Clear Sky Science · en
Bilobalide attenuates steroid-induced osteonecrosis of the femoral head by upregulating the ERK/HIF-1α signaling pathway and promoting angiogenesis-osteogenesis coupling
Why this matters for people on long-term steroids
Many people rely on steroid medications to control asthma, autoimmune diseases, or after organ transplants. While lifesaving, these drugs can silently damage the hip joint, sometimes leading to the collapse of the femoral head—the ball of the hip—causing severe pain and disability. This study explores whether bilobalide, a natural compound from Ginkgo biloba, can help protect the hip from this steroid-induced bone damage and how it might work inside the body.
A hidden cost of powerful medicines
Long-term or high-dose steroid use can starve the femoral head of both healthy bone cells and blood supply. Over time, this can progress to steroid-induced osteonecrosis of the femoral head, in which bone tissue dies and the hip joint may eventually fail. Current treatment options are limited, and many patients end up needing joint replacement, sometimes at a relatively young age. Researchers are therefore looking for early, non-surgical strategies to preserve bone and blood vessels before the joint collapses.
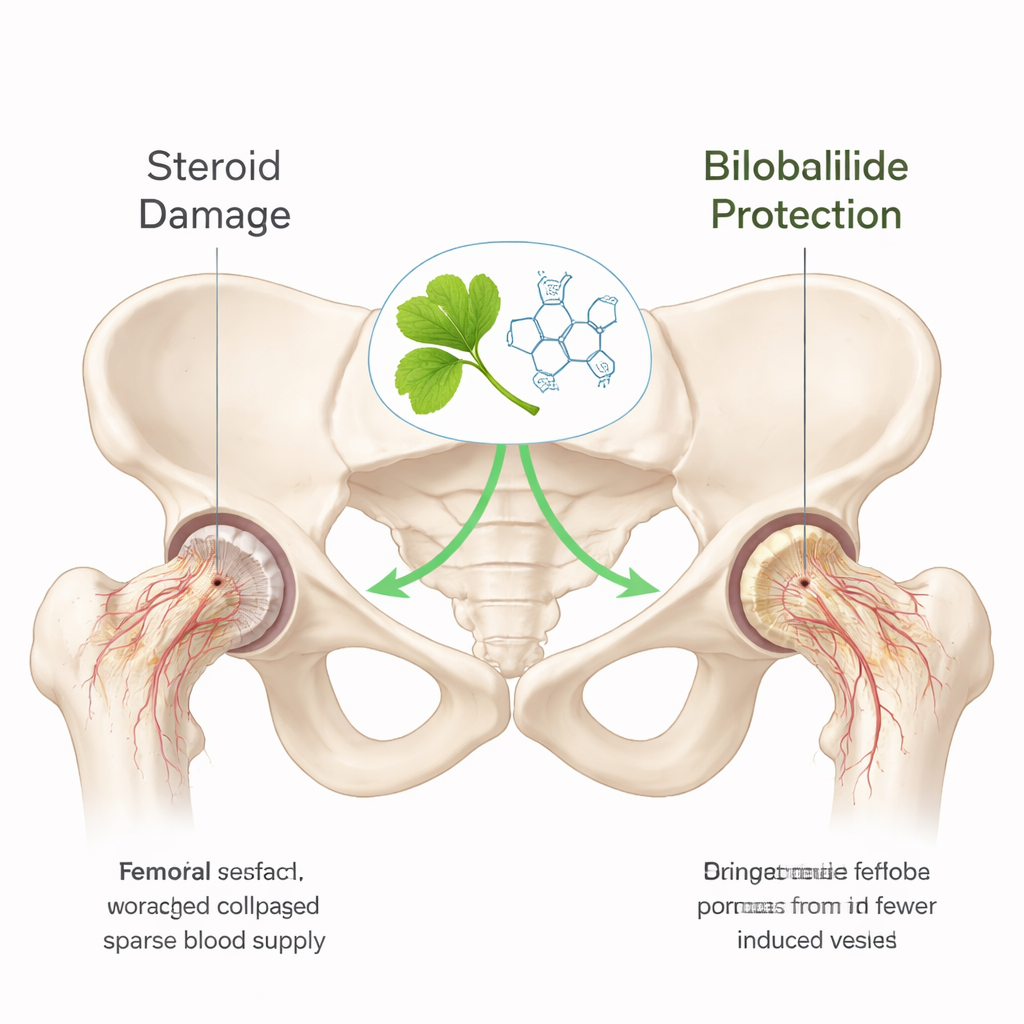
A plant molecule with a protective promise
Bilobalide is a small, ring-shaped molecule found in Ginkgo biloba extracts, already known for protecting cells from oxidative stress and encouraging the growth of new blood vessels. In this work, scientists first used large biological databases and computer modeling to predict how bilobalide might interact with human proteins linked to steroid-induced hip damage. They identified 94 shared targets between bilobalide and the disease, many of them involved in cell survival, blood vessel growth, and bone rebuilding. Computer docking simulations suggested that bilobalide could fit snugly into several key proteins, especially those tied to a cellular emergency system that helps tissues cope with low oxygen and stress.
Testing bilobalide in rat hips and bone cells
To see if these predictions held up in living tissue, the team created a rat model of steroid-induced hip damage using high-dose glucocorticoids. Some rats then received oral bilobalide. High-resolution CT scans showed that steroid-treated rats had weaker, more porous bone in the femoral head, while rats given bilobalide kept denser, better organized spongy bone. Classic tissue stains confirmed less bone collapse and fewer “empty” spaces where bone cells had died. Another test that specifically labels dying cells showed that bilobalide-treated rats had far fewer apoptotic (self-destructing) bone cells than untreated steroid-exposed animals.
Helping bone and blood vessels grow together
Healthy repair of the femoral head depends on a tight partnership between new bone formation and new blood vessel growth. The researchers examined markers of both processes in rat hip tissue. With bilobalide treatment, bone-forming cells showed higher levels of Runx2 and osteocalcin, proteins linked to active bone building and mineralization. Blood vessels in the same region expressed more CD31 and VEGF, indicators of a richer and more active microcirculation. These changes suggest that bilobalide encourages bone and blood vessels to rebuild together, helping to restore a supportive environment in areas threatened by steroid damage.
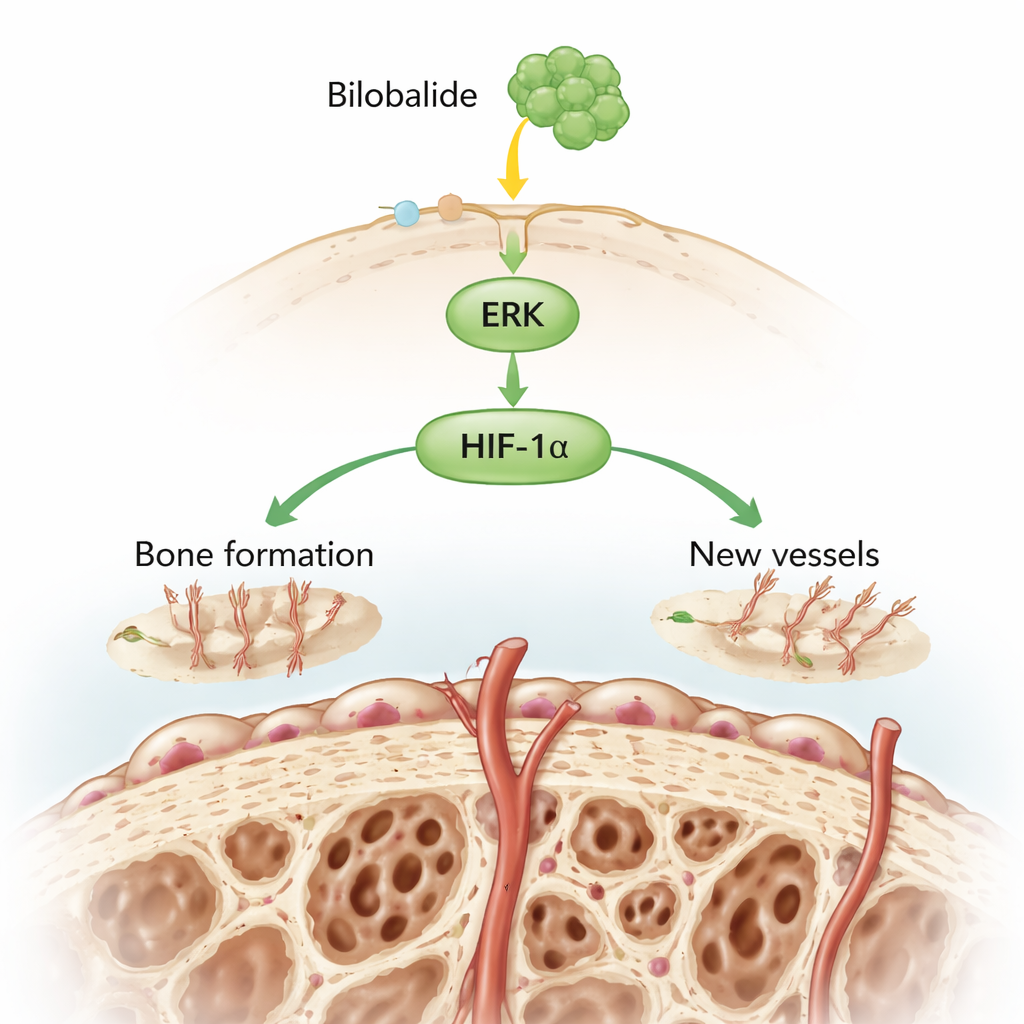
A key cell signal pathway switched back on
The team also studied bone-forming cells in the lab that had been damaged with the steroid dexamethasone. As expected, these cells became less viable and showed drops in activity in a signaling route known as the ERK/HIF-1α pathway, which normally helps cells survive stress and supports the growth of blood vessels. When bilobalide was added, cell survival rebounded, and the levels of activated ERK and HIF-1α protein rose again, while the total amount of ERK protein stayed the same. This indicates that bilobalide does not just increase protein levels randomly; it appears to switch this specific protective pathway back on, which in turn may stimulate both bone repair and new vessel formation.
What this could mean for patients
Together, these experiments suggest that bilobalide can blunt steroid-induced destruction of the femoral head by preserving bone structure, reducing bone cell death, and improving local blood supply, largely through reactivating the ERK/HIF-1α signaling pathway. While this work was done in rats and cultured cells, and more research is needed to confirm safety, dosing, and long-term effects in humans, it points to bilobalide as a promising natural candidate to help protect the hip joints of people who must rely on powerful steroid medications.
Citation: Chen, Q., Wang, B., Liang, H. et al. Bilobalide attenuates steroid-induced osteonecrosis of the femoral head by upregulating the ERK/HIF-1α signaling pathway and promoting angiogenesis-osteogenesis coupling. Sci Rep 16, 7755 (2026). https://doi.org/10.1038/s41598-026-37128-3
Keywords: steroid-induced hip damage, bilobalide, Ginkgo biloba, bone and blood vessel repair, osteonecrosis prevention