Clear Sky Science · en
Clinical outcomes and management strategies for moderate aortic regurgitation in patients undergoing rheumatic mitral valve surgery
Why this heart study matters
Heart valve problems are a major cause of disability and early death in many low‑ and middle‑income countries, especially when they stem from childhood rheumatic fever. Surgeons often face a tough choice when operating to fix a damaged mitral valve: if the neighboring aortic valve is moderately leaky but not yet severe, should they leave it alone, try to repair it, or replace it outright? This study follows hundreds of patients over several years to see which strategy best protects heart function without adding extra risk.
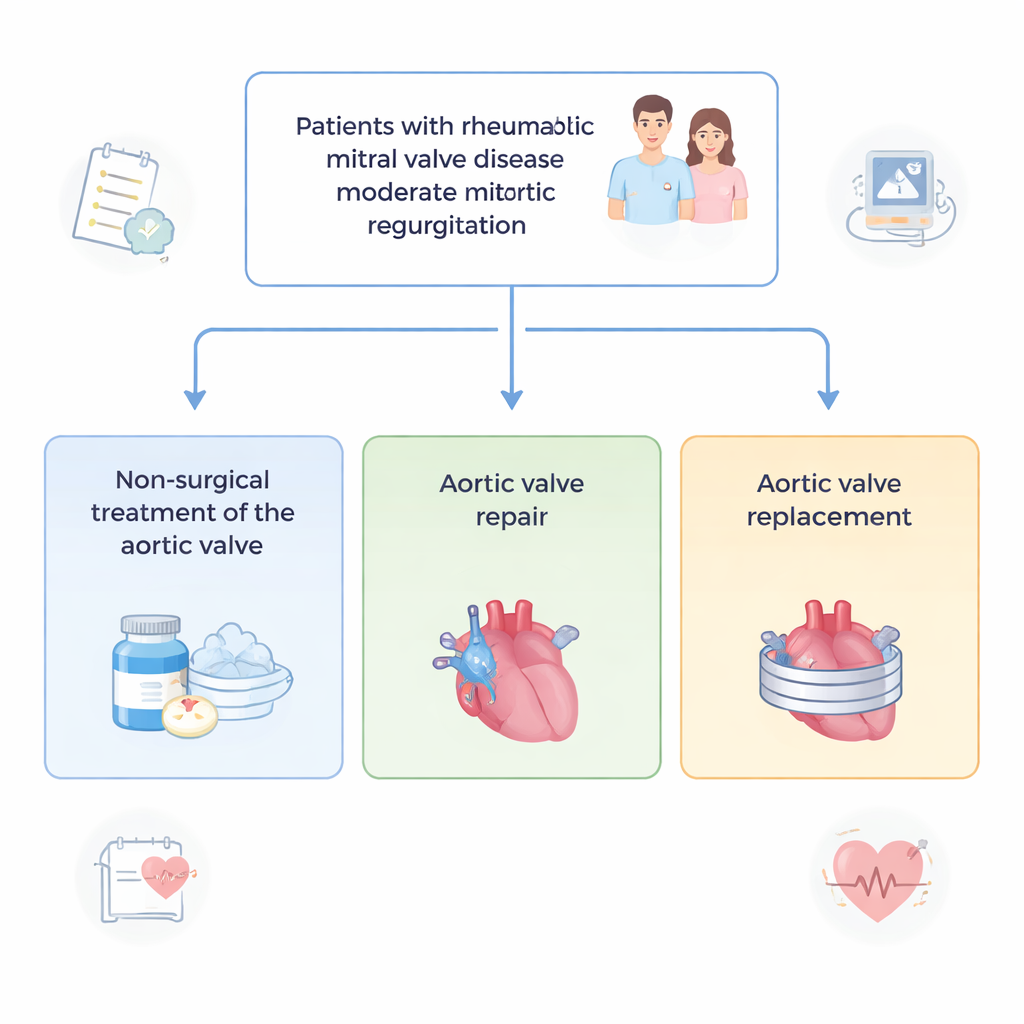
The surgical crossroads
The researchers focused on adults with rheumatic heart disease whose main problem was a diseased mitral valve, but who also had moderate leakage of the aortic valve, known as aortic regurgitation. All 338 patients needed mitral valve surgery. During the same operation, their surgeons chose one of three paths for the aortic valve: do nothing beyond careful protection of the heart (non‑surgical treatment), repair the existing valve, or replace it with an artificial valve. Because the study was retrospective, it did not assign treatments at random; instead, it analyzed what happened to real‑world patients treated in two large Chinese hospitals between 2015 and 2024.
Following patients over time
Patients were tracked for a median of just over three and a half years, with many followed substantially longer. The main question was how often the aortic valve later became clearly faulty again—worse than mild leakage or narrowing—on ultrasound scans. The team also recorded deaths, repeat valve operations, and complications such as stroke, major bleeding, or serious rhythm problems. About four in ten patients had their aortic valve replaced, slightly fewer had a repair, and the rest had no direct aortic valve procedure at all.
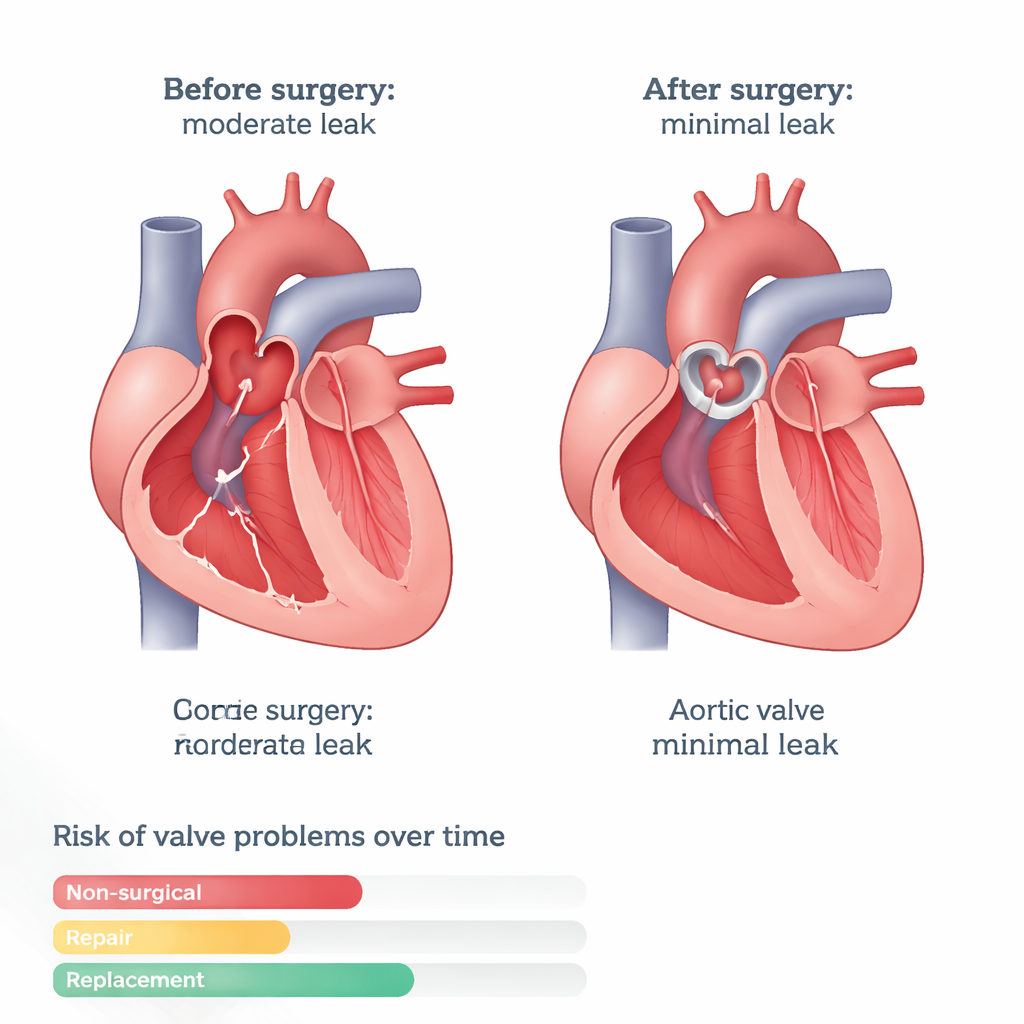
What happened to the leaky valve
The most striking finding was how rarely serious problems came back after aortic valve replacement. Only about 4% of patients in the replacement group developed more‑than‑mild aortic valve dysfunction during follow‑up, compared with about one‑third of patients whose valve was left alone or only repaired. Even after taking into account patient age, degree of valve calcification, and other heart measurements, replacement cut the relative risk of meaningful valve problems by more than half compared with no treatment, and by even more compared with repair. Yet many people in the non‑surgical group also did well: most had no or only mild leakage years later, suggesting that the aortic leak can stabilize or improve after the mitral valve is fixed.
Risks, repairs, and real‑world trade‑offs
Importantly for patients and surgeons, the safer valve function seen with replacement did not come at the cost of higher early or mid‑term risk. There were no in‑hospital deaths in any group, and over follow‑up the rates of death, repeat valve surgery, and valve‑related complications were similar whether the aortic valve was left alone, repaired, or replaced. Repair showed some short‑term benefit in reducing leakage right after surgery, but in this rheumatic population it did not clearly outperform simply leaving the valve alone in the long run. Replacement avoided recurrent leakage most effectively, but it also brings lifelong issues such as blood‑thinning medication for mechanical valves or eventual wear‑out of biological valves, so careful selection remains essential.
What this means for patients
For people with rheumatic mitral valve disease and a moderately leaky aortic valve, this study suggests there is no single “one‑size‑fits‑all” answer. Replacing the aortic valve during mitral surgery offers the most reliable protection against future aortic valve problems, without noticeably raising surgical risk in the medium term. At the same time, many patients whose aortic valve is not severely affected can safely delay aortic valve surgery and be monitored with regular heart scans, especially in an era when less invasive valve procedures are expanding. For patients and families, the key message is that both immediate replacement and watchful waiting can be reasonable; the best choice depends on valve appearance, overall heart health, and individual preferences discussed with an experienced heart team.
Citation: Liu, C., Liu, Z., Liang, Jj. et al. Clinical outcomes and management strategies for moderate aortic regurgitation in patients undergoing rheumatic mitral valve surgery. Sci Rep 16, 7059 (2026). https://doi.org/10.1038/s41598-026-37045-5
Keywords: rheumatic heart disease, aortic regurgitation, mitral valve surgery, aortic valve replacement, valve repair