Clear Sky Science · en
Machine learning models powered by emergency medical services data enhance stroke triage in prehospital settings
Why faster stroke decisions matter
Every minute counts when someone is having a stroke. Brain cells die quickly, and the chance of walking, talking, and living independently again shrinks with each delay. Yet many strokes are first seen not by doctors, but by paramedics in an ambulance. This study explores whether computers that learn from past cases can help emergency medical services (EMS) spot strokes earlier and direct patients to the right hospital faster—potentially saving brain tissue and long-term quality of life.
What happens before the hospital
The journey for a stroke patient usually begins with a 9-1-1 call. Dispatchers decide what kind of help to send, and EMS crews then examine patients at home or in the field. They record basic information such as age and weight, plus vital signs like heart rate, blood pressure, breathing rate, oxygen level, and level of alertness. These numbers are often taken before the hospital ever sees the patient. The researchers asked a simple question: are these early measurements reliable enough, and complete enough, for a computer to use them to flag possible strokes in real time?
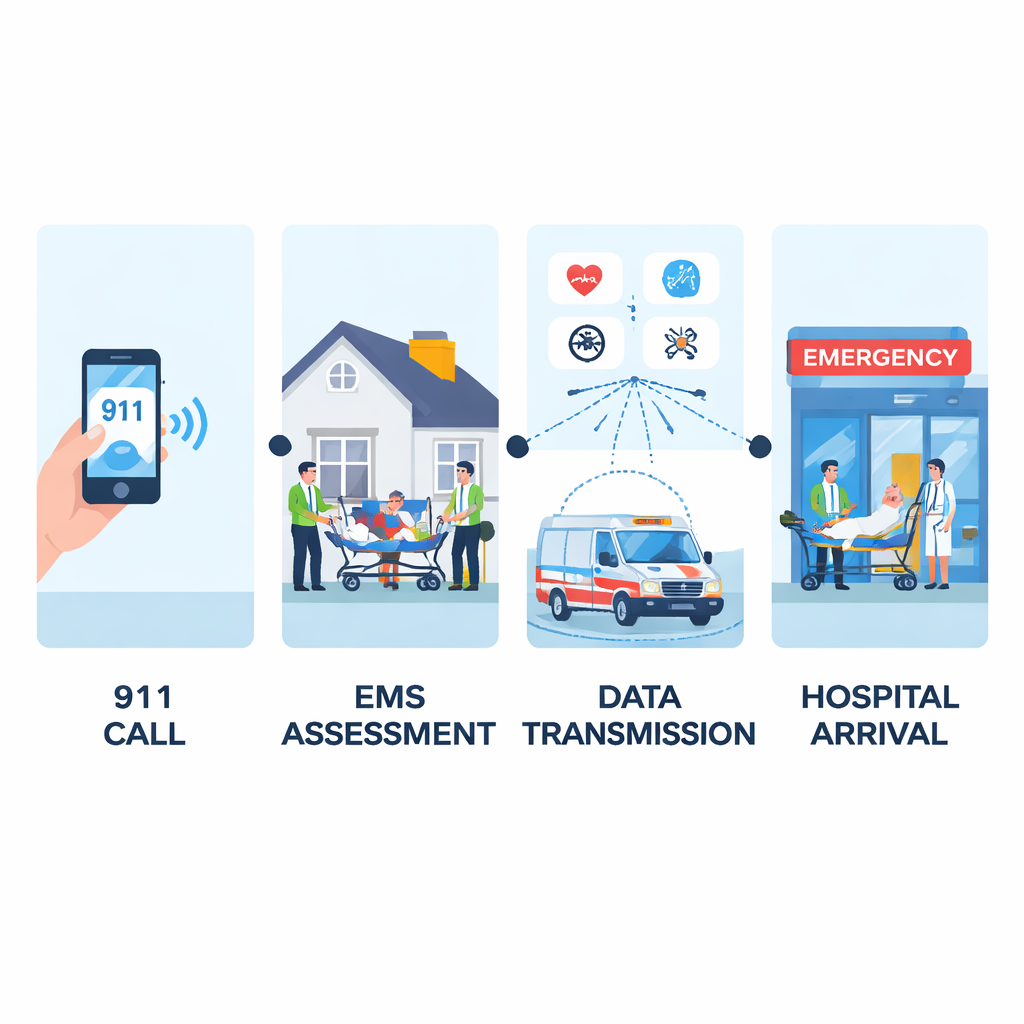
How the study was carried out
The team looked back at 8,221 ambulance trips involving 4,333 adults taken to a large hospital near Chicago between 2015 and 2020. Only about 2 percent of these encounters were confirmed strokes, and almost two-thirds of those were severe—patients who ended up in intensive care or on a ventilator. The researchers compared what EMS recorded on scene with what hospital staff measured shortly after arrival. Heart rate, blood pressure, blood sugar, oxygen levels, and a simple consciousness score were available for most patients and generally matched hospital readings, showing that ambulance data reflected patients’ true conditions quite well.
Teaching computers to recognize danger
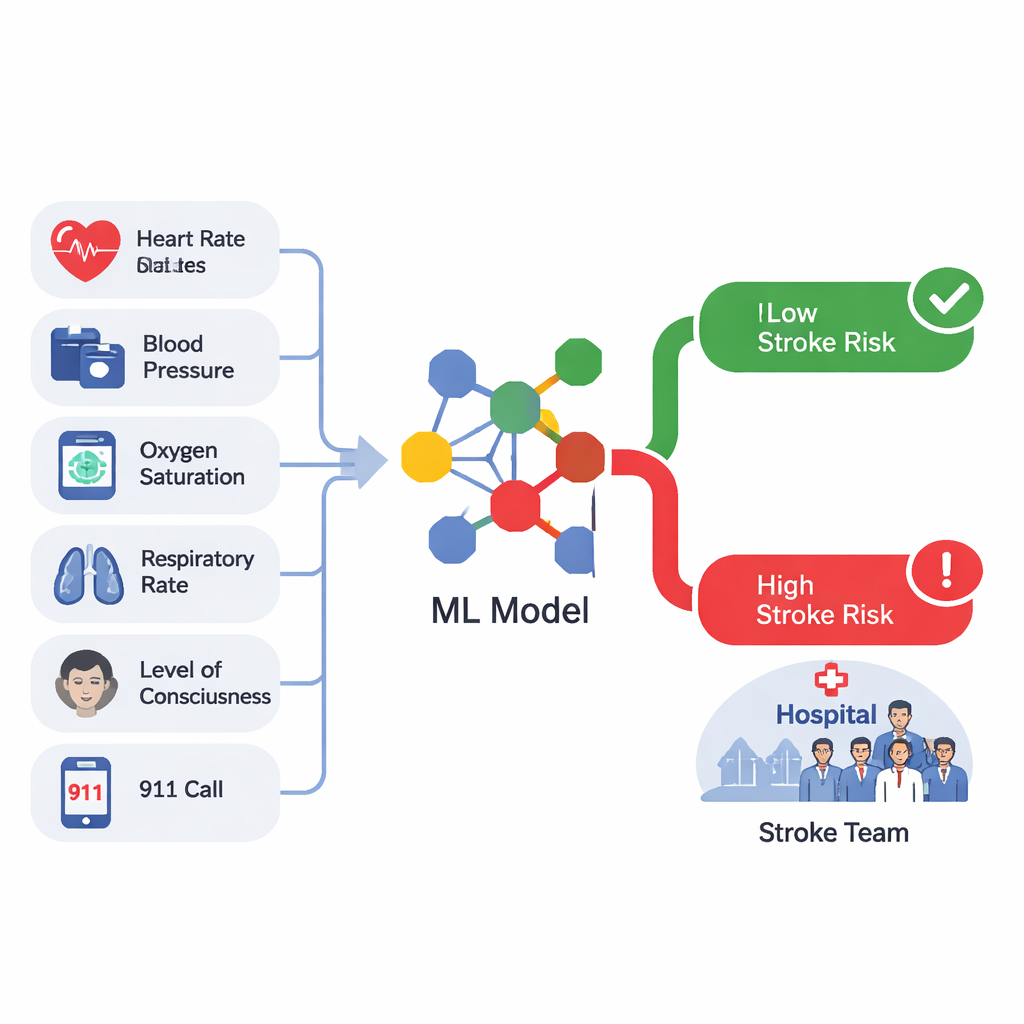
Using these prehospital numbers plus basic details about the 9-1-1 call and where patients were picked up, the researchers trained several types of machine learning models to solve two tasks: tell strokes from non-strokes, and tell severe strokes from all other cases. They tested three common approaches—random forests, XGBoost, and a simple neural network—on separate sets of data so the models would be judged fairly. Because strokes were rare, the models were adjusted to pay extra attention to the small number of stroke cases and were carefully checked so that their risk scores matched real-world probabilities as closely as possible.
How well the tools performed
Across the full group of ambulance trips, the best model for detecting any stroke was an XGBoost model, and the best for flagging severe strokes was a random forest model. These tools were good at ranking who was more or less likely to have a stroke, and, when tuned to a reasonable cutoff, they caught more strokes than current EMS screening methods while still avoiding most false alarms. For instance, at one operating point the stroke model correctly identified about two-thirds of stroke cases and correctly ruled out nearly nine out of ten non-stroke cases. The most influential signals were familiar clinical clues: higher blood pressure, changes in consciousness, abnormal pulse, older age, and 9-1-1 call codes that hinted at stroke-like problems such as sudden weakness or trouble speaking.
What this could mean for patients
Because strokes are uncommon among all ambulance patients, even a well-performing model will raise some false alarms. In practice, that would mean a number of patients flagged as “possible stroke” who turn out not to have one. The authors argue that, for a time-critical emergency, that trade-off may be worthwhile if the alert simply prompts faster evaluation rather than replacing human judgment. Their results suggest that machine learning tools could act as an extra set of eyes on the data EMS already collect, pointing paramedics and hospitals toward higher-risk patients who might otherwise be overlooked.
Where this work is headed
In plain terms, the study shows that the numbers recorded in the back of the ambulance can power smart computer tools that help decide who might be having a stroke and how urgently they need advanced care. These systems are not meant to diagnose on their own, but to support paramedics and emergency doctors as they make rapid decisions about where to send patients and how quickly to mobilize stroke teams. With better data sharing, more complete documentation, and testing in different regions, such tools could help more people get to the right hospital, sooner, and walk away from a stroke with less lasting damage.
Citation: Saban, M., Hiura, G., de la Peña, P. et al. Machine learning models powered by emergency medical services data enhance stroke triage in prehospital settings. Sci Rep 16, 7139 (2026). https://doi.org/10.1038/s41598-026-37069-x
Keywords: stroke triage, emergency medical services, machine learning, prehospital care, artificial intelligence in medicine