Clear Sky Science · en
Multimodal spatiotemporal graph convolutional attention network for dynamic risk stratification and intervention strategy generation in rare disease rehabilitation nursing
Why smarter rehab matters for rare diseases
People living with rare diseases often face long, uncertain paths to recovery. Their symptoms can change quickly, they may see many specialists, and there is usually little data to guide nurses and doctors. This study introduces a new artificial intelligence (AI) system designed to help rehabilitation teams spot which rare disease patients are heading toward trouble and to suggest safer, more personalized care plans along the way.
Challenges of caring for rare conditions
Although each rare disease affects few people, together they touch hundreds of millions worldwide. These patients often have several organs involved, unpredictable flare-ups, and complex medication lists. Standard hospital tools that estimate risks like falls, readmission, or serious decline were built for common conditions and steady patterns, not for rare disorders with scarce data. On top of this, useful information about a patient is scattered across vital signs, lab tests, scans, doctors’ notes, and rehab scores, which are recorded at different times and often have gaps. Clinicians must make high-stakes decisions from this messy picture, frequently without strong evidence to guide them.
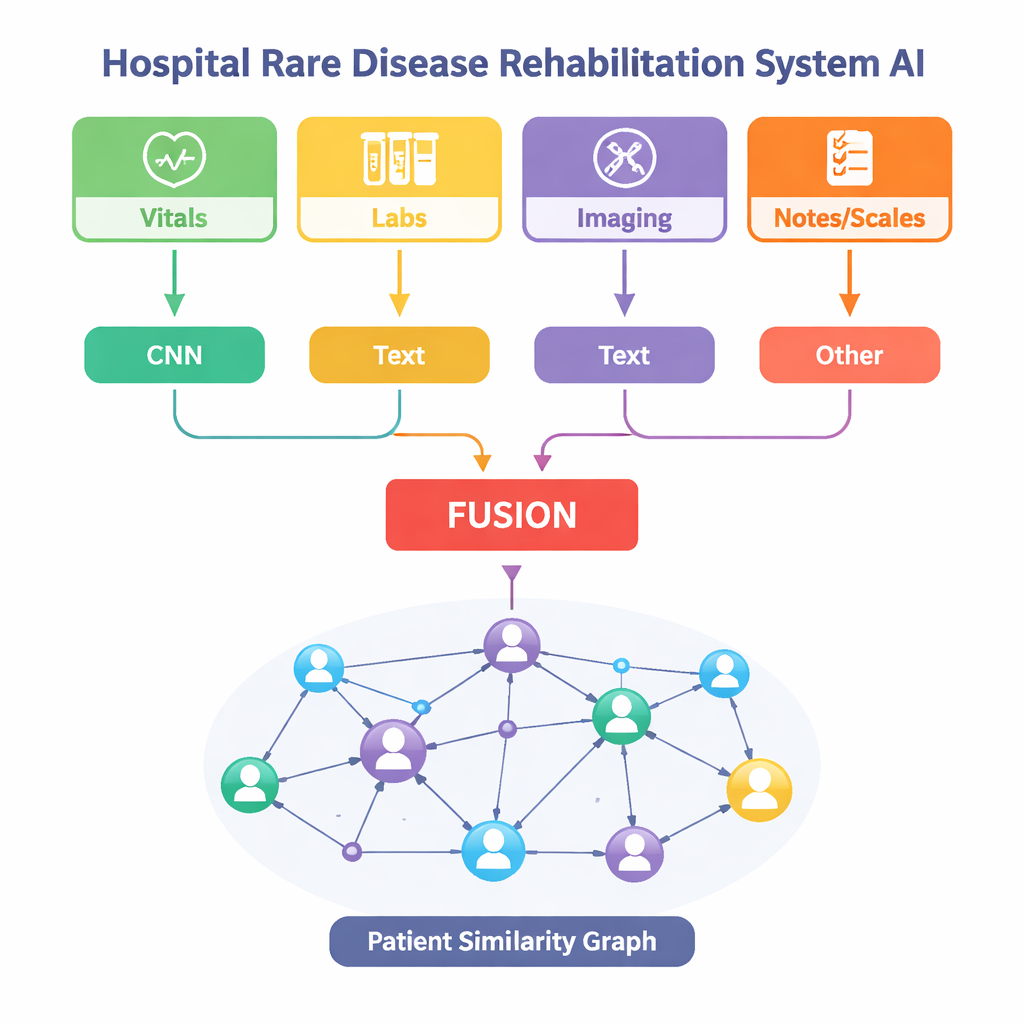
Turning scattered data into a patient network
The researchers built a system called MSTGCA-Net that pulls together many types of information for each patient: vital signs and lab results that track body function, images such as MRI or CT scans that show structure, written clinical notes and nursing observations, and standard scales measuring movement, pain, and daily activities. Each type is first translated into a compact numerical form using suitable tools, such as image-recognition networks for scans and language models for text. The system then learns how much to trust each data type for a particular patient and moment, rather than treating all sources as equally important. Next, it creates a network in which each patient is a node linked to others who share similar patterns of diagnoses, treatments, test results, and rehab progress. This patient network allows information to “flow” between people who resemble one another, helping compensate for the very small numbers seen in many rare conditions.
Following patients over time, not just at admission
Rehabilitation is a journey, not a single snapshot. The MSTGCA-Net model is designed to watch how patients change over weeks and months. On the patient network, it applies special layers that spread information along the links, so that each person’s profile is shaped by nearby, clinically similar patients. At the same time, another part of the system pays attention to when important events happened in the rehab timeline—such as a sudden lab spike, a new symptom in the notes, or a big gain or loss in function. This “attention” mechanism helps the AI focus on the most relevant moments in a person’s history, giving more weight to meaningful turning points while still considering the broader pattern. The end result is a rich, time-aware representation of each patient that can be used to sort them into different risk levels.
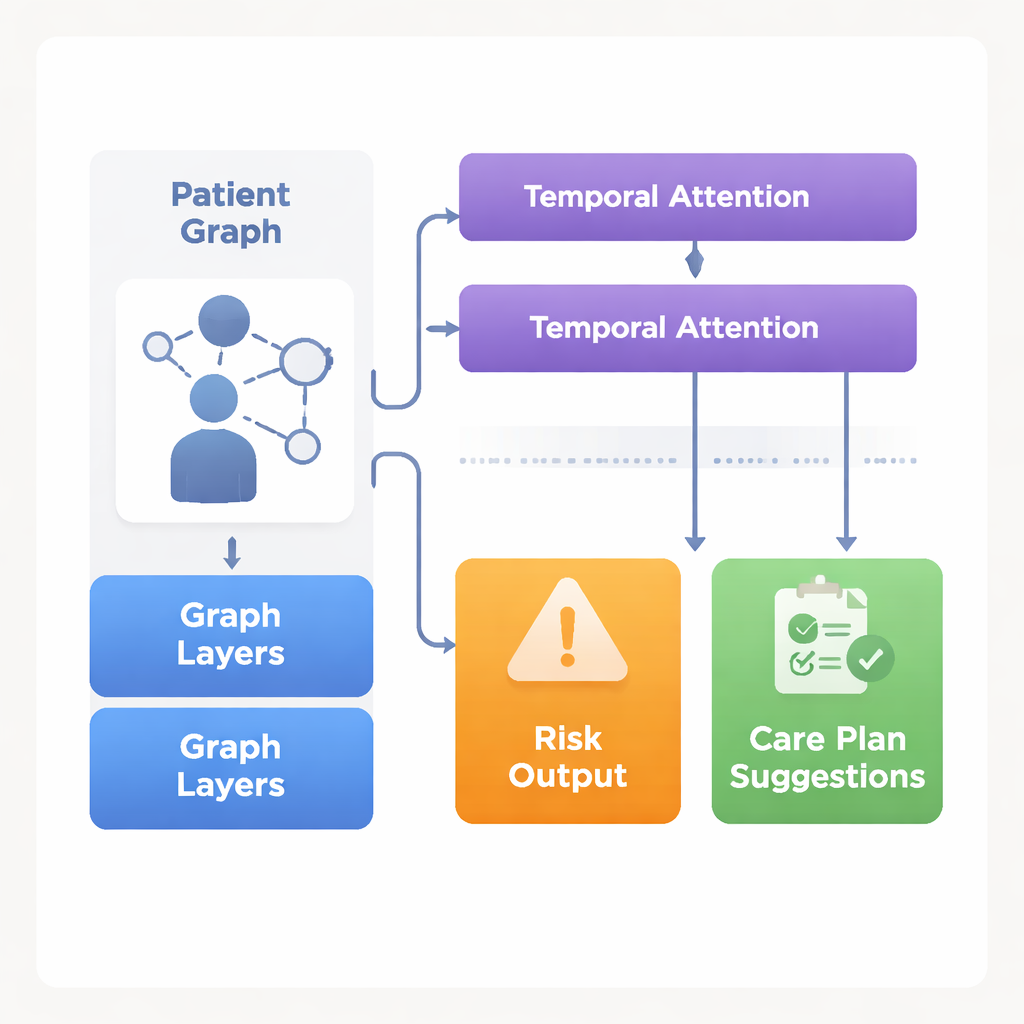
From risk scores to concrete care suggestions
Using data from 2,847 patients with 156 different rare diseases across three major centers, the model learned to predict who was at high, moderate, or low risk of bad outcomes such as serious functional decline, unplanned hospital stays, or death within 90 days. It outperformed a range of established methods, including classic statistics, standard deep learning, and other medical AI models, with an accuracy of about 0.87 and strong ability to distinguish high-risk cases. Crucially, MSTGCA-Net goes beyond numbers: it also proposes rehab actions, such as adjusting therapy intensity, changing monitoring frequency, or seeking specialist input. Built-in rules help prevent unsafe or impractical combinations. Expert rehabilitation clinicians later rated these AI-generated plans on safety, feasibility, and how well they fit the patient; scores were generally high, especially for avoiding dangerous advice.
What this means for patients and care teams
In plain terms, this work shows that AI can help turn scattered, irregular hospital data into clearer guidance for rare disease rehabilitation. By linking similar patients, tracking change over time, and highlighting which signals mattered most, MSTGCA-Net can better flag who needs extra attention and suggest concrete steps that align with usual practice. While the system still needs testing in more hospitals and in real-time care, it points toward a future where nurses and doctors caring for rare disease patients are supported by transparent, data-driven tools that make rehab safer, more efficient, and more personalized.
Citation: Zhao, S., Hu, M. & Fang, S. Multimodal spatiotemporal graph convolutional attention network for dynamic risk stratification and intervention strategy generation in rare disease rehabilitation nursing. Sci Rep 16, 6758 (2026). https://doi.org/10.1038/s41598-026-37095-9
Keywords: rare disease rehabilitation, clinical decision support, patient risk prediction, multimodal medical data, nursing care planning