Clear Sky Science · en
Association of human leukocyte antigen B genotypes with COVID-19 severity in Egyptian patients
Why some people get sicker than others
The COVID-19 pandemic revealed a puzzling pattern: while some infected people have only mild symptoms, others struggle for breath in intensive care units. This article explores one reason for those differences that lies deep in our DNA. By examining specific immune system genes in Egyptian patients, the researchers show how genetic variations can tilt the odds toward mild or severe illness, and how this knowledge might guide more personalized care in future outbreaks.
The body’s ID check for viruses
Our immune system depends on a set of genes called HLA, which help cells flag invading germs so immune defenders can destroy them. One part of this system, known as HLA-B, is especially variable from person to person. Think of HLA-B as a set of molecular ID cards: some versions display pieces of the coronavirus clearly, prompting a swift attack, while others may show fuzzier signals, slowing the response. The authors set out to see whether particular versions of HLA-B were linked to how sick people became after catching SARS-CoV-2, the virus that causes COVID-19.
Who was studied and what was measured
The team followed 45 adults with confirmed COVID-19 who came to a fever hospital in Alexandria, Egypt, between late 2022 and early 2023. Doctors grouped them by illness severity: 15 with mild symptoms who did not develop pneumonia, 15 with moderate disease, and 15 with severe disease requiring hospital care and showing diffuse “ground-glass” changes on lung scans. For each person, nose and throat swabs were tested by PCR to estimate viral load, using the cycle threshold (Ct) value: a lower Ct means more virus. Blood samples were then analyzed to determine each patient’s HLA-B type, along with routine lab tests such as liver enzymes, clotting markers, and electrolytes.
Patterns in age, viral load, and blood tests
Several familiar risk signals emerged. Patients in the severe group were notably older on average than those with mild or moderate illness, reinforcing the idea that age makes COVID-19 more dangerous. Their Ct values were lower, indicating higher levels of virus in the body. They also had fewer lymphocytes (a type of white blood cell crucial for fighting infections), lower platelet counts, and higher levels of liver enzymes and inflammation markers such as C-reactive protein and D-dimer. Together, these measures painted a picture of a stronger viral assault and broader organ stress in the sickest patients.
The genetic fingerprints of severe disease
The heart of the study lay in comparing HLA-B types across the three severity groups. In total, 39 different HLA-B genetic combinations and 22 individual versions (alleles) were identified, which the researchers also grouped into broader “supertypes” that share similar behavior. Two versions stood out: HLA-B*08 and HLA-B*44. These alleles were significantly more common among hospitalized patients (those with moderate or severe disease) than in the mildly ill group. When all three severity levels were compared, HLA-B*44 in particular showed a strong link with worse outcomes. This suggests that people carrying these genetic variants may be less efficient at presenting key coronavirus fragments to their immune cells, allowing the virus to multiply and damage the body more extensively.
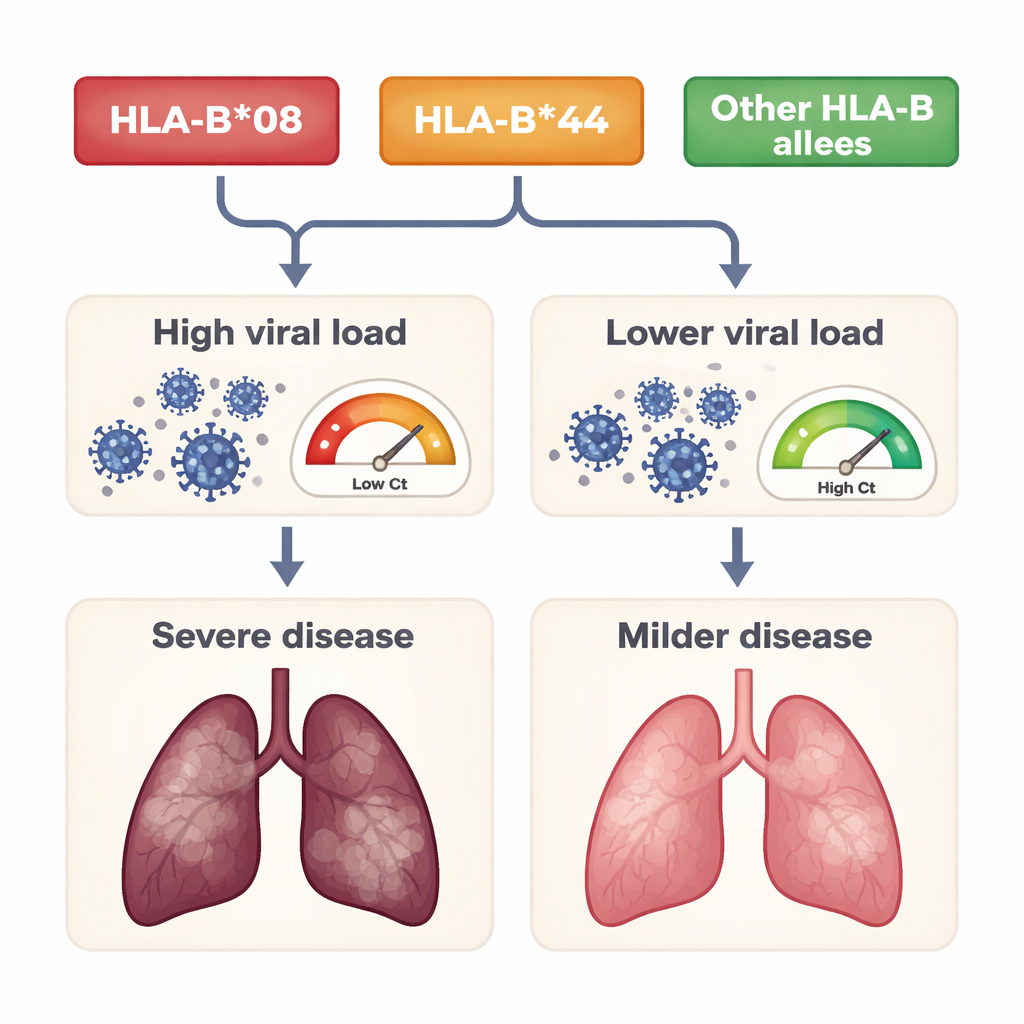
What this could mean for future care
For non-specialists, the key takeaway is that some people’s immune systems are genetically primed to cope better with COVID-19 than others. In this Egyptian group, higher viral loads, older age, and certain blood test abnormalities signaled more dangerous illness, and two HLA-B variants—HLA-B*08 and HLA-B*44—were closely tied to that severity. While the study is small and limited to one hospital, it supports a broader view that genetics helps shape who is most at risk. In the long run, such findings could feed into risk scores that combine age, lab tests, and gene profiles to identify patients who need closer monitoring or early aggressive treatment, and to design vaccines and therapies that work well across diverse genetic backgrounds.
Citation: Abdelmonem, R., Selim, H., Abdullah Mohamed, S. et al. Association of human leukocyte antigen B genotypes with COVID-19 severity in Egyptian patients. Sci Rep 16, 7193 (2026). https://doi.org/10.1038/s41598-026-36948-7
Keywords: COVID-19 severity, HLA-B genes, host genetics, viral load, Egyptian patients