Clear Sky Science · en
PERK/ATF4/LAMP3-arm contributes to the aggressive phenotype of hepatocellular carcinoma cells in response to the chronic ethanol exposure
How Alcohol Can Make Liver Cancer More Dangerous
Many people know that heavy drinking can damage the liver, but fewer realize that alcohol can also change how liver cancers behave. This study looks at what happens inside liver cancer cells when they are exposed to alcohol over time. The researchers uncover a hidden stress pathway in the cells that makes tumors more invasive, more resistant to cell death, and more likely to return—and they show that blocking this pathway can dial that aggression back down in the lab.
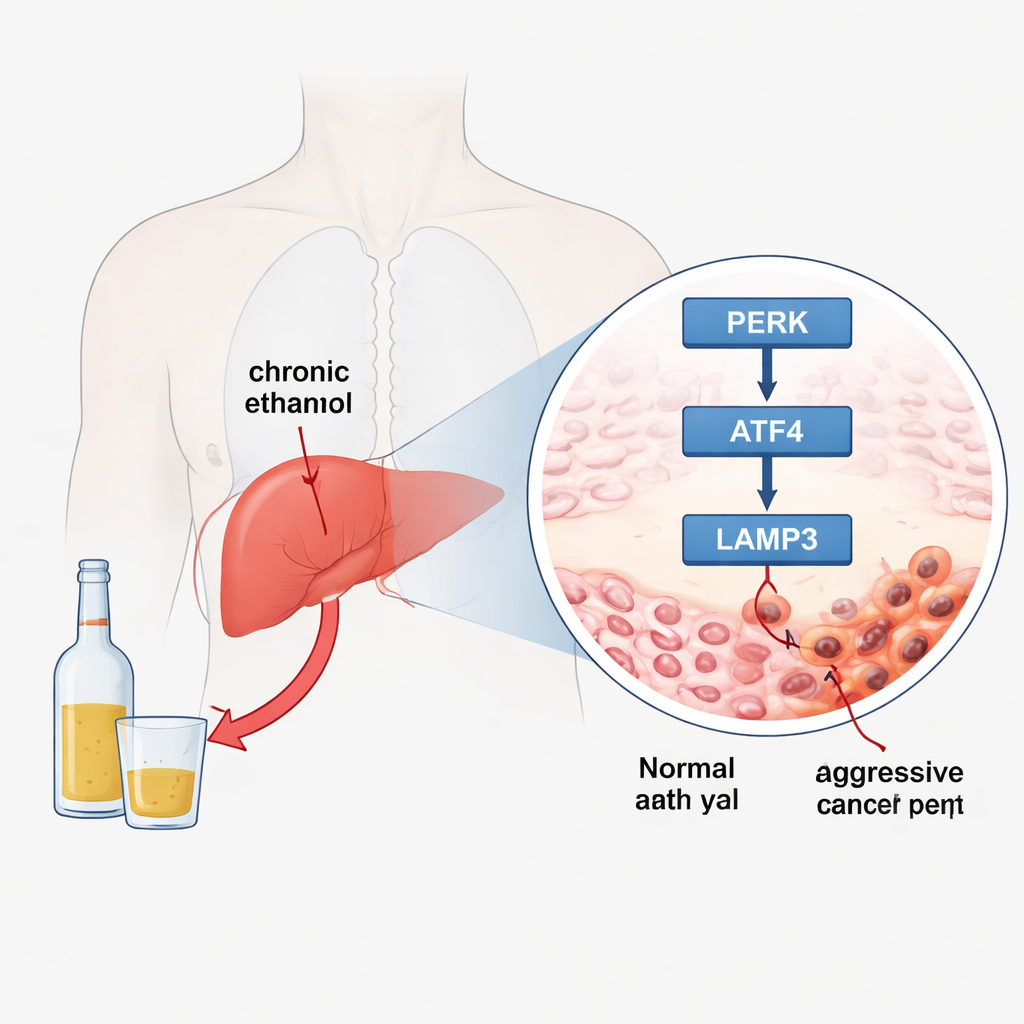
A Closer Look at Alcohol-Linked Liver Cancer
Liver cancer, particularly hepatocellular carcinoma, is one of the most common and deadly cancers worldwide. While infections such as hepatitis B and C have been widely studied as causes, cancers linked to long-term alcohol use remain less well understood. People who drink heavily experience ongoing damage in their liver cells, which are repeatedly stressed as they struggle to process alcohol and its toxic byproducts. The authors wanted to know whether this constant stress flips specific molecular switches that push alcohol-associated liver cancers into a more aggressive state than tumors arising from other causes.
Cellular Stress: When the Protein Factory Misfires
Inside every cell, the endoplasmic reticulum acts like a protein-folding workshop. When this workshop is overwhelmed, a built-in alarm system called the unfolded protein response switches on. One branch of this alarm, named the PERK–ATF4–LAMP3 arm, can either help cells survive stress or, if pushed too far, drive them to self-destruct. The researchers exposed three human liver cancer cell lines to different doses of ethanol for several days, mimicking chronic drinking. In two of these models, they saw strong activation of the PERK–ATF4–LAMP3 arm, along with boosts in factors linked to inflammation (NF‑κB), new blood vessel growth (VEGF‑A), and fat and cholesterol production (through SREBP genes). At the same time, the cells accumulated more triglycerides and cholesterol, echoing fatty liver changes often seen in heavy drinkers.
From Calm Cells to “On-the-Move” Tumors
Turning on this stress pathway did more than change gene readouts—it changed how the cancer cells behaved. With chronic ethanol exposure, liver cancer cells became markedly better at moving and invading through barriers in lab assays, traits that mirror metastasis in the body. They also formed many more spheres in special low-attachment cultures, a sign of increased “stemness,” meaning a larger pool of hardy, relapse-prone cancer cells. At the same time, fewer cells underwent programmed cell death, allowing damaged and dangerous cells to survive. The cells generated more reactive oxygen species—chemically reactive molecules that can further damage DNA and proteins—creating a vicious cycle of stress and survival that favors tumor progression.
Switching Off the Stress Arm to Tame the Tumor
The team then tested whether shutting down the PERK arm could reverse these alcohol-driven changes. They treated ethanol-exposed liver cancer cells with an orally available PERK inhibitor called GSK2606414. This drug reduced activation of key downstream players (ATF4 and LAMP3), lowered oxidative stress, and cut back the expression of many genes tied to tumor growth and inflammation. Functionally, cancer cells became less invasive and less mobile, and their ability to form cancer stem–like spheres collapsed—no spheres formed at all under PERK blockade. Importantly, inhibition also restored apoptosis, meaning more damaged cells were eliminated instead of lingering. Normal, untreated cells exposed only to the inhibitor did not show major harmful changes, suggesting that this approach mainly targets stress-primed, alcohol-exposed tumor cells.
What This Could Mean for People Who Drink Heavily
For non-specialists, the key message is that long-term alcohol exposure does more than just raise the risk of liver cancer—it can hardwire existing liver tumors into a tougher, harder-to-treat form by activating a specific stress pathway inside cells. This study, done in cell lines, shows that blocking the PERK–ATF4–LAMP3 arm can soften that aggressive behavior and re-open the door to cell death. While these findings still need to be confirmed in animals and, eventually, in patients, they point toward new drug strategies that could be especially useful for people with alcohol-associated liver cancer, complementing efforts to reduce or stop alcohol intake and improve overall liver health.
Citation: Goyal, H., Kaur, J. PERK/ATF4/LAMP3-arm contributes to the aggressive phenotype of hepatocellular carcinoma cells in response to the chronic ethanol exposure. Sci Rep 16, 6188 (2026). https://doi.org/10.1038/s41598-026-37114-9
Keywords: alcohol-associated liver cancer, cell stress pathways, PERK pathway, tumor aggressiveness, liver cancer therapy