Clear Sky Science · en
Deep learning-based system to predict hepatocellular carcinoma resection volume using contrast-enhanced CT
Smarter Planning for Liver Cancer Surgery
For people with liver cancer, one of the biggest challenges surgeons face is deciding how much of the liver to remove. Take too little, and the tumor can return; take too much, and the patient may not have enough healthy liver left to survive. This study introduces a new artificial intelligence (AI) system that uses CT scans to help doctors quickly and accurately plan liver operations, with the aim of making surgery safer, faster, and more consistent.
Why Liver Size Matters So Much
The most common primary liver cancer, called hepatocellular carcinoma, is both aggressive and increasingly common worldwide. Surgery that completely removes the tumor offers some patients the best chance for long-term survival. But the liver is not just another organ that can be cut away freely. It performs many vital jobs, from filtering toxins to processing nutrients. If surgeons remove too much of it, patients may suffer life-threatening liver failure after the operation. On the other hand, leaving too small a margin around the tumor increases the chance that cancer cells remain. Accurately calculating what portion of the liver can be safely removed is therefore central to modern liver surgery.
The Slow, Hands-On Status Quo
Today, this careful calculation is usually done manually. Radiologists and surgeons load contrast-enhanced CT scans into specialized three-dimensional (3D) planning software, outline the liver and tumors slice by slice, identify key blood vessels, and then simulate different cutting plans. This process can take many minutes per patient and requires highly trained staff. It is also subject to human differences: two experts may draw slightly different borders, and the same person may not be perfectly consistent from day to day. In busy hospitals where many patients need liver surgery, this time-consuming planning can slow down care and add cost.
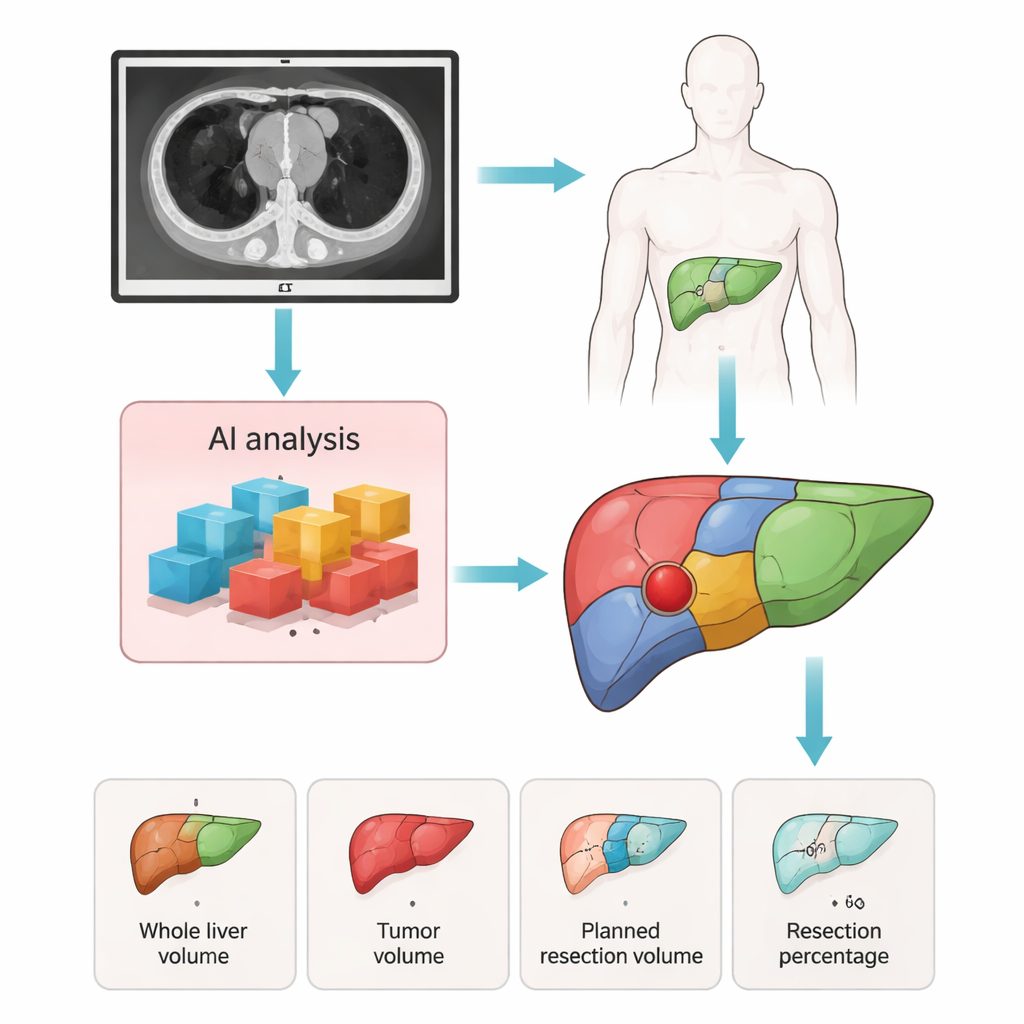
An AI Assistant Called LRVCD
The researchers developed an AI-based system they call Liver Resection Volume Calculation with Deep Learning, or LRVCD. It uses deep learning models trained on CT scans from 990 patients treated at two large hospitals over a decade. In the first stage, the AI automatically detects liver tumors and divides the liver into detailed anatomical segments on the CT images. In the second stage, the system combines these segment maps with the surgeon’s chosen plan—whether a standard segment removal or a more irregular, custom cut—to calculate how much healthy liver tissue and how much tumor would be removed. The system reports key numbers such as total liver size, tumor size, the planned resection volume, and the percentage of liver to be removed.
Putting the System to the Test
To check whether LRVCD is reliable, the team compared its results with those from experienced surgeons using established 3D planning software. They evaluated two independent groups of patients: one from the same hospital where the AI was trained and another from different centers. For each case, they measured how closely the AI’s estimates of liver volume, tumor volume, and planned resection matched the manual reference. The differences were small, and the agreement in the key measure—the percentage of liver to be removed—was close across both groups. While the AI tended to slightly underestimate the overall liver size and slightly overestimate tumor volume, these tendencies remained within acceptable clinical limits and mirrored known quirks of human-driven 3D planning.
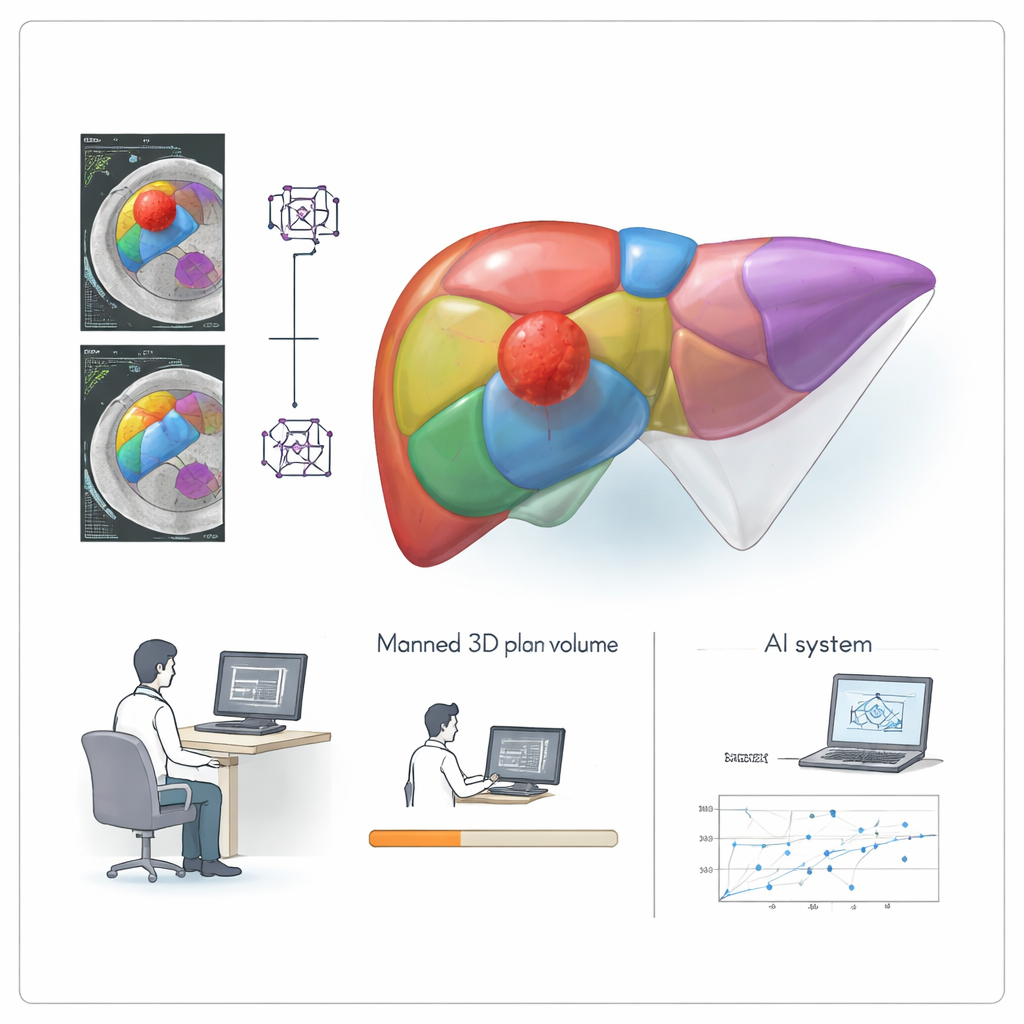
From Hours of Work to Seconds
One of the most striking advantages of LRVCD is speed. In both internal and external test groups, the AI-driven workflow reduced planning time roughly twenty-fold compared with the conventional 3D software process. What once took on the order of ten minutes or more could now be completed in under half a minute. Because the AI handles the heavy lifting of segmentation and volume calculation, human input is largely limited to entering basic surgical information and making small adjustments when needed. This means radiologists and surgeons can focus more on clinical decisions and less on repetitive mouse work.
What This Means for Patients
For patients, the technical details boil down to a simple promise: more precise and faster surgical planning, without extra scans or added cost. By providing quick, consistent estimates of how much liver can safely be removed, LRVCD may help surgeons push toward curative operations while keeping the risk of post-surgery liver failure in check. The study shows that this AI tool performs about as well as established 3D planning methods while greatly reducing workload. The authors note that more work is needed to test the system in broader patient groups and to further automate surgical decision-making, but their results suggest that AI-guided planning could soon become a practical ally in the operating room for liver cancer care.
Citation: Wang, X., Zhang, L., Liu, P. et al. Deep learning-based system to predict hepatocellular carcinoma resection volume using contrast-enhanced CT. Sci Rep 16, 6388 (2026). https://doi.org/10.1038/s41598-026-37085-x
Keywords: liver cancer surgery, medical imaging AI, hepatocellular carcinoma, CT scan planning, liver resection volume