Clear Sky Science · en
Conditional survival and prognostic nomogram for distant metastatic differentiated thyroid cancer after total thyroidectomy
Why this matters to patients and families
Thyroid cancer is often thought of as a “good cancer” with excellent survival, but some people develop distant spread to organs like the lungs or bones. For these patients and their families, the biggest questions are, “How long might I live?” and “Do my chances get better if I’ve already made it through the first few years?” This study looks beyond simple five‑ or ten‑year survival numbers and offers a more hopeful, evolving picture of risk over time, along with a practical tool doctors can use to tailor follow‑up care.
Looking at survival as a moving target
Traditional cancer statistics give a single survival estimate from the day of diagnosis, such as the chance of being alive five or ten years later. These snapshots are useful early on, but they become less informative for someone who has already survived several years after treatment. The researchers used a newer approach called “conditional survival,” which essentially asks, “Given that a person has already lived x years, what are the chances they will live y more years?” By updating the outlook as time passes, this method aims to reflect the real experience of long‑term survivors more accurately than fixed, one‑time estimates.
Who was studied and how
The team analyzed records from 1,235 people in the large U.S. SEER cancer registry who had differentiated thyroid cancer that had spread to distant sites and who had undergone complete removal of the thyroid gland. Most patients were over 55 years old, most had the common papillary type of thyroid cancer, and about three‑quarters received radioactive iodine treatment after surgery. Using standard survival analysis, they first measured overall survival at 3, 5, and 10 years after diagnosis. They then calculated conditional survival, showing how the chance of reaching 10 years changed for patients who had already lived one, two, or more years after their surgery.
Good news that grows with time
The initial outlook for patients with distant spread was clearly worse than for typical thyroid cancer: only about 47% were expected to be alive at 10 years when looking from the time of diagnosis. But when the researchers applied conditional survival, a very different picture emerged. For those who survived the first few years, their chances of ultimately reaching 10 years steadily climbed. After surviving one year, the estimated 10‑year survival rose above 51%; after several more years, it kept improving, eventually exceeding 90% for patients who had already lived nine years. In other words, making it through each additional year after surgery was associated with a better and better long‑term outlook, a pattern that can offer real reassurance to patients living with metastatic disease.
A personalized prediction tool
To move from group statistics to individual forecasts, the investigators built a visual prediction aid called a nomogram. Drawing on modern statistical methods, they identified five key factors that influenced survival: age, sex, the microscopic type of thyroid cancer, the size of the original tumor, and whether the patient received radioactive iodine therapy. Each factor was assigned a number of points, and the total score translated into a personalized estimate of the chance of being alive at 3, 5, and 10 years, updated for how long the patient had already survived. The tool was rigorously tested in separate patient groups and showed good accuracy in distinguishing those more likely to live longer from those at higher risk.
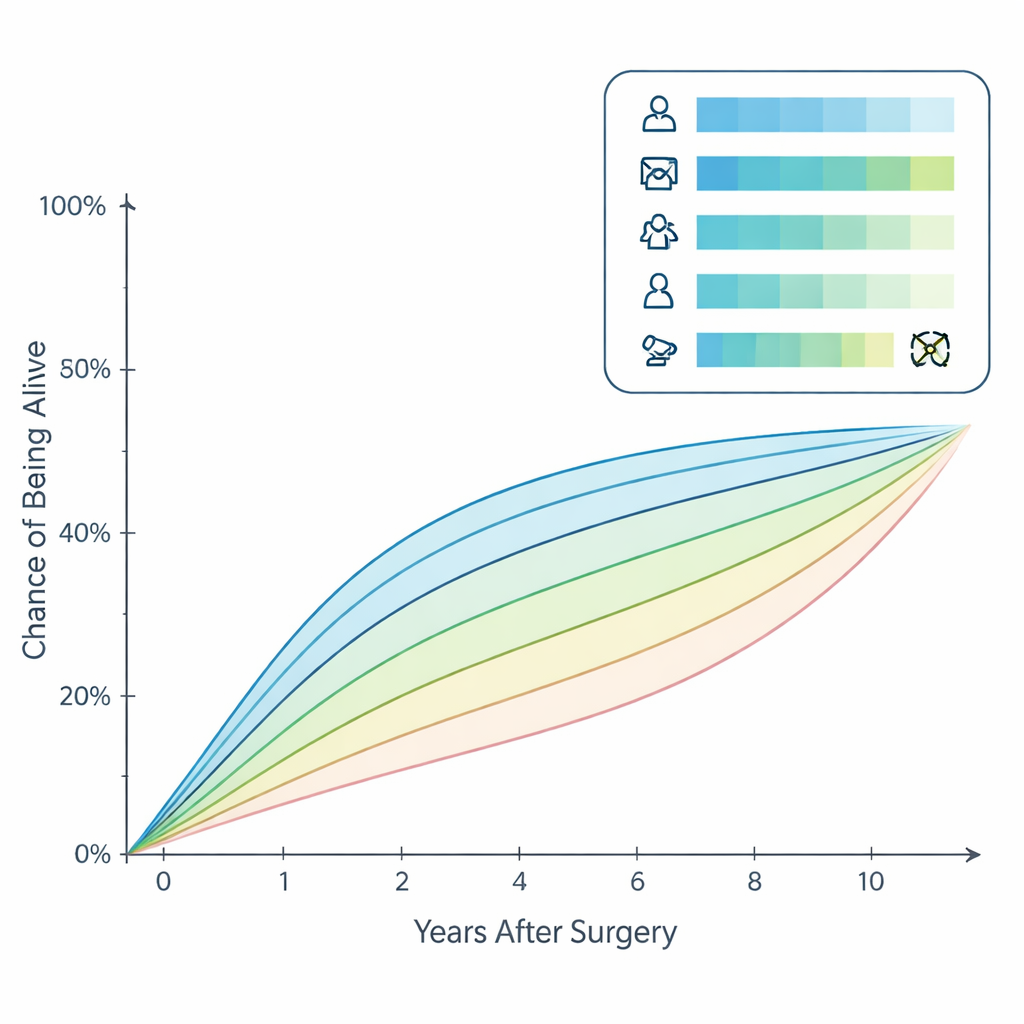
Turning numbers into practical care
Using the nomogram, the team created two broad groups: lower‑risk patients with more favorable scores and higher‑risk patients with less favorable ones. Survival curves for these groups separated clearly, suggesting that the model can meaningfully sort patients by outlook. This has direct implications for day‑to‑day care. People in the lower‑risk group, whose conditional survival improves markedly over time, may be able to space out clinic visits and scans after an initial period of close monitoring, reducing stress and inconvenience. Those in the higher‑risk group, by contrast, may benefit from more frequent check‑ups, earlier imaging, or closer attention from a multidisciplinary team.
What this means for someone living with this cancer
For patients with distant metastatic differentiated thyroid cancer, the diagnosis can sound frightening, especially when early survival statistics are quoted. This study shows that for those who undergo total thyroid removal and standard therapies, the outlook is not fixed on day one. If a person lives several years after surgery, their chances of long‑term survival can improve substantially, in some cases becoming quite favorable. The new prediction chart developed here helps doctors translate this dynamic risk into simple numbers tailored to each patient, supporting more informed conversations, better‑targeted follow‑up plans, and a more grounded sense of hope over time.
Citation: Guo, H., Qi, Y., Zhang, J. et al. Conditional survival and prognostic nomogram for distant metastatic differentiated thyroid cancer after total thyroidectomy. Sci Rep 16, 5897 (2026). https://doi.org/10.1038/s41598-026-37103-y
Keywords: thyroid cancer, metastatic cancer, survival prediction, radioactive iodine therapy, cancer prognosis