Clear Sky Science · en
Deep learning model for identification of metabolic bone disease of prematurity using wrist radiographs
Helping Fragile Newborn Bones
Very premature babies face many hidden health risks, and one of the most serious is weak, poorly mineralized bones that can fracture with little warning. Doctors often rely on wrist X‑rays to look for early damage, but the telltale signs can be faint and easily missed, especially in busy hospitals or where specialists are scarce. This study introduces a computer program based on deep learning that reads wrist X‑rays from preterm infants and helps doctors spot bone problems earlier and more accurately, potentially preventing painful fractures and long‑term complications.
Why Tiny Bones Need Extra Care
Metabolic bone disease of prematurity is a condition in which the bones of very small, very early babies do not mineralize properly. Because these infants miss out on the final weeks of pregnancy, when much of the body’s calcium and phosphorus is laid down in bone, they are especially vulnerable. The risk is highest in babies born before 28 weeks or weighing less than 1500 grams, and it peaks between four and eight weeks after birth. Blood tests can suggest trouble, but doctors usually confirm their suspicions with wrist X‑rays that show subtle changes in the growing end of the radius bone. Unfortunately, those changes may not appear until bone loss is already advanced, and even then they can be difficult for non‑experts to recognize.
Teaching a Computer to Read Wrist X‑Rays
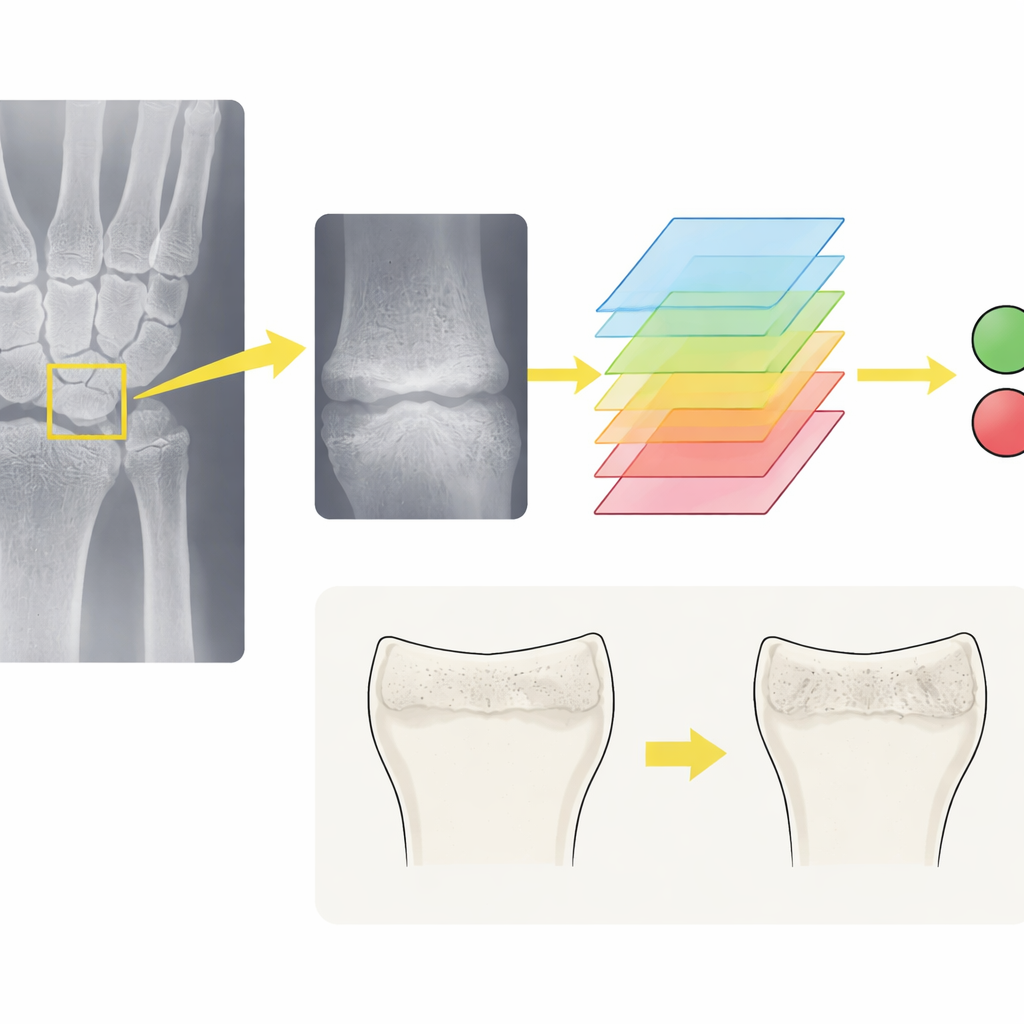
To tackle this problem, researchers in South Korea assembled a large collection of wrist X‑rays from more than a thousand very low birth‑weight infants treated at two major hospitals. Experienced specialists carefully reviewed 2239 images from 814 babies at one hospital, labeling each X‑ray as showing either normal bone or signs of metabolic bone disease. They drew a square around the key area at the end of the radius so the computer would focus on the same region human experts use. The team then trained several state‑of‑the‑art deep learning models on these cropped images, using standard techniques to slightly rotate, brighten, or blur the pictures so the algorithms would be robust to the messy reality of neonatal intensive care imaging.
How Well the Digital Reader Performs
Among the seven models tested, a network known as DenseNet‑121 performed best. On unseen X‑rays from the original hospital, it correctly discriminated between normal and abnormal images in about 92 percent of cases and was especially good at ruling out disease, rarely missing affected infants. When the model was challenged with X‑rays from a second hospital—with different equipment and patients—it still performed strongly, with high overall accuracy and an excellent ability to separate suspicious from normal images. Further analysis showed that when the model made correct calls, it concentrated on the same wrist region as human experts, suggesting it had learned medically meaningful patterns rather than random quirks of the data.
Giving Doctors a Smarter Second Opinion
The researchers then asked eight pediatricians and three radiologists to read wrist X‑rays twice: once on their own, and again with the model’s prediction displayed. With this digital assistant, clinicians became both more accurate and more consistent. On the original hospital’s images, average accuracy rose from about two‑thirds to more than four‑fifths, and the rate of both false alarms and missed cases dropped. Similar gains appeared when they interpreted images from the second hospital. The benefits were most striking for pediatricians, whose experience with skeletal imaging is often limited. For them, AI support turned a challenging, error‑prone task into one that more closely matched radiologist‑level performance, while slightly reducing reading time.
What This Could Mean for Preterm Babies
In plain terms, this study shows that a well‑trained computer program can act as a reliable second pair of eyes for doctors caring for fragile premature infants. While the model does not replace clinical judgment or blood tests, it makes it easier to flag X‑rays that deserve closer attention, especially in hospitals without ready access to pediatric radiologists. Earlier and more confident detection of bone weakness could prompt timely changes in nutrition, monitoring, and handling, reducing the risk of painful fractures and long‑term growth problems. With further refinement, larger datasets, and integration of blood markers, such AI tools could become standard companions in neonatal units worldwide, quietly working in the background to protect the smallest patients.
Citation: Park, S.G., Jeong, S., Cho, M. et al. Deep learning model for identification of metabolic bone disease of prematurity using wrist radiographs. Sci Rep 16, 7885 (2026). https://doi.org/10.1038/s41598-026-37116-7
Keywords: premature infants, bone health, medical imaging AI, wrist X-rays, neonatal intensive care