Clear Sky Science · en
Volume and functional changes of remnant pancreas after different types of pancreatectomy: Exploring the regenerative potential
Why surgeons and patients care about a “leftover” pancreas
When part of the pancreas is surgically removed—to treat cancer, cysts, or severe inflammation—patients often wonder what happens to the piece that stays behind. Does it grow back, shrink, or adapt in some way? And most importantly, how does this affect the risk of developing diabetes later on? This study followed people for two years after two common pancreatic operations to see how the remaining pancreas changed in size and how well it continued to make insulin, the hormone that keeps blood sugar in check.
Two different operations, two different leftovers
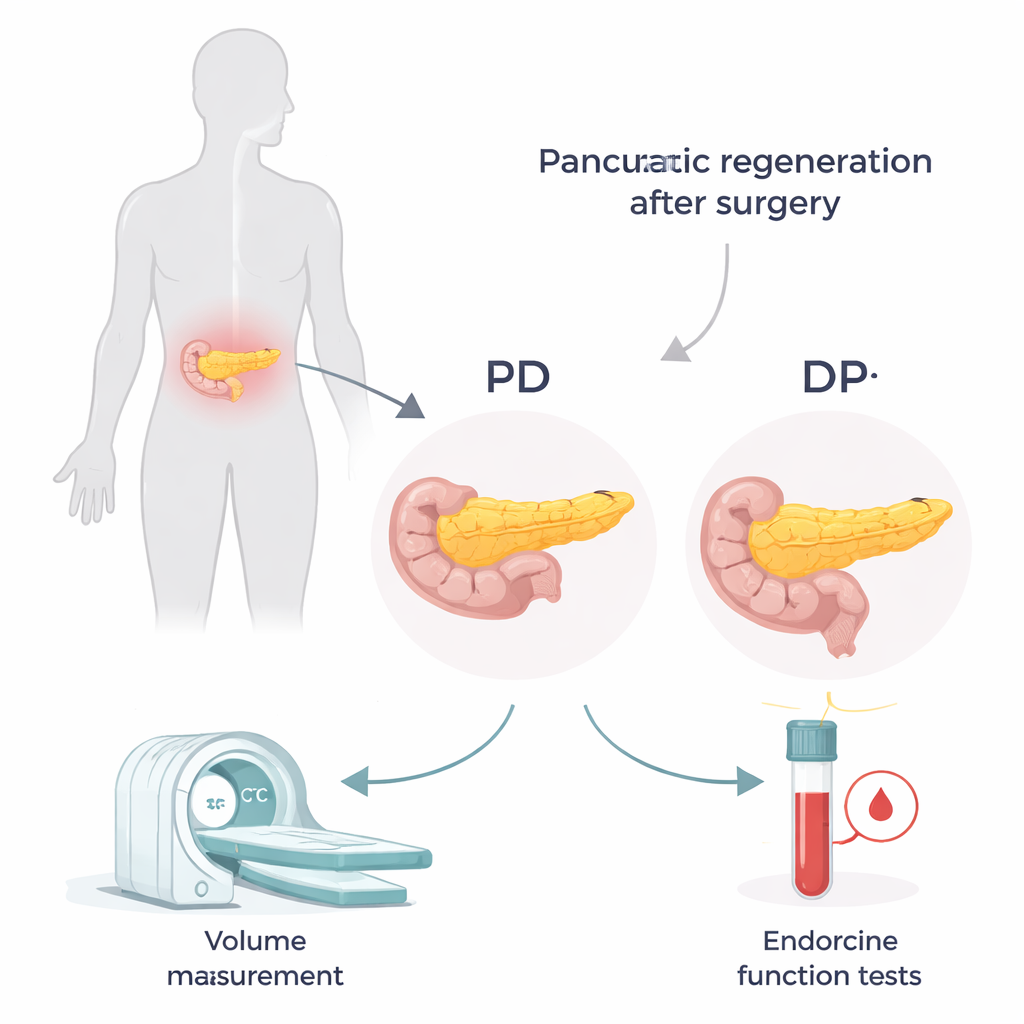
The pancreas sits deep in the abdomen and stretches from right to left. Surgeons choose between two main operations depending on where disease is located. In a pancreaticoduodenectomy (PD, often called the Whipple procedure), the right “head” portion is removed, leaving the middle and left “body and tail.” In a distal pancreatectomy (DP), the left “tail” portion is removed, leaving mainly the head. The head and tail are not identical: the tail is richer in the tiny clusters of cells that make insulin. That means losing the tail may have a bigger impact on blood sugar control, even if the overall amount of pancreas removed looks similar.
Measuring size and hormone power over time
To track how the pancreas adapted after surgery, the researchers reviewed records from 135 patients treated at a single hospital between 2009 and 2017. They used contrast-enhanced CT scans to measure the volume of the entire pancreas before surgery and the remaining portion at 3 months, 1 year, and 2 years afterwards. At the same visits, they checked blood tests related to sugar metabolism, including C-peptide—a marker of how much insulin the body is producing. By combining C-peptide with blood sugar levels into a simple index, they could estimate how efficiently the remaining pancreatic tissue was working.
When bigger does not mean better
The two surgeries produced strikingly different patterns of regrowth and shrinkage. After distal pancreatectomy, the remaining head region often grew larger over time: on average, its volume rose to about 110% of its immediate postsurgical size by two years, and nearly three-quarters of these patients showed clear hypertrophy, or enlargement. After pancreaticoduodenectomy, the opposite occurred: the remnant body and tail gradually wasted away to about two-thirds of its initial size, and true enlargement was rare. Dilatation of the main pancreatic duct—a sign that the drainage connection might be narrowed—was linked with greater shrinkage in PD patients. Yet, despite keeping more tissue overall, DP patients fared worse metabolically: about one-third of previously non-diabetic DP patients developed new diabetes, and none of those with existing diabetes went into remission.
The hidden strength of remaining insulin cells
Looking more closely at hormone output revealed why size alone did not tell the full story. In both groups, insulin production dipped at three months but then partially recovered. When the researchers adjusted insulin output for how much pancreas was left, they found that the pancreas after PD became surprisingly efficient: each unit of tissue produced more insulin over time. In contrast, patients who lost the insulin-rich tail in DP tended to have weaker endocrine recovery, even though their remaining pancreas was bulkier and sometimes even enlarged. This supports anatomical studies showing that the tail contains roughly twice as many insulin-producing cells as the head, and suggests that the surviving cells can “work harder” to compensate when needed.
Implications for surgery and long-term health
For patients and surgeons, these findings highlight that what matters most is not just how much pancreas is preserved, but which part. Removing the distal, islet-rich tail carries a higher risk for diabetes than removing the head, even when more total tissue is saved. Narrowing of the pancreatic duct after a Whipple procedure can further damage the remnant by causing scarring and shrinkage. The authors conclude that operations for benign or low-risk tumors should be planned to preserve as many insulin-producing cells as possible—sometimes favoring procedures that spare the tail—so that patients have the best chance at maintaining healthy blood sugar in the years after surgery.
Citation: Lu, WH., Tsai, HM., Liao, TK. et al. Volume and functional changes of remnant pancreas after different types of pancreatectomy: Exploring the regenerative potential. Sci Rep 16, 6947 (2026). https://doi.org/10.1038/s41598-026-36886-4
Keywords: pancreatectomy, pancreatic regeneration, pancreatogenic diabetes, endocrine function, pancreaticoduodenectomy vs distal pancreatectomy