Clear Sky Science · en
Serum interferon-λ3 as a short-term biomarker of disease control in anti-MDA5-positive dermatomyositis-associated ILD
Why this matters for patients and families
Some people with a rare muscle and skin disease called dermatomyositis develop serious scarring and inflammation in their lungs. This lung problem can worsen quickly and become life-threatening, so doctors need a fast and reliable way to see whether early treatment is actually working. This study explored whether a substance in the blood, called interferon‑lambda 3, can act like an early warning light on the dashboard, helping doctors tell—within just a month—who is doing well and who is still in danger.
A rare disease with dangerous lung involvement
Dermatomyositis is an autoimmune disease: the body’s own defenses mistakenly attack muscles, skin, and sometimes the lungs. A subset of patients carry antibodies against a protein known as MDA5 and are especially prone to developing interstitial lung disease, in which the lung tissue becomes inflamed and stiff. For these patients, the first weeks after diagnosis are critical. Powerful immune‑suppressing drugs are started quickly, but it can be difficult to know early on whether these treatments are truly calming the lung inflammation or whether the disease is marching on silently beneath the surface.
Hunting for a short-term blood signal
The researchers focused on a molecule called interferon‑lambda 3 (IFN‑λ3), part of the body’s antiviral defense system that also influences inflammation at barrier tissues such as the lungs. Earlier work showed that IFN‑λ3 levels are unusually high in people with MDA5‑positive dermatomyositis and that high levels at diagnosis are linked to worse outcomes. In this study, the team asked a new question: do changes in IFN‑λ3 within the first month of treatment track with how well a patient’s lung disease is controlled? To find out, they looked back at 24 patients treated at several hospitals over more than two decades, all of whom had blood samples stored from the time of diagnosis and again about one month after starting therapy.
Two paths: good control and poor control
The patients were divided into two groups based on what happened to their lung disease over the following year. The “good control” group included people who survived and had no lung flare‑ups for at least twelve months. The “poor control” group included those who either died from worsening lung disease or had a clear relapse within a year. At diagnosis, IFN‑λ3 levels were generally high in both groups. But by one month, a sharp split emerged. In the good‑control group, median IFN‑λ3 levels dropped from about 95 to 13 units, a strong and rapid fall. In the poor‑control group, levels barely changed, staying high—around 130 down to 119. Even patients in this group who showed some decrease still had clearly elevated levels after a month.
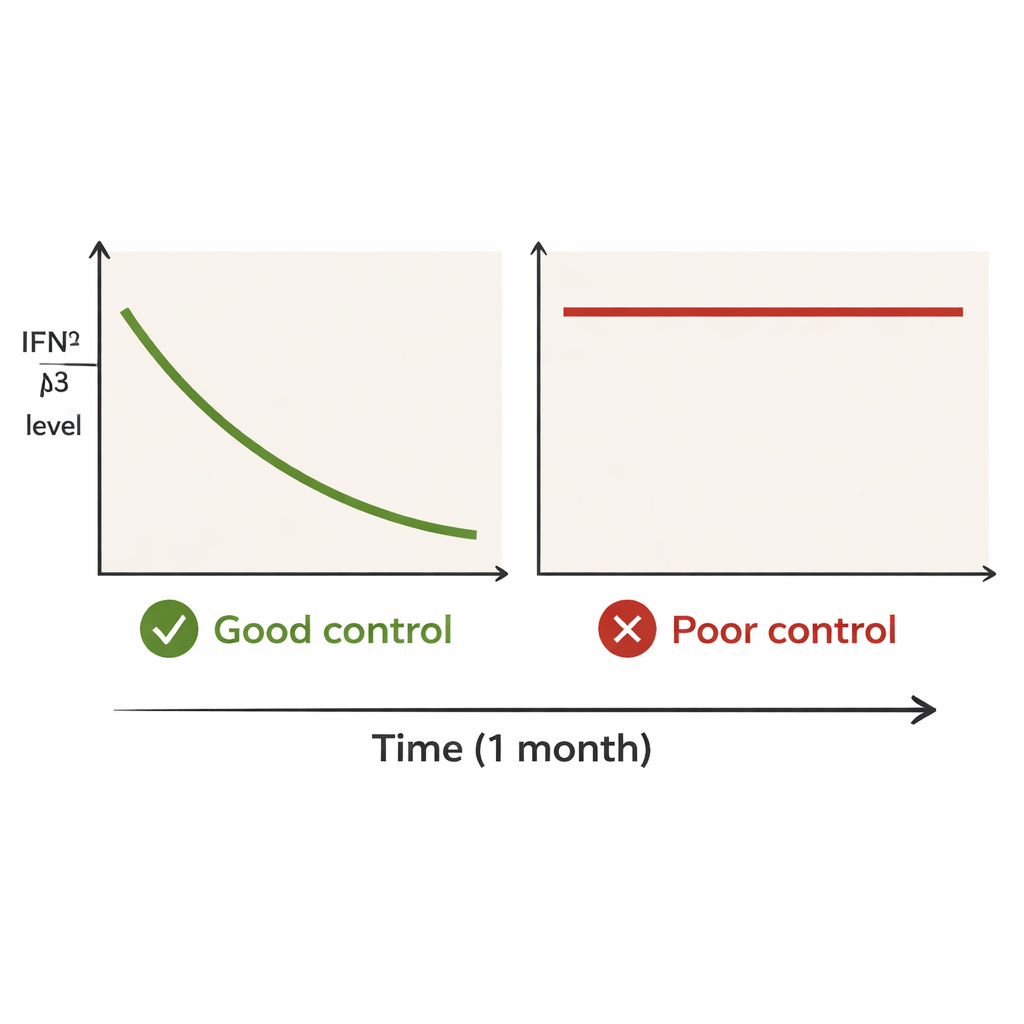
How this marker compares with others
Doctors already use other blood tests, such as ferritin and KL‑6, to help estimate the severity of this kind of lung disease. However, in this study those markers hardly changed over the first month and did not clearly separate the two outcome groups. IFN‑λ3 behaved differently: it fell quickly in patients whose disease came under control and stayed high in those who later died or relapsed. This suggests that the absolute IFN‑λ3 level at one month—how high or low it is at that point—may be more informative than simply whether it has gone up or down a little from baseline. Importantly, this pattern held even though many of the sicker patients received more aggressive drug combinations.
What this could mean for care
The study was relatively small and looked back at past patients, so its findings need to be confirmed in larger, prospective studies. Still, the results point toward a practical use: measuring IFN‑λ3 at diagnosis and again about a month later could give doctors an early readout of whether current treatment is doing enough. If levels remain high, that might prompt closer monitoring, adjustment of medicines, or consideration of additional therapies before irreversible lung damage occurs. For patients and their families, a simple blood test that reflects short‑term disease control could offer clearer guidance and a better chance of staying ahead of a dangerous lung complication.
Citation: Kitahara, Y., Fujisawa, T., Fukada, A. et al. Serum interferon-λ3 as a short-term biomarker of disease control in anti-MDA5-positive dermatomyositis-associated ILD. Sci Rep 16, 6134 (2026). https://doi.org/10.1038/s41598-026-37104-x
Keywords: dermatomyositis, interstitial lung disease, biomarkers, interferon lambda 3, autoimmune lung disease