Clear Sky Science · en
Impaired brain intrinsic connectivity in long COVID during cognitive exertion revealed by independent component analysis
Why thinking feels harder after COVID
Many people with long COVID describe “brain fog” – trouble focusing, slowed thinking, and mental fatigue that lingers months after infection. This study asked a simple question with very high‑tech tools: what is happening inside the brain when people with long COVID try to concentrate? Using an ultra‑powerful MRI scanner and a classic attention test, the researchers watched how different brain regions talk to each other during mental effort, and compared people with long COVID to healthy volunteers.
A mental tug‑of‑war test
To probe thinking under pressure, participants performed the Stroop color‑word task inside a 7‑Tesla MRI scanner. In this task, you might see the word for one color printed in a different colored ink, and must quickly decide whether the color and word match. It’s surprisingly demanding, because your brain has to suppress the automatic urge to read the word and instead pay attention to the ink color. The team ran the task twice in a row, each scan lasting seven and a half minutes, to see not only baseline performance but also what happened as people grew mentally tired. Nineteen adults with long COVID and sixteen healthy controls took part.
Slower thinking and overworked networks
People with long COVID consistently took longer to respond on the Stroop task than healthy participants, especially during the first scan, confirming that their thinking was slowed even when they tried their best. Yet by the second scan, their response times improved, hinting that they could adapt with practice despite feeling impaired. Meanwhile, the MRI data showed that the task activated a web of well‑known brain networks involved in attention, decision‑making, movement and vision. Using a mathematical method called independent component analysis, the researchers separated the brain activity into 15 distinct networks and then examined how strongly each network connected to other parts of the brain – the brain’s internal “wiring diagram” during mental exertion.
Key control hubs go offline
The most striking differences between long COVID and healthy brains appeared in networks that normally help us detect important events and control our responses. A “salience” network, centered on deep regions such as the insula and anterior cingulate cortex, usually decides which signals are important and routes resources to either outward‑focused control networks or inward‑focused, resting‑state networks. In long COVID, this salience network showed weaker connections to many other areas, particularly during the second scan after sustained effort. Networks supporting language, high‑level planning, and sensorimotor function also showed reduced connectivity, especially to frontal control regions and structures that help initiate movements. These deficits suggest that the brain’s traffic‑control system is faltering just when the task demands are high.
Work‑arounds and changes over time
The picture was not only one of loss. Some regions, especially the angular gyrus at the junction of visual and language areas, showed stronger connections in long COVID than in healthy participants. This region helps integrate sights, words, and actions, so its extra engagement may reflect the brain’s attempt to compensate for weakened pathways elsewhere. The researchers also looked at how connectivity varied with the length of time people had been ill. As illness duration increased, connections from key control networks in the frontal lobes tended to weaken, while links involving visual areas and the angular gyrus tended to strengthen, as if the brain were gradually rewiring to cope with ongoing damage.
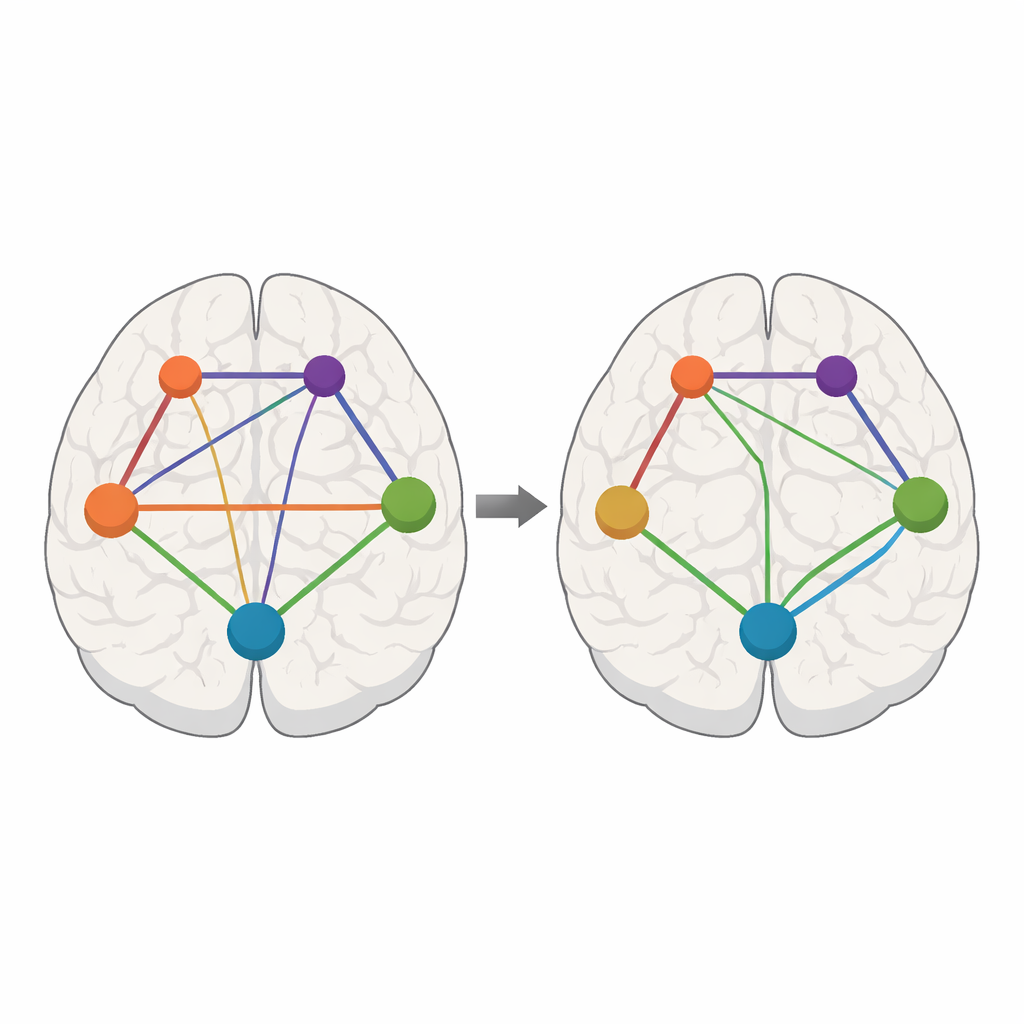
What this means for brain fog
Overall, the study paints long COVID brain fog as a problem of disrupted communication rather than a single damaged spot. When people with long COVID face a challenging thinking task, the networks that should coordinate attention and control appear under‑connected, especially as mental fatigue sets in. Other regions step in and strengthen their ties, hinting at partial compensation but not a full fix. These widespread changes support the idea that the virus, or its after‑effects, have altered brain function across many regions, possibly through direct effects on brain cells. Understanding this pattern of weakened and strengthened connections may help guide future treatments aimed at restoring healthier network balance and easing the mental burden of long COVID.
Citation: Barnden, L., Baraniuk, J., Inderyas, M. et al. Impaired brain intrinsic connectivity in long COVID during cognitive exertion revealed by independent component analysis. Sci Rep 16, 7872 (2026). https://doi.org/10.1038/s41598-026-36986-1
Keywords: long COVID brain, cognitive fatigue, functional MRI, brain networks, brain fog