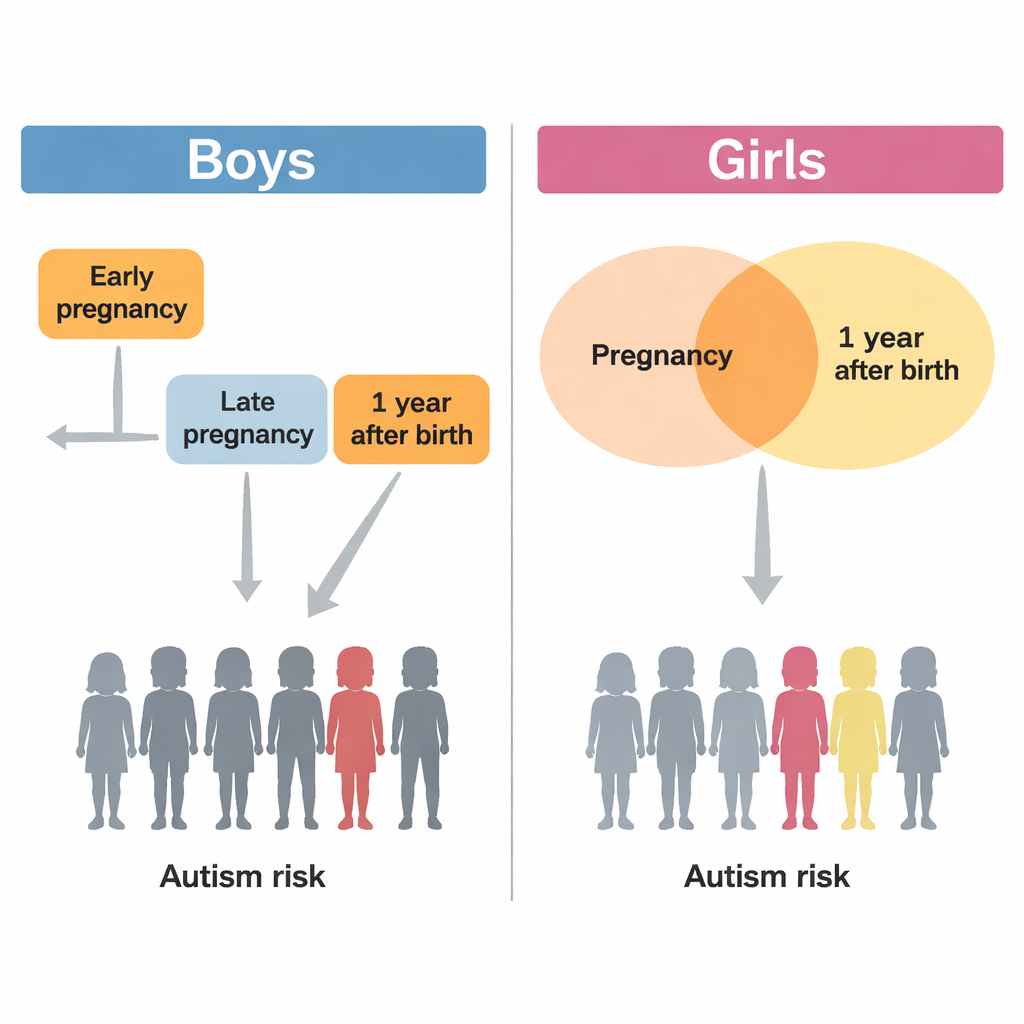
When the team analyzed the data separately for boys and girls, striking differences emerged. For boys, psychological distress in the first half of pregnancy was linked to higher odds of ASD at age six, even if the mother’s distress had eased by late pregnancy and she was well at one year after birth. Distress that continued through both early and late pregnancy was also associated with increased ASD risk in boys. In addition, boys whose mothers were distressed only at one year after birth—despite having relatively low distress during pregnancy—also had a higher likelihood of an ASD diagnosis. These associations remained even after accounting for many other factors, such as parents’ ages and education, income, pregnancy complications, and maternal mental health diagnoses.
For girls, timing and persistence both matter
For girls, the pattern was more conditional. Maternal distress during pregnancy by itself, no matter how strong or prolonged, was not clearly linked to ASD if the mother was not distressed at one year postpartum. Likewise, distress at one year postpartum on its own was not significantly associated with ASD in daughters. Instead, the increased risk appeared when mothers experienced distress both during pregnancy and again at one year after birth. In other words, for girls it was the combination of prenatal and ongoing postnatal distress—rather than any single period on its own—that was most closely tied to ASD diagnoses. This suggests that girls may be less affected by short‑lived prenatal stress but more sensitive to longer‑lasting difficulties that span pregnancy into early childhood.
What this might mean for care and prevention
These findings support the idea that a baby’s developing brain is shaped not only by genes but also by the emotional environment in the womb and early life—and that this influence is different for boys and girls. For boys, the first half of pregnancy seems to be a particularly sensitive window, while distress at one year after birth also appears important. For girls, ongoing distress that covers both pregnancy and the first year of life seems to matter more than temporary mood problems. The authors note that maternal distress likely acts together with inherited vulnerabilities and family circumstances rather than causing ASD on its own. Still, their results suggest that supporting women’s mental health before conception, throughout pregnancy, and into the toddler years could be one piece of a broader strategy to reduce ASD risk or severity, especially when interventions are tailored to the timing of distress and the sex of the child.
Take‑home message for families
For a lay reader, the central message is that feeling depressed, anxious, or overwhelmed around the time of pregnancy is common—and deserves attention not only for the mother’s sake but also for the developing child. In this very large Japanese cohort, boys showed higher ASD risk when their mothers were distressed early in pregnancy or at one year after birth, while girls were more affected when distress persisted from pregnancy into the postpartum period. These patterns do not mean that any individual episode of stress will cause autism, but they do highlight the value of early screening and accessible mental‑health support for prospective and new mothers as a way to promote healthier outcomes for both sons and daughters.
Citation: Nishigori, H., Nishigori, T., Kyozuka, H. et al. Sex-specific associations between maternal prenatal and postnatal psychological distress and autism spectrum disorder in the Japan Environment and Children’s Study. Sci Rep 16, 6899 (2026). https://doi.org/10.1038/s41598-026-37212-8
Keywords: autism spectrum disorder, maternal stress, prenatal mental health, postpartum depression, child development