Clear Sky Science · en
Evaluating the prognostic significance of HIST1H4C in breast cancer: implications for neoadjuvant therapy
Why this research matters
For many women with breast cancer, chemotherapy given before surgery—called neoadjuvant therapy—can shrink tumors and make operations safer and more successful. But not everyone benefits equally, and the treatment can carry serious side effects. This study explores whether a single gene, called HIST1H4C, measured in tumor samples, can help doctors predict who is most likely to respond well to this pre-surgery treatment and who may face a higher risk of the cancer coming back.
A gene hiding in the tumor’s packaging
HIST1H4C belongs to a family of genes that help package DNA inside cells, a bit like spools that thread is wrapped around. These “packaging” proteins, known as histones, do more than just organize DNA; they influence which genes are turned on or off, and therefore can shape how aggressive a cancer becomes and how it reacts to drugs. Earlier work using single-cell sequencing hinted that HIST1H4C is especially active in high-grade breast tumors—those that look more abnormal under the microscope and tend to behave more aggressively. This raised a key question: could HIST1H4C be a marker that links tumor aggressiveness, chemotherapy response, and long-term patient outcomes?
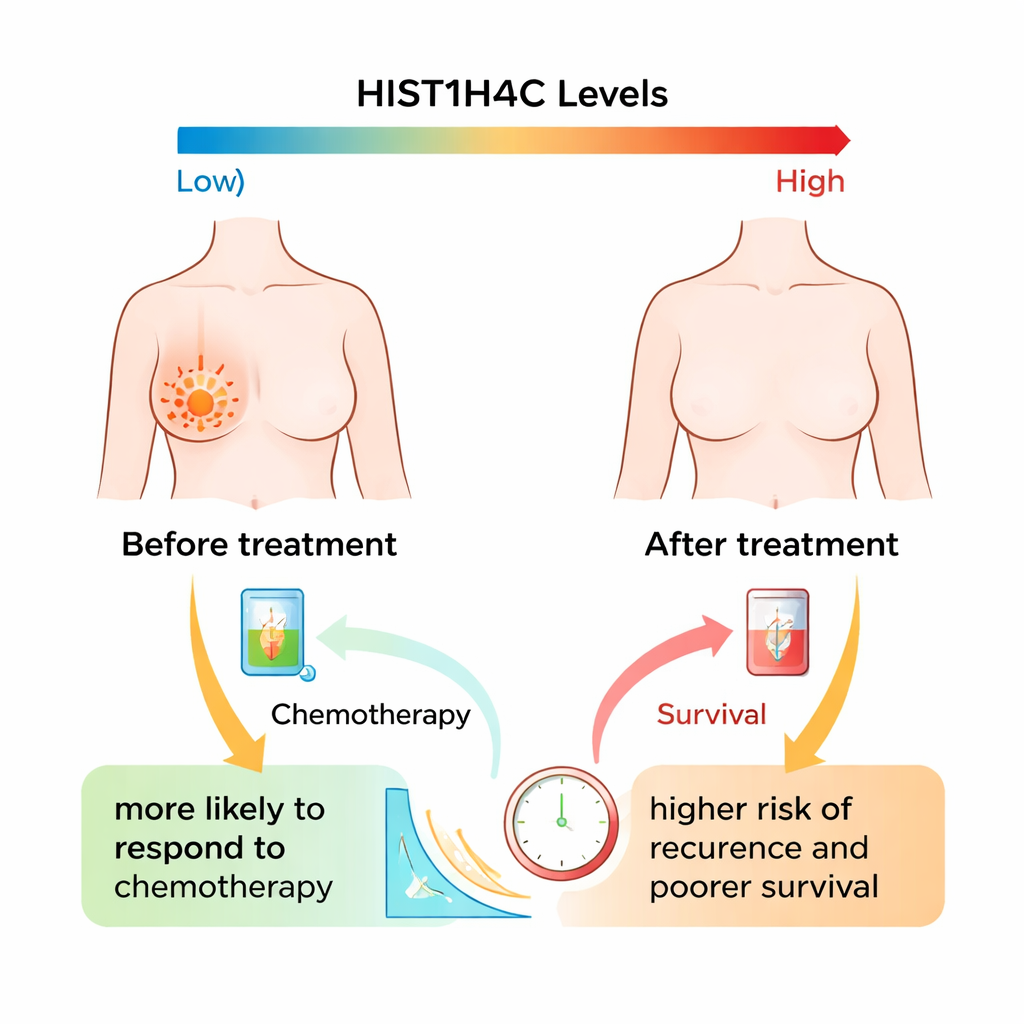
Testing tumors before and after treatment
The researchers followed more than one hundred women with stage II or higher breast cancer treated at a medical center in Guangzhou, China, between 2019 and 2022. All patients received standard neoadjuvant chemotherapy, including anthracycline- and taxane-based drugs, and some also received targeted therapy for HER2-positive disease. Tumor samples were collected before treatment and again after surgery. The team measured how much HIST1H4C mRNA—an indicator of how strongly the gene is expressed—was present in each sample, and then compared these levels to how well the tumors responded, whether they shrank completely or partially, and how long patients remained free of disease.
A surprising two-sided signal
The results revealed an intriguing pattern. Before treatment, tumors in patients who responded well—those with complete or partial shrinkage—actually had higher HIST1H4C levels than tumors in poor responders. In other words, higher starting levels of this gene were linked to greater chemotherapy sensitivity, even though these tumors often had other high-risk features like hormone receptor negativity, more lymph node involvement, and triple-negative status. After treatment, however, the story reversed: patients whose tumors still showed high HIST1H4C levels tended to have larger remaining cancers and worse progression-free survival. Across the whole group, HIST1H4C levels usually dropped after therapy, but this decrease was much more pronounced in good responders than in poor responders.
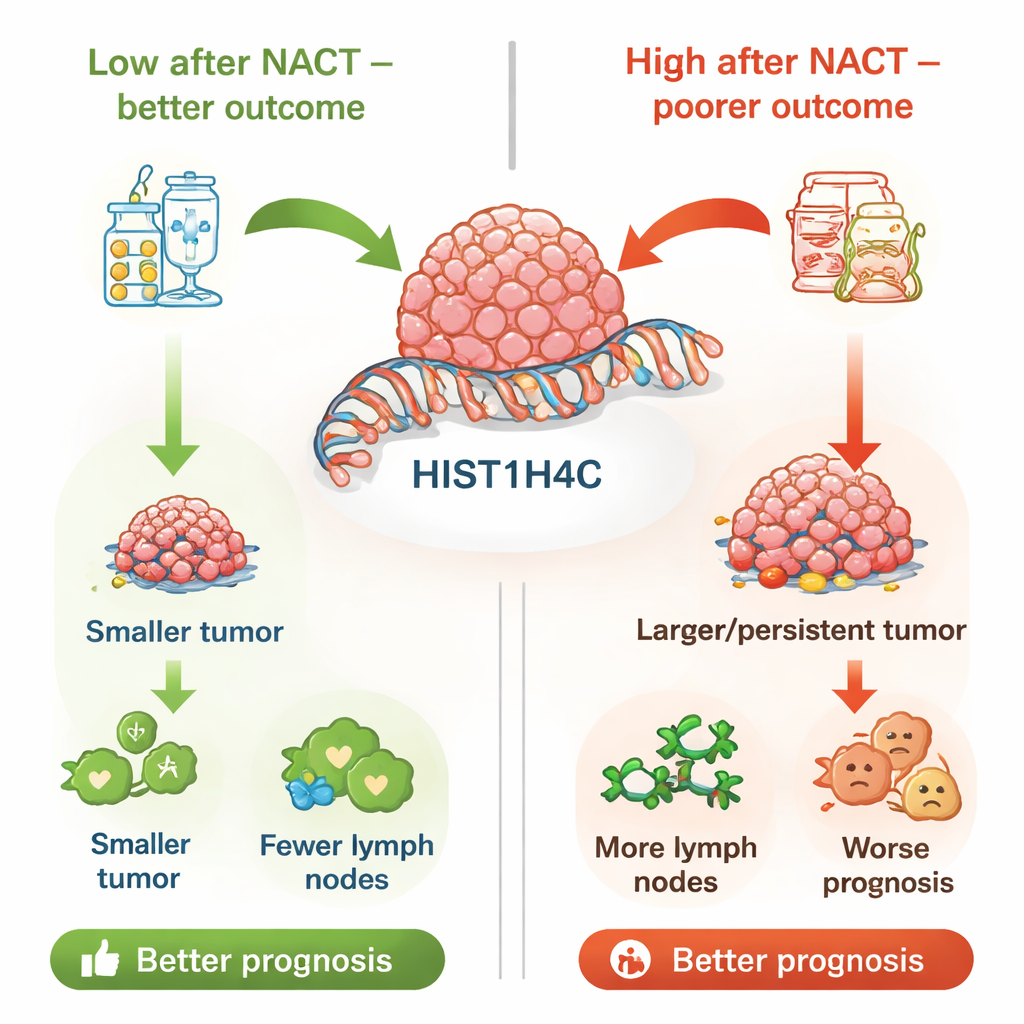
Connecting gene levels to long-term outlook
To test whether these findings held up in a broader context, the authors analyzed data from a large public breast cancer dataset known as the Curtis database. There, too, high HIST1H4C expression was linked to more advanced tumor grade, larger tumors, more lymph node metastases, and unfavorable tumor types such as triple-negative and hormone receptor–negative breast cancers. Most importantly, patients with higher HIST1H4C levels in this external dataset had shorter survival times. Taken together, both the hospital cohort and the big-data analysis pointed toward HIST1H4C as a marker of more aggressive disease and poorer prognosis, especially when its levels remain high after treatment.
Toward more tailored treatment decisions
For a layperson, the key message is that a simple laboratory test measuring HIST1H4C in tumor tissue could one day help doctors better match neoadjuvant therapy to the individual patient. High HIST1H4C before treatment may flag cancers that are aggressive but also more likely to shrink with chemotherapy, while persistently high HIST1H4C after treatment may signal a higher risk of relapse and the need for closer follow-up or additional therapies. Because the test relies on standard gene-expression methods already common in many hospitals, the authors argue it could be a practical, cost-effective tool, especially in resource-limited settings. Although further validation is needed, this work suggests that reading the “packaging” of the tumor’s DNA can offer powerful clues about which breast cancers will respond to pre-surgery treatment and how patients are likely to fare in the long run.
Citation: Qian, L., Ge, R., Haihu, Z. et al. Evaluating the prognostic significance of HIST1H4C in breast cancer: implications for neoadjuvant therapy. Sci Rep 16, 6792 (2026). https://doi.org/10.1038/s41598-026-36983-4
Keywords: breast cancer, neoadjuvant chemotherapy, biomarkers, HIST1H4C, treatment response