Clear Sky Science · en
An online interpretable machine learning model for predicting cardiometabolic multimorbidity risk in patients with type 2 diabetes mellitus
Why this matters for people with diabetes
Many people living with type 2 diabetes don’t have just one health problem—they also face heart disease, stroke, or high blood pressure. This combination, called cardiometabolic multimorbidity, greatly raises the chance of early death and costly hospital care. The study behind this article presents a new, easy-to-use online tool that helps doctors estimate an individual’s risk of developing these serious complications early, using routine test results, and explains in plain terms which factors are driving that risk.
Diabetes and its hidden partners
Type 2 diabetes has become one of the most common long-term illnesses worldwide. By the time many people are first diagnosed, they already have one or more other conditions, especially heart and blood vessel disease or high blood pressure. Together, these problems—collectively called cardiometabolic multimorbidity—greatly increase the risk of heart attacks, strokes, and early death, and they more than double medical costs. Current guidelines recommend regular heart risk checks for people with diabetes, but clinics often lack simple, accurate tools that capture the full picture of multiple conditions at once.
Turning everyday clinic data into a risk forecast
The researchers gathered information from 1,153 adults with type 2 diabetes treated at two large hospitals in Shanxi Province, China. After applying medical inclusion and exclusion rules and dealing carefully with missing values, they ended up with 793 patients to build the model and 360 more to test it independently. From each patient, they collected basic details such as age and how long they had diabetes, as well as common blood tests including long-term blood sugar (HbA1c), sugar levels after meals, liver enzymes, kidney markers, and a scan-based measure of belly fat. Cardiometabolic multimorbidity was defined as having diabetes plus at least one of these: heart disease due to blocked arteries, stroke, or high blood pressure.

Teaching a smart model and then opening the “black box”
To predict who would have cardiometabolic multimorbidity, the team tested several machine learning approaches—computer programs that learn patterns from data. They first used a method called recursive feature elimination to winnow dozens of measurements down to nine especially informative ones: post-meal blood sugar, HbA1c, age, visceral (deep belly) fat, platelet count, an insulin resistance score, the ratio of two liver enzymes (AST/ALT), years living with diabetes, and whether the person was using injected insulin under the skin. They then compared six different algorithms and found that a “Stacking” model—an ensemble that combines the strengths of several methods—gave the most reliable results. In internal testing it correctly separated high- and low-risk patients with an area under the curve (AUC) of 0.868, and in an independent hospital it still performed well with an AUC of 0.822.
Which factors matter most for risk
Because complex models can be hard to trust if they are opaque, the team applied two explanation tools, SHAP and LIME, that show how each input pushes a person’s risk up or down. Across the whole group, three factors stood out as especially important: HbA1c, age, and whether the person was using insulin injections. Higher HbA1c and older age clearly raised risk, as did higher post-meal blood sugar, more visceral fat, and a higher insulin resistance score. Platelet counts and the AST/ALT ratio also played supporting roles, reflecting clotting tendency and possible heart–liver strain. The explanations for individual patients showed, for example, how a middle-aged person with long-standing diabetes, high belly fat, and very high HbA1c could have an estimated risk close to 90%, while someone with better-controlled sugar and less visceral fat might have much lower risk even at a similar age.
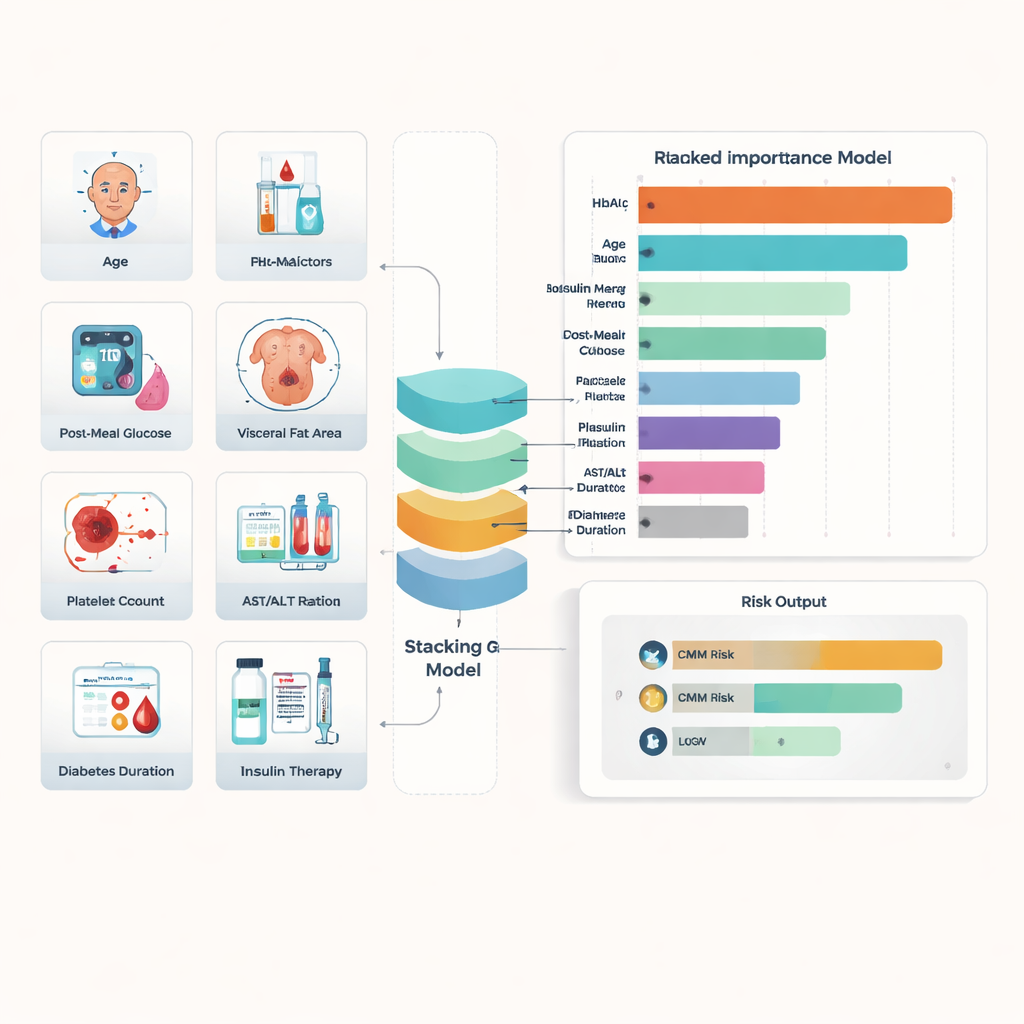
A web tool for real-world decisions—and its limits
To make the research practical, the authors built a free web application where a clinician can enter the nine selected measurements and instantly receive a personalized risk estimate along with a visual explanation of which factors are driving it. The system is designed not to store patient data and is currently intended as a support for education and research rather than a stand-alone diagnostic device. The study does have limits: it uses past records from two hospitals in one region of China, and it relies on measurements taken at a single point in time. The authors stress that larger, long-term studies in more diverse populations are needed before the tool can be considered universal.
What this means for people with type 2 diabetes
In everyday terms, this work shows that common tests already done in diabetes clinics—especially long-term blood sugar, post-meal sugar, belly fat measures, and how long someone has had diabetes—can be combined by a transparent smart algorithm to flag who is most likely to develop serious heart- and blood-pressure–related complications. Used alongside doctors’ judgment, such tools could help target intensive lifestyle changes and treatments to those who need them most, potentially preventing heart attacks and strokes and improving quality of life for people living with type 2 diabetes.
Citation: Liu, X., Li, C., Huo, X. et al. An online interpretable machine learning model for predicting cardiometabolic multimorbidity risk in patients with type 2 diabetes mellitus. Sci Rep 16, 5877 (2026). https://doi.org/10.1038/s41598-026-36923-2
Keywords: type 2 diabetes, heart disease risk, machine learning in medicine, multimorbidity, risk prediction tools