Clear Sky Science · en
Interpretable machine learning-based real-time sepsis diagnosis
Why a Silent Infection Needs Faster Alarms
Sepsis is a medical emergency that can turn a routine infection into a life‑threatening crisis within hours. Yet its early warning signs are often subtle, especially in busy hospitals or remote clinics with limited staff and equipment. This paper describes a low‑cost, interpretable machine‑learning system that watches basic vital signs in real time and raises the alarm when a patient may be slipping into sepsis, even outside an intensive care unit.
The Hidden Toll of a Fast-Moving Killer
Sepsis happens when the body’s response to infection spirals out of control, damaging vital organs and, in many cases, leading to death. Globally, tens of millions of people develop sepsis each year, and many do not survive. The condition is not only deadly but also extremely expensive to treat, placing a heavy burden on health systems and families. In wealthier countries, a single sepsis case can cost tens of thousands of dollars; in poorer regions, the lack of intensive care units and specialists means that many cases are never recognized in time. Early diagnosis is crucial, but doctors still lack simple, reliable tools that work where laboratory tests, advanced imaging, and constant bedside monitoring are unavailable.
A Smart Watchdog for Basic Vital Signs
Instead of relying on complex lab results, the authors built their system around seven routine, non‑invasive measurements: heart rate, body temperature, three types of blood pressure, blood oxygen level, and exhaled carbon dioxide. Using a large public database of intensive‑care patients, they carefully cleaned the data, filled in missing values in a way that mimics real bedside practice, and designed new features that track how these vital signs change over time rather than looking at single readings in isolation. They also incorporated simplified versions of existing bedside scoring tools used by nurses to spot deterioration. These engineered features fed lightweight machine‑learning models, particularly gradient‑boosting and random‑forest methods, tuned to balance fast computation with high accuracy. 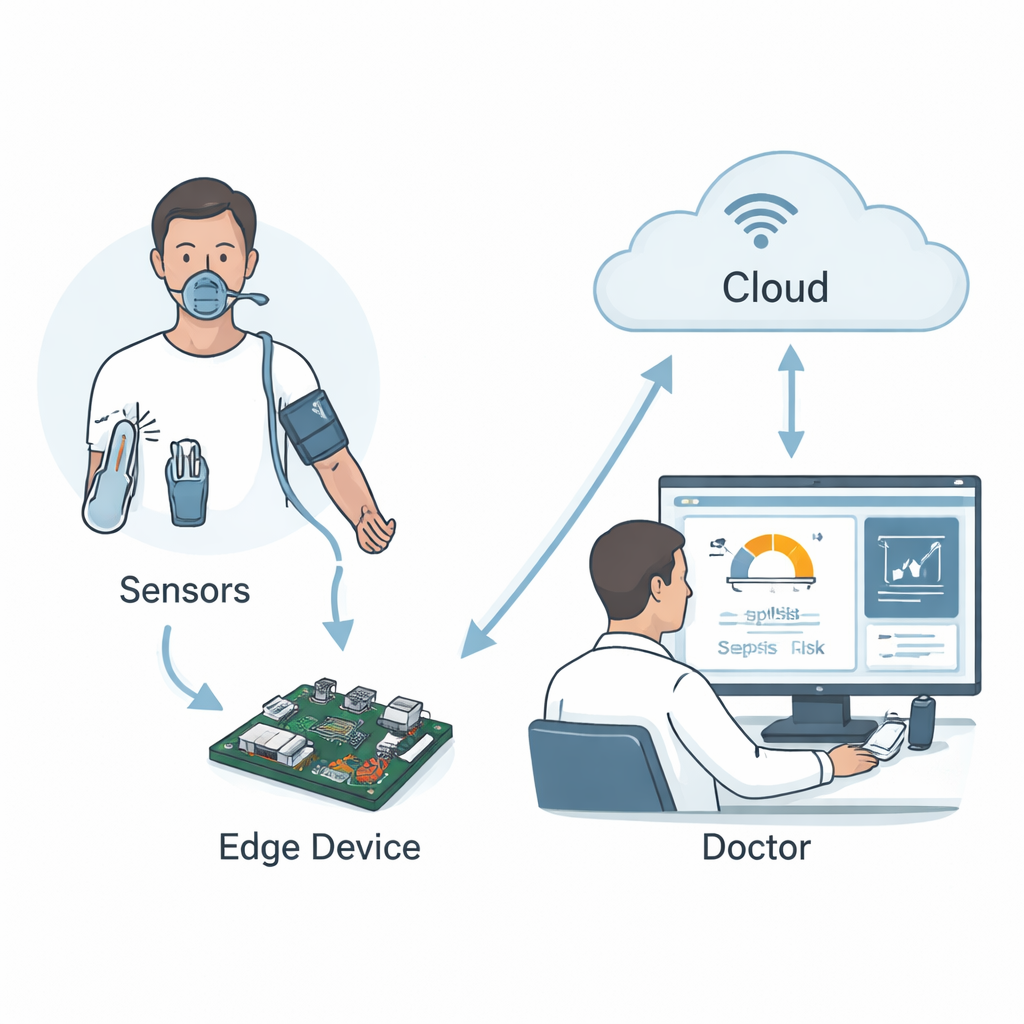
Balancing Rare Crises and Everyday Stability
One obstacle in training any medical prediction model is that dangerous events like sepsis are relatively rare compared with the many hours in which patients remain stable. If this imbalance is not handled well, an algorithm may “play it safe” and simply predict that no one has sepsis most of the time. The researchers compared several existing strategies and then proposed a new one they call Non‑Overlapping Subset Ensemble (NOSE). In NOSE, the large pool of low‑risk cases is sliced into several distinct groups, each combined with all the known sepsis cases to train its own model. These models are later combined into an ensemble so the system learns as much as possible from both sick and healthy examples without distorting the data through artificial copies. This design helped the system reach an accuracy of about 86% and a high ability to separate septic from non‑septic patients, as measured by an AUROC score of 0.94.
Opening the Black Box for Doctors
Medical staff are understandably wary of black‑box algorithms that cannot explain their decisions. To build trust, the authors used two explanation tools, SHAP and LIME, that highlight which vital signs and patterns most influenced each prediction. Across many patients, the system relied heavily on trends in temperature, breathing rate, heart rate, and blood pressure over time, rather than on one‑off spikes. For individual patients, it can show how, for example, a rising temperature combined with steadily climbing heart and breathing rates pushed the risk score upward. This kind of transparency lets clinicians check whether the model’s reasoning matches their own judgment and may help them spot errors in the data.
From Laptop to Portable ICU
To prove that the idea works outside a research lab, the team implemented a simplified version of the model on a Raspberry Pi microcomputer connected to an infrared thermometer and a pulse oximeter that measures heart rate and oxygen saturation. Despite relying on only a subset of the full vital‑sign set, this low‑cost prototype still performed well in small tests. The authors also sketched a telemedicine system in which readings from patients in remote villages are sent over the internet to doctors in city hospitals, who can review automated risk scores and explanations on a dashboard before recommending treatment. 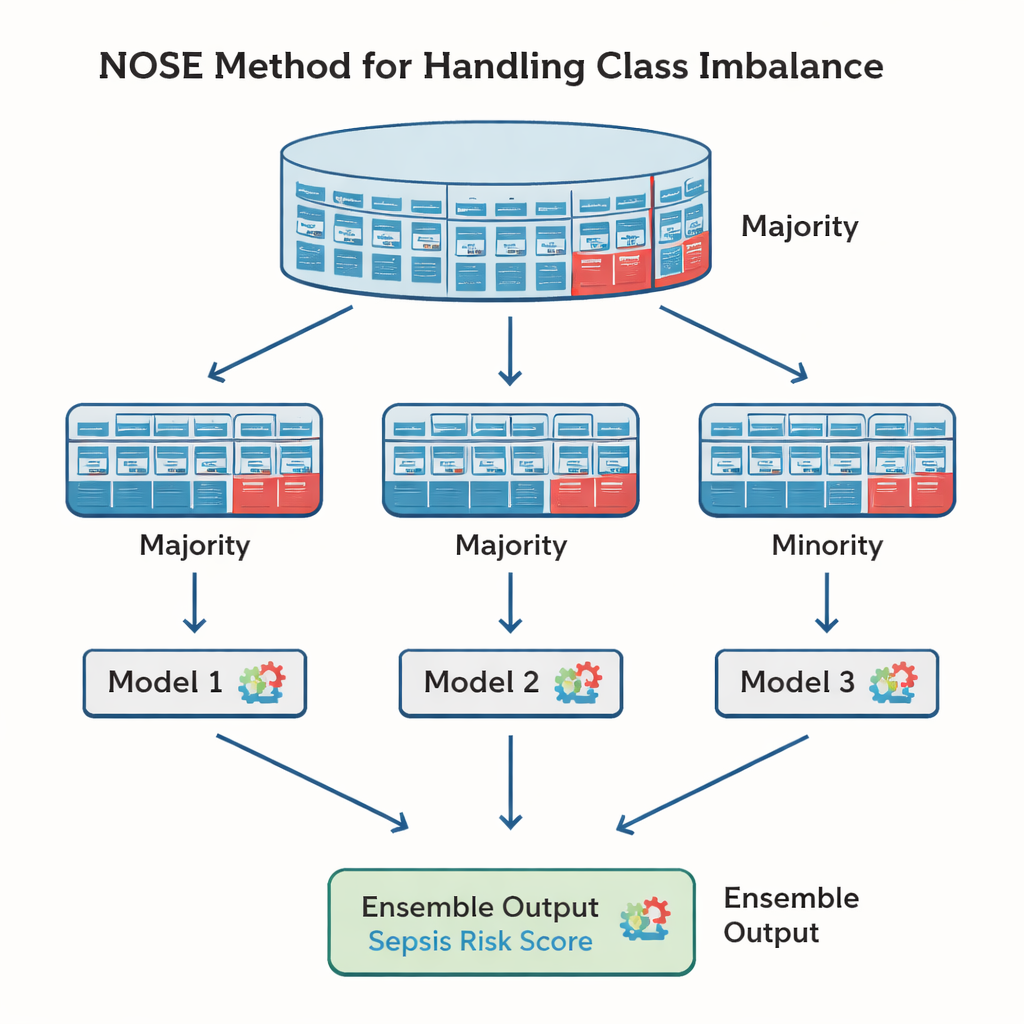
Bringing Early Sepsis Detection to the Bedside
In everyday terms, this work shows that a small, affordable device using only basic vital signs can act as an always‑on lookout for sepsis, flagging danger hours before a human might notice. By combining careful data handling, a novel way to learn from rare events, and clear explanations for its alerts, the system bridges the gap between advanced artificial intelligence and the practical needs of nurses and doctors. If expanded and rigorously tested in real‑world settings, such portable "mini ICUs" could help save lives in crowded hospitals and remote communities alike by turning silent early warnings into actionable, timely care.
Citation: Mahmud, F., Quamruzzaman, M., Sanka, A.I. et al. Interpretable machine learning-based real-time sepsis diagnosis. Sci Rep 16, 6702 (2026). https://doi.org/10.1038/s41598-026-36945-w
Keywords: sepsis, vital signs, machine learning, telemedicine, early diagnosis