Clear Sky Science · en
Structural and physicochemical stability of 3D-printed bolus materials used in radiotherapy
Why the Shape of Radiation Matters
When doctors use radiotherapy to treat cancer, they aim powerful X-ray beams at tumors hidden just below the skin. To hit the cancer while sparing healthy tissue, they often place a customized pad, called a bolus, on the patient’s skin. This pad subtly reshapes where the highest radiation dose lands. Today, many hospitals are exploring 3D printing to create perfectly fitted boluses, but a key question remains: do the plastics used in these printed pads stay stable after being bombarded with treatment-level radiation?
Custom Pads for Complex Bodies
Traditional boluses are often molded by hand from wax or gels, which can be slow to prepare and hard to reproduce exactly from one treatment session to the next. With 3D printing, clinicians can design pads that match a patient’s body based on medical scans, improving comfort and reducing tiny air gaps that can distort the dose. This is especially important in areas such as the head and neck, where the surface is irregular and critical organs lie close to the skin. The study focuses on two plastics commonly used in 3D printers: ABS, a stiff, widely available plastic, and TPC, a more flexible material that may contour better to the body.
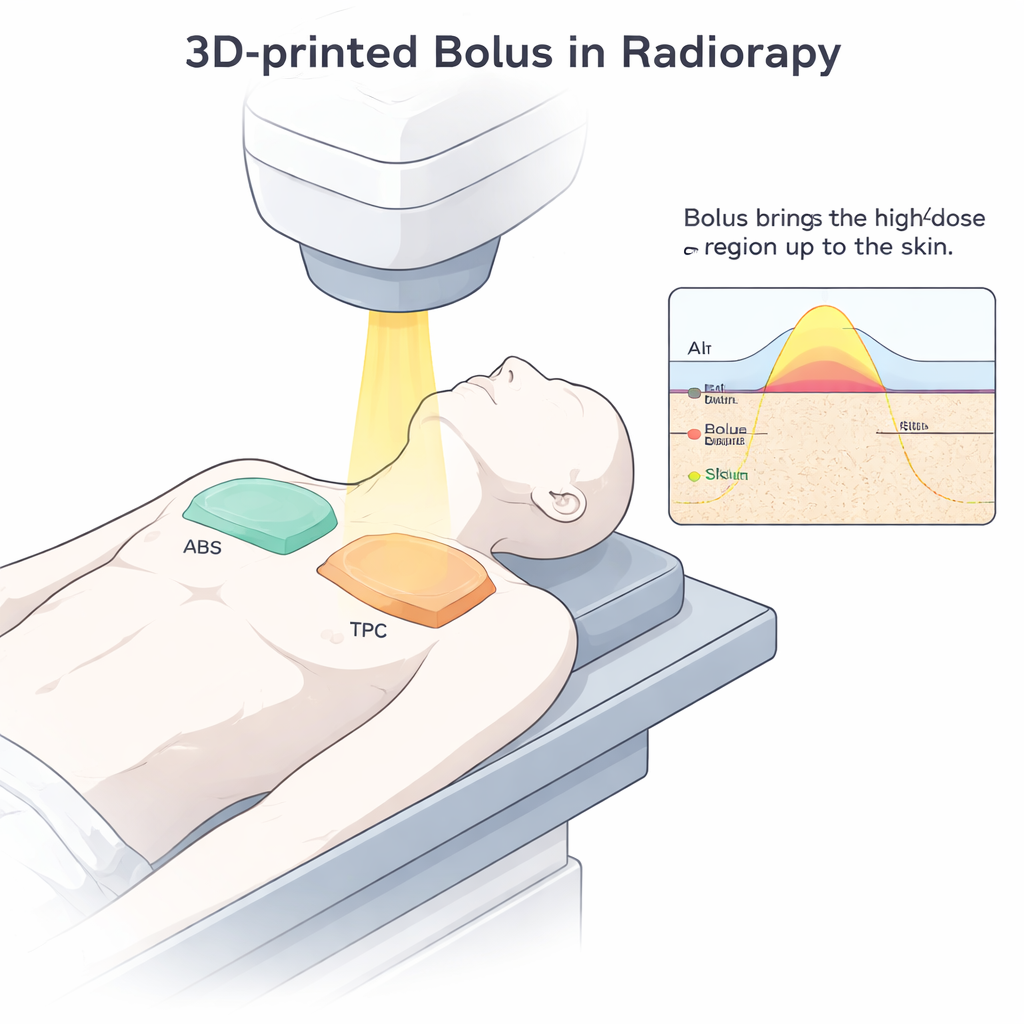
Putting 3D-Printed Plastics Under the Beam
To mimic what happens in real cancer treatment, the researchers printed small ABS and TPC blocks and exposed them to a total X-ray dose of 70 gray, similar to a full course of radiotherapy. Before and after irradiation, they measured size, hardness, surface roughness, friction, and internal changes in structure and thermal behavior. These tests show whether a bolus would keep its shape, continue to fit the skin well, and avoid cracking or wearing down during repeated use. Tiny shifts in thickness or texture, even by a few hundredths of a millimeter, can alter how radiation is delivered to shallow tumors.
How the Two Plastics Hold Up
Both materials remained almost the same size after exposure, with ABS showing only a very slight but measurable thickness change and TPC staying dimensionally stable. The surfaces of both plastics became smoother, which can improve skin contact and reduce air gaps. However, ABS showed more signs of surface degradation and a dramatic 70% drop in friction, meaning it could slide more easily on the skin. TPC, by contrast, changed very little in friction and wear behavior, suggesting its surface stays more predictable under repeated handling. Hardness increased slightly in both materials, which can help them keep their shape but may also reduce their ability to drape perfectly over complex anatomy.
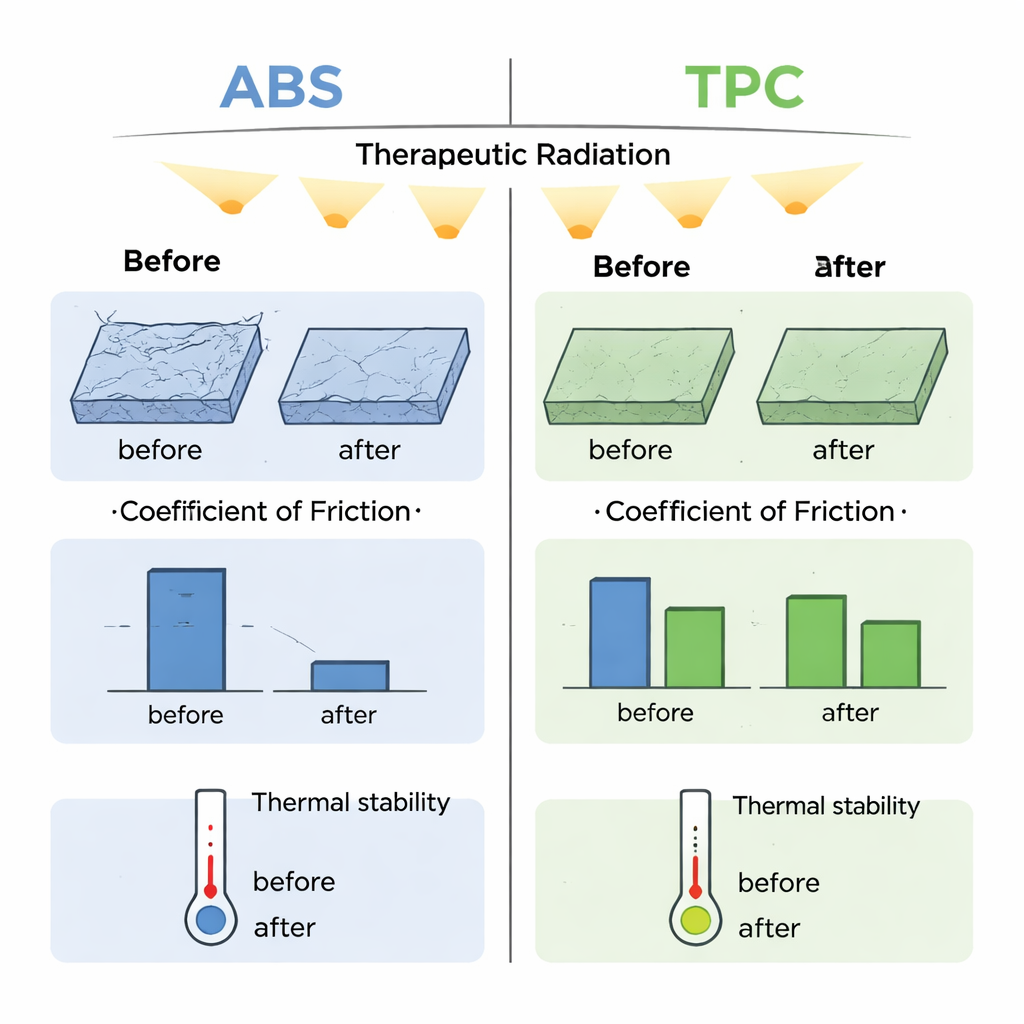
What Happens Inside the Materials
To see how radiation affects the plastics at the molecular level, the team used infrared spectroscopy to look for chemical fingerprints and a thermal technique to check how the polymers respond to heat. In ABS, they saw signs of mild damage: certain chemical groups associated with one of its rubbery components weakened, while signals linked to oxidation and subtle rearrangement of the chains appeared. The temperature at which ABS transitions from hard and glassy to more rubber-like dropped by about three degrees Celsius, hinting at slight internal breakdown. In TPC, the spectral changes were very small and its melting and softening behavior stayed essentially unchanged, indicating better resistance to radiation.
What This Means for Patients
For everyday clinical use, the findings suggest that both ABS and TPC 3D-printed boluses can survive realistic treatment doses and still do their job of shaping the radiation beam. Yet TPC appears more robust: it resists chemical and mechanical change, stays flexible, and keeps a more stable surface. This combination may translate into better stick-to-skin contact, fewer air gaps, and more reliable dose delivery over many treatment sessions. The authors conclude that while existing ABS boluses remain usable, TPC is a particularly promising candidate for future personalized bolus design. Ongoing work will test how these subtle material changes actually affect skin contact and radiation dose in realistic treatment setups.
Citation: Jezierska, K., Borůvka, M., Ryvolová, M. et al. Structural and physicochemical stability of 3D-printed bolus materials used in radiotherapy. Sci Rep 16, 6611 (2026). https://doi.org/10.1038/s41598-026-36952-x
Keywords: radiotherapy bolus, 3D printing, ABS plastic, thermoplastic copolyester, radiation effects on materials