Clear Sky Science · en
A hybrid blockchain migration framework for converting traditional databases into blockchain-based EMR systems
Why hospital records need a new safety net
Every time you visit a clinic, your story is written into an electronic medical record: diagnoses, test results, prescriptions, even allergies. These digital files help doctors coordinate care, but they also create a tempting target for mistakes, hackers, and quiet edits that are hard to trace. This paper explores a practical way to make hospital records far harder to tamper with—without slowing doctors down—by blending familiar database technology with blockchain, the same kind of ledger that underpins many cryptocurrencies.
The problem with one big hospital database
Most hospitals today keep patient information in a single, central database. All departments—emergency room, lab, pharmacy, billing—send their updates into this one system. That design is fast and convenient, but it creates a single point of failure. A cyberattack, software bug, or careless change by a powerful administrator can silently corrupt years of records, and backup copies often just preserve the damaged state. Regulators in places like Oman now demand strong proof of who accessed which data, when, and whether anything was altered. Traditional databases were never built to provide this kind of tamper-evident trail.
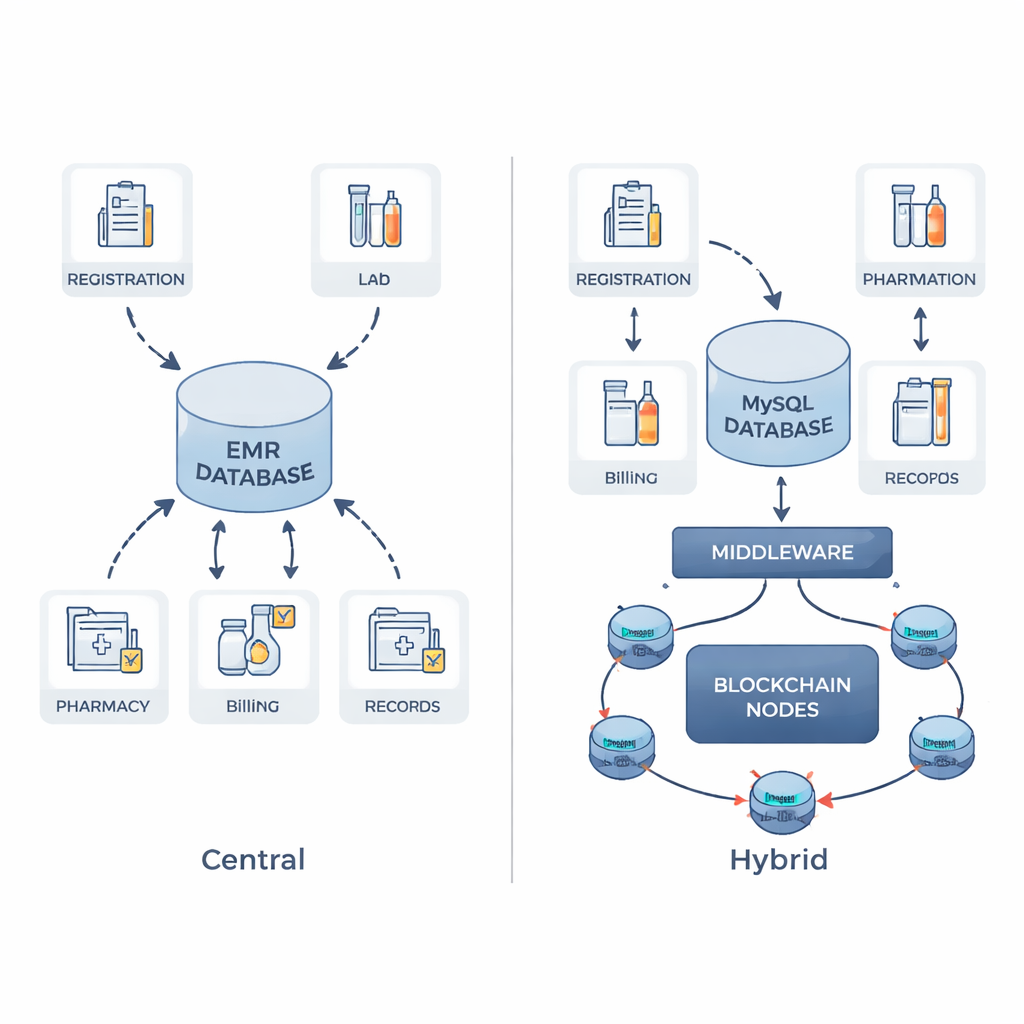
A blended approach instead of a risky overhaul
Replacing existing hospital systems with a full blockchain would be hugely disruptive and slow: blockchains process far fewer transactions per second than a tuned database. The authors instead propose a hybrid design. Doctors and nurses keep using the familiar OpenMRS record system backed by a MySQL database. Behind the scenes, only selected, sensitive pieces of information—such as patient IDs, diagnoses, prescriptions, and lab summaries—are turned into cryptographic fingerprints (hashes). These fingerprints, along with basic details about the change, are sent to a private blockchain network built with Hyperledger Fabric, which is shared across hospital departments and can later include outside partners such as the Ministry of Health.
How the "shadow ledger" quietly watches every change
The heart of the framework is a middleware service that acts like a vigilant clerk. When a record is created or updated in the database, small programs called triggers automatically compute a SHA-256 hash for that row and log the event. The middleware reads these logs, formats them as blockchain transactions, and submits them to the Fabric network, where multiple departmental computers must agree before a block is added. Only hashes and simple metadata travel to the blockchain; the actual medical details stay inside the hospital database. Later, a separate validator tool can recompute the hashes and compare database and blockchain versions, quickly exposing any hidden tampering or accidental change.
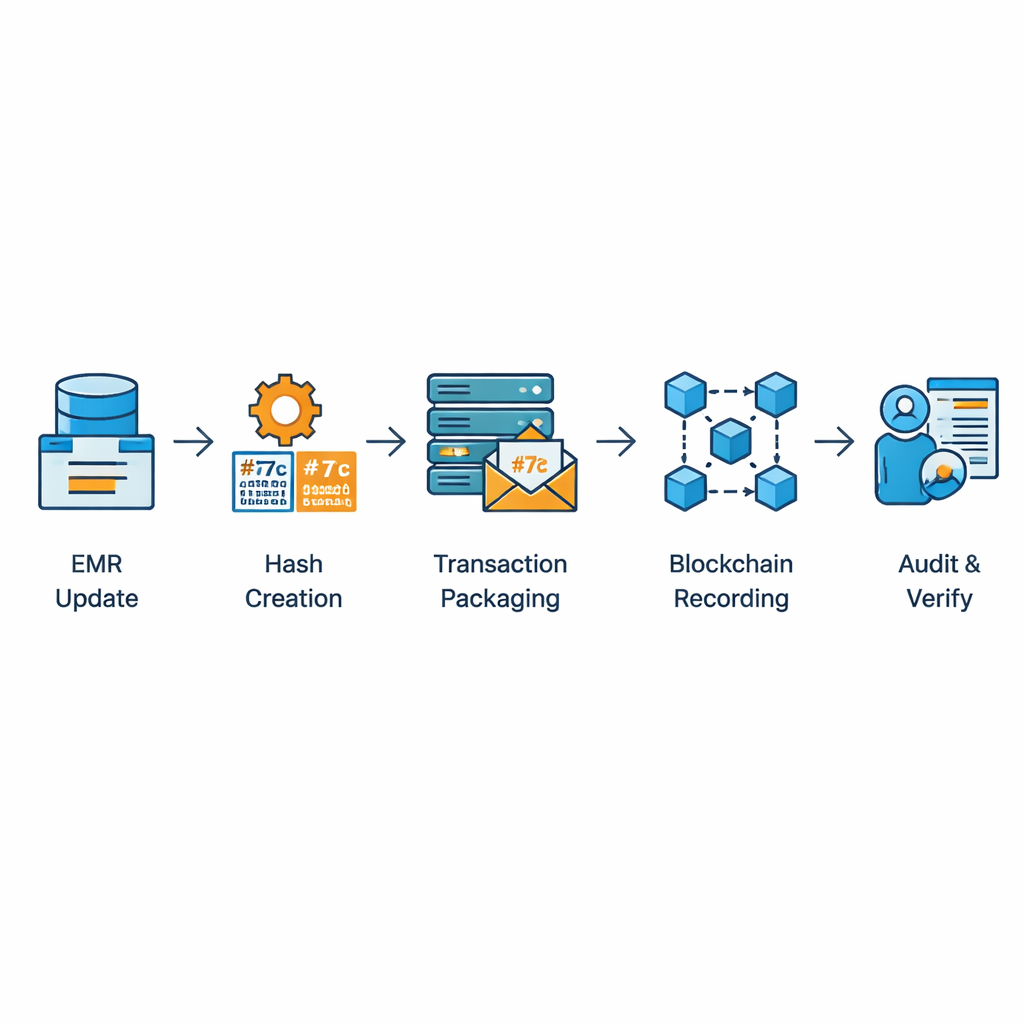
Putting performance, security, and law to the test
To see whether this design is practical, the team built a full lab setup: OpenMRS with MySQL, a six-organization Fabric network representing hospital departments, the middleware, and a web-based blockchain explorer for auditors. They then compared three scenarios: pure MySQL, pure blockchain, and the hybrid. The database alone handled about 560 transactions per second with response times around 1.6 milliseconds. Fabric alone was far slower—about 17 transactions per second with roughly 60 milliseconds delay. The hybrid system preserved near-database speed (about 480 transactions per second and 2.1 milliseconds delay) while still writing hashes to the blockchain. Resource use on a modern laptop-class machine remained moderate, suggesting the approach can scale to real hospitals. The design also maps directly onto Oman’s Personal Data Protection Law by providing immutable logs, strict access control, and tools for independent audits without exposing patient details on-chain.
What this means for future hospital care
In plain terms, the study shows that hospitals do not need to scrap their existing record systems to gain blockchain’s trust benefits. By adding a smart "shadow ledger" that records proofs of important changes, they can keep systems fast and familiar for clinicians while making it vastly harder for attackers—or insiders—to quietly rewrite history. Regulators gain a clear window into how data is used, and patients gain stronger assurance that their medical story cannot be silently edited. The authors argue that this kind of hybrid, step-by-step upgrade path is the most realistic way for blockchain to become part of everyday clinical practice.
Citation: Al-Busaidi, A., Mani, J., Yoosuf, M.S. et al. A hybrid blockchain migration framework for converting traditional databases into blockchain-based EMR systems. Sci Rep 16, 7348 (2026). https://doi.org/10.1038/s41598-026-36787-6
Keywords: electronic medical records, blockchain, health data security, audit trails, hybrid database systems