Clear Sky Science · en
Determinants of cervical cancer screening among women living with HIV in Lesotho using nationally representative 2023/24 DHS data
Why this matters for women’s health
Cervical cancer is one of the few cancers that can often be prevented with simple screening tests, yet many women around the world still die from it. This is especially true for women living with HIV, whose weakened immune systems make them much more vulnerable. Lesotho, a small mountain country in Southern Africa, has one of the highest HIV rates on the planet. Understanding whether women with HIV there are actually getting screened for cervical cancer, and which women are being left out, offers important lessons for improving women’s health in low‑resource settings everywhere.
A closer look at women most at risk
The study used data from the 2023/24 Lesotho Demographic and Health Survey, a large, nationally representative household survey. The researchers focused on 611 women aged 25 to 49 who were living with HIV, because national guidelines recommend that screening for cervical cancer in this group begin at age 25. All information came from women’s own reports, including whether they had ever been screened. By drawing on this country‑wide survey, rather than data from a few clinics, the team could see how screening varies across different communities and social groups.

How screening coverage measures up
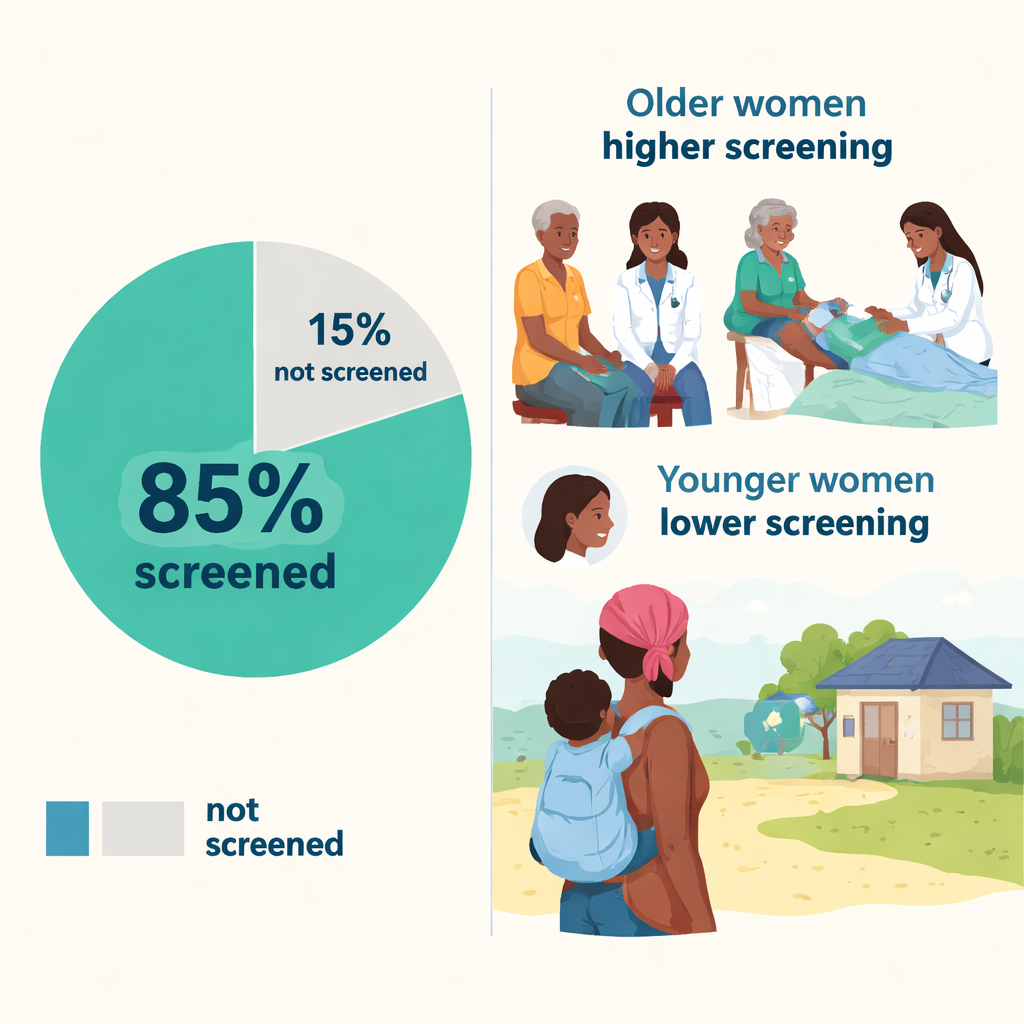
Contrary to expectations for a low‑income country, the study found that cervical cancer screening among women with HIV in Lesotho was strikingly high: about 85 percent said they had been screened at least once. Among those screened, more than 95 percent received a normal result, and only a tiny fraction had suspicious or clearly abnormal findings. Compared with reports from many other African countries, and even some European nations, this level of coverage is unusually strong. The authors suggest that one likely reason is that cervical screening has been deliberately built into HIV care, so that women are offered the test when they come for antiretroviral treatment and other routine services.
Who gets screened and who is left behind
High overall numbers, however, hide important gaps. Using a statistical approach that separates personal characteristics from community influences, the researchers identified several key patterns. Women in their early forties were more than four times as likely to have been screened as those in their late twenties, suggesting that younger adults are missing opportunities for early protection. Women who had also received a professional breast examination were over five times more likely to have undergone cervical screening, highlighting how one type of preventive care often opens the door to another. On the other hand, women with only one or two children were less likely to be screened than women with no children at all, and women living in rural areas had about half the odds of being screened compared with their urban counterparts, despite mobile outreach efforts.
Why these patterns matter
These findings point to deeper social and practical forces shaping who uses prevention services. Older women may have had more years of contact with the health system, more exposure to awareness campaigns, or personal experience with illness in themselves or relatives, all of which can motivate screening. Women who accept breast exams appear to be generally more engaged in preventive care, or may be visiting clinics that deliberately offer several checks at once. By contrast, women with fewer children may have fewer visits to reproductive health services where screening is offered, and rural women still face the familiar challenges of distance, cost, infrequent clinic visits, and limited information. The study also shows that differences between communities themselves explain a meaningful share of who gets screened, underlining the importance of local health systems and outreach.
What this means for saving lives
For a lay reader, the message is both hopeful and cautionary. Lesotho has made impressive progress in reaching women living with HIV for cervical cancer screening, showing that even a low‑income country with a heavy disease burden can approach global targets when services are integrated into existing HIV care. Yet younger women, those with fewer children, and women in rural communities are still more likely to miss out. The authors argue that bringing breast and cervical checks together in one visit, strengthening mobile and community‑based clinics in remote areas, and tailoring health education to women who may not see themselves as at risk could close these gaps. Doing so would not only prevent more cases of cancer but also move Lesotho—and similar countries—closer to a future in which no woman dies from a disease that can so often be detected and stopped in time.
Citation: Asefa, T., Endale, H.T., Mengstie, T.A. et al. Determinants of cervical cancer screening among women living with HIV in Lesotho using nationally representative 2023/24 DHS data. Sci Rep 16, 6429 (2026). https://doi.org/10.1038/s41598-026-37180-z
Keywords: cervical cancer screening, women living with HIV, Lesotho, rural health, preventive care