Clear Sky Science · en
Interpretable machine learning unveils non-linear inflammatory thresholds and synergistic interactions in post-burn hypertrophic scarring: development of an intelligent clinical decision support system
Why scars after burns matter
For people who survive severe burns, the battle does not end when the skin closes. Many go on to develop thick, raised scars that can itch, hurt, and even lock joints in place, making everyday tasks difficult. Doctors know that some patients are far more prone to these hypertrophic scars than others, but current prediction tools are crude. This study explores how an "intelligent" yet transparent computer system can help doctors foresee who is likely to develop severe scarring and act early to prevent it.
Looking beyond simple checklists
Traditional medical prediction tools often work like weighted checklists: each risk factor adds a bit to the final score in a straight line. But the biology of bad scarring after burns is anything but simple. It involves a storm of inflammation, massive tissue damage, and the body’s repair machinery sometimes going into overdrive. The authors followed 520 adults with major burns treated at a single hospital. For each patient, they collected 15 pieces of information at admission, including burn size and depth, early blood tests, infection status, and how long it took to reach the operating room. Instead of assuming that each factor acts independently, they used a modern pattern-finding approach to let the data reveal more complex relationships.
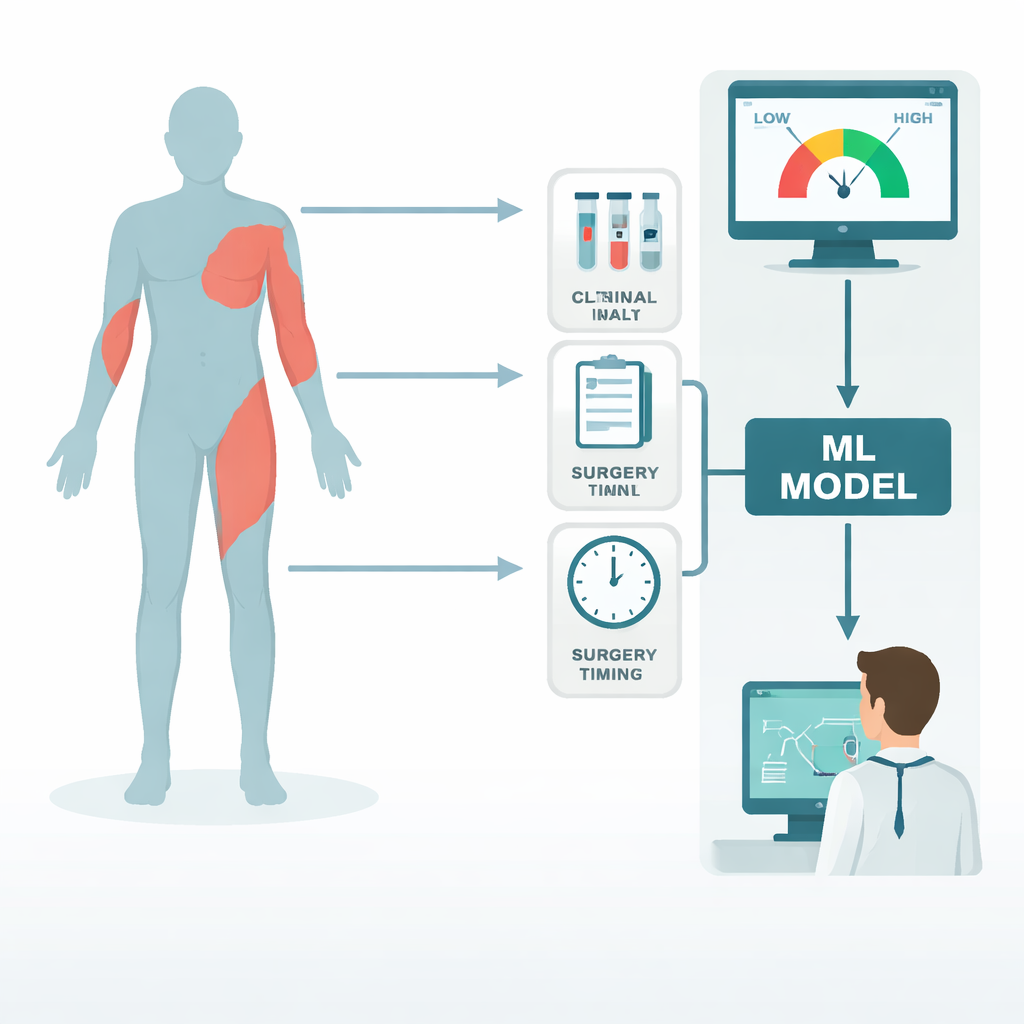
An intelligent risk calculator you can look inside
The team compared several types of computer models and found that a method known as gradient boosting best separated patients who later developed thick scars from those who did not. Importantly, they did not stop at accuracy. They paired the model with an explanation tool called SHAP that shows, for each prediction, how much every input nudged the risk up or down. In tests on unseen patients, the system correctly distinguished high- from low-risk cases most of the time and was better calibrated than classic statistical models, meaning its predicted probabilities closely matched what actually happened. Decision analyses suggested that using this system to guide prevention strategies would benefit more patients than simply treating everyone or relying on burn size alone.
Hidden tipping points in inflammation
When the authors opened the model’s “black box,” a striking pattern emerged: an inflammation blood test called C-reactive protein (CRP) was the single strongest predictor of scarring. But its effect was not linear. At moderate levels, changes in CRP barely altered risk. Once CRP climbed into roughly the 80–120 mg/L range, the model’s estimated risk shot up, forming an S-shaped curve rather than a straight line. Other markers of systemic stress, such as large full-thickness burn areas, high white blood cell counts, and low blood albumin, also pushed risk upward, while better nutritional status appeared protective. These findings hint that there may be practical thresholds of inflammation above which the body’s repair processes are more likely to leave lasting, rigid scars.
When risk factors team up
The study also shows that risk factors do not simply add up; they can amplify each other. Younger adults with the same burn size as older patients were more likely to be labeled high risk, suggesting that stronger immune and growth responses in youth may drive more aggressive scar formation. Large burn areas and high CRP levels together produced much higher risk than either alone, underlining the danger of a big burn combined with intense inflammation. Infection and timing of surgery formed another crucial pair: in patients without wound infection, a modest delay to surgery did not raise risk much, but in those with infected wounds, delays were linked to sharply higher predicted risk. These patterns emphasize the need to consider combinations of factors, not just single numbers in isolation.
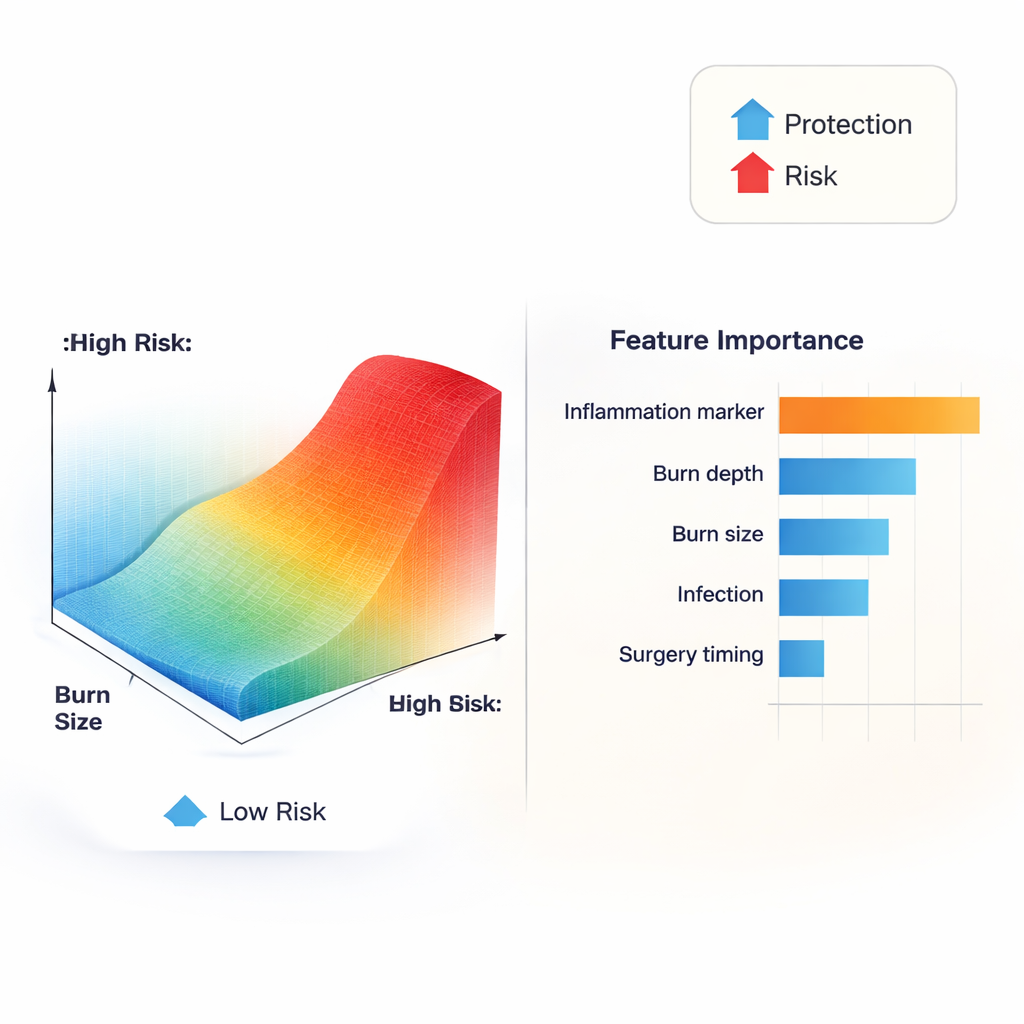
From complex data to bedside decisions
To make their work usable, the researchers built a prototype web-based decision support system. A clinician can enter routine clinical data and receive an immediate, individualized scar risk estimate. The system then displays a simple visual breakdown showing which factors are driving that patient’s risk up and which offer protection. One example patient had moderate burn size but extremely high CRP and infection; the tool clearly highlighted inflammation as the main culprit. Another patient’s low risk was traced primarily to very early surgery. While the system still needs testing at other hospitals and over longer follow-up periods, it illustrates how complex mathematics can be converted into clear, patient-specific guidance.
What this means for patients and doctors
In everyday terms, this research suggests that doctors may soon have a smarter way to see, early on, which burn survivors are on a collision course with severe scarring. By revealing hidden tipping points in inflammation and showing how age, burn extent, infection, and treatment timing interact, the system moves beyond rules of thumb toward tailored prevention. If validated more widely, such an interpretable tool could help teams intensify anti-inflammatory care, tighten infection control, and prioritize timely surgery for those who need it most, ultimately improving function and quality of life after devastating burns.
Citation: Tian, T., Liu, S. & Ji, G. Interpretable machine learning unveils non-linear inflammatory thresholds and synergistic interactions in post-burn hypertrophic scarring: development of an intelligent clinical decision support system. Sci Rep 16, 6908 (2026). https://doi.org/10.1038/s41598-026-36868-6
Keywords: burn scars, inflammation, machine learning, clinical decision support, precision medicine